Research Article - Biomedical Research (2017) Volume 28, Issue 19
Short-term efficacy of patients with brain metastases from lung cancer treated by micro catheter intervention chemotherapy
Qian Chen1,2, Jing Ren3, Xinyu Yang1# and Zaiyu Guo2*#
1Department of Neurosurgery, Tianjin Medical University General Hospital, Tianjin, PR China
2Department of Neurosurgery, Tianjin TEDA Hospital, Tianjin, PR China
3Department of Respiratory Medicine, Tianjin TEDA hospital, Tianjin, PR China
#These authors contributed equally to this work
Accepted date: August 30, 2017
Abstract
Objective: To evaluate the application of micro catheter technique in interventional treatment of Intracranial Metastatic Tumor (IMT) by observing the short-term efficacy of patients with IMT from lung cancer treated by micro catheter intervention chemotherapy.
Methods: From September 2012 to August 2016, a total of 33 patients with IMT from lung adenocarcinoma received Arterial Infusion Chemotherapy (AICT) using micro catheter technique. This procedure was performed every 4 w for 2 times in succession. Follow-up head enhanced MRI was used in 4 weeks after the last treatment to evaluate the short-term efficacy according to the RECIST.
Results: 33 cases were treated. Complete response was obtained in 1 (3.03%), partial response was obtained in 17 (51.52%), stable condition in 12 (36.36%), and deterioration in 3 (9.09%). The effective rate of IMT was 48.48%(16/33, p>0.05) and the 69.70% (23/33, p<0.05) were brought under control. All the side effects were grades I and II (27.27%, 9/33). The rate of cerebrovascular complication was 13.64% (9/66), without obvious sequelae after treatment.
Conclusion: Interventional chemotherapy of IMT using micro catheter technique has a reliable shortterm efficacy, with minor and controllable side effects, is one of the effective options in treatment of IMT.
Keywords
Lung adenocarcinoma, Intracranial metastatic tumor, Micro catheter technique, Arterial infusion chemotherapy
Introduction
Intracranial Metastatic Tumor (IMT) can be concealed, especially in the elderly, often with no characteristic clinical manifestation, and are found in the examination. Along with the progress of imaging technology and the improvement of the health level in urban and rural residents, patients with IMT have increased in recent years. The primary tumor is more common in lung cancer, especially in lung adenocarcinoma which metastatic rate is up to 43% [1]. The appropriate treatment for patients with advanced IMT who are in good general condition appear to be particularly important. Whole Brain Radiotherapy (WBRT) or systemic chemotherapy is less effective with systemic reaction and great cognitive impairment, so the overall treatment effect is poor [2]. The application of Bronchial Arterial Interventional Chemotherapy (BAICT) in patients with lung cancer has been widely used and achieved good results in the treatment of non-small-cell lung cancer. Interventional perfusion therapy for intracranial tumors was also adapted and the median survival time can be extended to 7 months [3]. However, chemotherapy drugs were often perfused through the catheter in the internal carotid or vertebral artery, which led to corresponding arterial convulsion or stroke after chemotherapy in many cases, especially in arteriae ophthalmica. Therefore, the application of Intracranial Perfusion Chemotherapy (IPCT) is restricted.
With the progress and development of the material science, micro catheter technology has been widely used in the field of neural intervention, including double micro catheter technology or even three micro catheter technology which has played an active role in the treatment of aneurysm embolization assisted with stent and other diseases. Thus, the author attempts to use the single micro catheter technology for perfusion treatment of chemotherapy drug in the 2-3 levels of intracranial arterial. The results showed that the method has better short-term efficacy in the treatment of IMT with the advantages of traditional infusion chemotherapy, the possible occurrence of intracranial complications and the side effects are smaller.
Materials and Method
General data
Single IMT patients from lung adenocarcinoma from September 2012 to August 2016 were retrospectively analysed and 33 patients were enrolled in the study. Patients received BIACT for lung adenocarcinoma and IMT by micro catheter under digital subtraction angiography (DSA). Median age was 60 y old (27-76) with 24 male and 9 females. Fourteen cases with IMT were firstly found in neurology department, and then CT-value found the biopsy of the lung, and lung adenocarcinoma was confirmed by bronchoscopy or percutaneous biopsy. Other 19 cases found lung adenocarcinoma in the department of respiration, IMT was found during the general check-up and confirmed by head enhanced MRI. Pathological diagnosis of all patients was lung adenocarcinoma, routine abdominal B ultrasound examination before the first treatment showed tumor did not transfer to other parts of the body, only in brain. The size was 0.5 cm-5 cm, 17 cases with less than 3 cm, and 16 cases with 3 cm-5 cm. The place of the tumor was in frontal lobe (8 cases), temporal lobe (13 cases), parietal lobe (6 cases), temporal and occipital lobe (3 cases), frontotemporal area (1 case), forehead top (1 case) and temporal lobe top (1 case). Karnofsky Performance Status (KPS) was 60 in 8 cases, 70 in 11 cases, 80 in 9 cases and 90 in 5 cases.
Inclusion criteria: 1) The patients was confirmed to lung adenocarcinoma by bronchoscopy or percutaneous biopsy without resection by intrathoracic surgery; 2) IMT was diagnosed by Imaging and confirmed by enhanced MRI; 3) IMT was solitary lesions with size of 0.5 cm-5 cm; 4) Brain angiography confirmed that IMT was supplied with anterior circulation including the branch of arteriae cerebri anterior or arteriae cerebri media; 5) First treatment was intravenous chemotherapy, radiotherapy or radiotherapy combined with chemotherapy; 6) KPS was more than 60 score; 7) No serious organ dysfunction, no abnormal coagulation and blood abnormalities; 8) Patients signed informed consent.
This study was approved by the ethics committee at our hospital and was conducted in accordance with the provisions of the Declaration of Helsinki, Good Clinical Practice guidelines, and local laws and regulations.
Methods
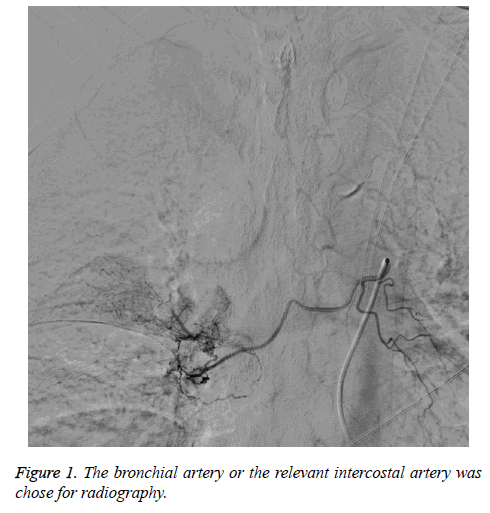
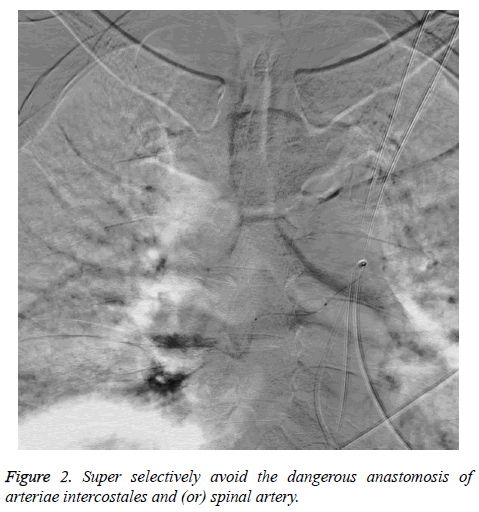
Perfusion chemotherapy for lung adenocarcinoma and IMT was done under DSA for two times. Tumor staining corresponding to the preoperative imaging examination was set as the standard to the selection of tumor nourishing vessel. Arterial Infusion Chemotherapy (AICT) of IMT adapted to combination with Teniposide (VM-26), Carmustine (BCNU), Carboplatin (CBP), and Pirarubicin (THP). Individualized dosage was calculated according to the patient's body surface area. Right femoral artery was punctured by Seldinger method and 5F arterial sheath (SCW, Shenzhen, China) was placed in. The 5F JL4.5 catheter (Cordis, Florida, USA) was placed near the mesenteric artery of the abdominal aorta and 8 mg ondansetron was pushed in slowly. And then bilateral bronchial artery or the relevant intercostal artery was chose for radiography (Figure 1). Guided by SilverSpeed-14 (ev3, Plymouth, MN, USA), Echelon-10 45º micro catheter (ev3, Plymouth, MN, USA) can super-selectively avoid the dangerous anastomosis of arteriae intercostales and (or) spinal artery. After blood supply artery of the tumor was confirmed by micro catheter angiography (Figure 2), 20 ml normal saline or glucose diluted Etoposide (VP-16), THP, Cisplatin (CDDP) were perfused with 2 ml/min by high pressure syringe. The position of the catheter and its tip should be observed during the process of perfusion. Timely angiography should be done again if the position was suspected to shift, to ensure the accuracy of perfusion vessels. 4 cases were supplied with bilateral bronchial artery, 2 cases with arteriae intercostales. The drug was perfused according to the size of the lesion, but the total amount of the lung was the same.
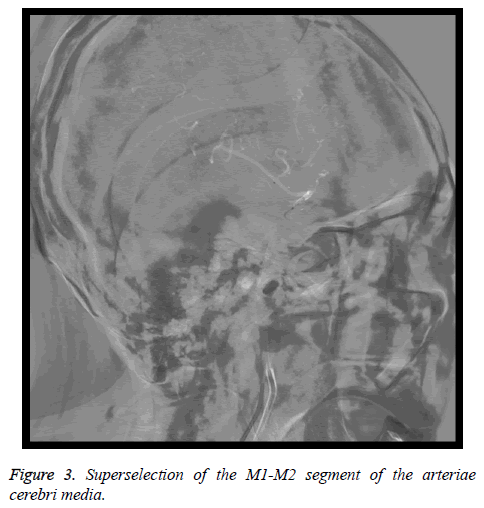
Whole cerebral angiography used 5 F catheter coude (Cordis, Florida, USA) for bilateral internal carotid artery angiography, bilateral external carotid artery angiography, and bilateral vertebral artery angiography. According to the location of the tumor staining, the super-selection of Echelon-10 45º micro catheter (ev3, Plymouth, MN, USA) guided by SilverSpeed-14 (ev3, Plymouth, MN, USA) was guided to the A1-A2 segment of the arteriae cerebri anterior and the M1-M2 segment of the arteriae cerebri media (Figure 3). At the same time, 0.3% papaverine injection was perfused through 5 F cordis catheter coude with 6 ml/min to prevent cerebral vasospasm, and then 30 ml 20% mannitol, 10 mg dexamethasone, 20 ml normal saline or glucose diluted VM-26, BCNU, THP, CBP were perfused with 3 ml/min by high pressure syringe. The position of the catheter tip should be observed during the process of perfusion. Timely angiography should be done again if the position was suspected to shift, to ensure the accuracy of perfusion vessels. Whole cerebral angiography showed 19 cases were supplied with the arteriae cerebri media, 10 cases with arteriae cerebri anterior and 4 cases with the both. The drug was perfused according to the size of the lesion, but the total amount of the brain was the same.
The artery sheath was removed after the perfusion and hemostasis by compression. The occurrence of side effects for chemotherapy drugs and blood vessel related complications should be observed after the operation, if necessary, treatments such as antiemetic, leukogenic, mannitol for dehydration, and nimodipine improving vascular spasm should be given. Patients were discharged after 1 w of operation. The above treatment was performed every 4 w for 2 times, and in 4 w after the last treatment, the head enhanced MRI was reviewed to evaluate the short-term curative effect.
Evaluation of short-term efficacy
Response Evaluation Criteria in Solid Tumors (RECIST) 1.1 version in 2009 was used to evaluate the efficacy of solid tumors [4]. According to the variation of the maximum diameter of the lesion, the results were divided into Complete Remission (CR, all lesions disappeared and were maintained for more than 4 w), Partial Remission (PR, the lesion was reduced at least 30% and maintained for more than 4 w), Stable Disease (SD, the situation was between PR and progression), and Progression of Disease (PD, The sum length of the single lesion increased more than 20%, the absolute value increased 5 mm or new lesions appear). Objective Response Rate (ORR)=CR+PR. Disease Control Rate (DCR)=CR+PR+SD.
Side effects during the treatment and follow-up were evaluated by Common Terminology Criteria Adverse Events (CTCAE) 3.0 version in 2003 produce by National Cancer Institute (NCI). Cerebrovascular complications during the treatment and after the operation mainly include stroke (irreversible ischemic or hemorrhagic events in intracranial vessels, showed in head CT or MRI), cerebral vasospasm (transient ischemia, not showed in head CT or MRI), and cerebral edema (normal tissue around metastatic tumor appear edema, chemotherapy may aggravate cerebral edema, head CT or MRI can be compared and evaluated).
Statistical analysis
The research data are calculated and analysed by using SPSS19.0 software. Data are shown as the relative number. Statistical significance was determined by χ2 test, with pvalue< 0.05 considered to be statistically significant.
Results
In this research, all 33 patients completed 2 times AICT treatment, and the survival time was more than 4 w after the last treatment, so short-term efficacy can be evaluated. The results showed CR in 1 case (3.03%), PR in 17 cases (51.52%), SD in 12 cases (36.36%), and PD in 3 cases (9.09%). ORR was 48.48% (16/33, p>0.05) and DCR was 69.70% (23/33, p<0.05). The clinical features and short-term efficacy of 33 patients were analysed, and the DCR of female patients was significantly higher than that of male patients (p<0.05). ORR and DCR of IMT patients supplied by arteriae cerebri media was higher than that by arteriae cerebri anterior or the both with significant difference (p<0.05). Overall, the short term efficacy of micro catheter intervention chemotherapy is better than that of conventional radiotherapy and chemotherapy.
Incidence rate of side effects associated with chemotherapy drugs was 27.27% (18/66), including 21.21% gastrointestinal reaction (14/66), and 12.12% blood toxicity reaction mainly with leukopenia. The side effects of this research all belong to grade I-II, which can be restored by symptomatic treatment. Incidence rate of side effects in patients with KPS<70 was significantly higher than others (p<0.05).
Incidence rate of cerebrovascular complications was 13.64% (9/66), including 3.03% stoke (2/66, all were ischemic stroke, lacunar infarction by CT or MRI without obvious neurological deficit after treatment), 10.61% cerebral vasospasm (7/66, papaverine infusion therapy during the operation and postoperative intravenous or oral nimodipine treatment), 12.12% cerebral edema (8/66, postoperative mannitol treatment). Incidence rate of cerebrovascular complications in IMT patients supplied by arteriae cerebri media was higher than that by arteriae cerebri anterior or the both with significant difference (p<0.05).
Discussion
The technique of AICT have been applied for many years, its effect and slightly controlled drug response are better than that of vein chemotherapy, especially for chemotherapy and embolization of peripheral tumors such as lung cancer, liver cancer, and renal cancer . The use of new techniques and new drugs has made great success. Most lung cancer was treated with bronchial artery perfusion chemotherapy, but some blood supply of lung cancer was from the arteriae intercostales, or bronchial artery originated from arteriae intercostales. Because thoracic spinal artery are more from the same origin with arteriae intercostales [5], or small branches connecting bronchial artery or arteriae intercostales with spinal artery, too high injection pressure or too fast speed during perfusion chemotherapy may cause the adverse flow of the liquid into the spinal artery causing complications, or even paraplegia [6]. Thus, angiography of bronchial artery or arteriae intercostales to find the tumor feeding artery must be accurate and careful, avoiding spinal artery by micro catheter technique. Injection pressure should be low, the speed should be slow with timely asking patients whether there is physical discomfort. After a period of perfusion, the position of the catheter and its tip should be confirmed under X-ray, low pressure and small dose angiography should be done to confirm perfusion vessels when necessary. Requirements of high operation technique and problems such as more cerebrovascular complications still exist in the interventional chemotherapy of IMT. Whole Brain Radiotherapy (WBRT) is still the most important method beyond surgical treatment, but which can appear neurologic deficit and the median survival time is no more than 6 months [7]. According to the author's experience, the cerebral angiography can determine the tumor range and one or more supplied artery branches according to tumor staining and imaging data. When metastatic tumors are small, staining may be unseen and this time the blood vessels of the metastatic tumors can be identified by angiography. Mannitol and other drugs was used to open the blood brain barrier [8], micro catheter can reach to the application site which vein chemotherapy is difficult to achieve, chemotherapy drugs cover almost all types of anticancer drugs. Thus, interventional therapy has important value in diagnosis and treatment of IMT. For well-defined IMT, interventional therapy can treat primary lesions and metastatic lesions in a surgery at the same time, also can adjust the plan according to the treatment effect and patients’ response to chemotherapy drugs with repeated treatment, prolonging the survival and improving the life quality of patients.
Micro catheter technique was more applied in interventional chemotherapy and embolization of liver cancer [9,10]. With mature technology, micro catheter technique used in the interventional treatment of uterine cancer [11] and lung neoplasms [12] are also reported. For bronchial artery angiography, the author firstly used the 5F JL 4.5 catheter and the hook in the bronchial artery opening is strong for its curvature which is conducive to the micro catheter transportation guided by micro-guide wire. Using micro catheter techniques to avoid the dangerous anastomosis between intercostal vessels and possible spinal artery is necessary and helpful [13]. But, when super selection of micro catheter is difficult and bronchial artery angiography was no dangerous anastomoses, catheter the perfusion with 5 F JL4.5 catheter is also satisfactory. The application of single micro catheter technique, and even dual micro catheter technique was more in the supplementary embolization and intracranial stent placement. Micro catheter has less damage to the cerebral blood vessel, but during the process of placing micro catheter, cerebral vascular spasm may occur and its degree depends on the operator's skill, experience and proficiency. In this research, the author used the continuous perfusion of papaverine to prevent cerebral vascular spasm. The occurrence of ischemic events and the time of perfusion chemotherapy may be related to the coagulation condition of patients, pending further study. The author's experience is that the use of a single micro catheter can be without whole body heparinization, the occurrence of ischemic events is related to the position of catheter tip. The selection of ultra-smooth micro catheter with the appropriate angle is very important, and steam shaping is not advised in order to minimize the damage of the ultra-smooth feature.
Complications such as decreased transient visual acuity, eye pain, amaurosis, or even blindness may occur after arteriae ophthalmica perfusion chemotherapy. General perfusion chemotherapy has been noted that the catheter tip is placed at the distal end of the arteriae ophthalmica, but is still in or near the small branches of internal carotid. Micro catheter technique can solve the problems such as the position of perfusion, but it should be adjusted according to the patient's situation, to prevent the side effects caused by adverse flow of chemotherapeutic drugs.
5 F catheter was placed in the second vertebral body of internal carotid to keep the support for micro catheter, while avoiding the stimulation of catheter instability during the operation for the carotid sinus. Micro catheter has good adaptability, the operation should be gentle, and the application of micro-guide wire shaping technology should reduce the stimulation of blood in the process of position [14]. Meanwhile continuous infusion of papaverine during the perfusion chemotherapy can alleviate cerebral vasospasm and expand tumor feeding artery [15]. ORR and DCR of IMT patients with single feeding artery in this paper were high, while cerebrovascular complication was high as well, suggesting that the operation of micro catheter requires a certain experience and proficiency, perioperative treatment is also very important.
The side effects of chemotherapy drugs are mainly gastrointestinal reactions and leukopenia [16]. We perfused ondansetron to prevent the occurrence of gastrointestinal reactions when the catheter passes through the mesenteric artery. According to the situation of patients, according to the appropriate symptomatic treatment was adapted to ensure the surgery go with a swing. After the operation, Chinese herbal medicine was used for strengthening immune system. Patients with high KPS before the operation had low incidence rate of side effects and fast recovery. Therefore, chemotherapy must maintain the balance of the patient's internal environment at the same time, improving the general situation of patients, which traditional Chinese medicine can be used for regulating the immune system and improving the prognosis of patients.
For the treatment of single IMT, at present, evidence-based medicine recommends the treatment “surgical excision +WBRT”. However, for the patients who refused surgical treatment, WBRT can damage the brain tissue with poor curative effect. AICT using micro catheter can accurately perfuse one or more tumor feeding arteries under the condition of identifying tumor staining and blood vessel distribution. Patients with poor short-term efficacy can be treated by radiotherapy or molecular targeted drug such as Erlotinib as early as possible [17]. AICT can reduce the size of large tumor (more than 3 cm) which are sensitive to chemotherapy, meeting the requirements of Stereotactic Radiotherapy (SRT). Thus, as a scientific and accurate treatment of IMT, AICT using micro catheter can be used alone or in conjunction with radiotherapy or surgical treatment to achieve the goal of improving the curative effect and the quality of life.
Conclusion
Micro catheter technique radically solves the intravascular administrative route of chemotherapeutic drugs. More targeted drugs chosen by the gene expression and chemosensitivity test can directly reach to the lesions through the artery using micro catheter technique which makes interventional chemotherapy is safe and effective, and the side effects of chemotherapy drugs reduced to a minimum. Good short-term efficacy and safe control of adverse reactions for the treatment of patients with advanced distant metastasis is essential for the establishment of confidence, the improvement of the compliance and the survival period, and the guarantee of living quality. Interventional chemotherapy of IMT using micro catheter technique has a reliable short-term efficacy, with minor and controllable side effects, is one of the effective options in treatment.
Acknowledgements
All data and experiments were done by my team. Here we thank Tianjin Tumour Hospital Prof. Guo and Prof. Xing support and help in the process of research. I really very much appreciate your months of guidance and help.
Funding
This work was supported in by Key support applications from Health and Family Planning Commission of Binhai New District, Tianjin, China in 2015. (No: 2015BWKZ005).
Conflict of Interest Statement
The authors declare no conflict of interest in preparing this article.
References
- Mujoomdar A, Austin JH, Malhotra R, Powell CA, Pearson GD, Shiau MC, Raftopoulos H. Clinical predictors of metastatic disease to the brain from non-small cell lung carcinoma: primary tumor size, cell type, and lymph node metastases. Radiology 2007; 242: 882-888.
- Wu YL, Zhou L, Lu Y. Intrathecal chemotherapy as a treatment for leptomeningeal metastasis of non-small cell lung cancer: A pooled analysis. Oncol Lett 2016; 12: 1301-1314.
- Ma C, Guo Z. Intracranial arterial infusion chemotherapy for lung cancer complicated by brain metastases: a clinical observation. J Interv Radiol 2011; 20: 692-695.
- Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S, Mooney M, Rubinstein L, Shankar L, Dodd L, Kaplan R, Lacombe D, Verweij J. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 2009; 45: 228-247.
- Zhang R, Jiang T. Curative effect of chemotherapy on advanced non-small cell lung cancer by bronchial artery infusion plus systemic chemotherapy. J Pract Oncol 2010; 24: 45-47.
- Hohenforst-Schmidt W, Zarogoulidis P, Stopek J, Kosmidis E, Vogl T, Linsmeier B, Tsakiridis K, Lampaki S, Lazaridis G, Mpakas A, Browning R, Papaiwannou A, Drevelegas A, Baka S, Karavasilis V, Mpoukovinas I, Turner JF, Zarogoulidis K, Brachmann J. Enhancement of intratumoral chemotherapy with cisplatin with or without microwave ablation and lipiodol. Future concept for local treatment in lung cancer. J Cancer 2015; 6: 218-226.
- Mahmood U, Kwok Y, Regine W, Patchell R. Whole-brain irradiation for patients with brain metastases: still the standard of care. Lancet Oncol 2010; 11: 221-222.
- Fortin D. The blood-brain barrier: its influence in the treatment of brain tumors metastases. Curr Cancer Drug Targets 2012; 12: 247-259.
- Wang SC, Zeng QL, Chen Y, Yang XL, Deng XW, Liang HH, Li LQ. Therapeutic effect of interventional treatment of small hepatocellular carcinoma by ultra-selective catheterization with micro catheter. J Pract Med 2012; 28: 1850-1852.
- Xu X, Chen Y, Wang Q. The application of microcatheter superselective catheterization in interventional chemoembolization for multiple hepatocarcinomas: an initial experience in 34 cases. J Interv Radiol 2012; 21: 252-255.
- Li H, Yang S, Wang Y, Zhao J. Application of microcatheter superselective catheterization in interventional treatment on primary uterine fibroids. J Med Imag 2013; 23: 1092-1094.
- Zou Z, Liu B, Zheng X, Yang J. 29 cases clinical observationof lung cancer treated by super selective bronchial artery embolization with micro catheter. Chinese J Clin Oncol Rehab 2011; 8: 82-84.
- Rad AN, Flores JI, Rosson GD. Free DIEP and SIEA breast reconstruction to internal mammary intercostal perforating vessels with arterial microanastomosis using a mechanical coupling device. Microsurg 2008; 28: 407-411.
- Yoshimura M, Hirota S, Thamamongood T, Ito N, Yamamoto S. An optimal visualization of a cerebral aneurysm without interference of other arteries by using modified double microcatheter technique during endovascular embolization. J Neuroendovasc Ther 2015; 9.
- Ghanem MA, Shabana AM. Effects of Milrinone continuous intravenous infusion on global cerebral oxygenation and cerebral vasospasm after cerebral aneurysm surgical clipping. Egypt J Anaesth 2014; 30: 73-82.
- Guo YM, Huang YX, Shen HH, Sang XX, Ma Xiao, Zhao YL, Xiao XH. Efficacy of compound kushen injection in relieving cancer-related pain: a systematic review and meta-analysis. Evid Based Complement Alternat Med 2015; 2015: 840742.
- Ma C, Guo Z. Erlotinib used for the treatment of advanced brain metastases from lung adenocarcinomas after arterial infusion chemotherapy: a clinical analysis. J Interv Radiol 2012; 21: 641-644.