Review Article - Journal of Pharmacology and Therapeutic Research (2018) Volume 2, Issue 2
Type 2 diabetes mellitus and metformin hydrochloride usage: A short review.
Gustavo Freire Petrovick*
Graduation Program in Cellular and Molecular Biology, School of Sciences, Pontifical Catholic University of Rio Grande do Sul (PUCRS), Av. Ipiranga 6681, 90619-900, Porto Alegre/RS, Brazil
- *Corresponding Author:
- Gustavo Freire Petrovick
Graduation Program in Cellular and Molecular Biology
School of Sciences
Pontifical Catholic University of Rio Grande do Sul (PUCRS)
Av. Ipiranga 6681, 90619-900 Porto Alegre/RS, Brazil
Tel: +55 51 3353.4147
E-mail: gustavo.petrovick@pucrs.br
Accepted on April 26, 2018
Citation: Petrovick. Type 2 diabetes mellitus and metformin hydrochloride usage: A short review. J Pharmacol Ther Res 2018;2(2):6-9.
DOI: 10.35841/pharmacology.2.2.6-9
Visit for more related articles at Journal of Pharmacology and Therapeutic ResearchAbstract
Diabetes mellitus is a group of disorders in the carbohydrate metabolism in which the insulin action is diminished or erased by a change in its secretion, a decrease in its activity (due to a decreased functionality of insulin sensors in the tissues) or a combination of these two factors. As the disease progresses, damage to tissues or to the vascular system can lead to severe complications such as retinopathy, nephropathy, neuropathy, cardiovascular problems, and alimentary ulceration. Diabetes mellitus can be classified into several types; however, there are two main forms: type 1 (insulindependent) and type 2 (non-insulin dependent). The most common disease of our time is the type 2 diabetes mellitus (DM2). The DM2 usually develops more in the adult age, affecting mainly the elderly and/or obese individuals. In this context, the use of metformin in the treatment of DM2 patients can be highlighted. Found in its salt form, metformin hydrochloride, it is still nowadays the drug of choice by the National Health System in South America, Europe, and North America. Its usual oral dose is 500 mg, administered two to three times a day, which can be increased gradually to 1000 mg. There are more than one thousand articles and reviewed studies reporting the efficacy of metformin in treatment and prevention of DM2. A comprehensive study called United Kingdom Prospective Diabetes Study demonstrated the efficacy of metformin in the treatment and prevention of DM2. This study evidenced metformin as safe, cost effective and corroborates other studies that define metformin as the first line of diabetes therapy.
Keywords
Diabetes mellitus, Metformin
Type 2 Diabetes Mellitus
Diabetes was first described 3500 years ago by the ancient Egyptians. One of the first clinical descriptions was made by Aretaeus, who practiced medicine in Cappadocia around 120 A.D. [1]. The term diabetes mellitus describes a metabolic disorder of multiple etiology characterized by chronic hyperglycemia with disturbances in carbohydrate, fat, and protein metabolism, resulting from failings in insulin secretion, insulin action, or even both [2].
Diabetes mellitus can be classified into several types; however, there are two main forms: type 1, also defined as insulin-dependent form of the disease, and type 2, a non-insulin dependent form. The DM2 usually develops more in the adult age, affecting mainly the elderly and/or obese individuals. However, recently due to changes in the quality of the food diet and its cultural changes, this disease is more often observed in children [3,4]. In this type of the disease, the secretion of insulin may seem normal or even excessive, but is still insufficient to compensate the insulin resistance [5].
They usually occur when the body cannot produce enough insulin or cannot use insulin effectively. Insulin is a peptide hormone that regulates the metabolism of carbohydrates and fats by promoting the absorption of glucose from the blood to skeletal muscles and adipose tissue [6,7]. The most common type of diabetes is the type 2 (DM2), also known as non-insulin dependent diabetes mellitus (NIDDM). It generally occurs in adults, but it is increasingly diagnosed in children and adolescents [6]. DM2 constitutes 85 to 95% of all diabetes cases in developed countries and has reached epidemic proportions in several nations [8,9]. In 2007, 246 million cases of diabetes were estimated in the world. A more recent report estimated that this number has risen from 108 million in 1980 to 422 million in 2014 [10]. Additionally, this study reports that in 2015, 1.6 million deaths were directly caused by diabetes. Additionally, because of inefficiency, lack of professional and material resources, the public health system in developing countries will have to face an even greater number of people with this type of disease in the future [9]. This particular type is characterized by impaired insulin secretion and reduced peripheral insulin sensitivity, in other words, the body is able to produce insulin but either this is not sufficient, or the body is unable to respond to its effects (called insulin resistance). Even though it is quite known that the pathogenesis originates from documented defects at the level of pancreatic β-cell, muscle, and liver, the causes or specific reasons for the development of these abnormalities are not completely understood [2,11-13].
For human health, as well as in financial terms, the burden of diabetes in the world is enormous, causing around 5.1 million deaths a year and taking up 548 billion US dollars in health spending in 2013 (11% of the total spent worldwide). DM2 represents a significant proportion of health care expenditures for treatment and prevention of complications [14]. In 1997, DM2 represented the major public health issue all over the world, becoming the status of a “diabetes epidemic” [8]. An estimation of the International Diabetes Federation (IDF) indicated that, in 2013, 8.3% of the adult population (around 382 million people) suffers from diabetes; and the number of people with the disease is expected to rise to 592 million in less than 25 years [6]. The burden of diabetes is not only reflected in the increasing number of people with diabetes, but also in the related growing number of premature deaths. In 2013, roughly half of all deaths due to diabetes in adults were related to people under the age of 60. In less developed regions, like Africa, this proportion climbs to over 75% [6]. Despite the public awareness, the development of innovative pharmaceutical therapies, and the implementation of new measures to improve diagnosis and treatment, diabetes persists as a cost driver in worldwide care systems [14]
Markedly, diabetes has increased alongside rapid cultural and social changes, such as aging populations, increasing urbanization, dietary changes, reduced morphological activity, and unhealthy behaviours [15]. Obesity is considered one of the main risk factors for DM2. All over the world, the diabetes epidemic is associated to the increase of obesity, due to a “westernized” lifestyle: namely changes in nutritional habits with increased intake of saturated fats, refined sugars and alcohol, reduced intake of fibres, and at the same time, reduction in morphological activity [16]. Treatment options include diet, oral antihyperglycemic agents, and insulin [11]. When dietary treatment fails and glycemic control deteriorates, some pharmacological oral treatment must be started [17]. Although dietary management is the easiest approach, at least 50% of type 2 diabetic patients require the addition of an oral antihyperglycemic agent to achieve satisfactory glycemic control [18].
Likewise, aging is becoming a risk factor for DM2 since the world population is aging and the number of elderly diabetic patients is also increasing [17]. With aging two phenomena occur: physiologic declining functions and an increase in the prevalence of diseases. Although these processes influence each other, physiologic impaired functions occur independent of illnesses [19]. In this context, the prevalence of DM2 related to elderlies is increasing and already affects 18 to 22% of people over 65 years old in United States, for example [20].
The United Kingdom Prospective Diabetes Study (UKPDS), in the year of 1999, demonstrated that DM2 can be successfully treated with a monotherapy using a single oral agent. Furthermore, this study showed improved glycemic control, irrespective of the agent used (sulfonylureas, metformin, or insulin), decreased the incidence of microvascular complications (retinopathy, neuropathy, and nephropathy) [21]. However, pharmacological treatment of DM2 in elderly patients is becoming a growing and complex problem in the clinical practice, since longevity in almost every population is increasing and is accompanied with complex physiological alterations [17]. Due to physiological heterogeneity of elderly ranges from healthy and active to very frail, clinicians’ approach to what constitutes acceptable glucose control must be carefully individualized [22]. With the growing number of effective and available drugs and drug products, drug therapy is and will continue to be an integral part of older age [23].
Metformin Hydrochloride
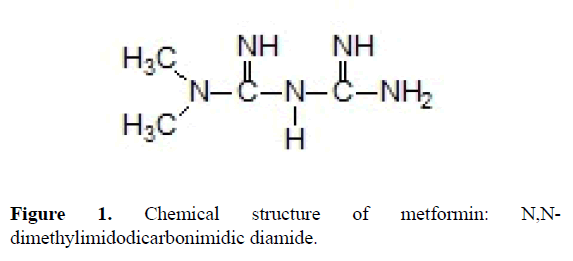
Metformin is widely used for the treatment of DM2. It is a biguanide developed from galegine, a guanidine derivative found in Galega officinalis [24]. Chemically, metformin is a hydrophilic base (Figure 1), however, is usually present in oral dosage forms in its hydrochloride salt form. Metformin HCl has acid dissociation constant values (pKa) of 2.8 and 11.5 and, therefore, exists very large as the hydrophilic cationic species at physiological pH values (>99.9%) [24]. The lipid solubility of the unionized species is low as shown by its low water-oil partition coefficient value (logP=1.43) [25]. This chemical parameter indicates low lipophilicity and, therefore, rapid passive diffusion of metformin trough cell membranes is unlikely [24]. Based on these properties, metformin HCl is defined as class III (low permeability, high solubility) by the Biopharmaceutics Classification System (BCS) [26].
Absorption from the stomach is likely to be negligible and it therefore appears that the absorption of metformin is confined largely to the small intestine with negligible absorption also from the large intestine [24]. The gastrointestinal absorption of metformin is incomplete with an absolute bioavailability of 40 to 60% (under fasting conditions) in combination with rapid elimination, and 20 to 30% of an oral dose is recovered in faeces. Interestingly, its absorption rate decreases as the dose increases, suggesting some form of saturable absorption or permeability/transit time-limited absorption [27] and negligible hepatic metabolism [28]. Passive diffusion of metformin through cell membranes is low because of the hydrophilic chemical nature of metformin. However, it is a substrate for several organic cation transporters [24]. Metformin is excreted unchanged in urine and the elimination half-life (t½) of metformin during multiple dosages in patients with good renal function is approximately 5 hours [24].
Metformin is an antihyperglycemic agent which improves glucose tolerance in type 2 diabetic patients, lowering both basal and postprandial plasma glucose levels [11]. It is also considered an “insulin sensitizer”, since it lowers glucose levels without increasing insulin secretion. Metformin also lowers endogenous glucose production in the liver [29]. The antihyperglycemic properties of metformin are mainly attributed to the suppression of hepatic glucose production, especially hepatic gluconeogenesis, and increased peripheral tissue insulin sensitivity. Although the precise mechanism of hypoglycemic action of metformin remains unclear, it probably interrupts mitochondrial oxidative processes in the liver and corrects abnormalities of intracellular calcium metabolism in insulin-sensitive and cardiovascular tissue [30]. Other proposed mechanisms of action include decreased hepatic glucose production, increased peripheral glucose disposal and reduced intestinal glucose absorption [29].
The American Diabetes Association (ADA), European Association for the Study of Diabetes (EASD), and the International Diabetes Federation (IDF) recommend metformin as first-choice treatment in all newly diagnosed patients [31,32]. Additionally, although sulfonylureas traditionally have been used as first-line pharmacological therapy for DM2 patients, many experts, as also the results of the UKPDS, suggest that, in the absence of contraindications, metformin may be the agent of first choice for diabetic patients, especially those who are overweight [1]. Metformin is also indicated for the treatment of type 2 diabetic patients whose hyperglycemia cannot be satisfactory managed by diet alone [33]. Furthermore, some studies reported the antidiabetic effectiveness of metformin in the treatment of diabetic patients over 70 years old, demonstrating its positive use within the geriatric population [17,34].
The oral dose of metformin is considered as hydrochloride salt, but all concentrations in biological fluids are expressed as the free base [24]. The initial dose is generally 500 mg, two or three times daily, or 850 mg once or twice daily. Furthermore, it can be gradually increased if necessary, at intervals of at least 1 week, from 2 to 3 g daily [5,21]. In some cases, immediaterelease metformin is administered in divided doses with meals to minimize gastrointestinal side effects. A dose of 500 mg has a low oral bioavailability, which decreases with higher starting doses [28,35,36]. As is generally recommended, metformin HCl should be administered initially at low doses in order to mitigate the adverse gastrointestinal effects. The doses should be increased to a maximum of 2.5 to 3 g daily in patients with good renal function although lower dosage may be sufficient. However, the dose of metformin HCl should be individualized because of intersubject variation in the bioavailability [24].
Conclusion
Nowadays, diabetes mellitus is still an increasing world problem that requires attention, in special the type 2 of the disease. Although there is several APIs that could be used to treat DM2, metformin HCl is still the first choice to its treatment. It is an oral antidiabetic API that has been used for more than 50 years. It still shows adequate results especially for overweight and elderly patients, when used as monotherapy.
References
- King P, Peacock I, Donnelly R, The UK Prospective Diabetes Study (UKPDS): clinical and therapeutic implications for type 2 diabetes. Br J Clin Pharmacol. 2001;48(5):643-648.
- Alberti KGMM, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus. Provisional report of a WHO Consultation. Diabet Med. 1998;15(7):539-553.
- TODAY Study Group. A clinical trial to maintain glycemic control in youth with type 2 diabetes. N Engl J Med. 2012;366(24):2247-2256.
- American Diabetes Association. Type 2 Diabetes in Children and Adolescents. Pediatrics. 2000;105(3):671-680.
- Sweetman SC. Martindale: The Complete Drug Reference, 35th edition ed. Pharmaceutical Press. 2006.
- International Diabetes Federation. IDF Diabetes Atlas, 6th edition ed. International Diabetes Federation. 2013.
- Tibaldi JM. Evolution of Insulin: From human to analog. Am J Med. 2014;127(10):S25-S38.
- Zimmet PZ, McCarty DJ, DeCourten MP. The global epidemiology of non-insulin-dependent diabetes mellitus and the metabolic syndrome. J Diabetes Complications. 1997;11(2):60-68.
- Giannella-Neto D, Gomes MB. Diabetology & Metabolic Syndrome: providing an open access future for diabetes research. Diabetol Metab Syndr. 2009;1(1):1-3.
- Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med. 2006;3(11):e442.
- Davidson MB, Peters AL. An overview of metformin in the treatment of type 2 diabetes mellitus. Am J Med. 1997;102(1):99-110.
- Bailey CJ, Turner RC. Metformin. N Engl J Med. 1996;334(9):574-579.
- Pickup JC, Crook MA. Is type II diabetes mellitus a disease of the innate immune system?, Diabetologia. 1998;41(10):1241-1248.
- Dailey G, Kim MS, Lian JF. Patient compliance and persistence with antihyperglycemic drug regimens: evaluation of a medicaid patient population with type 2 diabetes mellitus. Clin Ther. 2001;23(8):1311-1320.
- W.H.O. Prevention of diabetes mellitus: report of a WHO study group, in: W.H. Organization (Ed.). World Health Organization. 1994.
- Virally M, Blicklé JF, Girard J, et al. Type 2 diabetes mellitus: epidemiology, pathophysiology, unmet needs and therapeutical perspectives. Diabetes Metab. 2007;33(4) :231-244.
- Gregorio F, Manfrini S, Testa I, et al. Metformin treatment in elderly type II diabetic patients. Arch Gerontol Geriatr. 1996;22:261-270.
- Campbell IW. Management of type 2 diabetes mellitus with special reference to metformin therapy. Diabetes Metab. 1991;17:191-196.
- Abrass IB. The biology and physiology of aging. West J Med. 1990;153(6):641-645.
- Harris MI. Diabetes in America: Epidemiology and scope of the problem Diabetes Care.1998;21(S3):C11-C14.
- DeFronzo RA. Pharmacologic therapy for type 2 diabetes mellitus. Ann Intern Med. 1999;131(4):281-303.
- Wallace JI. Management of Diabetes in the Elderly. Clin Diabetes. 1999:17.
- Stegemann S, Gosch M, Breitkreutz J. Swallowing dysfunction and dysphagia is an unrecognized challenge for oral drug therapy. Int J Pharm. 2012;430(1-2):197-206.
- Graham GG, Punt J, Arora M, et al. Clinical pharmacokinetics of metformin. Clin Pharmacokinet. 2011;50(2):81-98.
- Pentikainen PJ. Bioavailability of metformin. Comparison of solution, rapidly dissolving tablet, and three sustained release products. Int J Clin Pharmacol Ther Toxicol. 1986;24(4):213-220.
- FDA waiver of in vivo bioavailability and bioequivalence studies for immediate release solid oral dosage forms based on a biopharmaceutics classification system. Food and Drug Administration. 2000.
- Tucker GT, Casey C, Phillips PJ, et al. Metformin kinetics in healthy subjects and in patients with diabetes mellitus. Br J Clin Pharmacol. 1981;12(2):235-246.
- Scheen AJ. Clinical pharmacokinetics of metformin. Clin Pharmacokinet. 1996;30(5):359-371.
- Hundal RS, Inzucchi SE. Metformin: new understandings, new uses. Drugs. 2003;63(18):1879-1894.
- Kirpichnikov D, McFarlane SI, Sowers JR. Metformin: An update. Ann Intern Med. 2002;137(1):25-33.
- Nathan DM, Buse JB, Davidson MB, et al. Management of hyperglycemia in type 2 diabetes: A consensus algorithm for the initiation and adjustment of therapy. Diabetes Care. 2006;29(8):1963-1972.
- International Diabetes Federation. Global guideline for type 2 diabetes: recommendations for standard, comprehensive, and minimal care. Diabetes Metab. 2006;23(6):579-593.
- Hu L, Liu Y, Tang X, et al. Preparation and in vitro/in vivo evaluation of sustained-release metformin hydrochloride pellets. Eur J Pharm Biopharm. 2006;64(2):185-192.
- Di Cianni G, Benzi L, Giannarelli R, et al. A prevalence study of known diabetes mellitus in Tuscany assessed from pharmaceutical prescriptions and other independent sources. Acta Diabetol. 1994;31(2):87-90.
- Cullen E, Liao J, Lukacsko P, et al. Pharmacokinetics and dose proportionality of extended-release metformin following administration of 1000, 1500, 2000 and 2500 mg in healthy volunteers. Biopharm Drug Disposition. 2004;25(6):261-263.
- Pentikäinen PJ, Neuvonen PJ, Penttilä A. Pharmacokinetics of metformin after intravenous and oral administration to man. Eur J Clin Pharmacol. 1979;16(3):195-202.