Research Article - Journal of Clinical Dentistry and Oral Health (2022) Volume 6, Issue 4
Marginal adaptation of class I ceramic restorations-A retrospective analysis
Ravichandran V and Pradeep S*
Department of Conservative dentistry and Endodontics, Saveetha University, Chennai, Tamil Nadu, India
- Corresponding Author:
- Pradeep S
Department of Conservative dentistry and Endodontics
Saveetha University, Chennai, India
E-mail: pradeeps@saveetha.com
Received: 27-Jun-2022, Manuscript No. AACDOH-22-67809; Editor assigned: 29-Jun-2022, PreQC No. AACDOH-22-67809(PQ); Reviewed: 14-Jul-2022, QC No. AACDOH-22-67809; Revised: 19-Jul-2022, Manuscript No. AACDOH-22-67809(R); Published: 26-Jul-2022, DOI:10.35841/aacdoh-6.4.117
Citation: Ravichandran V, Pradeep S. Marginal adaptation of class I ceramic restorations: A retrospective analysis. J Clin Dent Oral Health.2022; 6(4):117
Abstract
Introduction: Ceramic inlay is a more appealing option than metal class I or class II restorations. Their principal application is in the treatment of impaired posterior teeth with healthy buccal and lingual walls. These restorations allow you to keep your natural tooth structure while also benefiting from the mechanical advantages of contemporary adhesive technology, which can help to strengthen a weak tooth. A feasible alternative to amalgam or cast gold restoration is ceramic inlays. Materials and Methods: A total of 58 class I ceramic restoration data were extracted from Dental information archive system (DIAS) of Saveetha dental college. The ceramic Inlay restorations were analysed and graded accordingly on shade matching and marginal adaptation. Results: 70.7 % of the patients were between 20 to 35 years old. 55.2 % were Male. 36.2 % of Class I ceramic restorations were done in 37 followed by 34.5 % in 47. 44.8 % were graded as Good and 34.5 % were graded as very good. Conclusion: The ceramic inlay allows a new alternative restoration treatment for aesthetic restoration of posterior compromised teeth. For the success of any indirect restoration, it is imperative that good marginal adaptations are deemed necessary to prevent marginal leakage.
Keywords
Aesthetic consideration, Class I ceramic inlay, Marginal adaptation, Novel method Posterior restoration.
Introduction
Ceramic inlays are a more appealing option than metal class I or II repairs. Their principal application is in patients with compromised posterior but healthy buccal and lingual walls. These restorations allow you to keep your natural tooth structure while also benefiting from the mechanical advantages of contemporary adhesive technology, which can help to strengthen a weak tooth. Ceramic inlays are a good alternative to amalgam or cast-gold restorations, both of which have a lengthy track record of success in the clinic. In contrast to the demands of adhesive bonding, amalgam restorations have proven to be rather forgiving when perfect isolation is a concern. Alternative restorations must be compared to cast-gold inlays as the gold standard. The durability and strength of a well-made gold inlay are unsurpassed: they are exceedingly robust and strong, cause minimum wear on metal, and, unlike amalgam [1], are not corrosive. When superior strength is required, such as in high-load places in the dental arch, such as second molars, gold inlays remain a viable treatment [2]. When the patient's look is unimportant, gold is a reliable option, especially for larger restorations. Ceramic inlays, on the other hand, allow the dentist to obtain a perfect shade match with the surrounding natural tooth structure [3- 5]. Ceramic inlays can be nearly indistinguishable from the tooth being restored if the appropriate shade is chosen and the restoration is produced with correct translucency. Ceramic inlays have better physical qualities than direct posterior composite resin restorations, and when preparation margins are located in enamel, they have the potential for less micro leakage than amalgam or gold. When cervical margins are placed in dentin, however, existing adhesive techniques have not totally eradicated microleakage [6].
Multiple parameters influence the longevity of dental restorations such as material properties, Patient’s health status, Dentist’s experience and fabrication methods. Restorations generated with indirect methods have desirable mechanical properties and they are produced under slightly ideal conditions in Virgo conditions. Additionally, patient's increasing demand for tooth coloured posterior restorations has stimulated the improvement of indirect methods and materials for the posterior aesthetic restorations. Heat pressed technique is one of the frequently used methods for making ceramic restorations. Industrially fabricated machinable ceramics are produced for technicians use in laboratories and clinicians use for chair side applications. Digital systems such as CAD/CAM have evolved as an alternative for high temperature injection molding using the lost - wax technique.
Marginal adaptation is also crucial for ceramic inlay restorations to avoid resin cement wear and plaque accumulation. Marginal gap formations at restorations expose resin cement to the oral environment leading to resin cement wear. Marginal discrepancies cause debris and food to act as potentially irritants which might induce secondary caries and devitalisation of pulp. Moreover, an unsuitable fit of the restoration cannot be supported by the remaining tooth substance and influences the longevity of the restoration.
One of the most significant advances in dentistry has been the introduction of CAD/CAM systems. Popularity of these systems has increased significantly in the last decade due to the simplicity of their application. Some studies which examined the marginal adaptation of different ceramic inlay systems have shown acceptable results. Our team has extensive knowledge and research experience that has translate into high quality publications [7-26]. The aim of this study was to evaluate the marginal adaptation of Class I ceramic restorations.
Materials and Methods
The DIAS data of 58 Class I ceramic restorations were extracted from Dental Information Archive Software of Saveetha Dental College. The post-operative restoration photographs were evaluated and graded. Cross verification was done. The data were transferred to MS excel. They were imported to SPSS software and statistically analysed.
Results
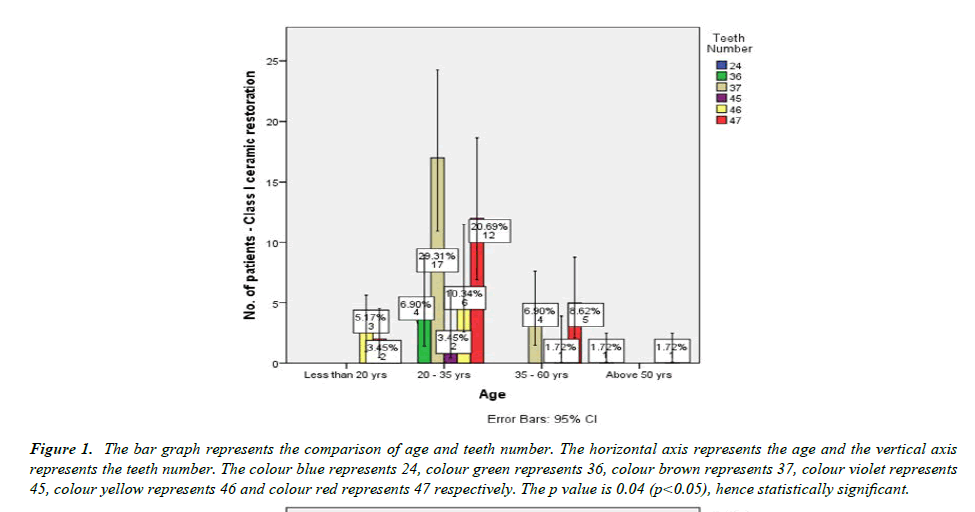
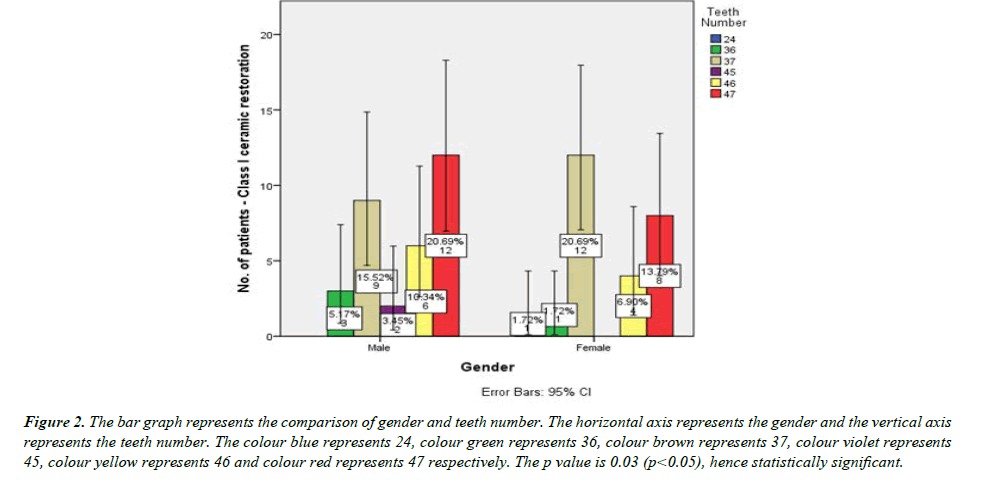
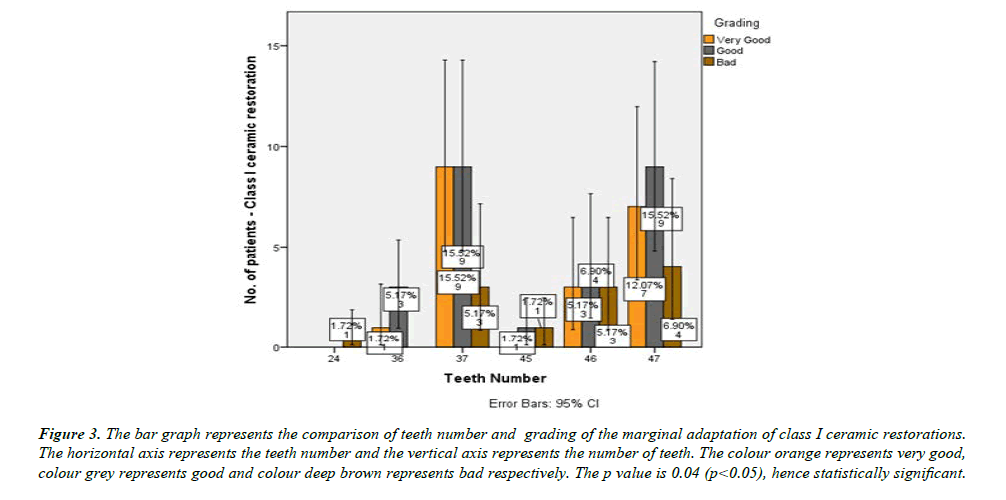
Among the total 58 patients who underwent Class I Ceramic restoration, 70.7 % (49) were 20 to 35 years old, 17.2 % (10) were 35 to 60 years old, 8.6 % (5) were less than 20 years old (Figure 1) and 3.4 % (2) were above 50 years old.55.2 % (32) were Male and 44.8 % (26) were Female (Figure 2). 36.2 % (21) of Class I ceramic restorations were done in 37, 34.5 % (20) were done in 47, 17.2 % (10) were done in 46, 6.9 % (4) were done in 36, 3.4 % (2) were done in 45 and 1.7 % (1) was done in 24.44.8 % (26) of Class I ceramic restorations were Graded as Good, 34.5 % (20) were graded as Very good and 20.7 % (12) were graded as bad in marginal adaptation (Figure 3).
Figure 1: The bar graph represents the comparison of age and teeth number. The horizontal axis represents the age and the vertical axis represents the teeth number. The colour blue represents 24, colour green represents 36, colour brown represents 37, colour violet represents 45, colour yellow represents 46 and colour red represents 47 respectively. The p value is 0.04 (p<0.05), hence statistically significant.
Figure 2: The bar graph represents the comparison of gender and teeth number. The horizontal axis represents the gender and the vertical axis represents the teeth number. The colour blue represents 24, colour green represents 36, colour brown represents 37, colour violet represents 45, colour yellow represents 46 and colour red represents 47 respectively. The p value is 0.03 (p<0.05), hence statistically significant.
Figure 3: The bar graph represents the comparison of teeth number and grading of the marginal adaptation of class I ceramic restorations. The horizontal axis represents the teeth number and the vertical axis represents the number of teeth. The colour orange represents very good, colour grey represents good and colour deep brown represents bad respectively. The p value is 0.04 (p<0.05), hence statistically significant
Discussion
The results show that the majority of the Class I ceramic restorations [70.7 %] were done in patients between 20 to 35 years old. Majority of the study population patients [55.2 %] were Male. The highest of 36.2 % of Class I ceramic restorations were done in 37 followed by 34.5 % in 47. 44.8 % of the Class I ceramic restorations were graded as Good and 34.5 % were graded as very good in Shade matching and marginal adaptation respectively. The cross comparison of teeth number and grading shows that 9 Out of 21 restorations in 37 were graded as very good and in 7 Out of 20 restorations in 47 were graded as very good. 9 Out of 21 restorations in 37 were good and in 47 as well.
The majority of the indications for cast-metal inlays apply to ceramic inlays, with the addition of the need for a tooth-colored restoration. Ceramic inlays are tooth-conserving and allow for the preservation of significant coronal tissue. Ceramic inlays are more durable than direct posterior composite resins, with better physical qualities. Direct posterior composites' strength is restricted by the limited degree of polymerization conversion [27]. However, the ceramic inlay's advantage over composite resin may be restricted by the necessity for a second appointment, the higher degree of skill necessary to administer the treatment, and the higher cost of the materials employed. Restoration wear, which is common with posterior composite resins, is rarely a clinical concern with ceramic inlays, which have comparable or even better aesthetics.
Inlays have lower retention values than full-veneer crowns, which limits their use as retainers for fixed partial dentures that are subjected to higher loads and for Fixed Dental Prostheses (FDPs) that replace several teeth. The possibility of zirconium inlays as conservative retainers for short-span FDPs has recently been described by a number of publications [28-30]. Zirconia substructures are planned to be veneered with a pressed ceramic overlay in some of these attempts, allowing adhesive luting methods.
The chosen restorative material (weaker materials require more bulk), the fabrication method, and the capacity to bond the restoration all influence the preparation design. Aesthetics, fracture resistance, and edge-strength capabilities of the chosen restorative material must also be considered by clinicians. The advantages of enamel bonding over dentin bonding, as well as the variation in bonding to different kinds of dentin and the likelihood of limited retentive form, should all be considered. Ceramics have a high brittleness. Despite tremendous advances in the creation of new and superior materials, inherent brittleness remains a limiting element that can be reduced with correct preparation design. Ceramic inlays require different preparation than cast gold inlays. Because of the bonded nature of the restoration, retention form isn't as important, and bevels aren't allowed. To enable restoration fabrication, cavosurface angles of 90° are desirable, and the preparation must have smooth-flowing margins. Many parts of traditional laboratory or chair-side inlay manufacturing are made easier by the rounded internal line angles and the buttjoint cavosurface margins. The bulk of the ceramic must be created in locations where adjacent and opposing teeth may come into contact, and adequate visual access to all prepared surfaces makes optical capture and subsequent manufacturing easier [31,32].
Indirectly, ceramic inlays can be made in a dental laboratory or in the dental office utilizing chair-side CAD/CAM technologies. Dental porcelain can be fired on a foil or refractory die system, pressed glass ceramics can be used with a lost-wax technique, cast able ceramics can be used, or the restoration can be milled from prefabricated ceramic blocks at the dentist laboratory or in the dental office. Ceramic inlays can be fabricated from a number of materials, each of which has unique advantages and disadvantages. Current choices include feldspathic porcelains, leucite-reinforced, lithium disilicate, and glass-infiltrated ceramics.
The diversity of multilayer porcelains allows a skilled ceramist and physician to achieve natural-looking Chroma, shade, hue, translucency, and surface polish. Improvements in their aesthetic features and physical properties have acted as a continuing catalyst for aesthetic material development. Ceramic and composite inlays have been compared in terms of stress distribution and flexure in a number of studies. According to finite-element modeling, composite-restored teeth have more coronal flexure, but ceramic inlays have more coronal rigidity. Composites with a low modulus of elasticity demonstrate increased tension at the dentin-bonding agent junction when compared to ceramics, implying that porcelain inlays have a lower chance of debonding [33] . The ceramic inlay should have a better long-term performance than the metal inlay. If this is the case, the ceramic inlay would be the more cost-effective option because the restoration would need to be replaced less frequently.
Conclusion
The ceramic inlay allows a new alternative for restorative treatment. This technique provides the clinician with yet another treatment option for aesthetic restoration of a compromised tooth. The system investigated offers a promising method for the indirect restoration of posterior teeth with aesthetic material but a longer observation period is necessary to substantiate the results.
Acknowledgement
The authors would like to acknowledge the support rendered by the Department of Conservative dentistry and Endodontics, Department of Aesthetic dentistry & Saveetha dental college and hospitals and the management.
Author Contribution
All the authors contributed equally to the study
Source of Funding
The present project is supported/funded/sponsored by Saveetha Institute of Medical and Technical Sciences, Saveetha Dental College and Hospitals, Saveetha University, India
Kumaran TV center and Furnitures, Attur, Salem
Conflict of Interest
The author has no conflict of interest
References
- Neme AL, Evans DB, Maxson BB. Evaluation of dental adhesive systems with amalgam and resin composite restorations: comparison of microleakage and bond strength results. Oper Dent 2000; 25: 512–519.
- Bonsor SJ. Bonded amalgams and their use in clinical practice. Dent Update 2011; 38: 222–4, 226–8, 230.
- Chin G, Chong J, Kluczewska A, et al. The environmental effects of dental amalgam. Aust Dent J 2000; 45: 246–249.
- Rowe NH, Sidhu KS, Chadzynski L, et al. Potential public health risks related to mercury/amalgam discharge from dental offices. J Mich Dent Assoc 1996; 78: 32–36.
- Shraim A, Alsuhaimi A, Al-Thakafy JT. Dental clinics: a point pollution source, not only of mercury but also of other amalgam constituents. Chemosphere 2011; 84: 1133–1139
- Jackson R. Esthetic Inlays and Onlays. Contemporary Esthetic Dentistry 2012; 469–481.
- Muthukrishnan L. Imminent antimicrobial bioink deploying cellulose, alginate, EPS and synthetic polymers for 3D bioprinting of tissue constructs. Carbohydr Polym 2021; 260: 117774.
- PradeepKumar AR, Shemesh H, Nivedhitha MS, et al. Diagnosis of Vertical Root Fractures by Cone-beam Computed Tomography in Root-filled Teeth with Confirmation by Direct Visualization: A Systematic Review and Meta-Analysis. J Endod 2021; 47: 1198–1214.
- Chakraborty T, Jamal RF, Battineni G, et al. A Review of Prolonged Post-COVID-19 Symptoms and Their Implications on Dental Management. Int J Environ Res Public Health; 18. Epub ahead of print 12 May 2021.
- Muthukrishnan L. Nanotechnology for cleaner leather production: a review. Environ Chem Lett 2021; 19: 2527–2549.
- Teja KV, Ramesh S. Is a filled lateral canal - A sign of superiority? J Dent Sci 2020; 15: 562–563.
- Narendran K, Jayalakshmi, Ms N, et al. Synthesis, characterization, free radical scavenging and cytotoxic activities of phenylvilangin, a substituted dimer of embelin. ijps; 82. Epub ahead of print 2020.
- Reddy P, Krithikadatta J, Srinivasan V, et al. Dental Caries Profile and Associated Risk Factors Among Adolescent School Children in an Urban South-Indian City. Oral Health Prev Dent 2020; 18: 379–386.
- Sawant K, Pawar AM, Banga KS, et al. Dentinal Microcracks after Root Canal Instrumentation Using Instruments Manufactured with Different NiTi Alloys and the SAF System: A Systematic Review. NATO Adv Sci Inst Ser E Appl Sci 2021; 11: 4984.
- Bhavikatti SK, Karobari MI, Zainuddin SLA, et al. Investigating the Antioxidant and Cytocompatibility of Mimusops elengi Linn Extract over Human Gingival Fibroblast Cells. Int J Environ Res Public Health; 18. Epub ahead of print 4 July 2021.
- Karobari MI, Basheer SN, Sayed FR, et al. An In Vitro Stereomicroscopic Evaluation of Bioactivity between Neo MTA Plus, Pro Root MTA, BIODENTINE & Glass Ionomer Cement Using Dye Penetration Method. Materials ; 14. Epub ahead of print 8 June 2021.
- Rohit Singh T, Ezhilarasan D. Ethanolic Extract of Lagerstroemia Speciosa (L.) Pers. Induces Apoptosis and Cell Cycle Arrest in HepG2 Cells. Nutr Cancer 2020; 72: 146–156.
- Ezhilarasan D. MicroRNA interplay between hepatic stellate cell quiescence and activation. Eur J Pharmacol 2020; 885: 173507.
- Romera A, Peredpaya S, Shparyk Y, et al. Bevacizumab biosimilar BEVZ92 versus reference bevacizumab in combination with FOLFOX or FOLFIRI as first-line treatment for metastatic colorectal cancer: a multicentre, open-label, randomised controlled trial. Lancet Gastroenterol Hepatol 2018; 3: 845–855.
- Raj R K, D E, S R. β-Sitosterol-assisted silver nanoparticles activates Nrf2 and triggers mitochondrial apoptosis via oxidative stress in human hepatocellular cancer cell line. J Biomed Mater Res A 2020; 108: 1899–1908.
- Vijayashree Priyadharsini J. In silico validation of the non-antibiotic drugs acetaminophen and ibuprofen as antibacterial agents against red complex pathogens. J Periodontol 2019; 90: 1441–1448.
- Priyadharsini JV, Vijayashree Priyadharsini J, Smiline Girija AS, et al. In silico analysis of virulence genes in an emerging dental pathogen A. baumannii and related species. Archives of Oral Biology 2018; 94: 93–98.
- Uma Maheswari TN, Nivedhitha MS, Ramani P. Expression profile of salivary micro RNA-21 and 31 in oral potentially malignant disorders. Braz Oral Res 2020; 34: e002.
- Gudipaneni RK, Alam MK, Patil SR, et al. Measurement of the Maximum Occlusal Bite Force and its Relation to the Caries Spectrum of First Permanent Molars in Early Permanent Dentition. J Clin Pediatr Dent 2020; 44: 423–428.
- Chaturvedula BB, Muthukrishnan A, Bhuvaraghan A, et al. Dens invaginatus: a review and orthodontic implications. Br Dent J 2021; 230: 345–350.
- Kanniah P, Radhamani J, Chelliah P, et al. Green synthesis of multifaceted silver nanoparticles using the flower extract of Aerva lanata and evaluation of its biological and environmental applications. ChemistrySelect 2020; 5: 2322–2331.
- Cramer NB, Stansbury JW, Bowman CN. Recent advances and developments in composite dental restorative materials. J Dent Res 2011; 90: 402–416.
- Monaco C, Cardelli P, Bolognesi M, et al. Inlay-retained zirconia fixed dental prosthesis: clinical and laboratory procedures. Eur J Esthet Dent 2012; 7: 48–60.
- Wolfart S, Ludwig K, Uphaus A, et al. Fracture strength of all-ceramic posterior inlay-retained fixed partial dentures. Dental Materials 2007; 23: 1513–1520.
- Ohlmann B, Rammelsberg P, Schmitter M, et al. All-ceramic inlay-retained fixed partial dentures: preliminary results from a clinical study. J Dent 2008; 36: 692–696.
- Bergman MA. The clinical performance of ceramic inlays: a review. Aust Dent J 1999; 44: 157–168.
- Saridag S, Sevimay M, Pekkan G. Fracture Resistance of Teeth Restored With All-ceramic Inlays and Onlays: An In Vitro Study. Operative Dentistry 2013; 38: 626–634.
- Thordrup M, Isidor F, HörstedBindslev P. A one-year clinical study of indirect and direct composite and ceramic inlays. Eur J Oral Sci. 1994; 102: 186–192.
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref
Indexed at, Google Scholar, Cross Ref