- Biomedical Research (2014) Volume 25, Issue 2
Effect of Stress on Intervertebral Disc and Facet Joint of Novel Lumbar Spine Soft Implant: Biomechanical Analysis.
Hong-liang Chen, Kai-jin Guo*, Feng Yuan and Ning DingDepartment of Orthopaedics, Affiliated Hospital of Xuzhou Medical Collage, Xuzhou, Jiangsu 221002, China
- *Corresponding Author:
- Kai-jin Guo
Department of Orthopaedics
Affiliated Hospital of Xuzhou Medical Collage
Xuzhou, Jiangsu 221002, China
Accepted date: December 02 2013
Abstract
This study was to evaluate the effect of stress on the intervertebral disc and facet joint after implantation of device for intervertebral assisted motion (DIAM). Nine fresh human lumbar (L1-L5) cadavers were studied. The stress on L3-4, adjacent intervertebral disc and facet joints was measured in four groups. The cadavers in Group 1 were measured without special treatment; the lumbar discectomy and facet joint arthroplasty without implant were performed on L3-4 in Group 2. DIAM and ISOLA screw fixation in L3-4 interspinous was carried out in Group 3 and Group 4, respectively. The stress on disc intervertebrales and facet joint of L3-4 increased after lumbar diskectomy and facet joint arthroplasty. After DIAM fixation, the stress on L4-5, adjacent disc intervertebrales and facet joint was comparable to that under the normal condition. After ISOLA fixation, the stress on disc intervertebrales and facet joint of L3-4 decreased while that on adjacent disc intervertebrales increased. DIAM fixation can efficiently reduce the undesirable increase in stress due to lumbar diskectomy and facet joint arthroplasty and decrease the risk for the degeneration of adjacent disc intervertebrales caused by spinal fusion.
Keywords
lumbar; soft implant; biomechanics
Introduction
Numerous deficiencies have become apparent currently following wide application of rigid spinal fixation. The related problems include the complexity of surgery, neurological complications, major surgical trauma, incomplete fusion of bone graft and accelerated degeneration of adjacent spinal segments [1-4]. Spinal elastic fixation, however, is an alternative intervention for patients with low back pain. In order to investigate the effectiveness of inter-spinous process implant Device for Intervertebral Assisted Motion (DIAM), a case-control biomechanical study was carried out to investigate the effect of stress on the intervertebral discs and facet joints in human cadavers.
Materials and Methods
Samples and instrument
Spinal segments (T12-S1) including interosseous membranes, discs, intervertebral joint capsules and all ligaments were obtained from 9 cadavers (middle-aged, died of acute brain injury). Psoas major muscle, bilateral sacral spine muscle and other paravertebral soft tissues were removed. After preliminary manipulation, the specimens were examined by X ray to exclude any potential abnormalities. Finally, none were abnormal. Specimens were measured, numbered and subpackaged in plastic bags and subsequently stored at -40°C.
The instrument used included WE-5 Hydraulic Universal Testing Machine (Hongshan tester factory production) and digital strain gauge YJ-14 (Shanghai Huadong Electronics Instrument Factory production).
Detection of Spinal Stress
Sample preparation
Samples were progressively thawed 2 h before experiment. Intervertebral discs at both ends of L1-5 were removed along the ligament stumps. Both the caudal and cranial ends were fixed with bone cement (poly methyl methacrylate ester) to a platform. In order to ensure the accuracy and load-up condition, both ends of the bone cement platform of all the specimens were maintained at the same height.
Piezoresistor sensor adhesion
The sensor was embedded in the simulated operation segments, the adjacent segment discs and facet joints at both sides. The embedding was done strictly according to the requirements for experimental analysis of stress. After arranging piezoresistor, glueing, patching, sealing wax and temperature compensation, the piezoresistor was linked to a resistance strain guage.
Measurements
The stress distribution of surgical segment, adjacent discs and facet joint were measured in 4 groups: 1) control group: no processing; 2) simulated surgery group: bilateral fenestration of L4-5 + hemisection of facet joint + resection of 2/3 intervertebral disc; 3) DIAM group: installation of DIAM at L4-5 (NLSI is "H"-shaped made of medical silicone coated with nylon cover, and placed between spinous processes which were fixed between upper and lower spinous process by fixing strap)(Fig 1A); 4) ISOLA group: simulated spinal fusion by installing ISOLA posterior fixation system (Johnson & Johnson)(Fig 1B).
Test conditions
A standard physiological load of 500 N was applied to specimens in three ways: graduated model, quasi-static state, and continuous load. The load was set at 15 Nm and loading velocity was 0.25 Nm/s when the lumbar spine was in the extension of 15°.
The standard load was applied before each test to assure that the creep and relaxation effect of bone were removed. Data was recorded once every 30 sec during the test. To ensure accuracy, each test was done twice. After each test, the specimens were allowed to be idle for more than 30 min’s before the next test. During the test, all specimens were covered with a normal saline containing gauze to avoid dehydration.
Statistical analysis
All data obtained were mechanical quantities of load. The initial data was error corrected to attain credibility interval and content evaluation before calculating the means and standard error. Statistical analysis was performed using SPSS version 10.0, and one way analysis of variance was employed to assess the difference between four study groups. A value of P <0.05 was considered statistically significant.
Results
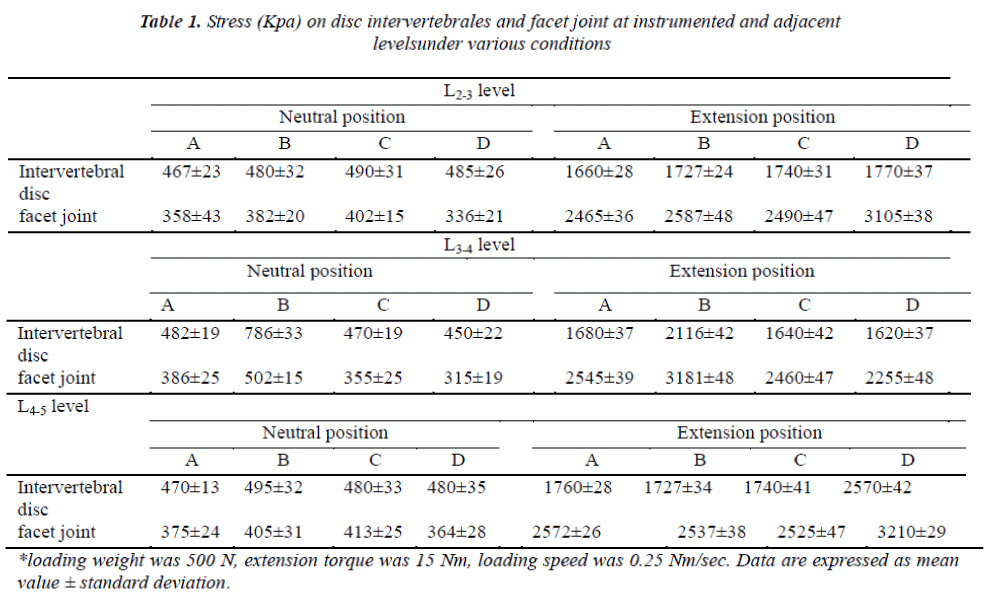
When the 1/2 lamina of lumbar specimen and facet joint were resected, the stress on the intervertbral discs and facet joint increased to the action of an axial 500 N static force. After installation of DIAM, the stress decreased to the normal level. The stress after installation of ISLOA system was lower than normal level at the operative segments. However, under the static loading, there was no significant difference in the stress on operative segments among 4 groups. When the loading weight was 15 Nm and the loading speed was 0.25 Nm/sec, the stress on the intervertebral discs and facet joint increased significantly in the posterior extension. The difference between Group 1 and 2 was significant. That is, the resection of posterior structure can obviously increase the stress on the corresponding segments. This stress could be reduced by installing DIAM. Furthermore, the stress on adjacent segments was not markedly affected. After installation of ISOLA system, the stress on the operative segments was lower than the normal level but notably higher than that on adjacent segments. The specific data are described as follows (Table 1).
Discussion
Relationship between facet joint and low back pain
Currently, no consensus has been reached on the exact cause of low back pain. However, studies on the pathogenesis of low back pain have frequently taken the facet joint into account. In 15-40% of patients suffering from chronic low back pain, there is a close relationship between facet joint disorders and low back pain [5]. Although it’s difficult to diagnose the low back pain solely caused by facet joint disorders, this kind of pain can be aggravated by over-extension and alleviated by flexing the back. Researches have shown the capsule surrounding the facet joint is innervated by nociceptor nerve fibers. The receptors are stimulated due to the change in pressure. The load on the facet joints increases at extension and the capsule is deformed, which then stimulates the nociceptor receptors in the capsule. [6,7].
The present study showed that resection of lumbar intervertebral discs and posterior structure can increase the stress on the adjacent discs and facet joints. After installing the soft implant between L3-4 spinous processes, the stress on operative segments was similar to that under the physiological condition. Installation of ISOLA system did not change the stress on the L3-4 intervertebral discs and the facet joint but significantly increased the stress on adjacent segments. These results suggest that rigid internal fixation of the spine can strengthen the operative segments but may increase the stress on adjacent segments with higher risk for degeneration in the future [8]. DIAM can protect the posterior structure of the lumbar spines from high stress. The biomechanical characteristics of the operative segments and adjacent structures are similar to those under the physiological condition. Therefore, the stability of lumbar spines is preserved [9-12]. The decrease in the harmful stress on the facet joints can slow down the degeneration process. That is, the vicious cycle of destructive interaction of disc and facet joint stopped.
Application prospect of DIAM
In the surgical installation of DIAM, only the interspinal ligament is resected. When compared with conventional surgical treatment, this surgery is an effective way to treat neurogenic claudication and lumbar spinal stenosis caused by hypertrophy of ligamentum flavum. The stress distribution of the lumbar vertebrae fixed with DIAM is similar to that under the physiological condition and the degeneration of adjacent segments is avoided [9-12]. This device can also be used with artificial nucleus replacement as it can decrease the disc stress and reduce the correlated damage. However, there are some limitations of DIAM. As a conservative treatment, DIAM only strengthens the sagittal stability of the spinal column. Spinal fusion is still recommended for spondylolisthesis and severe spinal stenosis. As this study was conducted on cadavers, further studies are still warranted. The three dimension finite element analysis would be a good option to investigate the impact of DIAM on the spinal movement.
References
- Villavicencio AT, Burneikiene S, Bulsara KR, Thramann JJ. Perioperative complications in transforaminal lumbar interbody fusion versus anterior-posterior reconstruction for lumbar disc degeneration and instability. J Spinal Disord Tech 2006; 19(2): 92-97.
- Kanayama M, Togawa D, Hashimoto T, Shigenobu K, Oha F. Motion-preserving surgery can prevent early breakdown of adjacent segments: Comparison of posterior dynamic stabilization with spinal fusion. J Spinal Disord Tech 2009; 22(7): 463-467.
- Sim HB, Murovic JA, Cho BY, Lim TJ, Park J. Biomechanical comparison of single-level posterior versus transforaminal lumbar interbody fusions with bilateral pedicle screw fixation: segmental stability and the effects on adjacent motion segments. J Neurosurg Spine 2010; 12(5): 700-708.
- Ekman P, Möller H, Shalabi A, Yu YX, Hedlund R. A prospective randomised study on the long-term effect of lumbar fusion on adjacent disc degeneration. Eur Spine J 2009; 18(8): 1175-1186.
- Manchikanti L, Singh V, Falco FJ, Cash KA, Pampati V. Evaluation of lumbar facet joint nerve blocks in managing chronic low back pain: a randomized, double blind, controlled trial with a 2-year follow-up. Int J Med Sci 2010; 7(3): 124-135.
- Yamashita T, Cavanaugh JM, el-Bohy AA, Getchell TV, King AI. Mechanosensitive afferent units in the lumbar facet joint. J Bone Joint Surg Am 1990; 72(6): 865-870.
- Avramov AI, Cavanaugh JM, Ozaktay CA. The effect of controlled mechanical loading on group-II,III, and IV afferent units from the lumbar facet joint and surrounding tissue. J Bone Joint Surg Am 1992; 74(10): 1464-1471.
- Lee CS, Hwang CJ, Lee SW, Ahn YJ, Kim YT, Lee DH, Lee MY. Risk factors for adjacent segment disease after lumbar fusion. Eur Spine J. 2009; 18(11): 1637-1643.
- Sénégas J, Vital JM, Pointillart V, Mangione P. Longterm actuarial survivorship analysis of an interspinous stabilization system. Eur Spine J 2007; 16(8): 1279-1287.
- Rohlmann A, Zander T, Burra NK, Bergmann G. Effect of an interspinous implant on loads in the lumbar spine. Biomed Tech 2005; 50(10): 343-347.
- Ryu SJ, Kim IS. Interspinous implant with unilateral laminotomy for bilateral decompression of degenerative lumbar spinal stenosis in elderly patients. J Korean Neurosurg Soc 2010; 47(5): 338-344.
- Krappel FA. [Long-term results, status of studies and differential indication regarding the DIAM implant. Orthopade 2010; 39(6): 585-594.