- Biomedical Research (2013) Volume 24, Issue 4
Case Report: An unusual observation of elastophagocytosis in a patient with cutaneous CD5+ diffuse large B cell lymphoma.
Yuji Ohtsuki1*, Yuki Matsuka1, Wakana Tanihata1, Masako Izumimoto1, Yuhei Okada1, Gang-Hong Lee2, Mutsuo Furihata2, Katsuyoshi Takata3, Tadashi Yoshino3
1Division of Pathology, Matsuyama-shimin Hospital, Matsuyama, Ehime, 790-0067, Japan
2Department of Pathology, Kochi Medical School, Kochi University, Kochi, Japan
3Department of Pathology, Okayama Graduate School of Medicine, Okayama University, Okayama, Japan
- *Corresponding Author:
- Yuji Ohtsuki
Division of Pathology
Matsuyama-shimin Hospital
Matsuyama, Ehime 790-0067,Japan
Accepted August 16 2013
Citation: Ohtsuki Y, Matsuka Y, Tanihata W, Izumimoto M, Okada Y, Lee G-H, Furihata M, Takata K, Yoshino T. Case Report: An unusual observation of elastophagocytosis in a patient with cutaneous CD5+ diffuse large B cell lymphoma. Biomedical Research 2013; 24 (4): 521-524.
Abstract
A Japanese man in his mid-60s reported having a subcutaneous mass for a period of 8 months, after which it gradually enlarged in size and was surgically extirpated. The resected tumor was 10 × 8 mm in size, and the cut surface was smooth, solid, and whitish. Histological analysis revealed the presence of medium to large lymphoid cells that had proliferated to form a solid mass. The diffuse proliferating cells stained positive for CD20, CD79a, and CD5, but were negative for CD3, CD30, and CD10, and the MIB-1 index was very high. On the basis of these findings, the tumor was diagnosed as cutaneous CD5+ diffuse large B cell lymphoma. Interestingly, detailed analysis revealed elastophagocytosis, with scattered, fragmented elastic fibers engulfed by macrophages that were intermixed with tumor cells. These macrophages were mostly multinucleated giant cells, apparently forming part of a foreign body-type reaction. Elastic fiber staining clearly revealed positively stained fragmented fibers in the cytoplasm of the macrophages, which were densely positive for CD68, in sharp contrast to the CD68-negative tumor cells. The final diagnosis was cutaneous CD5+ diffuse large B cell lymphoma exhibiting unusual elastophagocytosis. The patient’s clinical course was good, and the tumor disappeared completely after 3 cycles of rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP) therapy with radiation.
Keywords
Elastophagocytosis, CD5, Diffuse large B cell lymphoma, Cutaneous lymphoma, Macrophage
Introduction
Diffuse large B cell lymphoma (DLBCL) is a common form of B cell lymphoma with a number of subtypes, one of which is CD5-positive (CD5+) DLBCL [1]. This subtype is reported to account for 5% [2] to 7.2% [3] of all DLBCL cases and is associated with a poor prognosis and high recurrence rate [2,4]. During the histopathological investigation of a case of cutaneous CD5+ DLBCL, we noted an unusual observation of elastophagocytosis (EPC) involving multinucleated macrophages intermixed with lymphoma cells. Generally, EPC is observed in nonmalignant cutaneous diseases such as actinic granuloma [5], mid-dermal elastolysis[6], upper dermal elastolysis[7], granulomatous inflammation adjoining atypical fibroxanthoma [8], persistent reticulate erythema[9], sarcoidosis[10], cutaneous elastolytic granulomas [11], reticular erythema with focal mid-dermal elastophagocytosis [12], extragenital lichen sclerosus [13], and annular elastolytic giant cell granuloma [14]. With respect to the lymphoid malignancies, to date, only two cases of granulomatous mycosis fungoides have been reported [15,16]. Here we report a rare case of cutaneous CD5+ DLBCL exhibiting EPC.
Case Report
The patient was a Japanese man in his mid-60s who had noticed a gradually enlarging mass in his left shoulder region, which was subsequently resected. The excised mass was fixed in 10% formalin solution and embedded in paraffin. Dewaxed sections were stained with hematoxylin and eosin and Elastica van Gieson (EVG) stains.
Immunohistochemical staining was performed as described previously [17,18], using labeled streptavidinbiotin complex 2 kit/horseradish peroxidase (DakoCytomation, Kyoto, Japan) with diaminobenzidine as the substrate and specific antibodies as listed in Table. Written informed consent was obtained from the patient, and his identity has been strictly protected.
Pathological Findings
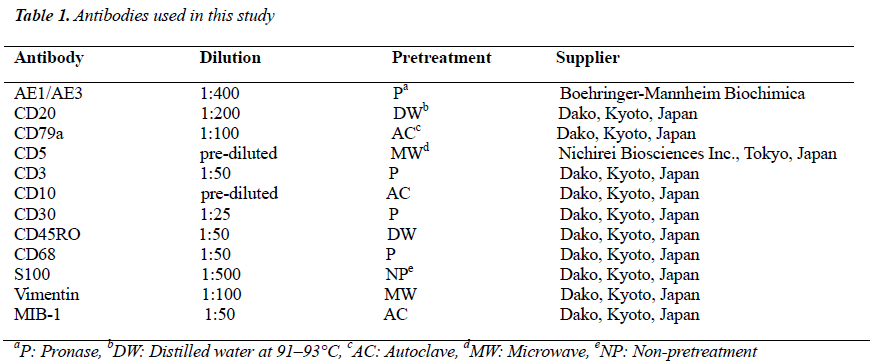
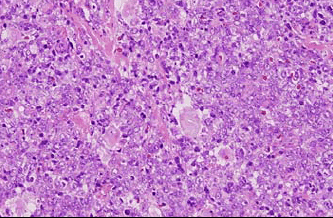
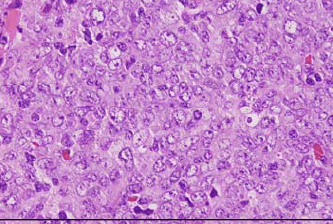
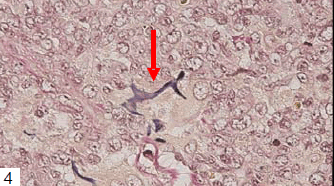
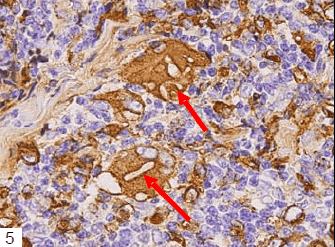
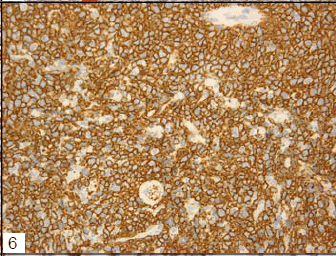
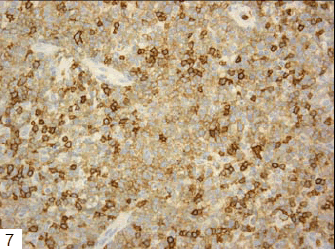
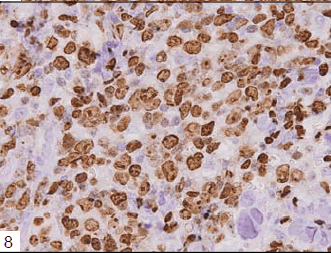
Tumor cells had proliferated to form a dense mass, consisting of medium to large-sized lymphoid cells (Figs 1 and 2). Interestingly, multinucleated macrophages engulfing elastic fibers were occasionally detected (Fig 3), which were positive on EVG staining (Fig 4). CD68, a macrophage marker, was strongly positive in the cytoplasm of these macrophages, but not in that of the fragmented elastic fibers (Fig 5). EPC were detected both within and around the tumor, as revealed by EVG staining. Tumor cells were positive for vimentin, CD79a (Fig 6), CD20, and CD5, and notably, the non-malignant T cells were negative for CD5 (Fig 7). The MIB-1 index was very high (Fig 8). Tumor cells were negative for CD3, CD10, CD30, CD45RO, and S-100 protein.
On the basis of these findings, this case was diagnosed as cutaneous CD5+ DLBCL with unusual EPC. CD5+ DLBCL associated with marked EPC is rare. After a final diagnosis had been made, the patient was treated with rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP) and radiation. The tumor disappeared completely, with no evidence of a residual tumor on a computed tomography scan, and no recurrence has been noted to date. The patient therefore has a good prognosis.
CD5 positivity defines a subtype of DLBCL with an unfavorable prognosis and a high rate of recurrence [2]. This subtype accounts for 5% of all DLBCL cases [2] and can be further divided into 2 groups depending on whether [1] it develops during the clinical course of chronic lymphocytic leukemia (Richter syndrome) or originates de novo. This subtype is generally found as an extranodal lesion in elderly female individuals and is associated with a poor prognosis[2]. It has been reported to have a cutaneous location in 5% [2] to 7.2% [3] of cases, with no lymph node involvement. Tumor cells and non-malignant, small lymphocytes were intermixed, and both stained positive for CD5. Centroblastic morphology was the most common, and CHOP therapy was effective as in the present case. Complete remission is achieved in 63% of cases, and the 5-year survival rate is 34% in Japan [2].
The significance of EPC remains unknown. It has been suggested that EPC is non-specific [10,13] and that cytokines from inflammatory cells stimulate macrophages, thereby augmenting phagocytic activity [8,19,20]. However, degenerated and fragmented elastic fibers appear to be easily taken up phagocytes, as observed in upper dermal elastolysis [5] and actinic granuloma [7], where elastic fibers disappear in the upper dermis due to EPC [5,7]. Furthermore, in pulmonary ossification [21], altered elastic fibers in blood vessels were mineralized and enriched in both iron and aluminum [21] and were easily phagocytized by macrophages.
In the present case, EPC was mainly found within the tumor mass, where the phagocytic activity of macrophages was probably stimulated by factors released by tumor cells. However, this could not be proved conclusively.
Further investigation of both neoplastic and nonneoplastic cases involving EPC is warranted.
Acknowledgements
We are grateful to Mrs. K. Matsushita and Ms. K. Takasuka for secretarial assistance.
References
- Matolcsy A, Chadurn A, Knowles DM. De novo CD5- positive and Richter`s syndrome-associated diffuse large B cell lymphoma are genotypically distinct. Am J Pathol 1995; 147: 207-215.
- Yamaguchi M, Seto M, Okamoto M, Ichinohasama R, Nakamura N, Yoshino T, Suzumiya J, Murase T, MiuraI, Akasaka T, Tamaru J, Suzuki R, Kagami Y, Hirano M,Morishima Y, Ueda R, Shiku H, Nakamura S. De novo CD5+ diffuse large B cell lymphoma:a clinicopa- thologic study of 109 patients. Blood 2002; 99: 815-821.
- Maeshima AM, Taniguchi H, Nomoto J, Maruyama D, Kim SW, Watanabe T, Kobayashi Y, Tobinai K, Ma- tsuno Y. Secondary CD5+ diffuse large B-cell lym- phoma not associated with transformation of chronic lymphocytic leukemia/small lymphocytic lymphoma (Richter syndrome). Am J Clin Pathol 2009; 131: 339-346.
- Yamaguchi M, Nakamura N, Suzuki R, Kagami Y, Okamoto M, Ichinohasama R, Yoshino T, Suzumiya J,Murase T, Miura I, Ohshima K, Nishikori M, Tamaru J, Taniwaki M, Hirano M, Morishima Y, Ueda R, Shiku H, Nakamura S. De novo CD5+ diffuse large B cell lym- phoma:Results of a detailed clinicopathological review in 120 patients. Haematologica 2008; 93: 1195-1202.
- O`Brien JP. Actinic granuloma.An annularconnective tissue disorder affecting sun- and heat-damaged (elas- totic) skin. Arch Dermatol 1975; 111: 460-466.
- Ortel B, Rappersberger K, Konrad K. Middermal elas- tolysis in an elderly man with evidence of elastic fiber phagocytosis. Arch Dermatol 1992; 128: 88-90.
- Hashimoto K, Tye MJ. Upper dermal elastolysis a comparative study with mid-dermal elastolysis.J Cutan Pathol 1994; 21:533-540.
- Sweeney EC, McDermott M. Tumour related cutaneous elastophagocytosis. J Clin Pathol 1996; 49: 81-83.
- Bannister MJ, Rubel DM, Kossard D. Mid-dermal elas-tophagocytosis presenting as a persistent reticulate ery- thema. Australas J Dermatol 2001; 42: 50-54.
- Ball NJ, Kho GT, Martinka M. :The histologic spec- trum of cutaneous sarcoidosis:a study of twenty eight cases. J Cutan Pathol 2004; 31: 160-168.
- Limas C. :The spectrum of primary cutaneous elasto- lytic granulomas and their distinction from granulomaannulare:a clinicopathological analysis. Histopathology 2004; 44: 277-282.
- Hillen U. Reticular erythema with focal mid-dermalelastophagocytosis(REMDE). J Dtsch Dermatol Ges 2008; 6: 857-860.
- Abbas O, Chatrath V, Goldberg LJ. Elastophagocytosisin extragenital lichen sclerosus.J Cutan Pathol 2010; 37: 1032-1037.
- Le Corre Y, Steff M, Prophette B, Celerier P, MaillardH. Annular elastolytic giant cell granuloma. Ann Der- matol venereal 2010; 137: 532-535.
- Kempf W, Osteeren-Michaelis S, Paulli M. istopathol-ogy Task Force Group of the European Organization for Research and Treatment of Cancer (EORTC).Arch Dermatol 2008;144:1609-1617.
- Ishida M, Hotta M, Takikita-Suzuki M, Kojima F, Oka- be H. CD8-positive granulomatous mycosis fun-goides:a case report with review of the literature.J Cu- tan Pathol 2010; 37: 1072-1076.
- Ohtsuki Y, Fujita J, Hachisuka Y, Uomoto M, OkadaY,Yoshinouchi T, Lee G-H, Furihata M, Kohno N. Immu- nohistochemical and immunoelectron microscopic studies of the localization of KL-6 and epithelial mem- brane antigen(EMA) in presumably normal pulmonary tissue and in interstitial pneumonia. Med Mol Morphol 2007; 40: 198-202.
- Ohtsuki Y, Kuroda N, Umeoka T, Watanabe R, Ochi K, Okada Y, Lee G-H, Furihata M. KL-6 is another useful marker in assessing a micropapillary pattern in carci- nomas of the breast and urinary bladder, but not the co- lon. Med Mol Morphol 2009; 42: 123-127.
- Carlson JA, Grabowski R, Chichester P, Paunovich E, Malfetano J. Comparative immunophenotypic study oflichen sclerosus: epidermotropic CD57+ lymphocytesare numerous-implication for pathogenesis. Am J Der- matol 2000; 22: 7-16.
- Romppanen U, Rantala I, Lauslahti K, Reunala T.Light- and electron microscopic findings in lichen scle- rosus of the vulva during etretinate treatment. Derma- tologica 1987; 175: 33-40.
- Ohtsuki Y, Yamanaka A, Ohyama H, Yamada E, Terada N, Fujita J, Lee G-H, Furihata M:Histochemical dem- onstration of aluminum and iron deposition in pulmo- nary bony tissues in three cases of diffuse pulmonary ossification. Histol Histopathol 2008; 23: 137-141.