Research Article - Journal of Advanced Surgical Research (2018) Volume 2, Issue 1
Our experience of 20 cases of mucocele
Chintale Sambhaji G1*, Sonali L1, Kirdak Vilas R1 , Kaleem S11 Department of Otorhinolaryngology, Maharashtra, India.
- Corresponding Author:
- Chintale sambhaji G
Department of Otorhinolaryngology
Maharashtra
India
Tel: +91 9970323030
E-mail: drsamchinto@gmail.com
Accepted Date: May 29, 2017
Citation: Chintale Sambhaji G, Sonali L, Kirdak Vilas R, et al. Our experience of 20 cases of mucocele. Adv Surg Res. 2017;1(1):29-32
Abstract
Mucocele is one of the most common benign soft tissue tumor present in the oral cavity. They are of two types - one is extravasation and second one is retention type but the majority are extravasation type [1 2] . There clinical presentation in respect to site ,size ,appearance, aetiology and symotoms are improatant to differentiate these benign lesion from other premalignant benign lesion of oral cavity there surgical excision and histopathological confirmation are necessary OBJECTIVES To study the aetiology and clinical presentation of mucucele. To study surgical management and histopathological findings of mucocele MATERIALS AND METHODS: This is hospital based prospective study carried out from march 2014 to march 2016. This study include 20 cases of mucocele presented to our ENT opd. Detail history and examination of ear nose throat of all the patients done investigated and operation done histopathological diagnosis were made . All patient were followed up over period for recurrence . RESULTS: This study includes 20 cases in which 13( 65%) are males 7 (35%) are female mean age of study is 16.6 year. Male to female ratio 1.8:1 peak age of occurance is 2nd decade of life 9( 45%)cases CONCLUSION: We conclude that there was male predominance and they were more affected in 2nd decade. We must understand the importance of histopathology examination mucocele to rule out other oral benign and premalignant malignant oral lesion .Thus, clinical knowledge of oral lesions is necessary for the correct diagnosis and for the indication of appropriate treatment.
Keywords
Mucocele, retention, cyst, granuloma.
Introduction
Oral mucoceles are kind delicate tissue masses and are clinically described by single or numerous, easy, delicate, smooth, round, translucent, fluctuant knob, which is typically asymptomatic [1- 2]. Mucoceles (muco - bodily fluid and coele - depression), by definition, are cavities loaded with bodily fluid [3]. It is the most widely recognized minor (frill) salivary organ sore influencing the all-inclusive community. Minor salivary organs are found in many parts of the oral pit aside from the gingiva. Oral mucoceles are generally arch formed amplification with in place epithelium [4]. They are delegated extravasation or maintenance type 1. The extravasation sort is a pseudo cyst without characterized dividers and are brought on because of mechanical injury to the excretory channel of the organ prompting transection or burst, with subsequent extravasation of mucin into the connective tissue stroma and are seen much of the time on lower labial mucosa, buckle mucosa and retromolar zone; they are not lined by epithelial lining [1]. The bodily fluid extravasation triggers an auxiliary [4].
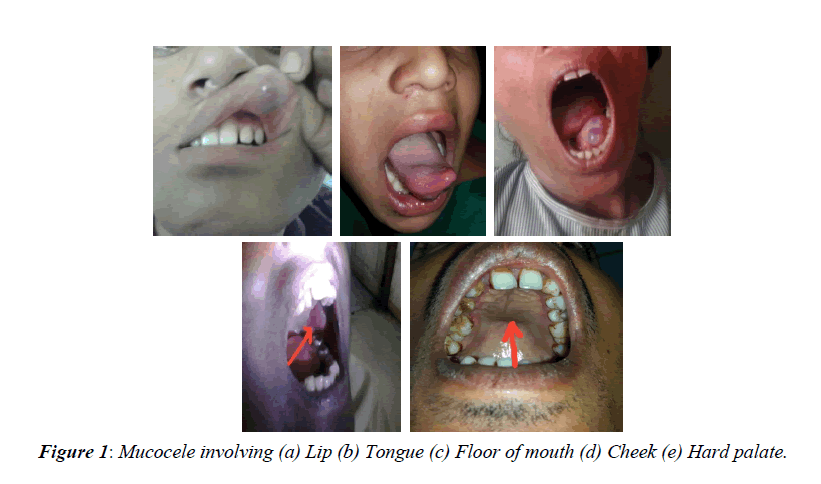
Incendiary response Numerous patients report the occasional release of gooey liquid from the sore. The maintenance sort is less normal than extravasation, ordinarily influences more seasoned people and is seen as often as possible on upper lip, hard sense of taste, floor of mouth and maxillary sinus1 [5]. In mucous maintenance wonders, bodily fluid might be held in the pipe or potentially acini subsequently of channel hindrance by sialolith or strictures [6]. The ductal narrowing can happen because of continuous mouth washing with hydrogen peroxide, antiperspirant mouth washes, attract -control toothpastes or hostile to plaque arrangements, which are conceivable reasons for bothering (Figure 1).
Materials and Methods
This study is carried out from March 2014 to march 2016 .This study include 20 subjects present to otorhinolaryngology department at our hospital. Detail history of all the subject taken through ear nose throat examination done in all patients history of trauma is asked, blood investigation done patient subjected to operation and there sample sent for histopathology to confirm diagnosis and subjects were follow up over a period for any recurrence. The permission to undertake this study was obtained from the Institutional Ethics Committee. Informed consent of all the patient and parent in paediatric patient taken. The descriptive data of these patients were evaluated .The study variables included age, gender, type, site, aetiology, symptoms of mucosae. The results were analysed by using appropriate statistical test chi square test.
Results
This study includes 20 cases in which 13 (65%) are males 7(35%) are female mean age of study is 16.6 year, male to female ratio is 1.8:1. Most common histological findings of mucocele is extravasation type 15 (75%) least common histological finding were retention 5 (25%). Peak age of occurrence is 2nd decade of life. Lower lip is more common site for mucocele 7 (35%) least common site were cheek 1(5%), submandibular 1(5%) and sub mental region 1(5%). Common symptom was difficulty in speech and chewing 10 (50%) and the history of trauma appear the major etiological factor in 18 (90%) cases. All these18 (90%) mucocele surgically excised 2(10%) were marsupialised with follow up recurrence seen in 3 (15%) case.
Discussion
Mucocele is a clinical term used to depict a swelling brought about by pooling of salivation from a disjoined or impeded minor salivary organ duct [1]. It is a self-constraining mucous containing blister of salivary organs normally happening in the oral depression, with generally quick onset and with fluctuating size [7]. The reduction in size might be because of break of the injury and consequent musing gathering or re-assimilation of salivation stores make the sore reform [5-6].
The majority of the mucocele are without the epithelial coating or are secured by granulation tissue1. Oral mucoceles can be single or numerous frequently breaking and leaving marginally difficult disintegrations that normally recuperate inside few days [8]. The length of injury is definitely not steady, from a couple days to 3 years. The clinical introduction may differ contingent upon the profundity of the lesion. The injuries are found straightforwardly under the mucous film (shallow mucocele) or in the upper sub-mucosa (established mucocele) [7]. Oral mucoceles might be found either as a liquid filled vesicle or rankle in the shallow mucosa or as a fluctuant knob profound inside the connective tissue. Unconstrained seepage of the inspisatted mucin, particularly in shallow injuries taken after by resulting repeat, may happen. The surface of long-standing sores may demonstrate fibrosis [8]. The shallow sores show up as thin-walled, somewhat blue swellings that burst effortlessly while the more profound sores are very much encompassed swellings generally secured by typical seeming oral mucosav [4]. Oral mucoceles are accepted to influence patients of any age, with the most astounding rate in the second decade of life. Adolescents and youngsters are most normally influenced by mucoceles1. Menta et al. [9] Yamasoba et al. [10] and Oliveira et al. [11] revealed that over 65% of their patients with oral mucocele were under 20 years old Our discoveries renacted these discoveries. Nonetheless, this dependably may not be valid as the asymptomatic way of the injury may defer the patients in looking for treatment. Oral mucoceles are said to emerge similarly in both the genders. The investigations of Menta et al. [9] Yamasoba et al. [10] and Oliveira et al. [11] additionally revealed comparable outcomes as of our review with male to female proportion of 1.8:1. Oral mucoceles happen in shifting areas on the oral mucosal surfaces overlying embellishment minor salivary organs. Be that as it may, they happen all the more as often as possible in specific areas. Bring down lip is most regularly influenced by mucoceles. In any case, uncommon instances of mucoceles including the upper lip, sense of taste, buccal mucosa, lingual frenum and dorsal tongue have been accounted for. Ranula assigns mucoceles situated on the floor of the mouth [5]. Our outcomes coordinated the discoveries about event of sore at lower lip and other oral locales. Shockingly our discoveries repudiated the discoveries of Menta et al [9] and Alethea et al [8]. At the point when these extravasation blisters reach out into the submandibular or submental space, they are called diving ranula. These blisters usually stretch out into the submandibular triangle, once in a while they may augment superiorly into the parapharyngeal space similar to the base of the skull. They may stretch out poorly to the supraclavicular region and upper mediastinum or posteriorly into the retropharyngeal space [12-14]. As indicated by Gupta et al., Kalra et al., and Zhao et al. concentrates the cervical ranula shows up as an asymptomatic, constantly extending mass that may vacillate in size. Most revealed ranulas are 4–10 cm in size. The overlying skin is normally in place. The mass is fluctuant, openly versatile, and nontender [15-17].
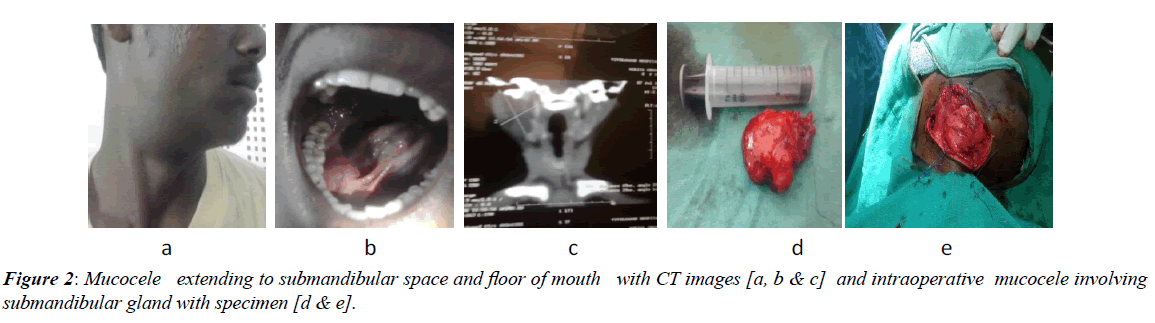
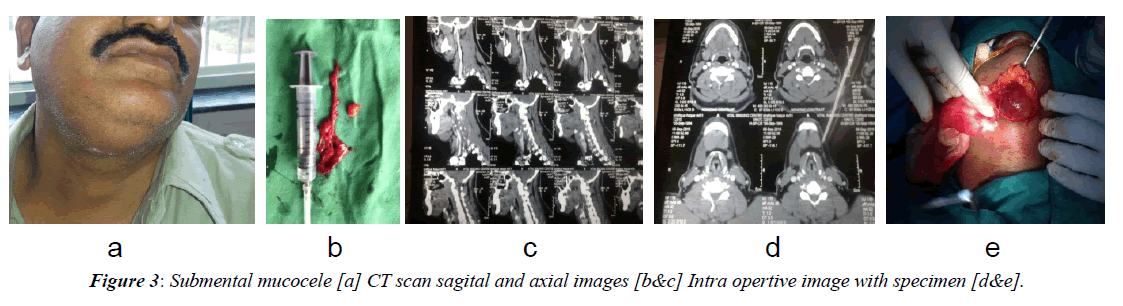
Our study include two cases of rare presesentation of mucocele which we dicussed here In one case mucocele present in right submandibular extending to submental region posterior upto angle of mandible inferiorly up to the mid thyroid region it invole right submandibular gland completely superiorly it involve floor of mouth and sublingual space on right side medialy up to parapharyngeal wall (Figure 2A) USG finding shows soft cystic swelling presenting over submandibular region and extending to submental area and floor of mouth suggesting of soft cystic bening etiology mostly mucocele CT scan also reveals soft cystic swelling approx 7 cm × 5 cm into submandibular region Extending to sumental area and parapharyngeal wall superiorly upto to floor of mouth (Figure 2B). This mucocele of submandibular gland removed surgically with their specimen (Figure 2C and 2D) and histopathological repost confirmed as etravasation mucocele (Figures 2A-2D). In another case mucocele swelling present over sub mental region extending below up to hyoid bone superiorly upto floor of mouth it was soft cystic swelling (Figure 3A). USG of this swelling suggestive of soft cystic swelling in submental region which extend up to hyoid bone and superiorly up to floor of mouth having benign aetiology CT scan shows solitary elongated well encapsulated cystic lesion arising from right submandibular gland inferior aspect approximately 6 cm × 5 cm and extending to right myelohyoid muscle (Figure 3B) lesion excised (Figure 3C and 3D) and histopathology confirmed with extravasation mucocele. In both the cases FNAC shows hick mucinous material containing scattered dense population of foamy cystic macrophages no epithelial cell lining seen suggestive of mucocele (Figures 3A-3D). The colour of mucoceles ranged from deep blue to the normal colour of oral mucosa (pink) [5]. The deep blue colour results from tissue cyanosis, vascular congestion associated with the stretched overlying tissue and the translucency of the accumulated fluid beneath. The variation in colour depends on the size of the lesion, its proximity to the mucosal surface and the elasticity of the overlying tissue [15].
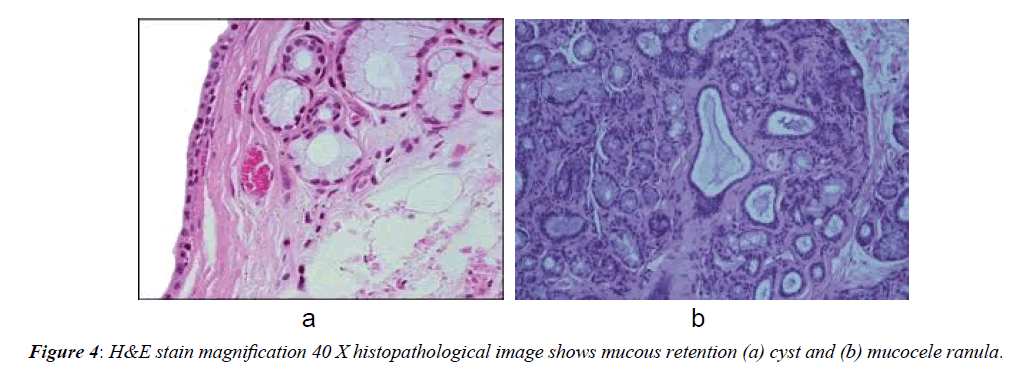
The oral mucocele of this study simulated these findings and matched with the studies of Jani et al. [15-18]. Oral mucoceles rarely cause significant problems. Discomfort, interference with speech, mastication, swallowing and external swelling may occur depending on the size and location of mucoceles [5]. All these symptoms were present in our study with varying intensity. These findings simulated with the studies of Bagán et al. [16-19]. The etiology of oral mucocele is obscure. Trauma and obstruction of salivary gland ducts are considered crucial factors. Surprisingly, in majority of our cases, we could not elicit the cause of mucocele, although lip biting and trauma history was established in few cases, which simulated the findings of Flaitz et al. [17-20]. The histopathologic aspect of this lesion ranged from acute inflammation intermingling with the mucus collection to patterns of mature lesions with scarce amounts of mucus and connective tissue fibrosis (Figure 4A and 4B).
The age, gender and oral site differ according to the type of oral mucocele 11 our study noted that 75% of the cases had extravasation type and was more prevalent in the age group of 10 to 25 years and lower lip. Thorough history taking and examination of the lesion is crucial for diagnosing oral mucocele correctly. Although diagnosis is mainly clinical, anamnesis should be carried out correctly, searching for trauma Mucoceles are mobile lesions with soft and elastic consistency depending on how much tissue is present over the lesion. Despite this fluctuation, a drained mucocele would not fluctuate and a chronic mucocele with a developed fibrosis would have less fluctuation. For specific cases, the diagnosis may require routine radiographs, ultrasonography or advanced diagnostic methods - computed tomography and magnetic resonance imaging for better visualizing the form, diameter, position and determination of the lesion origin. Oral mucocele shall be differentiated from lymphoma, oral haemangioma, oral lymphangioma, benign or malignant salivary gland neoplasms, venous varix irrigational fibroma, oral lymph epithelial cyst, gingival cyst of adults, soft tissue abscess, cysticercoids, pyogenic granuloma, etc. The superficial mucoceles may be confused with cicatricle pemphigoid, bullous lichen plan us, etc. the treatment for oral mucocele shall be either complete excision, marsupialization, dissection, cryosurgery, carbon dioxide lasers, electrocautery, intra-lesional injection of sclerosing agent OK-432 or steroid injection [5]. However, recurrence can occur and a new surgical intervention is necessary.
Conclusion
The non-neoplastic ailments of salivary organ represent an analytic and remedial test to the clinician due to close likeness of clinical introduction regardless of various etiologies, for example, reaction fiery procedures, metabolic and safe issue, contaminations and iatrogenic reactions. Consequently, clinical information of oral sores, and in addition the assurance of viewpoints identified with the aetio-pathogenesis of these sores, is essential for the right analysis and for the sign of suitable treatment.
References
- Davies PH, Benger JR. Foreign bodies in the nose and ear: a review of techniques for removal in the emergency department. J Accid.Emerg. Med.2000;17:91-4.
- Kalan A, Tariq M. Foreign bodies in the nasal cavities: A comprehensive review of the aetiology, diagnostic pointers, and therapeutic measures. PostgradMed.J. 2000;76:484-7.
- Peridis S, Athanasopoulos I, Salamoura M, Parpounas K, Koudoumnakis E, Economides JC. Int J PediatrOtorhinolaryngol. 2009;73:205-8.
- 4.Das SK. Aetiological evaluation of foreign bodies in the ear and nose. J Laryngol Otol.1984;98:989-91.
- 5.Gregori D, Salerni L, Scarinzi C, et.al. Foreign bodies in the nose causing complications and requiring hospitalization in children 0–14 age: Results from the European survey of foreignbodies’ injuries study. Rhinology. 2008;46:28-33
- 6. Kuzy FD, Korbich M. Foreign body in nasal cavity. Oral Surg Oral Med Oral Pathol.1982;54:254.
- 7. Thawley SE, Ferriere KA. Supernumerarynasal tooth. Laryngoscope.1977;87:1770-3.
- 8. Baluyot ST. Foreign bodies in the nasal cavity. In: Paparella MM, Shumrick DA, eds. Otolaryngology. 1980; 2009-16.
- 9. Cheng PT, Prizker KP, Richards J, et al. Fictitious calculi and human calculi with foreign nuclei. Scanning Microsc.1987; 12025-32.
- 10.Yeung, K.H. Intranasal tooth in a patient with a cleft lip and alveolus.Cleft Palate Craniofac J.1996;33: 157-9.
- 11. Kohli GD, Verma PL. Ectopic supernumerary tooth in the nasal cavity. J Laryngol Otol.1970;84:537-8.
- 12. Lee FP. Endoscopic extraction of an intranasal tooth: a review of 13 cases, Laryngoscope 2001;111:1027-31.
- 13. Carver DD, Peterson S, Owens T.Intranasal teeth: a case report. Oral Surg. Oral Med. Oral Pathol.1990;70: 804-5.
- 14. Nastri AL, Smith AC.The nasal tooth.Case report. Aust Dent. J. 1996;41:176-7.
- 15. Medeiros AS, Gomide MR, Costa B, et al. Prevalence of intranasal ectopic teeth in children with complete unilateral and bilateral cleft lip and palate.Cleft Palate Craniofac. J. 2000;37:271-3.
- 16. Werman HA. Removal of foreign bodies of the nose,Emerg Med Clin North Am. 1987;5:253-63.
- 17. Oh TH, Gaudet T. Acute epiglottitis associated with nasal foreign body: occurrence in a 30-month-old girl. ClinPediatr. 1977;16:1067-8.
- 18. Sarniak AP, Venkat G. Cephalic tetanus as a complication of nasal foreign body. Am J Dis Child 1981;135:571-2.