- Biomedical Research (2014) Volume 25, Issue 4
Ossification of the transverse atlantal ligament in ankylosing spondylitis- A case report
Zhen Zhang#, Zhonghan Liu# and Jianguang Zhu*Department of Spine Surgery, East Hospital, Tongji University School of Medicine, Shanghai 200120, China
#Zhen Zhang and Zhonghan Liu contributed equally
- *Corresponding Author:
- Jianguang Zhu
Department of Orthopedics, East Hospital
Tongji University School of Medicine
150 Jimo Road, Shanghai 200120, China
Accepted date: July 18 2014
Abstract
Ossification of the transverse atlantal ligament (OTAL) is rarely reported in literature. We describe a case of OTAL complicated with ankylosing spondylitis (AS). Patient’s history, physical examination, radiographic evaluation and nonsurgical interventions are examined. Relevant literature is also reviewed. On systemic examination, the patient was complicated with ossification of ligamentum flavum and posterior longimental ligament in the thoracic spine. Since the symptom of cervical spine was mild, the patient was treated with decompression laminectomy of the thoracic spine firstly. OTAL may also occur in AS patient because of its clinicopathological characteristics. Conservative treatment plays an important role in the treatment of some cases of OTAL.
Keywords
ossification; transverse atlantal ligament; ankylosing spondylitis; etiology; therapy
Introduction
Ossification of the transverse Atlantal ligament (OTAL) is rarely reported in the literature. The real cause of OTAL is still unclera. Because of large spinal canal space at atlas and axis, most of the cases can be treated. Here, we report one OTAL patient complicated with ankylosing spondylitis (AS), which has rarely been reported in literature.
Case Reports
A 64-year-old man, who was diagnosed with AS 30 years ago, complained of lower extremity weakness and clumsiness for 8 months. A gait disturbance grandually developed in 3 months.
On examination he had hyperactive deep tendon reflexes in lower extremity and a positive Hoffmann’s sign in his left hand. But sensation and motor function are normal in upper extremity.
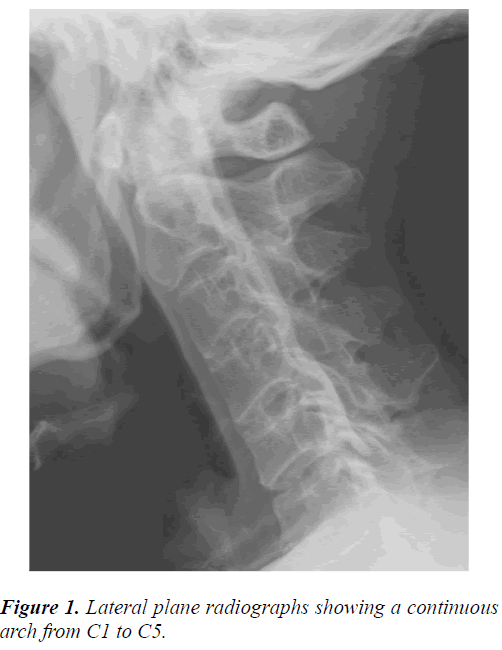
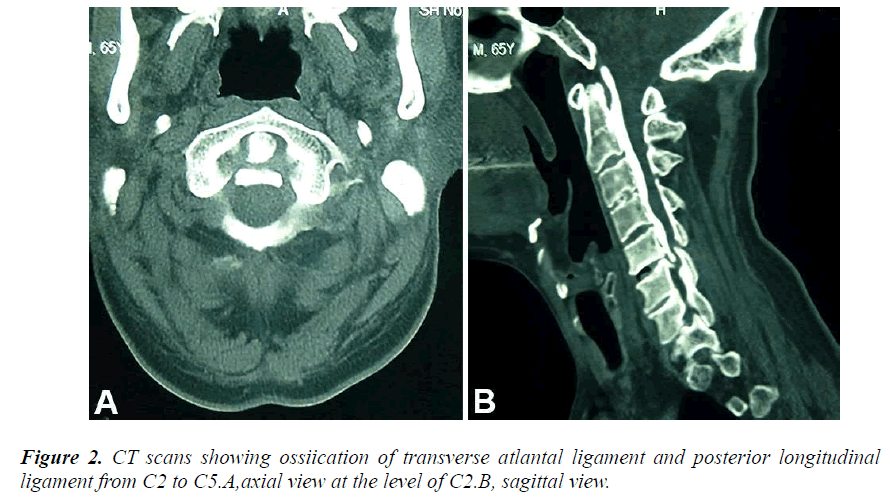
Lateral plain radiographs of the cervical spine revealed a continuous arch from C1 to C5 (Figure 1). Plain radiographs of pelvic revealed disappearance of bilateral sacroiliac joint space. Axial and sagittal CT scans revealed significant ossiication of transverse atlantal ligament and posterior longitudinal ligament from C2 to C5 (Figures 2A, B). Ossification of ligamentum flavum and posterior longimental ligament were also found in the thoracic spine. Since the symptom of cervical spine was mild, the patient was treated with decompression laminectomy of the thoracic spine firstly.
Discussion
OTAL was firstly reported by Wackenheim in 1978 [1]. Although it has rarely been reported in literature, but as described by Wang that they encounted 2 cases in one month [2], the real incidence may not be so scarce and needs further investigation. It is essential for us to take a routine holospine CT scan in the patient with spinal ligament ossification to find the possible ossification of the transverse atlantal ligament and other vertebra. We should also recognize the low density signal behind the dens in MRI. Causes of OTAL are still unclear, the possible reasons may include calcium phosphate alterations, dysmetabolic syndrome, diabetes mellitus, obesity, at lantooccipital malformation, atlanto-axial ligament injury, fluorosis and spinal ligament ossification, etc [2-4].
Calcification of the transverse atlantal ligament in rheumatoid arthritis had been reported by Castor [5], but OTAL in AS was rarely described in English literature. AS is a chronic inflammatory disease of the axial skeleton, with variable involvement of peripheral joints and nonarticular structures. Inflammation of AS originates in the the anatomical zone where tendons, ligaments, and capsules insert onto the underlying bone [6]. Because there are several ligaments and synovial tissue around atlantoaxial region, and the transverse atlantal ligament attaching on both side to a small tubercle on the medial surface of the lateral mass of the atlas, so destruction of ligaments, cartilage and bone may occur around this area in AS patients [7]. In the late stage, the fibrous tissue in the destructive area was replaced by fibrocartilage and bone [8], and therefore syndesmophyte and ossification may be observed there. This may be the possible pathomechanism of OTAL in AS.
It is difficult to distinguish between calcification and ossification of TAL, confirmation needs histopathological examination. Normally ossification usually originates bilaterally of TAL and calcification originating centrally [9]. Calcification can reduce in the size with the administration of anti-inflammatory drug [10,11]. If a consecutive dense string is also found in the other cervical spine, it always implies the existence of ossification.
Since the sagittal retrodental space has been reported as 16 to 25 mm at the level of the atlas [4,12], the spinal canal space at atlas and axis is usually large enough even with OTAL, Patients suffering from OTAL can be asymptomatic or only have mild symptoms, and being treated. The surgical indication for OTAL is in accordance with that for cervical OPLL [13], which means progressively moderate to severe myeloradiculopathy that is refractory to conservative treatment. Posterior decompression is mostly used and surgical outcomes seem to be encouraging [3,14-16].
Conclusion
One rare case of ossification of the transverse atlantal ligament in is reported. OTAL may also occur in AS patient because of its clinicopathological characteristics. Symptom caused by ossification of the transverse atlantal ligament may not be so serious and conservative treatment may be adapted firstly.
References
- Wackenheim A. [Ossification of the transverse ligament. Two observations (author's transl)]. J Radiol Electrol Med Nucl 1978; 59: 413-414.
- Wang W, Kong L, Zhao H, Jia Z. Ossification of the transverse atlantal ligament associated with fluorosis: a report of two cases and review of the literature. Spine (Phila Pa 1976) 2004; 29: E75-78.
- Hayashi T, Hirose Y, Sagoh M, Murakami H. Ossification of transverse ligament of the atlas associated with atlanto-axial dislocation--case report. Neurol Med Chir (Tokyo) 1998; 38: 425-428.
- Hinck VC, Sachdev NS. Developmental stenosis of the cervical spinal canal. Brain 1966; 89: 27-36.
- Castor WR, Miller JD, Russell AS, Chiu PL, Grace M, Hanson J. Computed tomography of the craniocervical junction in rheumatoid arthritis. J Comput Assist Tomogr 1983; 7: 31-36.
- Carter S, Lories RJ. Osteoporosis: a paradox in ankylosing spondylitis. Curr Osteoporos Rep 2011; 9: 112-115.
- Hunter T. The spinal complications of ankylosing spondylitis. Semin Arthritis Rheum 1989; 19: 172-182.
- Appel H, Loddenkemper C, Miossec P. Rheumatoid arthritis and ankylosing spondylitis - pathology of acute inflammation. Clin Exp Rheumatol 2009; 27: S15-19.
- Tsuruta W, Yanaka K, Okazaki M, Matsumura A, Nose T. Cervical myelopathy caused by hypoplasia of the atlas and ossification of the transverse ligament--case report. Neurol Med Chir (Tokyo) 2003; 43: 55-59.
- Kobayashi Y, Mochida J, Saito I, Matui S, Toh E. Calcification of the alar ligament of the cervical spine: imaging findings and clinical course. Skeletal Radiol 2001; 30: 295-297.
- Bouvet JP, le Parc JM, Michalski B, Benlahrache C, Auquier L. Acute neck pain due to calcifications surrounding the odontoid process: the crowned dens syndrome. Arthritis Rheum 1985; 28: 1417-1420.
- Nagashima C. Cervical myelopathy due to developmental stenosis of the cervical spinal canal: the sagittal diameter of the spinal canal. Neurol Surg 1973; 1: 163-171.
- Tang JG, Hou SX, Shang WL, Wu WW. Cervical myelopathy caused by anomalies at the level of atlas. Spine (Phila Pa 1976) 2010; 35: E77-79.
- Sasaji T, Kawahara C, Matsumoto F. Ossification of transverse ligament of atlas causing cervical myelopathy: a case report and review of the literature. Case Rep Med 2011; 2011: 238748.
- Shoda N, Anamizu Y, Yonezawa N, Ishibashi H, Yamamoto S. Ossification of the posterior atlantoaxial membrane and the transverse atlantal ligament. Spine (Phila Pa 1976) 2005; 30: E248-250.
- Perera S, Davis CH, Gupta RC. Spinal cord compression caused by ossification of the transverse ligament of the atlas. Br J Neurosurg 1995; 9: 787-788.