Review Article - Biomedical Research (2017) Volume 28, Issue 8
Mild cognitive impairment in idiopathic Parkinson's disease without dementia
Hurtado Gonzalez CA1,2*, Ladera V3, Perea MV3 and García R31Department of Neuropsychology, Faculty of Psychology, Cooperative University of Colombia, Cali Branch Campus, Colombia
2Department of Neuroanatomy, Faculty of Medicine, Libre University, Cali Branch Campus, Colombia
3Departament of Basic Psychology, Psychobiology and Behavioural Sciences Methodology, Universidad de Salamanca, Spain
- *Corresponding Author:
- Hurtado-Gonzalez CA
Faculty of Psychology
Professor of Neuropsychology
Cooperative University of Colombia
Cali Branch Campus, Colombia
Accepted date: January 9, 2017
Abstract
Mild Cognitive Impairment (MCI) is a non-motor common symptom of idiopathic Parkinson's disease (PD) without dementia. Different studies have shown that the MCI is a strong predictor for dementia in advanced clinical stages. Early and timely identification of the MCI in PD allows to generate new lines of treatment, specifically, Neurorehabilitation, functional techniques, tended to improve the quality of life for people diagnosed with PD. It was found that individuals had deficits to retain stimuli in a time given (sustained attention), inability to consolidate information and new learning, as well as alterations in executive functions and visuospatial functioning. New lines of research should not only focus on defining MCI. Non-pharmacological treatment options are a scientific trend that will slow down the disease and improve emotional, individual, and family aspects of people with PD as far as possible.
Keywords
Mild cognitive impairment, Parkinson’s disease, Initial stages, Functional neurorehabilitation
Introduction
Idiopathic Parkinson's disease without dementia (PD) is a neurodegenerative pathology characterized by motor alterations (bradykinesia, rigidity, tremor resting and postural instability), non-motor alterations (cognitive impairment, depression, anxiety, apathy, constipation, sleep alterations, sensory alterations, behavioural alterations among others) that directly and negatively impact on the quality of life of the people who suffer from it [1].
Clinical tests for Mild Cognitive Impairment (MCI) in PD arise from alterations in focal type to clinical stages of dementia [2]. PD patients in early stages present different cognitive alterations that affect functional family dynamics and the quality of life of patients and their immediate caregivers [3,4]. Clinical pictures of dementia are associated in later stages of the disease [5], unlike MCI which is common in the early stages of the disease, but they are studied as risk factors for the progress they may have in dementia [5,6].
The recognition early MCI offers the possibility of generating therapeutic intervention targets at the level of functional Neurorehabilitation plans, which purpose is to slow down the progression of the disease and reduce its emotional impact.
This article aims to describe the common cognitive disorders in patients suffering from PD without dementia at early stages.
Method
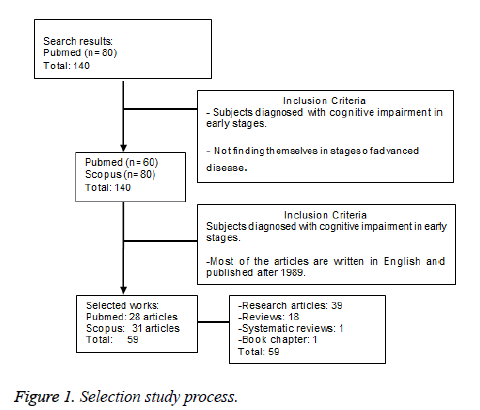
Fort the preparation of this review primary references have been used such as 39 research articles aimed to study cognitive mild impairment in PD without dementia, 18 review articles, 1 systematic review and 1 chapter of a book. The search of the information is held in PubMed and Scopus databases. The initial search was carried out using key words (mild cognitive impairment, EP, initial stages, functional Neurorehabilitation), obtaining a total of 220 references. Summaries of these works were analysed and 100 were selected. Then, those works that met the criteria set out in Figure 1 were selected. There was total of 59 (Figure 1).
Mild cognitive impairment in the idiopathic Parkinson disease without dementia
The variability of the cognitive impairment in PD is given from 20% and 57% at the early stages [7-9]. The clinical profile of cognitive impairment in PD, is often difficult due to the heterogeneity shown in the disease by clinical, pathophysiological, neuropsychological and biochemical commitment that makes unclear the etiology of cognitive deficits at present [10].
Different studies [7-9] indicate the presence of heterogeneous cognitive disorders in patients with idiopathic PD without dementia. Cognitive domains that are usually damaged are: tasks of sustained attention, memory [11], executive functions [12,13] memory, and visuospatial functioning [14].
The pathology of MCI in PD is confusing and contradictory [15,16]. Different studies indicate that low cognitive performance in subjects with PD is related to different cerebral dysfunction [16], and a reduction in the volume of gray matter in medial temporal areas, which have as main function the elaboration of new processes of learning [16].
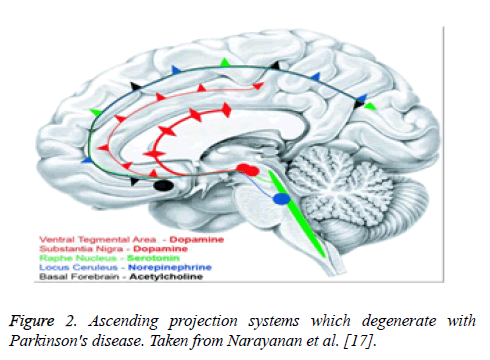
Other studies have shown [17,18] abnormalities or a series of dysfunctions in different systems of neurotransmission such as noradrenaline, serotonin, and dopamine (upward projection systems) (Figure 2), limbic system, states of neuroinflammation, apoptosis and different cortical areas that are likely to progress to clinical stages of dementia and worsening of cognitive functioning in individuals with PD idiopathic.
Figure 2: Ascending projection systems which degenerate with Parkinson's disease. Taken from Narayanan et al. [17].
Some studies [19,20] show alteration in fronto-striatal circuits. Degeneration occurs in the early stages, with dysfunctions in the striated nucleus and the neocortex, areas that are related to the inability that individuals with PD have to plan and perform tasks that involve greater cognitive flexibility.
For this reason, it is necessary to conduct investigations focused on identifying and analysing the brain areas that are most vulnerable in the early degeneration of PD. Likewise, it is vital to study the role of biomarkers that are associated with cognitive decline in PD. This will allow establishing patterns of systematic analysis that give Neurorehabilitation functional lines as a result, in order to improve the quality of life of patients [21].
MCI in patients with idiopathic PD without dementia is often under-diagnosed because of the subtle way it appears in incipient states of the pathology. Different alterations in tasks of sequencing, organization, direction, visuospatial and visuoconstructive skills, as well as problems in tasks of sustained attention, are related to dysfunctions in the frontalsub cortical circuits, reduction of gray matter, basal ganglia cortical and subcortical atrophy [22].
MCI in PD is kept being investigated, especially at early stages of the disease. The heterogeneous character of the disease has not allowed establishing a Neuropsychological profile according to the etiopathogenic picture of the pathology, especially in initial stages [23].
Attention
The inability to perform more complex tasks and those of sustained attention, are present in subjects with PD, due to the decline of the executive functioning and the slowing on the motor cardinality of pathology.
Different studies [24] show that individuals in the early stages of PD also have deficits in selective attention tasks, associated with dysfunctions in the caudate nucleus, the pre frontal cortex, and the decrease of dopaminergic projections of the brainstem towards cortical areas and basal ganglia [25].
Another study [5] has found that patients have an inability to process their thinking. This slowing is due to the aortic which does not respond to the diversity of stimuli. This is also a result of the problems that individuals have to organize and plan Metacognitive strategies that allow them to be focused on the beginning and attainment of an external stimulus.
The found thing so far indicates that there is a loss of cognitive flexibility that does not allow individual to elaborate for immediate action plans that require strategic or Meta-cognitive solutions [5].
Studies on attentional processes in idiopathic PD without dementia are not conclusive, since different works [26] point out that the control of the states of mind l and attention are not altered in the early stages of PD.
Memory
Similar to attention and other cognitive domains, memory presents a heterogeneous profile that goes from the normality of memory processes to a deterioration of processing and consolidation of the information [27,28]. Different studies have shown that individuals with idiopathic EP without dementia have disability in operational and episodic memory tasks as well as procedural memory [11].
Apparently, the ability to store and consolidate new information is not altered [11]. Free and delayed recall is affected, possibly associated with the volumetric reduction of the cortical gray matter at the level of the right parietal lobe [29,30]. It is different for recognition, which apparently is not altered since they are related to a dysfunction of the cortical nigro-striatal-thalamus circuit that interconnects the associative striatum with the pre frontal dorsolateral cortex [31].
Other studies have pointed out that the deficit of dopamine level mesocortical is associated with memory impairment in early stages of PD [17], also due to a disruption of cortical cholinergic function [32].
Alterations of memory in early stages are often related to a secondary impairment of attentional processes and cognitive flexibility (Executive function) [33].
In the same way, patients with EP show problems in prospective memory tasks, related to dysfunctions in the temporary medial lobe, basal ganglia, cortical areas and neural circuits of the spline body [34].
Other studies [35] have found changes in the entorhinal cortex and hippocampal formation, brain areas that are related to the processing, consolidation, and evocation of the information [27,28].
It is necessary to have into account that not all the components of the memory are found committed [28]. Other research has shown that memory as cognitive function in PD is not altered in a general way. The heterogeneity of the disease makes different research results to be highly variable, since many individuals retain skills for activities of procedural type [34].
Currently, the research is focused on determining the Neuropsychological profile in patients with EP in initial stages, hoping that their results can show a greater and systematic approach to the cognitive deterioration of the pathology, despite the heterogeneity shown in each one of the stages.
Executive functions
Executive functions include a diversity of processes that aim to organize, plan and direct the immediate conduct towards a specific objective [36]. Inhibition, initiation and task change processes are part of the Executive functioning of human behavior. Alterations in these cognitive domains are related to the clinical Neuropsychological profile shown in patients with idiopathic PD without dementia [13].
PD patients in early stages often present difficulties in motor planning, deliberate action, efficient implementation and initiation [12]. Some studies [12,13,37,38] indicate that the deterioration of the executive functions in EP is due to dysfunction of dopamine in the pars compact [13,38] causing alterations at the level of the cerebral cortex and the basal ganglia [39-43].
Data from different studies [44] demonstrate that the verbal fluency is affected by the evolution or the deterioration that generates disease. Others [45] have pointed out having not found these functions altered, in comparison with control subject groups. So this leads to infer that the heterogeneity of PD plays an important role in the pathophysiology of the disease and at the time of analysing the data.
The difficulty in tasks of function Executive is related to emotional alterations like depression [46,47] that as emotional alteration impacts on the cognitive performance of the subject with EP; apathy [39,41,43] which influences on the deterioration of initiation and sequencing tasks. Anxiety is not related to the deterioration of Executive functions. However, in a Foster study [48], it was found that patients in early stages of EP showed alterations to perform tasks of operational memory, possibly due to dysfunctions in the lobe front, affecting the elaboration of an organized and directed behavior.
Other [49,50] studies have found commitment of the prefrontal cortex, the basal ganglia, the medial temporal system and the entorhinal cortex in motor planning, sequencing and change of task and initiation tasks.
So far it is known that the executive functions are the most affected cognitive domain in people with idiopathic PD without dementia, and they are an excellent predictor to identify and diagnose clinical pictures of dementia in the medium or long term [51]. Functional Neurorehabilitation techniques not only improve the quality of people's lives but also slow down the process of neurodegenerative pathology.
Visuospatial functioning and visuoconstructive skills
Visuospatial functioning in subjects with idiopathic PD without dementia plays an important role, since the executive dysfunction showed by this type of patients, is associated with the disability that individuals have to integrate responses that require a greater complexity in higher psychological functions, especially those where the frontal lobe [52,53] is involved.
In the early stages of PD, subjects with this disease experience difficulty to perform tasks that involve synthesis and analysis of visual stimulation process [54]. Also, it has found difficulty in processing or face recognition, related to possible malfunctions in the visual cortex, Hippocampus and temporoparietal junction [55].
Other studies have found abnormalities in the frontal lobe, neocortical grey substance, cortico-striatal-thalamic circuit and primary visual areas [14,40].
The area that shows greater commitment in alterations of the visuospatial operation is the prefrontal cortex. Its main function is to integrate the information that comes from the outside [40,53].
It has been found that the deficit in visuospatial functioning is associated with declining those subjects with PD show in the theory of mind. It seems that there is a mediator of tasks as a predictor of a visuospatial effect on cognitive States or theory of mind. This could explain why PD patients show incipient alterations in executive domains [56].
In relation to the visuoconstructive skills, different studies [57-59] show that this type of disturbance is not frequent in the early stages. However, other data have pointed out that some patients tend to present disability to perform situations at perceptual and motor level [57]. The heterogeneity of the disease shows a significant role for the discrepancy that occurs in the Neuroanatomical correlation and its Neuropsychological profile, especially in the early stages of the disease.
Conclusions
Mild Cognitive Impairment in PD is currently one of the most important non-motor symptoms, since it is considered a predictor of dementia in advanced stages of the disease. Investigations should focus their efforts on carrying out works or multidisciplinary studies that have as objective the patient and the family, with the patient because it will allow to improve the quality of life and the slowing down of the disease through functional neurorehabilitation techniques, and with the immediate caregiver, the prevention of Burnout Syndrome.
Data obtained by different research [2,5,12] demonstrate that mild cognitive impairment is a common feature in initial stages of PD. It is important that studies are not only limited to the research of this non-motor disorder in them. It is necessary to include aspects of non-pharmacological treatment that cover different individual, social and family dimensions that allow intervening the consequences given in the initial stages of PD. Therefore, we detail the following suggestions:
1. Investigations and interventions on PD should be focused on early detection of MCI with the aim of generating functional Neurorehabilitation strategies that slow down the disease.
2. The systemic Neuropsychological evaluation will establish criteria of diagnosis that allow rating MCI in subjects with PD in early stages.
3. The intervention of the family, especially immediate caregivers is going to generate that PD does not destabilize the social and family structure of each one of the patients.
It is expected that the thing exposed above improves the quality of life of each one of the patients and relatives. Cognitive impairment is common in PD, but as it is identified and functional action plans are generated, patients will be able to have more episodes of stigma and emotional well-being.
References
- Jenner P, Morris HR, Robbins TW, Goedert M, Hardy J, Ben-Shlomo Y. Parkinsons disease-the debate on the clinical phenomenology, aetiology, pathology and pathogenesis. J Parkinsons Dis 2013; 3: 1-11.
- Gonzalez-Redondo R, Garcia-Garcia D, Clavero P, Gasca-Salas C, Garcia-Eulate R, Zubieta JL. Grey matter hypometabolism and atrophy in Parkinsons disease with cognitive impairment: a two-step process. Brain 2014; 137: 2356-2367.
- Fernández de BR, Pagonabarraga J, Martínez-Horta S, Pascual SB, Campolongo A, Kulisevsky J. Parkinsons disease-cognitive rating scale: Psychometrics for mild cognitive impairment. Mov Disord 2013; 28: 1376-1383.
- Hu M, Szewczyk KK, Tomlinson P, Nithi K, Rolinski M, Murray C. Predictors of cognitive impairment in an early stage Parkinsons disease cohort. Mov Disord 2014; 29: 351-359.
- Palavra NC, Naismith SL, Lewis SJ. Mild cognitive impairment in Parkinsons disease: a review of current concepts. Neurol Res Int 2013; 2013: 576091.
- Janvin CC, Larsen JP, Aarsland D, Hugdahl K. Subtypes of mild cognitive impairment in Parkinsons disease: progression to dementia. Mov Disord 2006; 21: 1343-1349.
- Barone P, Aarsland D, Burn D, Emre M, Kulisevsky J. Cognitive impairment in nondemented Parkinsons disease. Mov Disord 2011; 26: 2483-2495.
- Benito LJ, Louis ED, Posada IJ, Sánchez FA, Trincado R. Population-based case-control study of cognitive function in early Parkinsons disease (NEDICES). J Neurol Sci 2011; 310: 176-182.
- Ibarretxe-Bilbao N, Junque C, Marti MJ, Tolosa E. Brain structural MRI correlates of cognitive dysfunctions in Parkinsons disease. J Neurol Sci 2011; 310: 70-74.
- Kehagia AA, Barker RA, Robbins TW. Neuropsychological and clinical heterogeneity of cognitive impairment and dementia in patients with Parkinsons disease. Lancet Neurol 2010; 9: 1200-1213.
- Helkala EL, Laulumaa V, Soininen H, Riekkinen PJ. Different error pattern of episodic and semantic memory in Alzheimers disease and Parkinsons disease with dementia. Neuropsychologia 1989; 27: 1241-1248.
- Mak E, Zhou J, Tan LC, Au WL, Sitoh YY. Cognitive deficits in mild Parkinsons disease are associated with distinct areas of grey matter atrophy. J Neurol Neurosurg Psychiatry 2014; 85: 576-580.
- Poletti M, Bonuccelli U. Acute and chronic cognitive effects of levodopa and dopamine agonists on patients with Parkinsons disease: a review. Ther Adv Psychopharmacol 2013; 3: 101-113.
- Pereira JB, Junque C, Martí M, Ramirez-Ruiz B, Bargallo N, Tolosa E. Neuroanatomical substrate of visuospatial and visuoperceptual impairment in Parkinsons disease. Mov Disord 2009; 24: 1193-1199.
- Christopher L, Strafella AP. Neuroimaging of brain changes associated with cognitive impairment in Parkinsons disease. J Neuropsychol 2013; 7: 225-240.
- Pavese N. PET studies in Parkinsons disease motor and cognitive dysfunction. Parkinsonism Relat Disord 2012; 18: 96-99.
- Narayanan NS, Rodnitzky RL, Uc EY. Prefrontal dopamine signalling and cognitive symptoms of Parkinsons disease. Rev Neurosci 2013; 24: 267-278.
- Vazey EM, Aston-Jones G. The emerging role of norepinephrine in cognitive dysfunctions of Parkinsons disease. Front Behav Neurosci 2012; 6: 48.
- Lauretani F, Maggio M, Silvestrini C, Nardelli A, Saccavini M. Parkinsons disease (PD) in the elderly: an example of geriatric syndrome (GS)? Arch Gerontol Geriatr 2012; 54: 242-246.
- Polito C, Berti V, Ramat S, Vanzi E, De Cristofaro MT, Pellicano G. Interaction of caudate dopamine depletion and brain metabolic changes with cognitive dysfunction in early Parkinsons disease. Neurobiol Aging 2012; 33: 206.
- Poletti M, Emre M, Bonuccelli U. Mild cognitive impairment and cognitive reserve in Parkinsons disease. Parkinsonism Relat Disord 2011; 17: 579-586.
- Pagonabarraga J, Kulisevsky J. Cognitive impairment and dementia in Parkinsons disease. Neurobiol Dis 2012; 46: 590-596.
- Biundo R, Calabrese M, Weis L, Facchini S, Ricchieri G, Gallo P. Anatomical correlates of cognitive functions in early Parkinsons disease patients. PLoS One 2013; 8: 64222.
- Luque MC, Lopez GJC, Díaz AE. Análisis de la atención sostenida en pacientes parkinsonianos en tratamiento con precursores de dopamina. Revista de Neurología 2012; 55: 257-262.
- Sawada Y, Nishio Y, Suzuki K, Hirayama K, Takeda A. Attentional set-shifting deficit in Parkinsons disease is associated with prefrontal dysfunction: an FDG-PET study. PLoS One 2012; 7: e38498.
- Galtier I, Nieto A, Barroso J, Norelis LJ. Visuospatial learning impairment in Parkinson disease. Psicothema 2009; 21: 21-26.
- McDonald WM, Richard IH, DeLong MR. Prevalence, etiology, and treatment of depression in Parkinsons disease. Biol Psychiatry 2003; 54: 363-375.
- Weintraub D, Moberg PJ, Culbertson WC, Duda JE, Stern MB. Evidence for impaired encoding and retrieval memory profiles in Parkinson disease. Cogn Behav Neurol 2004; 17: 195-200.
- Ellfolk U, Joutsa J, Rinne JO, Parkkola R, Jokinen P. Brain volumetric correlates of memory in early Parkinsons disease. J Parkinsons Dis 2013; 3: 593-601.
- Demakis GJ. The neuropsychology of Parkinsons disease. Dis Mon 2007; 53: 152-155.
- Picconi B, Piccoli G, Calabresi P. Synaptic dysfunction in Parkinsons disease. Adv Exp Med Biol 2012; 970: 553-572.
- Bohnen NI, Kaufer DI, Ivanco LS, Lopresti B, Koeppe RA, Davis JG. Cortical cholinergic function is more severely affected in Parkinsonian dementia than in Alzheimer disease: an in vivo positron emission tomographic study. Arch Neurol 2003; 60: 1745-1748.
- Pillon B, Deweer B, Michon A, Malapani C, Agid Y, Dubois B. Are explicit memory disorders of progressive supranuclear palsy related to damage to striatofrontal circuits? Comparison with Alzheimers, Parkinsons, and Huntingtons diseases. Neurol 1994; 44: 1264-1270.
- Gobel EW, Blomeke K, Zadikoff C, Simuni T, Weintraub S, Reber PJ. Implicit perceptual-motor skill learning in mild cognitive impairment and Parkinsons disease. Neuropsychol 2013; 27: 314.
- Goldman JG, Stebbins GT, Bernard B, Stoub TR, Goetz CG, deToledo-Morrell L. Entorhinal cortex atrophy differentiates Parkinsons disease patients with and without dementia. Mov Disord 2012; 27: 727-734.
- Tirapu UJ, Muñoz CJ, Pelegrín VC. Funciones ejecutivas: necesidad de una integración conceptual. Revista de Neurología 2002; 34: 673-685.
- George JS, Strunk J, Mak MR, Houser M, Poizner H, Aron AR. Dopaminergic therapy in Parkinsons disease decreases cortical beta band coherence in the resting state and increases cortical beta band power during executive control. Neuroimag Clin 2013; 3: 261-270.
- Sawamoto N, Piccini P, Hotton G, Pavese N, Thielemans K. Cognitive deficits and striato-frontal dopamine release in Parkinsons disease. Brain 2008; 131: 1294-1302.
- Dujardin K, Sockeel P, Delliaux M, Destée A, Defebvre L. Apathy may herald cognitive decline and dementia in Parkinsons disease. Mov Disord 2009; 24: 2391-2397.
- Filoteo JV, Reed JD, Litvan I, Harrington DL. Volumetric correlates of cognitive functioning in nondemented patients with Parkinsons disease. Mov Disord 2014; 29: 360-367.
- Meyer A, Zimmermann R, Gschwandtner U, Hatz F, Bousleiman H. Apathy in Parkinsons disease is related to executive function, gender and age but not to depression. Front Aging Neurosci 2015; 6: 350.
- Pedersen KF, Alves G, Aarsland D, Larsen JP. Occurrence and risk factors for apathy in Parkinson disease: a 4-year prospective longitudinal study. J Neurol Neurosurg Psychiatry 2009; 80: 1279-1282.
- Varanese S, Perfetti B, Ghilardi MF, Di Rocco A. Apathy, but not depression, reflects inefficient cognitive strategies in Parkinsons disease. PLoS One 2011; 6: 17846.
- Kudlicka A, Clare L, Hindle JV. Executive functions in Parkinsons disease: Systematic review and meta-analysis. Mov Disord 2011; 26: 2305-2315.
- Fournet N, Moreaud O, Roulin JL, Naegele B, Pellat J. Working memory in medicated patients with Parkinsons disease: the central executive seems to work. J Neurol Neurosurg Psychiatry 1996; 60: 313-317.
- Monastero R, Di Fiore P, Ventimiglia GD, Camarda R, Camarda C. The neuropsychiatric profile of Parkinsons disease subjects with and without mild cognitive impairment. J Neural Transm (Vienna) 2013; 120: 607-611.
- Poletti M, De Rosa A, Bonuccelli U. Affective symptoms and cognitive functions in Parkinsons disease. J Neurol Sci 2012; 317: 97-102.
- Foster PS, Drago V, Yung RC, Skidmore FM, Skoblar B, Shenal BV. Anxiety affects working memory only in left hemibody onset Parkinson disease patients. Cogn Behav Neurol 2010; 23: 14-18.
- Cardoso EF, Maia FM, Fregni F, Myczkowski ML, Melo LM, Sato JR. Depression in Parkinsons disease: convergence from voxel-based morphometry and functional magnetic resonance imaging in the limbic thalamus. Neuroimag 2009; 47: 467-472.
- Weintraub D, Burn DJ. Parkinsons disease: the quintessential neuropsychiatric disorder. Mov Disord 2011; 26: 1022-1031.
- Karrasch M, Laatu S, Martikainen K, Marttila R. CERAD test performance and cognitive impairment in Parkinsons disease. Acta Neurol Scand 2013; 128: 409-413.
- Gullett JM, Price CC, Nguyen P, Okun MS, Bauer RM, Bowers D. Reliability of three benton judgment of line orientation short forms in idiopathic Parkinsons disease. Clin Neuropsychol 2013; 27: 1167-1178.
- Theilmann RJ, Reed JD, Song DD, Huang MX, Lee RR. White-matter changes correlate with cognitive functioning in Parkinsons disease. Front Neurol 2013; 4: 37.
- Cooper JA, Sagar HJ, Jordan N, Harvey NS, Sullivan EV. Cognitive impairment in early, untreated Parkinsons disease and its relationship to motor disability. Brain 1991; 114: 2095-2122.
- Levin BE, Llabre MM, Reisman S, Weiner WJ, Sanchez-Ramos J. Visuospatial impairment in Parkinsons disease. Neurology 1991; 41: 365-369.
- McKinlay A, Albicini M, Kavanagh PS. The effect of cognitive status and visuospatial performance on affective theory of mind in Parkinsons disease. Neuropsych Dis Treat 2013; 9.
- Sanchez Rodriguez JL. Neuropsychological deficit in Parkinsons disease. Its relation with clinical variables. Rev Neurol 2002; 35: 310-317.
- Uc EY, Rizzo M, Anderson SW, Qian S, Rodnitzky RL. Visual dysfunction in Parkinson disease without dementia. Neurology 2005; 65: 1907-1913.
- Zheng Z, Shemmassian S, Wijekoon C, Kim W, Bookheimer SY. DTI correlates of distinct cognitive impairments in Parkinsons disease. Hum Brain Mapp 2014; 35: 1325-1333.