Research Article - Biomedical Research (2018) Volume 29, Issue 10
Implication of serum microRNA-7a/B with myocardial cell injury induced by ischemia reperfusion
Xue Han, Ruan Zhongbao, Chen Xiaofeng, Pu Xuehua, Ye Jilu*People’s Hospital of Taizhou, PR China
Accepted date: November 13, 2017
DOI: 10.4066/biomedicalresearch.29-17-2915
Visit for more related articles at Biomedical ResearchAbstract
Objective: To investigate the association between serum microRNA-7a/b and Myocardial Cell Injury (MCI) induced by ischemia reperfusion in Acute Myocardial Infarction (AMI) patients.
Methods: Sixty (60) senile AMI patients were selected and placed in the observation group (A group), while 60 healthy people served as the healthy control group (group B). Depending on their conditions after emergency thrombolytic therapy, the AMI patients were sub-divided into no-reflow group (A1 group, 23 cases) and reperfusion group (A2 group, 37 cases). Blood levels of high-sensitive C-reactive protein (hs-CRP) and N-terminal pro-natriuretic peptide (NT-proBNP) were determined in all patients. MicroRNA-7a/b expressions were measured in venous blood 24 h and 120 h before and after thrombolytic therapy.
Results: There were significant, time-dependent increases in microRNA-7a/b expression after thrombolytic therapy, when compared with the control group (p<0.05). Results of correlation analysis showed that microRNA-7a/b was positively correlated with hs-CRP (r1=0.666, p<0.05; but negatively correlated with D-D (r2=-0.642, p<0.05).
Conclusion: In myocardial cell injury induced by ischemia reperfusion, microRNA-7a/b expression is linked to oxidative stress and apoptosis of cardiomyocytes. Thus I/RI might be mitigated by regulating the expression of this microRNA.
Keywords
MicroRNA-7a/b, Ischemia reperfusion injury, Myocytes, Relevance.
Introduction
Acute Myocardial Infarction (AMI) is a major cause of death in cardiovascular diseases. Fortunately, the patient may be saved by surgical opening of the affected artery at the onset of infarction [1]. However, reperfusion after repeated myocardial ischemia damages the structure of the myocardium, resulting in Ischemia/Reperfusion injury (I/RI), which may cause arrhythmia. The disease has attracted much attention since it was first reported by Jennings and his co-workers in 1960 [2]. In spite of numerous research efforts, no effective treatment for I/RI has so far been developed. The clinical management of AMI requires the re-establishment of blood circulation in the coronary artery.
Studies have shown that the expression of specific microRNA may have a protective effect against I/RI in myocytes [3]. MicroRNA is an endogenous non-coding, single stranded, small molecular RNA which is capable of regulating gene expression. MicroRNAs have been implicated in cardiac growth, apoptosis of myocytes, heart failure and cardiac hypertrophy [4]. In recent years, many studies have demonstrated that microRNAs play important roles in regulation of I/RI [4-7]. However, the precise implication of microRNA-7a/b in I/RI expression is still unclear. Therefore, this study was aimed at investigating the relevance of serum microRNA-7a/b of patients in myocardial cell injury induced by ischemia reperfusion, so as to establish a basis for further clinical studies.
Materials and Methods
General attributes of the study population
In this study, 60 AMI patients seen in People's Hospital of Taizhou (Taizhou City, China) from April, 2014 to March, 2016 were selected as the observation group (A group), consisting of 34 male cases and 26 female cases. Their ages ranged from 62 to 74 y (mean age was 63.2 ± 5.3 y). Their cardiac function was KILLIP classes I and II.
Inclusive criteria
2. Ethical approval was given by the medical ethics committee of People's Hospital of Taizhou with the following reference number: 2014014. The inclusive criteria covered patients with obvious clinical disease history of ischemic chest pain, and patients with changes in ECG and serum markers of myocardial necrosis for more than 18 y.
Exclusive criteria
Patients with hereditary chest pain, psychological diseases; severe impairment of cardiac, pulmonary and renal functions; and patients with chronic diseases (e.g. tumor) were excluded. Sixty (60) confirmed healthy through medical examination in our hospital, were placed in the healthy control group (B group). They comprised 35 males and 25 females whose ages ranged from 61 to 74 y (mean age=64.1 ± 5.3 y).
Equipment and reagents
Bacterial incubators were bought from Germany Binder Company (Tuttlingen, Deutschland). High speed freezing centrifuge and low-temperature, high speed desktop centrifuge were products of Zhuhai Heima Medical Instruments Limited (Germany). Flow cytometer was purchased from American Beckman Coulter Company (USA). Real-time PCR instrument was product of American Roche Medical Instrument Company. Real-time quantitative PCR instrument was from Xian’ Tianlong Technology Limited, China, while BM-37XB inverted biological microscope was product of Shanghai BM optical Instruments Manufacture Company Ltd, China. DNA gel extraction kits were obtained from Tiangen Biotech (Beijing) Company Ltd., China. Gold View dye was product of Beijing BLKW Biotechnology Co. Ltd., China, while RNA enzyme inhibitor was obtained from Shanghai Promega Company, China. Serum troponin I kits were products of Nanjing GeteinBiotech Co., Ltd., China. Urokinase was bought from Zhuhai and Lizhu manufacturing in China.
Sample collection, preservation and analyses
The 60 AMI patients were sub-divided into no-reflow group (A1 group) and reperfusion group (A2) group, depending on their status after thrombolytic surgery. There were no obvious statistical differences in general data of sex and age of patients in the three groups (p ≥ 0.05). All patients and their families signed patients’ informed consent forms issued by the ethics committee of our hospital before the study. Venous blood samples were taken by trained personnel before, 24 h and 120 h after thrombolysis. The blood samples were centrifuged and the plasma samples were stored in liquid nitrogen. Freezing and thawing were avoided. The plasma samples were analysed for hs-CRP, D-D and microRNA-7a/b. Hs-CRP was measured by electro-chemiluminescence immunoassay, while D-D was determined by colloid gold double antibodies sandwich method. MicroRNA-7a/b was measured by RT-PCR using assay kits according to manufacturer’s instructions. The primers were synthesized by Shanghai Bioligo Co., Ltd using Primer Premier5.2 software. All primers were prepared at a concentration of 10 pmol/pL. The reference gene used was U6. The primer sequences are shown in Table 1. All assays were done under sterile conditions.
| Gene | Primer sequence (5'- 3') | Annealing temperature (°C) | Premier length (bp) |
|---|---|---|---|
| U6 | F: 5' GCTTCGGCAGCACATATACTAAAAT 3' | 60 | 89 |
| R: 5' CGCTTCACGAAGCGTGTCAT 3' | |||
| GSP: 5' CACCTATATTGCACTTGTCC 3' | |||
| MicroRNA-7a/b | R: 5' TGCGTGTCGTGGAGTC 3' | 60 | 65 |
| GSP: S' GGGGTCGTACCGTGAGT 3' |
Table 1: Primer sequences.
This research was approved by the Ethical Committee of People's Hospital of Taizhou according to the declaration of Helsinki promulgated in 1964 as amended in 1996, the approval number is 20170101; [8].
Statistical analysis
Measurement data were represented by mean ± s. The data were input into Excel, and analysed statistically by t-test using SPSS 18.0 statistical software. Enumeration data were analysed with χ2 test. Data were subjected to Pearson and Spearman correlation analysis. Statistical significance was assumed at p<0.05.
Results
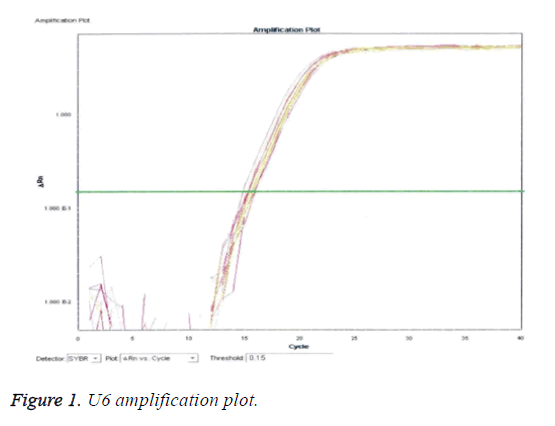
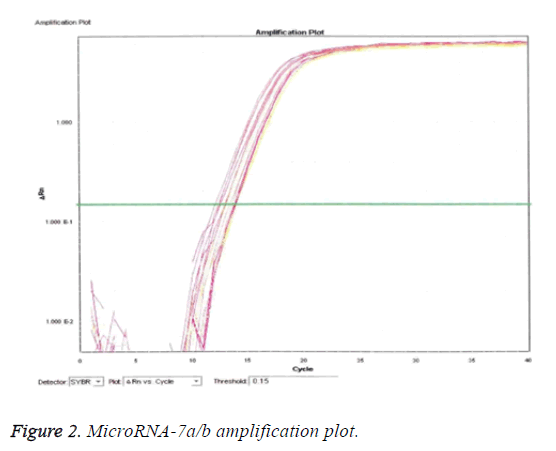
Evaluation of microRNA-7a/b amplification by RTPCR
From Figures 1 and 2, it is clear that the pattern of amplification of the reference gene (U6) was exhibited by microRNA7a/b. evidently, the presence and level of U6 can be equated to microRNA7a/b qualitatively and quantitatively, since it is the reference gene.
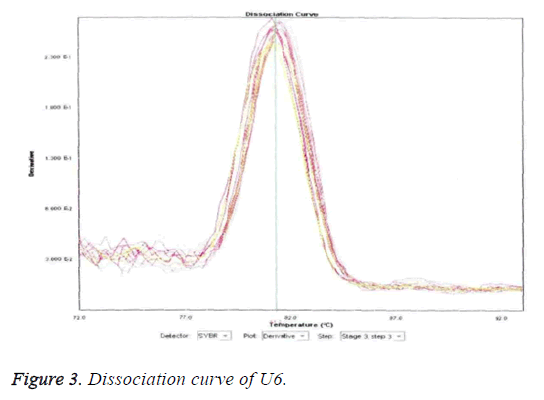
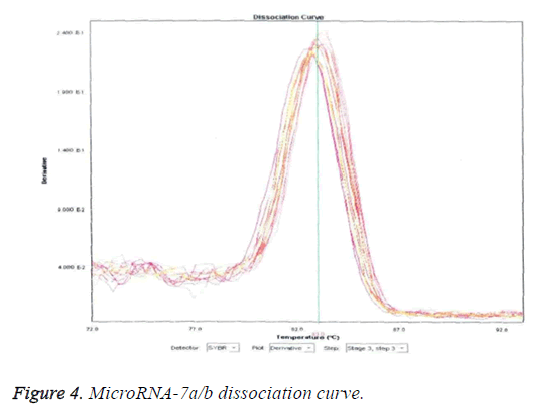
Detection of microRNA-7a/b by agarose gel electrophoresis
The results of detection of microRNA7a/b are displayed in Figures 3-5. Figures 3 and 4 reveal that U6 (reference gene) and microRNA7a/b sequences were predominantly amplified as evident by the prominent single peak in each the two Figures. Impure peaks were relatively few and less obvious.
Determination of microRNA-7a/b expression by RTPCR
Table 2 shows the levels of expression of microRNA-7-a/b before and after thrombolysis. There were significant increases in the expression of microRNA-7a/b after thrombolytic treatment, and between the two time points (p<0.05). Thus, microRNA-7a/b expression was significantly influenced by time and thrombolysis (p<0.05). In contrast, there were no significant changes in microRNA7a/b expressions in the healthy, control group (Table 2).
| Group | Period | ||
|---|---|---|---|
| Before treatment | Â 24 h after treatment | Â 120 h after treatment | |
| A | 0.48 ± 0.04 | 0.48 ± 0.03 | 0.49 ± 0.04 |
| B1 | 0.47 ± 0.03 | 0.48 ± 0.04 | 0.550 ± 0.04 |
| B2 | 0.35 ± 0.05* | 0.41 ± 0.04* | 0.50 ± 0.05* |
Table 2: MicroRNA-7a/b expression before and after thrombolysis.
Expressions of hs-CRP, D-D and MicroRNA-7a/b in AMI patients after acute thrombolytic treatment
The levels of D-D and microRNA-7a/b expressions were significantly lower in the reperfusion group than in the noreflow group (p<0.01). From correlation analyses, microRNA-7a/b was positively correlated with hs-CRP (r1=0.666, p<0.05) but negatively correlated with D-D (r2=-0.642, p<0.05). These results are shown on Table 3.
| Group | Cases | hs-CRP (mg/L) | D-D (µg/L) | MicroRNA-7a/b |
|---|---|---|---|---|
| B1 | 23 | 45.64 ± 16.75 | 679.75 ± 135.64 | 2.75 ± 0.43 |
| B2 | 37 | 5.53 ± 2.13 | 190.64 ± 99.75 | 1.76 ± 0.21 |
| T | 3.756 | 7.767 | 4.886 | |
| P | = 0.05 | <0.01 | <0.01 |
Table 3: Comparison of hs-CRP, D-D and microRNA-7a/b expressions in the two AMI groups.
Discussion
Improvements in quality of life and changes in lifestyle have made ischemic heart disease a major threat to people’s health [9]. Statistics have shown that there are about 20 million ischemic heart disease patients in China, with a projected annual increase of 0.5% [10]. Although the re-establishment of blood flow by surgical re-opening of the infarcted arteries is key to saving patients’ lives, studies have shown that reperfusion after constant myocardial ischemia damages the structure of the myocardium. The damage to the myocardium is due to oxygen free radical-mediated apoptosis, and impairment of intracellular energy metabolism [11,12]. Thus, myocardial ischemia reperfusion is associated with complications. However, the mechanisms underlying the reperfusion-induced myocardial damage have not been fully understood. Acute thrombolytic treatment is the main emergency percutaneous coronary intervention in clinical treatment for AMI patients. The major thrombolytic drug used is urokinase, a bi-serine protein extracted from human urine or tissue culture medium of renal cells. Urokinase activates plasminogen to active plasmin which dissolves blood clots in circulation in the AMI patient.
MicroRNAs are expressed in various tissues. In the cardiovascular system, it participates in multiple physiological processes of heart growth, cardiac hypertrophy and apoptosis. Recent studies have suggested that microRNA expression might have anti-apoptotic effects in cardiac ischemia reperfusion injury [13,14]. These findings have elicited a lot of research interest on the regulation of cardiac ischemia. Indeed, studies have reported that cardiac ischemia reperfusion injury can be controlled by regulating the expression of microRNA [15,16]. It has also been reported that microRNAs can function as tumor inhibitory factors through the regulation and inhibition of multiple cancers [17,18]. However, the specific roles of microRNA-7a/b expressions in cardiac ischemia reperfusion injury, and the mechanisms involved are still unclear.
In the present study, the expression of microRNA-7a/b in AMI patients was significantly increased in a time-dependent manner after reperfusion. Moreover, the microRNA-7a/b levels were positively correlated with hs-CRP.
Limitation of the Study
This study is one correlational research. The mechanism is still unclear.
Conclusion
The results obtained in this study strongly suggest that in cardiac ischemia reperfusion injury, microRNA-7a/b expression is correlated with oxygen free radicals and myocardial apoptosis. Thus, ischemia reperfusion injury might be reduced by regulating the expression of this microRNA.
Acknowledgement
This research was supported by Taizhou municipal social development project Science and technology item number: TS2013006.
Conflict of Interest
No conflict of interest associated with this work.
Contribution of Authors
We declare that this work was done by Xue Han, Ruan Zhongbao, Chen Xiaofeng, Pu Xuehua1 and Ye Jilu in this article and all liabilities pertaining to claims relating to the content of this article will be borne by the authors, all authors read and approved the manuscript for publication. Ye Jilu conceived and designed the study, Xue Han, Ruan Zhongbao, Chen Xiaofeng, Pu Xuehua1 and Ye Jilu, Xue Han wrote the manuscript.
References
- Li-Feng Z, Liang ZR, Xiu-Hua J, Chen C, Chen W. MicroRNA-15a/b are up-regulated in response to myocardial ischemia/reperfusion injury. J Geriatr Cardiol 2012; 9: 28-30.
- Jennings RB, Sommers HM, Smyth GA, Flack HA, Linn H. Myocardial necrosis induced by temporary occlusion of a coronary artery in the dog. Arch Pathol 1960; 70: 68-70.
- Li B, Li R, Zhang C, Bian HJ, Wang F, Xiao J, Liu SW, Yi W, Zhang MX, Wang SX. MicroRNA-7a/b protects against cardiac myocyte injury in ischemia/reperfusion by targeting poly(ADP-ribose) polymerase. Plos One 2014; 9: 90096.
- Eisenhardt SU, Weiss JB, Smolka C, Maxeiner J, Pankratz F, Bemtgen X, Kustermann M, Thiele JR, Schmidt Y, Bjoern SG. MicroRNA-155 aggravates ischemia-reperfusion injury by modulation of inflammatory cell recruitment and the respiratory oxidative burst. Basic Res Cardiol 2015; 110: 32-35.
- Ren XP, Wu J, Wang X, Sartor MA, Jones K, Qian J, Nicolaou P, Pritchard TJ, Fan GC. MicroRNA-320 is involved in the regulation of cardiac ischemia/reperfusion injury by targeting heat-shock protein 20. Circulation 2009; 119: 2357-2366.
- Xiao J, Zhu X, He B, Zhang Y, Kang B, Wang Z, Ni X. MiR-204 regulates cardiomyocyte autophagy induced by ischemia-reperfusion through LC3-II. J Biomed Sci 2011; 18: 35-38.
- Shan DKSXW, An LN. MicroRNA: myocardial ischemia-reperfusion injury regulation personnel. Int J Cardiovasc Dis 2013; 40: 269-271.
- Organization WH. Declaration of Helsinki. Br Med J 1996; 313: 1448-1449.
- Tan J, Xiao J. Changes of the expression profile of microRNAs in myocardium of rats with ischemia reperfusion injury. J Pract Med 2012; 45: 1-8.
- Yang Q, Yang K, Li A, Tan W. Anti-apoptosis and expression of microRNA-21 in rat myocardium during early ischemia-reperfusion injury. J Central South Univ 2013; 38: 483-489.
- Wang E, Yu N, Qian Z, Wei W, Jie H, Liao Z, Hao Z, Hu S, Zhe Z. Circulating miRNAs reflect early myocardial injury and recovery after heart transplantation. J Cardiothorac Surg 2013; 8: 1-11.
- Wang H. Circulating mirnas in heart failure. J Am Coll Cardiol 2016; 67: 1340.
- Ye Y, Perezpolo JR, Qian J, Birnbaum Y. The role of microRNA in modulating myocardial ischemia-reperfusion injury. Physiol Genom 2011; 43: 534-536.
- Rong LR, Jun L, Jiu Yu G. MicroRNA-141 regulates the expression level of ICAM-1 on endothelium to decrease myocardial ischemia-reperfusion injury. Am J Physiol Heart Circ Physiol 2015; 309: 1303.
- Jiang C, Ji N, Luo G, Ni S, Zong J, Chen Z, Bao D, Gong X, Fu T. The effects and mechanism of miR-92a and miR-126 on myocardial apoptosis in mouse ischemia-reperfusion model. Cell Biochem Biophy 2014; 70: 1901-1906.
- Tao Z, Zhao H, Wang R, Liu P, Yan F, Zhang C, Ji X, Luo Y. Neuroprotective effect of microRNA-99a against focal cerebral ischemia-reperfusion injury in mice. J Neurol Sci 2015; 355: 113-119.
- Chen Q, Kong L, Xu X, Geng Q, Tang W, Jiang W. Down-regulation of microRNA-146a in the early stage of liver ischemia-reperfusion injury. Transpl Proc 2013; 45: 492-495.
- Hori K, Tsujii M, Iino T, Satonaka H, Uemura T, Akeda K, Hasegawa M, Uchida A, Sudo A. Protective effect of edaravone for tourniquet-induced ischemia-reperfusion injury on skeletal muscle in murine hindlimb. BMC Musculoskelet Disord 2013; 14: 1-8.