Case Report - Current Pediatric Research (2019) Volume 23, Issue 1
A Report of Pediatric Giant Congenital Melanocytic Nevi
Mohammed Abdulrahmen Alzahrani*
Department of Pediatrics, King Saud bin Abdul-Aziz University for Health Sciences, Saudi Arabia
- *Corresponding Author:
- Mohammed Abdulrahmen Alzahrani
Department of Pediatrics
King Saud bin Abdul-Aziz University for Health Sciences, Saudi Arabia
Tel: +966556180164
E-mail: Muhmdzh@outlook.com
Accepted on February 13th, 2019
Abstract
Giant congenital melanocytic nevi are rare with an estimated incidence of approximately 1 in 20,000 live births. They increase the lifetime risk for malignant melanoma and neurological deficits, including leptomeningeal melanocytosis and epilepsy. Recently, we encountered a baby girl in whom giant congenital melanocytic nevi was noted at birth. She presented with large nevus over upper back. MRI and biopsy showed no pathology. Plan was to reassure parents and regular follow-ups. Last follow up was at age of 14 months and the patient is well and achieving her milestones. Here, we describe this rare case with congenital melanocytic nevi to expand the literature about its clinical manifestations, outcomes, risks for malignant melanoma and neurocutaneous melanosis, and possible surgical interventions.
Keywords
Giant, Congenital, Nevus.
Introduction
Congenital melanocytic nevus is defined as pigmented lesion that present at birth or in the first year of life with unknown etiology. Most of giant congenital melanocytic nevus (GCMN) cases are sporadic but familial cases have been reported in literature [1]. It has been suggested by Kopf et al., to classify the lesions by surface diameter: small lesions <1.5 cm, intermediate lesions ≤ 1.5-20.0 cm and giant lesions, ≥ 20.0 cm. It has been linked that GCMN is associated with increased risk of cutaneous melanoma and neurological deficits; therefore, the interest in studying this condition is increasing over time [2]. Thus, we report this case of 7 months old baby girl with GCMN to expand the literature about this rare condition.
Case Presentation
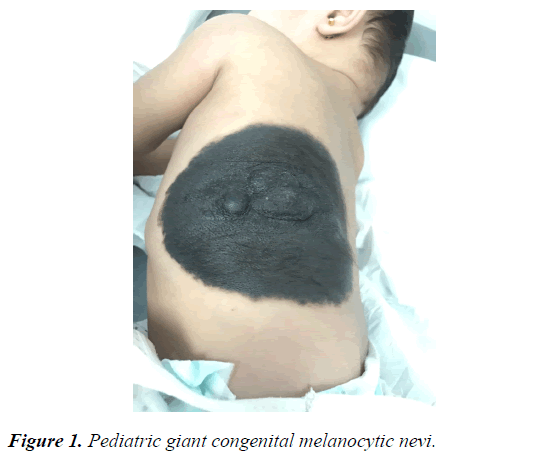
7 months old baby girl, with uneventful antenatal history of exposure to radiation, drugs or complications after delivery, presented with large dark brown area on her back found at birth. It was measured to be 21 × 11 cm (Figure 1). On physical examination, lesions were well demarcated hairy brown plaque with two nodules in the center. There were no other associated congenital anomalies. There was no family history of any similar lesion. Plan was to reassure parents and regular follow-ups. Last follow up was at age of 14 months; and the patient is well and achieving her milestones.
Discussion
GCMN begins as flat pigmented patch that may develop to be elevated. It is rarely invade fascia and muscle rather it is confined to the skin. It appears to be in the back and over thigh areas. It is rare entity occurring in 1 per 500,000 newborns. The etiology of this condition is unknown but researchers relate this condition to be due to chromosomal rearrangements. GCMN increases the risk of melanoma by 80% by the age of seven years old; therefore, patients with GCMN should be screened at a regular basis. When there is bleeding focal growth or pruritus, malignancy should be suspected [3]. MRI is recommended to be ordered when the patient is aged 4-6 months to evaluate the melanocytic deposition in the CNS. However, a normal MRI brain study does not rule out the future risk of CNS melanosis. Thus MRI at a yearly basis is important. The management of GCMN needs to be individualized for each patient depending on different variables such as size and location. All of the following variables should be considered when taking the decision of the mode of treatment: cosmetic issues, risk of surgery, psychological implications, and risk of melanoma. The recommended treatment for GCMN is appeared to be surgical as it decreases risk of malignant melanoma (MM) [4]. Surgical management is suggested to be accomplished in the first weeks of life to extract the cells early before migrating to deep dermis. Furthermore, following-up the patients in a long term period is essential part of the management [5].
Conclusion and Recommendation
GCMN is a rare skin condition that defined as pigmented lesion presents at birth or in the first year of life with unknown etiology. Its necessities a correct diagnosis and proper management due to its risk of developing MM. Moreover, following-up the patients is essential part of the management.
References
- Bhagyalakshmi PV, Sudhakar P, Uma P, et al. Giant congenital melanocytic nevus scalp: Report of a rare case. Int J Res Med Sci 2013; 1: 317-319.
- Kopf A, Bart R, Hennessey P. Congenital nevocytic nevi and malignant melanomas. J Am Acad Dermatol. 1979; 1: 123-130.
- Nevi and Malignant Melanoma. In: Habit TP, Clinical Dermatology: A colour guide to diagnosis and therapy 4th Edinburgh: Mosby. 2004; pp: 776-777.
- Foster RD, Williams ML, Barkovich AJ, et al. Giant congenital melanocytic nevi: The significance of neurocutaneous melanosis in neurologically asymptomatic children. Plast Reconstr Surg 2001; 107: 933-941.
- Schaffer JV, Bolognia JL. The clinical spectrum of pigmented lesions. Clinics in Plastic Surgery. 2000; 27: 391-408.