Research Article - Journal of Clinical Pathology and Laboratory Medicine (2017) Journal of Clinical Pathology and Laboratory Medicine (Special Issue 1-2017)
Role of C3a in Regulating Thymocyte Infection by HIV-1.
- *Corresponding Author:
- Tomasz Rozmyslowicz
Department of Pathology & Laboratory Medicine University of Pennsylvania, Philadelphia, PA USA
Tel: +1 215-898-5000
E-mail: rozmyslo@mail.med.upenn.edu
Accepted date: January 25, 2017
Citation: Rozmyslowicz T, Conover DO, Ratajczak MZ, et al. Role of C3a in Regulating Thymocyte Infection by HIV-1. J Clin Path Lab Med. 2017;1(1):1-5
Abstract
The primary physiological role of complement proteins lies in augmenting host defense to microorganisms. Among several cascade products, complement components C3 and C5 are cleaved and activated through proteolytic processing during immune activation following exposure to HIV-1. This reaction generates the small peptide anaphylatoxins C3a and C5a, which bind to G-protein coupled membrane receptors that sensitize the response of human T-lymphocytic cells to multiple cytokines including CXCL12/SDF-1. CXCL12 is an alpha chemokine that binds to the CXCR4 membrane receptor, which also functions as a co-receptor for X4-tropic HIV-1. Given the importance of complement activation in immune function and the bioactive nature of complement cleavage products we investigated here the role of C3a in HIV-1 infection of human thymocytes. Our data illustrate a potential new link between HIV-1 infection and complement activation in which C3a anaphylatoxin may modulate infectivity by reducing the susceptibility of thymocytes to HIV-1 infection.
Keywords
Thymocytes, HIV-1 infection, Complement, C3a.
Introduction
The complement system is a crucial element of innate immunity and is involved in several processes related to host-pathogen defense mechanisms including during HIV-1 infection [1,2]. The complement system consists of over 30 soluble and membrane-bound proteins and is activated by three distinct pathways in response to the presence of pathogens [3,4]. In each instance the products of these pathways result in cleavage of complement system components C3 and C5 to yield the small peptides C3a and C5a. C3a and C5a function as anaphylatoxins, binding to G-protein coupled membrane receptors that, among several actions, sensitize the response of human T-lymphocytic cells to XCXL12/SDF-1 [5,6].
Activation of the proinflammatory components of the complement cascade is observed in even well managed HIV infected subjects [7]. These elements serve to augment virus opsonization and cell-mediated lysis of infected cells [1,8]. However, a number of other much less well characterized, and seemingly contradictory effects of complement have also been described. For example, complement activation may augment HIV-1 infectivity. Here it was shown that the interaction between HIV-1 gp41 surface protein and the complement receptor C3R modified viral entry to support intracellular viral spread [9]. Similarly, in vitro studies suggested that the complement activation peptide C5a increased the susceptibility of monocytes and monocyte-derived macrophages to HIV infection by enhancing tumor necrosis factor-alpha (TNF-alpha) and IL-6 secretion from these cells [10].
In contrast, we previously reported that human T-lymphocytic cells secrete multiple chemokines that may auto-protect for HIV- 1 infection and that production of these compounds is greatly reduced during active infection [11]. Along these lines, the α-chemokine CXCL12/SDF-1 binds to the membrane receptor CXCR4, which serves as a major co-receptor for X4 HIV-1, and is known to interfere with X4-tropic HIV-1 infection in several cell populations [12]. In view of the overlapping observations of both chemokine production and complement activation during HIV-1 infection, in the present study we examined the potential direct role of the complement component C3a on HIV- 1 infection in thymocytes, a cell population that is crucial to continued maintenance of the mature peripheral T lymphocyte pool.
Materials and Methods
Thymic cell Isolation, tissue culture and C3A incubation
As described previously [13], fresh neonatal human thymic tissue was obtained from elective thoracic surgeries of HIV- 1 negative individuals aged 1 day-6 month. Tissue was diced into 3-10 mm fragments, and incubated with 0.1% collagenase (Sigma, St. Louis, MO) and DNAase 10 IU/ml (Sigma) solution in Dulbecco’s phosphate-buffered saline (PBS) without calcium chloride and magnesium chloride (GibcoBRL, Gaithersburg, MD) for 2 hours at 37°C. The fragments were subsequently passed through a 100 μm nylon cell strainer (Becton Dickinson, Franklin Lakes, NJ), and washed with ice cold PBS. Mononuclear cells were isolated from whole blood by Ficoll-Paque (Amersham Pharmacia, Uppsala, Sweden), and plated onto 10 cm Biocoat tissue culture plates with collagen cover (BD, Bedford, MA) or directly into Biocoat (collagen cover) 6-well plates. Non-adherent cells (thymocytes) were placed in separate dishes (Falcon 24 well plate) for further culture. After 12 hours incubation in RPMI medium (GibcoBRL) cells were supplemented with 10% to 20% fetal bovine serum (FBS), 2 mM glutamine, 100 IU/ml of penicillin, 100 μg/ml of streptomycin and 0.25 μg/ml of amphotericin B. In some experiments, indicated in Results, cells were incubated with C3a or C3adesArg (1 μg/ml) at either -12 hr, 0 hr or +6 hr relative to HIV-1 addition.
HIV infection and assay
Thymocytes were isolated as described above and plated onto either Falcon 24, 48 or 96 well plates as required for subsequent assay. Cells were maintained for one week in RPMI medium supplemented with 10% FBS and subsequently incubated with X4-tropic HIV-1 viral stocks HXB2 or IIIB (gift of Dr. F. Gonzalez-Scarano, Univ. of Texas) at a concentration of 10 ng/ml. After 12-hour incubation, cells were washed 5 times in PBS solution to remove residual virus and zero time samples were collected. Cells were then re-cultured in the presence of RPMI medium supplemented with 10% FBS for the times indicated in the figures. Samples were then analyzed by p24 ELISA or qRT-PCR to determine infection status. ELISA reactions were performed using the Alliance HIV-1 p24 ELISA kit (PerkinElmer, Boston, MA) as previously described [13,14].
Virus measurement by quantitative real-time polymerase chain reaction (RT-qPCR)
Thymocytes were incubated in vitro with IIIB or HXB2 virus. Purified RNA from these cells was reverse-transcribed with MultiScribe Reverse Transcriptase, oligo (dT), and a random hexamer primer mix (all from Applied Biosystems Life Technologies, CA, USA). Quantitative evaluation of the target gene was then performed by using an ABI Prism 7500 sequence detection system (Applied Biosystems Life Technologies) with Power SYBR Green PCR Master Mix reagent and specific primers-reverse primer (HXB2 positions 622 to 642, 5=-AAAATCTCTAGCAGTGGCGCC-3=) was similar to a previously described primer, and the forward primer (HXB2 positions 523 to 539, 5=-SSCTCAATAAAGCTTGCC-3=) had a position and length similar to that previously described [15]. The PCR cycling conditions were 95 °C (15 s), 40 cycles at 95°C (15 s) and 60°C (1 min). According to melting point analysis, only one PCR product was amplified under these conditions.
Detection of complement receptors by RT-PCR
Total RNA was extracted and purified from cells using the RNeasy Mini kit (Qiagen Inc, Valencia, CA, USA) as previously described [16] after treatment with DNase I (Qiagen Inc.) and reverse-transcribed into cDNA. The sequence- specific primers employed for amplification were as follows: human complement component C3 a receptor-1 (hC3aR1; sense, 5′-agaaagacagccaccac cacg-3′; antisense, 5′-gccgcctggagaaatgaatgatagg-3′); human complement component 5a receptor 1 (hC5AR1; sense, 5′-accttcgatcctcggggagc-3′; antisense, 5′-gcgtacatgttgagcaggat-3′); human C5a receptor-2 (hC5L2; sense, 5′-ggattacagcgacctctcgg-3′; antisense, 5′-gcagagacaaacagcacagc-3′). Samples without template controls and reverse transcriptase were used in each run. All primers were designed using the NCBI/Primer-Blast program, and at least one primer in each pair included an exon-intron boundary. Afterwards, all PCR products were analyzed by 2% agarose gel electrophoresis.
Statistical analysis
Arithmetic mean and standard deviation from p24 ELISA and qRT-PCR results were performed using Microsoft Excel 2011. Data was analyzed using the Student t-test for paired and unpaired samples. Statistical significance was defined as p<0.05.
Results/Observations
HIV-1 infection of thymocytes
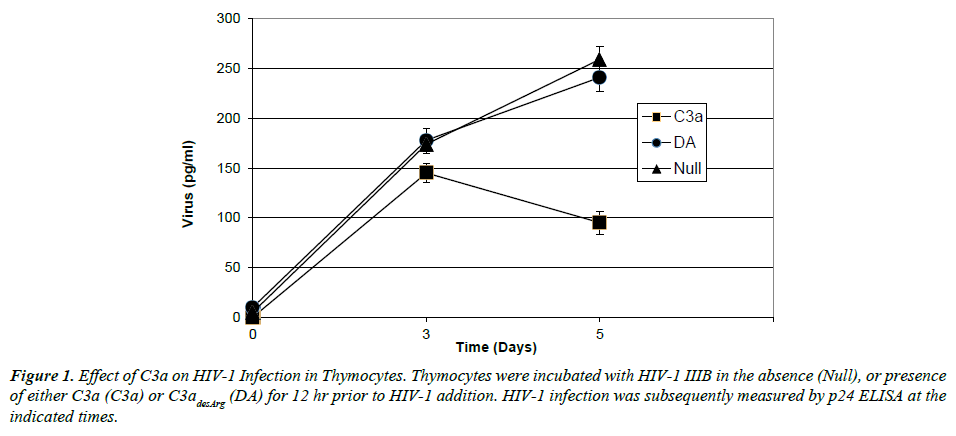
We first studied infection of cultured human thymocytes by the X4 (T-tropic) viruses IIIB and HXB2. Thymocytes were incubated with virus at 10 ng/ml (MOI 0.02) and infection status analyzed by p24 ELISA assay. As shown in Figure 1 for HIV-1 IIIB, virus replicated robustly in thymocytes over a 5 day time course. To assess the impact of C3a peptide on HIV-1 replication, thymocytes were pre-incubated with either C3a or the less active inflammatory C3a cleavage product C3adesArg for 12 hours prior to addition of HIV-1. As also shown in Figure 1, pre-incubation with C3a had a significant inhibitory effect on HIV-1 replication at day 3 and more dramatically so by day 5. In contrast, pre-incubation with C3adesArg had no effect on HIV-1 replication at any time point.
Expression of complement component receptors C3a and C5a on thymocytes
To clarify whether the results presented in the Figure 1 potentially result from the direct action of C3a on thymocytes, we next examined these cells for the presence of both C3a and C5a receptor mRNA (C3aR and C5aR respectively) by RTPCR analysis. Reaction products from the RT-PCR reaction were run an agarose gels and visualized as shown in Figure 2. These results demonstrate that mRNA for both C3aR (555 bp) and C5aR (400 bp) were readily detected in thymocytes.
qRT-PCR analysis of acute C3a effects on HIV-1 replication
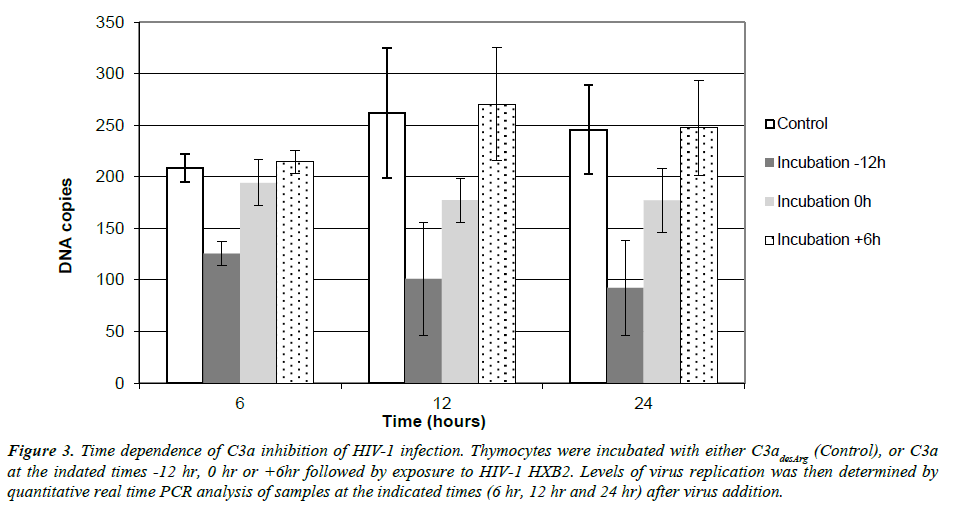
The potential effects of C3a anaphylatoxin on HIV-1 replication may occur at multiple points along the HIV-1 replication cascade. Results presented in Figure 1 demonstrate that C3a significantly inhibited HIV-1 replication when thymocytes were preincubated with this anaphylatoxin. To clarify the time dependence of this effect we conducted qRT-PCR analysis for virus over a 24 hr time course following the addition of C3a either before (-12 hr), simultaneously with (0 hr), or following (+6 hr) incubation with virus. Given that the less active C3a derivative C3adesArg was shown not to inhibit HIV-1 replication (Figure 1), we used this compound as a control for all incubations. Data presented in Figure 3 demonstrate robust HIV-1 replication (240-245 DNA copies) in thymocytes over 24 hr in the presence of 1 μg/ml C3adesArg (Control). In contrast, and in agreement with results shown in Figure 1, pre-incubation with 1 μg/ml C3a for 12 hr resulted in a statistically significant reduction in HIV-1 replication at each time point measured. The magnitude of this inhibition ranged from 49% at 6 hr to 67% at 24 hr. Similar but less substantive effects were observed when incubation with C3a was intiated coincident with (0 hr) the addition of virus. In this instance replication of virus at 6 hr was inhibited by 19%, while at both 12 hr and 24 hr a 27% inhibition was observed; the latter points being statistically signifcant. Lastly, incubation with C3a at +6 hr after HIV-1 exposure resulted in a mixed effect. The impact ranged from a modest 12% inhibition at 6hr, to a slight increase in HIV-1 replication at 12 hr (9%) and 24 hr (2%). None of these differences were statistically significant from control.
Figure 3: Time dependence of C3a inhibition of HIV-1 infection. Thymocytes were incubated with either C3adesArg (Control), or C3a at the indated times -12 hr, 0 hr or +6hr followed by exposure to HIV-1 HXB2. Levels of virus replication was then determined by quantitative real time PCR analysis of samples at the indicated times (6 hr, 12 hr and 24 hr) after virus addition.
Discussion
Dissecting the mechanisms of HIV-1 pathogenesis and aligned host defence mechanisms is a dauting task as the central sites of HIV-1 infectivity reside in and disrupt fundamental components of both innate and adaptive immunity. One clear example lies in the binding of HIV-1 to both CD4 molecules and chemokine receptor CXCR4 and CCR5 family members. These membrane proteins serve critical roles in, respectively, the recognition and chemokine driven regulation of immune function. Thus, HIV-1 binding to these elements in itself may profoundly alter the subsequent immune response to HIV-1. In previous works we demonstrated that HIV-1infection triggers marked alterations in the patterns of cytokine production by cells of the hematopoietic lineage and that these cytokines serve to reduce HIV-1 infectivity [13,17,18]. While multiple studies have elucidated the primary effects of HIV-1 within adaptive immunity, far fewer focus on the impact of virus on components of the innate immune repsponse.
As noted above, the complement system plays a central role in innate immunity and yet the impact of HIV-1 infection on complement activation, and in a related fashion the corresponding effects of complement cascade cleavage products on HIV-1 infection and immunity, are poorly understood [1,2]. It is well documented that complement activation contributes to a proinflammatory state in even well controlled HIV infection [7], and that this activation regulates virus clearance through both cell-mediated lysis and enhanced opsonization [1,8]. However, the consequences of complement activation also significantly augment production of C3a and C5a, and these anaphylatoxins have profound proinflammatory effects on immune function [7,19]. C3a and C5a are highly active biopeptides that exert their effects through the G-protein coupled receptors C3aR and C5aR and are known to regulate the production of multiple chemokines [10].
Our studies focused on the anaphylatoxin C3a and its capacity to modify HIV-1 infection. It is well established that C3a binding triggers production of CXCL12/SDF-1, and although CXCL12 may inhibit HIV-1 entry via the CXCR4 co-receptor the effects of C3a binding beyond this effect are not known [20]. In this study we examined the effects of C3a on HIV-1 replication in thymocytes using the well characterized X4-tropic viruses IIIB and HXB2. Thymocytes were chose as target cells as they support X4-tropic HIV-1 replication and are a fundamental precursor to the generation of mature Tcells.
The thymus is the primary site of T-lymphocyte development and selection for MHC [21]. Although a dependence on thymic function for immune maintenance decreases with age, thymic tissue persists in adults and may be reactivated following the depletion of peripheral T cells [22]. T cell maturation in the thymus is regulated by the interaction of thymocytes with nonlymphoid thymic stroma via a multifaceted process, which may be disrupted by infectious agents such as HIV-1 [23,24]. There are two primary pathways by which HIV-1 is believed to affect thymocyte development. The first is direct infection and toxicity within thymocytes. Infection of thymocytes by HIV-1 is well documented and, much like with mature T cell infection, can have profound effects on cell viability and function [25,26]. The second means is through HIV-1 infection of the thymic stroma. Although this process is poorly understood the primary mechanisms are believed to occur through alterations in cytokines and/or stromal adhesion events critical to thymocyte selection and maturation [27-29].
The results presented in the present study demonstrated a clear inhibitory effect of complement component C3a on HIV-1 infection. When added prior to HIV exposure C3a resulted in a 60% reduction in HIV replication over a 5 day period as meaure by p24 ELISA and a 67% reduction by 24hr when measure by qRT-PCR. Our results also suggest that the mechanism of this effect is coupled to alterations in the intial events of HIV- 1 binding and entry in thymocytes. We demonstrated that thymocytes produce C3aR, that the inhibitory effects were not observed with the poorly active C3a dervative C3adesArg, and that the inhibitory effects of C3a additon were maximal when added 12 hr prior to HIV-1 exposure. Inhibition was diminshed when C3a was added coincident with HIV-1 and was absent when added 6 hr post HIV-1 exposure. Whether the impact of C3a on HIV-1 replication occurs by direct membrane effects at entry and/or whether C3a binding induces the production of cytokines, such as CXCL12, that subsequently inhibit HIV-1 binding is the subject of our ongoing studies.
References
- Yu Q, Yu R, and Qin X. The good and evil of complement activation in HIV-1 infection. Cell Mol Immunol. 2010;7:334-40.
- Stoiber H,Kacani L,Speth C,et al. The supportive role of complement in HIV pathogenesis. Immunol Rev. 2001;180:168-76.
- Walport MJ. Complement: First of two parts. N Engl J Med. 2001;344:1058-66.
- Wetsel RA. Structure, function and cellular expression of complement anaphylatoxin receptors. Curr Opin Immunol. 1995;7:48-53.
- Volanakis JE. Overview of the complement system. In: Volanakis JE, editor. The human complement system in health and disease. New York, NY: Marcel Dekker.1998; p 9-32.
- Reca R,Mastellos D,Majka M, et al. Functional receptor for C3a anaphylatoxin is expressed by normal hematopoietic stem/progenitor cells, and C3a enhances their homing-related responses to SDF-1. Blood. 2003;101(10):3784-93.
- RossheimEBA, Cunningham TD, Hair PS, et al. Effects of well-controlled HIV infection on complement activation and function. JAIDS. 2016;73(1): 20-6.
- Tjomsland V,Ellegård R,Burgener A, et al. Complement opsonization of HIV-1 results in a different intracellular processing pattern and enhanced MHC class I presentation by dendritic cells. Eur J Immunol. 2013;43(6):1470-83.
- Stoiber H, Frank I, Spruth M, et al. Inhibition of HIV-1 infection in vitro by monoclonal antibodies to the complement receptor type 3 [CR3]: An accessory role for CR3 during virus entry? Mol Immunol. 1997;34:855-63.
- Kacani L,Banki Z,Zwirner J, et al. C5a and C5a (desArg) enhance the susceptibility of monocyte-derived macrophages to HIV infection. J Immunol. 2001; 166: 3410-5.
- Rozmyslowicz T, Kijowski J, Conover DO, et al. New T-lymphocytic cell lines for studying cell infectability by HIV. Eur J Haematol. 2001; 67: 142-151.
- Arenzana-Seisdedos F. SDF-1/CXCL12: A chemokine in the life cycle of HIV. Front Immunol. 2015;6(256):1-4.
- Rozmyslowicz T, Murphy SL, Conover DO, et al. HIV infection inhibits cytokine production in human thymic macrophages.Exp Hematol. 2010; 38[12]: 1157-66.
- Rozmyslowicz T, Conover DO. and Gaulton GN. HIV-1 infection of human thymic stromal cells and thymocytes in vitro. HIV/AIDS. Res Treat Open J. 2015;2(4):92-96.
- Etienne L,Eymard-Duvernay S,Aghokeng A, et al. Single real-time reverse transcription-PCR assay for detection and quantification of genetically diverse HIV-1, SIVcpz, and SIVgorstrains. J Clin Microbiol. 2013;51(3):787-98.
- Abdelbaset-Ismail A,Borkowska-Rzeszotek S,Kubis E, et al. Activation of the complement cascade enhances motility of leukemic cells by downregulating expression of HO-1. Leukemia. 2016;198:1-13.
- Majka M,Rozmyslowicz T,Ratajczak J, et al. The limited infectability by R5 HIV of CD34+ cells fromthymus, cord and peripheral blood and bone marrow is explained by their ability to produce b-chemokines.Exp Hematol. 2000;28:1334-42.
- Majka M, Rozmyslowicz T,Honczarenko M, et al. Biological significance of the expression of HIV-relatedchemokine coreceptors (CCR5 and CXCR4) and their ligands by human hematopoietic cell lines. Leukemia.2000;14:1821-32.
- Moreno-Fernandez ME, Aliberti J, Groeneweg S, et al. A novel role for the receptor of the complement cleavage fragment C5a, C5aR1, in CCR5-mediated entry of HIV into macrophages. AIDS Res Hum Retrovir. 2016;32(4):399-408.
- Altenburg JD, Broxmeyer HE, Jin Q. et al. A naturally occurring splice variant of CXCL12/stromal cell-derived factor 1 is a potent human immunodeficiency virus type 1 inhibitor with weak chemotaxis and cell survival activities. J Virol. 2007;81(15):8140-8.
- Haynes BF, Martin ME, Kay HH,et al. Early events in human T cell ontogeny. Phenotypiccharacterization and immunohistologic localization of T cell precursors in early human fetal tissues. J ExpMed. 1988;168:1061-80.
- Spits H. Development of alphabeta T cells in the human thymus. Nat Rev Immunol. 2002;2:760-2.
- Stanley SK, McCune JM,Kaneshima H,et al. Human immunodeficiency virus infection of the human thymus and disruption of the thymic microenvironment in the SCID-hu mouse. J Exp Med. 1993;178:1151-63.
- Rosenzweig M, Clark DP, Gaulton GN (1993) AIDS.Selective thymocyte depletion in neonatal HIV-1 thymic infection. 1993;7:1601-1605.
- Gaulton GN, Scobie JV, Rosenzweig M. HIV-1 and the thymus. AIDS. 1997;11:403-14.
- Su L,Kaneshima H,Bonyhadi M, et al. HIV-1-induced thymocyte depletion is associated with indirectcytopathogenicity and infection of progenitor cells in vivo. Immunity. 1995;2:25-36.
- McCune JM. Thymic function in HIV-1 disease. SemImmunol. 1997;9:397-404.
- Ho Tsong Fang R, Colantonio AD, Uittenbogaart CH. The role of the thymus in HIVinfection: A10 year perspective. AIDS. 2008;22:171-84.
- Gaulton GN. Viral pathogenesis and immunity within the thymus. ImmonolRes. 1998;17:75-82.