Case Report - Journal of Cardiovascular Medicine and Therapeutics (2018) Volume 2, Issue 1
Pseudo-normalization of deep T-wave inversions in a patient with apical hypertrophic cardiomyopathy when presenting as apical ballooning syndrome.
- *Corresponding Author:
- Hiten Patel
Department of Cardiology
St Joseph’s Regional Medical Center
New York Medical College
Paterson, New Jersey, USA.
Tel: +1 914-594-4000
E-mail: hiten0409@yahoo.com
Accepted on March 10, 2018
Citation: Patel H, Vasudev R, Rampal U, et al. Pseudo-normalization of deep T-wave inversions in a patient with apical hypertrophic cardiomyopathy when presenting as apical ballooning syndrome. J Cardiovasc Med Ther. 2018;2(1):1-4.
Abstract
Differential diagnosis of T wave inversions in anterolateral leads includes acute coronary syndrome, intracranial hemorrhage or apical hypertrophic cardiomyopathy (HCM). Later is a rare variant of HCM that usually involves the apex of the left ventricle. Takotsubo cardiomyopathy (TCM) or transient left ventricular (LV) apical ballooning syndrome is a clinical entity mimicking an acute coronary syndrome and characterized by reversible LV dysfunction that is frequently precipitated by a stressful event either emotional or physical stress. We present a case of a 48 year old male with apical HCM that developed TCM causing pseudo-normalization of the baseline T wave inversions. Through this case authors suggest that TCM can cause apical ballooning and can mask the typical ECG changes as seen in patients with apical HCM.
Keywords
Apical hypertrophic cardiomyopathy, HCM, Takotsubo cardiomyopathy, TCM, Pseudo-normalization, ECG, Masking.
Introduction
T wave inversions in anterolateral leads on electrocardiogram (ECG) are typically seen in acute coronary syndrome, intracranial hemorrhage or apical hypertrophic cardiomyopathy (HCM). Later is a rare variant of HCM that usually involves the apex of the left ventricle and is characterized by giant T wave inversions usually >10mm deep on ECG. Takotsubo cardiomyopathy (TCM), also known as stress-induced cardiomyopathy or transient left ventricular (LV) apical ballooning syndrome, is a clinical entity mimicking an acute coronary syndrome and characterized by reversible LV dysfunction that is frequently precipitated by a stressful event either emotional or physical stress. We present a case of a 48-year-old male with a history of depression that developed TCM masking typical ECG features of apical HCM.
Case Report
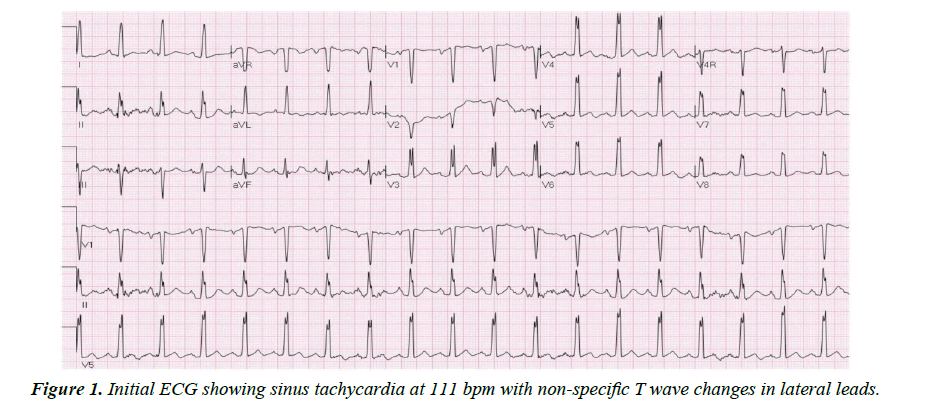
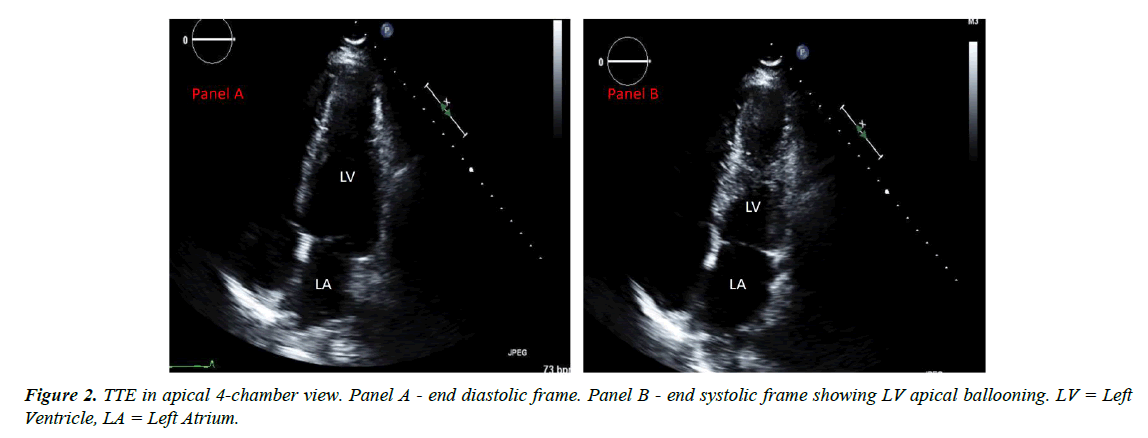
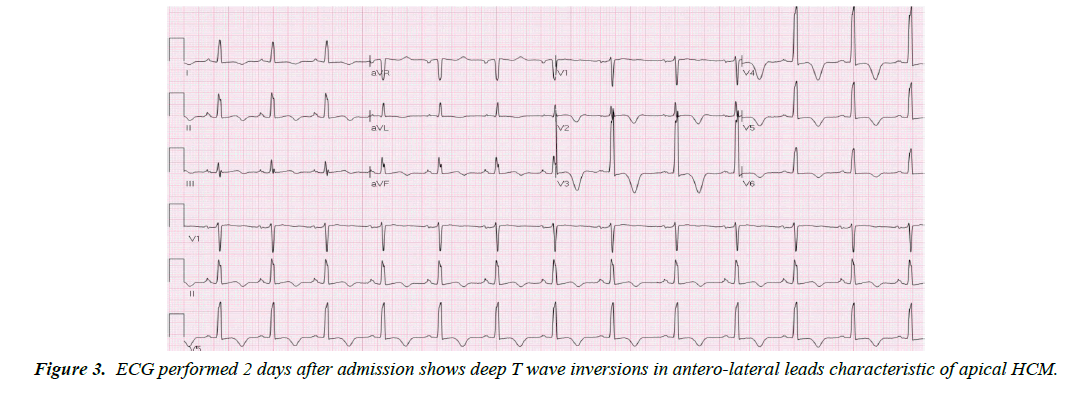
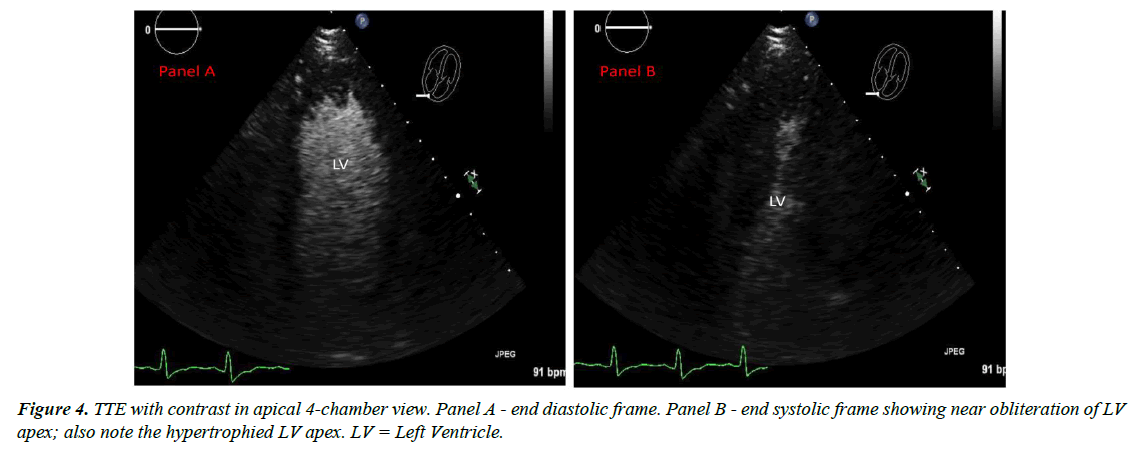
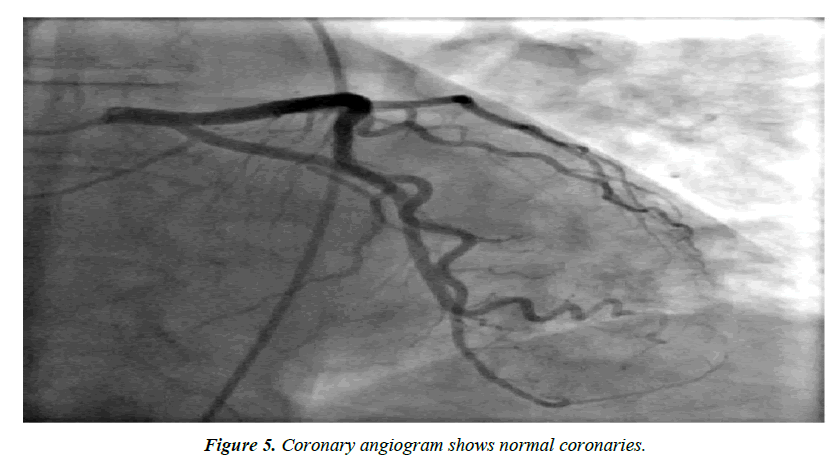
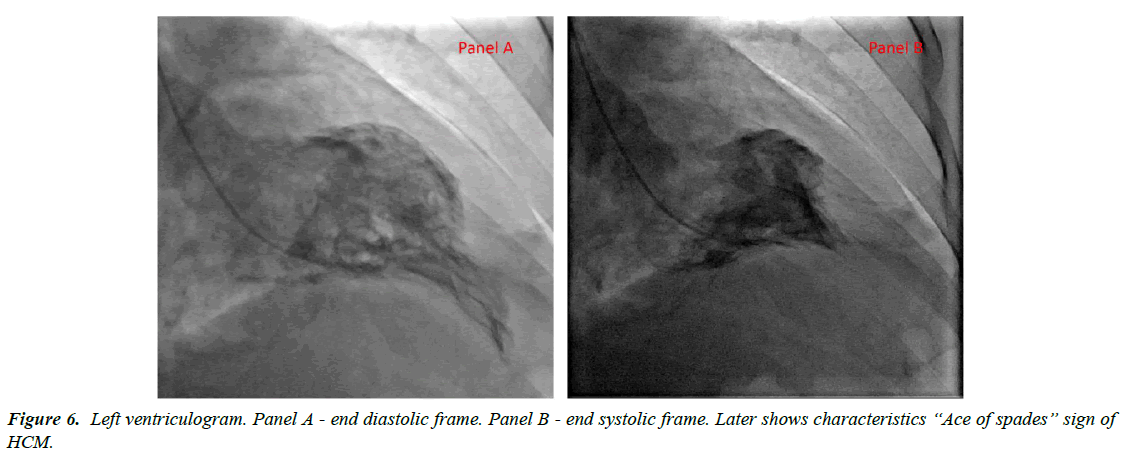
A 48-year-old Asian male with past medical history of major depression was brought to the hospital as he was found to be obtunded and unresponsive after a suspected suicide attempt. He was intubated for airway protection. Home medications were paroxetine, buspirone and alprazolam; there was empty bottle of alprazolam lying beside him. Subsequently it was known that he had a fight with his wife. There was no family history of cardiomyopathy or sudden cardiac death. Initial vitals: blood pressure 168/98mmHg, heart rate 114 bpm, temperature 98.8ᵒF, respiratory rate of 27/min and oxygen saturation 97%. Physical examination was benign. Initial ECG (Figure 1) showed sinus tachycardia at 111 bpm with nonspecific T wave changes. CT head was negative for any acute intracranial pathology and laboratory findings were normal including three sets of troponin. Urine and serum toxicology screen was negative for any benzodiazepines. Telemetry ECG monitoring throughout the hospitalization showed no ventricular arrhythmias. Initial transthoracic echocardiogram (TTE) showed LV wall motion abnormality involving mid antero-septal, mid anterior and apical walls (apical ballooning) with borderline ejection fraction (EF) of 45% (Figure 2). After 2 days, ECG (Figure 3) revealed deep T wave inversions in antero-lateral leads that is characteristic of apical HCM. TTE with contrast the same day revealed resolution of LV wall motion abnormality and hypertrophied LV apex (Figure 4). Later that day, patient’s coronary angiography showed normal coronaries (Figure 5), which suggest patient presented with apical ballooning syndrome secondary to his emotional stress. Left ventriculogram showed extensive apical hypertrophy and overall hyperkinesia with the “Ace of Spades” sign characteristic of HCM (Figure 6). Patient was treated medically; he recovered fully and was discharged home. Two months after discharge, ECG still showed characteristic deep T wave inversions in antero-lateral leads as seen in apical HCM, which were masked on initial (admission) ECG by apical ballooning syndrome.
Discussion
Apical HCM (Yamaguchi syndrome) is a rare variant of HCM, historically found in Japanese population. In Japan, it constitutes 15-25% of all cases of HCM whereas it is only seen in 1-3% of Non-Asian population [1]. It has an autosomal dominant inheritance pattern caused by mutation in one of nine genes encoding sarcomere proteins and it more commonly affects younger men. It is characterized by giant T wave negativity (usually > 10 mm deep) on the ECG and a spade like configuration of the LV cavity on left ventriculography [2]. On TTE with contrast, there is asymmetric LV hypertrophy predominantly involving the apex. MRI is considered gold standard to differentiate hypertensive LV hypertrophy and HCM [3] but it was contraindicated in our patient due to prior metal implant. Apical HCM usually has good long term prognosis [4].
On the other hand, TCM or apical ballooning syndrome is characterized by reversible LV regional wall-motion abnormality in the absence of obstructive CAD, pheochromocytoma, and myocarditis. Patients are typically post-menopausal women who present with clinical, ECG, and biochemical features of an acute coronary syndrome usually after intense emotional and/or physical stress [5]. Our patient is a male and about 10% of patients presenting with TCM are males. Depression, anxiety and antidepressant use among other factors like genetic predisposition can induce catecholamine production and lead to direct myocyte injury and microvascular dysfunction that might increase susceptibility to TCM [6,7]. TCM can be complicated with cardiogenic shock, LV thrombus or ventricular arrhythmias [8]; however, LV dysfunction is transient and prognosis is usually better.
Conclusion
There are only few case reports of TCM affecting the apical HCM [9] suggest that TCM can cause apical ballooning in patients with apical HCM especially if the apical hypertrophy is mild (apical wall thickness of < 15 mm). And it is unknown whether apical HCM patients with greater wall-thickening at the apex would also show apical ballooning with stress-induced myocardial stunning. However, our patient has apical thickness of 15 mm, so he was susceptible to developed TCM. Differential diagnosis of deep T wave inversions in anterolateral leads on ECG includes acute coronary syndrome, any intracranial hemorrhage or apical HCM. Our patient presented with TCM and the initial EKG showed normal upright T waves, suggesting pseudo-normalization of T waves which masked the deep T wave inversions characteristic of apical HCM. To our knowledge this is the first case of stress induced cardiomyopathy causing pseudo-normalization of the baseline T wave inversions as seen in apical HCM.
Stress induced cardiomyopathy can cause apical ballooning and can mask the typical ECG changes as seen in patients with apical hypertrophic cardiomyopathy.
References
- Kitaoka H, Doi Y, Casey SA, et al. Comparison of prevalence of apical hypertrophic cardiomyopathy in Japan and the United States. Am J Cardiol. 2003;92:1183-186.
- Yamaguchi H, Ishimura T, Nishiyama S, et al. Hypertrophic non-obstructive cardiomyopathy with giant negative T waves (apical hypertrophy): ventriculographic and echocardiographic features in 30 patients. Am J Cardiol.1979;44:401-12.
- Sipola P, Magga J, Husso M, et al. Cardiac MRI assessed left ventricular hypertrophy in differentiating hypertensive heart disease from hypertrophyc cardiomyopathy attribuable to a sarcomeric gene mutation. Eur Radiol. 2011;21:1383-389.
- Klarich KW, Jost ACH, Binder J, et al. Risk of death in long-term follow-up of patients with apical hypertrophic cardiomyopathy. Am J Cardiol. 2013;111:1784-791.
- Prasad A, Lerman A, Rihal CS. Apical ballooning syndrome (tako-tsubo or stress cardiomyopathy): a mimic of acute myocardial infarction. Am Heart J. 2008;155:408-17.
- Corrigan FE, Kimmel MC, Jayaram G. Four cases of Takotsubo cardiomyopathy linked with exacerbations of psychiatric illness. Innov Clin Neurosci. 2011;8:50-53.
- Vasudev R, Rampal U, Patel H, et al. Selective serotonin-norepinephrine reuptake inhibitors-induced Takotsubo cardiomyopathy. N Am J Med Sci. 2016;8:312-15.
- Patel H, Rampal U, Vasudev R, et al. Cardiomyopathy and an Acute Stroke: What is the role of anticoagulation? J Heart Stroke. 2017;2:1030.
- Roy RR, Hakim FA, Hurst TR, et al. Two cases of apical ballooning syndrome masking apical hypertrophic cardiomyopathy. Tex Heart Inst J. 2014;41:179-83.