- Biomedical Research (2015) Volume 26, Issue 4
Prevalence of postpartum depression in an urban setting
Maria Ahmad1, Maryam Shabbir Butt2, Bilal Umar3, Hafiz Sheraz Arshad4*, Nayab Iftikhar5, Umer Maqsood6
1Children Hospital & Institute of Child Health Lahore maria_ahmad27@hotmail.com
2Riphah College of Rehabilitation Sciences, Riphah International University, Lahore maryambutt85@hotmail.com
3Riphah College of Rehabilitation Sciences, Riphah International University, Lahore dptbilal@gmail.com
4Azra Naheed Medical College, Department of Physical Therapy, Main Raiwind Road,, Lahore drhafizsheraz@gmail.com
5Riphah College of Rehabilitation Sciences, Riphah International University, Lahore speechpathologist88@gmail.com
6Azra Naheed Medical College, Department of Physical Therapy, Main Raiwind Road,, Lahore Umer.maqsood@gmail.com
- *Corresponding Author:
- Hafiz Sheraz Arshad
Department of Physiotherapy
Azra Naheed Medical College
Superior University
17 KM Raiwind Road
Lahore, Pakistan
Accepted : July 02 2015
Abstract
Women undergo various physical and mental changes during their postpartum period and are in a vulnerable state of mind. Some women may not cope with these situations as better than others and consequently they undergo a depressive state known as postpartum depression. It is a debilitating disorder and should be screened at an early stage to avoid long term adverse effects. The objectives of this study were to quantify the prevalence of postpartum depression in an urban setting where literacy rate is higher and medical facilities are readily available. This observational cross sectional study was performed in National Hospital, Lahore and Fatima Memorial Hospital, Lahore and was accumulated at RCRS Lahore. Study was accomplished in 4 months after the ratification of synopsis. Non-probability, purposive sampling was used. Sample size was calculated to be of 88 women. Self-administered questionnaire consisting of validated 10 items, Edinburgh postnatal depression scale (EPDS) [1] was employed to detect depression among women living in an urban setting. The grand mean of all the 10 items of Edinburgh postnatal scale was 6.7 ± 2.6 SD. The grand mean of question number 10 was calculated to be 2.37 ± 3.48 SD which shows that most women hardly ever thought about committing suicide. The results depicts that prevalence of postpartum depression in an urban setting is very low. The association between age, postnatal week, educational level and socioeconomic status states that depression most commonly occurs in undergraduate adolescents belonging to lower class families and peeks in their third postnatal week. The prevalence of postpartum depression is quite low in urban settings. This shows that the depressive states are avoided in better literate and socioeconomic statuses. Women are more capable of coping with new challenges and their families are better apt of supporting them through this period.
Keywords
Postpartum depression, urban setting, prevalence, Edinburgh postnatal depression scale
Introduction
Pregnancy and childbirth is the most beautiful phase in a women`s life filling her with the contentment of the ability to nurture a new living being. However some women could not cope with the jumble of emotional upsurges and tend to undergo various sentimental disturbances through their childbearing episode resulting in despair and melancholy. The average profusion rate of this debilitating postpartum mood affliction, estimated using an authentic measure, is 13% [2]. A study declared that up to 50% of the cases of postpartum depression go unperceived [3].
Postpartum depression [PPD) usually begins within four weeks of childbirth and may continue for several months or even a year [4]. Sadness, guilt, anxiety, emptiness, social abolition, deeming oneself insubstantial in taking care of the baby, sleeping and eating disorders are some promising manifestations of PPD [5]. The major contributor of this disorder is hormonal imbalance which starts occurring in a woman immediately after delivery of the baby. The imbalance between estrogen and progesterone causes severe baby blues. Stressful life events such as abuse, poverty, poor relationships, death of a loved one or looking after a dependant family member can trigger depression. With an overabundance of persistent life hassles, women may feel incapable to cope with the over and above demands of pregnancy.
Along with the immense pleasure of having a baby comes sleepless nights and irregular feeding schedules which enhance the stress both physically and emotionally [6]. The ill health of the baby may add insult to injury and the mother may start feeling reckless and inept. Studies have suggested that mothers of preterm, very low birth weight infants may be at increased risk for psychological distress postpartum [7]. Clinical observation has also suggested that mothers of temperamentally demanding infants have expressed signs of despair and inadequacy [8].
Lack of education plays a vital role in development of depressive disorders. Illiteracy leads to lack of awareness of the various changes a woman will bear through this period and so the sudden challenge of looking after an infant is over whelming. Illiteracy also hinders the provision of adequate medical facilities to women who undergo postpartum depression. Families are unable to recognize symptoms and no help is sought. Lack of social support, poor marital status and unintended pregnancies are also contributing factors of post partum depression [9].
Infants are highly sensitive to their interpersonal environment but depressed mothers are inconsistent in childcare and have poor coping strategies. The developmental progress of a newborn is undermined consequently of this disruption of normal infant engagements with the mother. Some severely distressed mothers may even have infanticidal thoughts and approximately 4% of them do slay their children [10].
This study aimed at quantifying the prevalence of postpartum depression in an urban setting.
It is hypothesized to be low due to better literacy rate and socioeconomic status. Early recognition of this disorder and consequently demolition is very crucial for the sake of healthy mother infant relationship as there is growing evidence that new mothers and their entire families are shattered due to it.
The Primary objectives are
• Estimate the prevalence of depressing symptoms in women soon after delivery.
• Highlight the incidence of depression in women during childbirth in an urban and developed setting.
The Secondary objectives are
• To identify the causative factors of postpartum depression.
• To assess the level of various factors like age, education, postnatal week and socioeconomic status and their effect in causing depression.
Rationale
The rationale of the study is to improve the health of patients of depression after postpartum
Materials and Methods
Study Design
It was a descriptive cross sectional study.
Setting
National hospital Lahore and Fatima memorial hospital Lahore
Study Population
Women in their 1st puerperium month were included and so were those who have undergone miscarriage or still births
Duration of Study
Study was completed 4 months after the approval of synopsis
Sample size
Data from 88 women was taken Sample size was calculated by the following formula
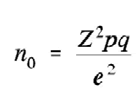
Where Confidence level = 95%
For 95% Confidence levelZwas1.96
p ( proportions/Confidence interval) =10%
q= 1-p, e= half width of the desired interval
Eligibility
Inclusion Criteria
• Women in their 1st puerperium month
• who have undergone miscarriage
• who have undergone still births
Exclusion Criteria
• diagnosed history of depression
• had a recent death
• widow or divorced
Data collection
This method was created by Cox et al. to screen for postpartum depression as well as antenatal depression. It consists of 10 items with a grand total of 30 points. For each query, women were asked to choose one of the four responses that most closely describe how they have felt over the past 7 days. Each response has a range between 0 and 3. Women scoring more than 10 points were considered depressed. Women were asked to check the response that comes closest to how they have been feeling in the previous 7 days. The overall EPDS score was computed as the mean of the scores for the 10 items. Sensitivity for the identification of major depression in pregnancy has been found to be >95% with a specificity of >95% at this cut-off point. Question 10 was given special consideration as it was regarding suicidal thoughts and hence a deciding factor of presence of depressive disorder.
Ethical consideration
The administration, ethical committee and Department of Medical Education of National hospital Lahore and Fatima memorial hospital Lahore approved to conduct the study in Hospital. Only those patients were included in the study who signed the written consent. All the personal information of participants were kept hidden
Statistical Procedure
All collected data was entered in computer programme SPSS version 20 and analyzed through this software. Mean ± standard deviation were calculated for quantitative variable while frequency (%) was used for qualitative variable. Total agreement score of Edinburgh Postnatal Depression Scale (EPDS) tool was calculated and Mean ± Standard deviation for agreement on individual attributes in EPDS tool was also be calculated.
Results
Discussion
Postpartum depression is a widespread disorder that engulfs countless women into its darkness and despair. Its prevalence varies from region to region but its occurrence is a known fact as well as its debilitating effects. It is significant that we investigate its prevalence in our society so that appropriate measures can be taken to avoid its occurrence and treat the effected.
In Pakistan very few studies have been carried out in this regard and are mostly concerning the rural or socioeconomically lower areas. In those areas postpartum depressive symptoms are understandable as the mother goes through so many life stressors. This study aims at the detection of PPD in urban areas where its occurrence is seldom heard of and usually thought to be nonexistent due to better living environment and health facilities. Cultural mindset also poses hindrance in our cognition of presence of such a disorder as child birth is thought to be a huge blessing and a festive occasion.
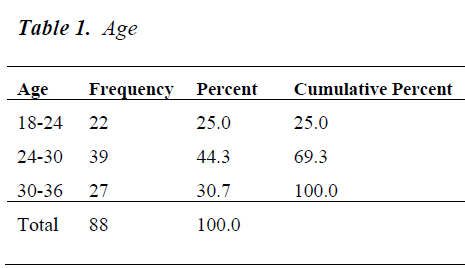
Among the women participating in this study 22 (25%) were aged between 18 to 24, 39 (44%) between 24 to 30 and 7 (30%) between 30 and 36.
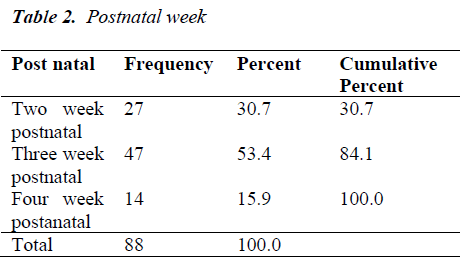
27 women were in their second postnatal week, 47 were in third and 14 in fourth postnatal weeks.
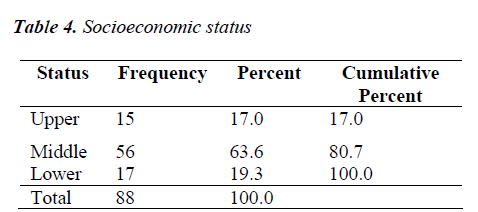
Socioeconomically, 63% of these women belonged to middle class families. 17% from upper class and only 19% from lower class families.
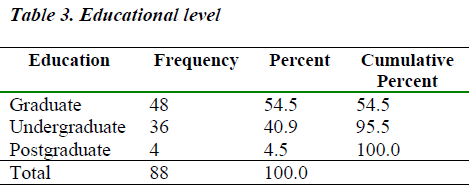
As it was an urban setting literacy rate was also quite commendable with 54% graduate women, 4% postgraduates and around 40% undergraduates.
The depressive symptoms were measured using the Edinburgh postpartum depression scale, a 10-item self-report scale. This instrument was designed by Cox et al. to screen for postpartum depression. It is the most widely used screening questionnaire for postpartum depression and has been widely validated for not only this condition but also antenatal depression. For every item, women are asked to opt one of the four responses that most closely describe how they have felt over the past 7 days. Each response has a value between 0 and 3. Scores for the 10 items are added to give a total score between 0 and 30. We chose to regard an EPDS score greater than 12 as indicating depression. Although a number of cut-off points have been used, sensitivity for the identification of major depression in pregnancy has been found to be >95% with a specificity of >95% at this cut-off point.
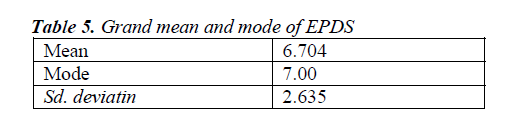
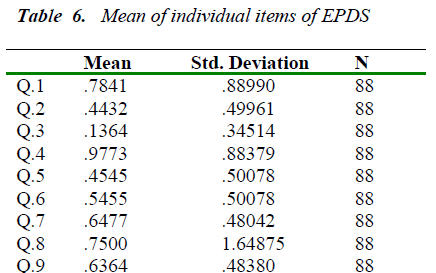
The mean of individual items of EPDS was calculated as shown in table 6. The grand mean of EPDS was calculated to be 6.7 ± 2.64 SD. Mode was 7 which indicates that most women who participated in this study were not depressed. The prevalence of PPD enumerated by this study was very low.
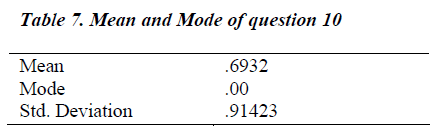
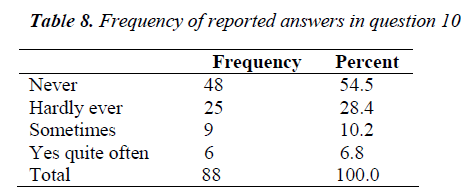
Question no. 10 of EPDS holds special significance as it inquires of any suicidal thoughts that might have occurred to these women. The grand mean of this question was calculated to be 0.693 ± 0.914 SD. Mode was 0 which indicates that most women never thought of committing suicide (Table 7). According to the frequencies show in table 8, 48 women never had suicidal thoughts. 25 hardly ever thought of it, 9 gave it a thought sometimes but only 6 contemplated it often.
After deliberating the results it came became evident that only 6 women out of 88 had their EPDS scores above 1 and were depressed. This shows that prevalence of postpartum depression according to this study is 6.8% (Table 9)
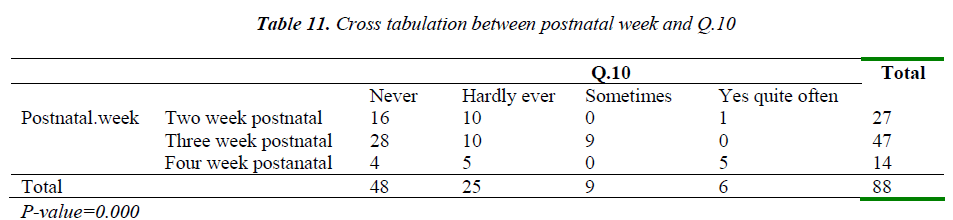
Table 10 shows association between age and depression depicting that adolescents undergo more depression than older women. Similarly table 11 shows association of postnatal week with depression and uncovers that women undergo more depression their third postnatal week.
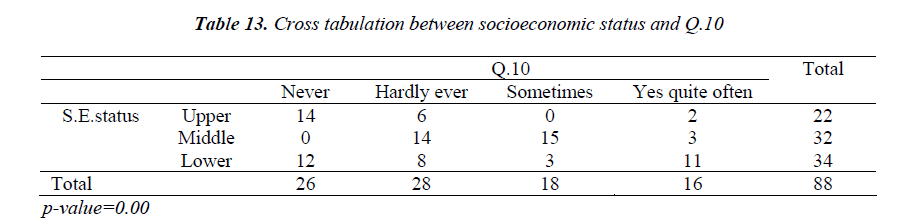
Tables 12 and 13 indicate that undergraduate women tend more towards committing suicide and they usually belong to lower class families.
The limiting fact of this study is that this cross sectional study was done only once with a small sample size. The concealment of emotions by women themselves is a hindrance in compiling proper results. The unavailability of reporting women in the gynecological and psychiatry departments of the hospitals where this study was conducted and further the dishonest attempt of the questionnaire provided. Despite the above mentioned facts, women are still unwilling to disclose their personal feelings of melancholy just to avoid their weakened mental state and their incompetence as a parent
References
- Cox JL, Jolden JM, Sagovsky R. Detection of postpartumdepression - development of the 10-item Edinburgh Postnatal Depression Scale. British Journal of Psychiatry, 1987; 150: 782-786
- O’Hara MW, Swain AM..Rates and risk of postpartum depression-A meta-analysis.International Review of Psychiatry 1996; 8: 37-54.
- Beck CT. The effects of postpartum depression on maternal- infant interaction: A meta-analysis. Nursing Research.1995; 44: 298-304.
- Miller LJ. Postpartum depression. JAMA 2002; 287 (6): 762-765.
- Spinelli MG. Postpartum psychosis: Detection of risk and management. American Journal of Psychiatry 2009; 166(4): 405-408.
- Wendland-Carro J., Piccinini CA, Millar WS. The role of an early intervention on enhancing the quality of mother - infant interaction.Child Development.1999; 70: 713-721.
- McCoy SJ, Beal JM, Shipman SB, Payton ME, Watson GH. Risk factors for postpartum depression: a retrospective investigation at 4-weeks postnatal and a reAhmad/ view of the literature. J Am Osteopath Assoc. 2006;106 (4): 193-198.
- Cutrona CE, Troutman BR. Child Development 1986; 57(6): 1507-1518
- Leathers SJ, Kelley MA. Unintended pregnancy and depressive symptoms among first-time mothers and fathers. American Journal of Orthopsychiatry, 2000; 70 (4): 523
- Sit D, Rothschild AJ, Wisner KL. A review of postpartum psychosis. J Womens Health (Larchmt) 2006; 15: 352-368