Original Article - Journal of Public Health Policy and Planning (2018) Volume 2, Issue 2
Pediatric maxillofacial injuries in madinah - a retrospective study
Hasan Albeshir*, Sayed Waheed Ahmed, Mashael Awaji, Saeed Albalawi, Mahmood Samman, Hani AlahmadiDepartment of Oral Maxillofacial Surgery, King Fahad Hospital, Madinah, Kingdom of Saudi Arabia
- Corresponding Author:
- Hasan Albeshir
King Fahad Hospital, Madinah, Saudi Arabia
Tel: +964 (3) 647 662
E-mail: mindsreader122@gmail.com
Accepted date: April 09, 2018
Citation: Albeshir H, Ahmed SW, Awaji M, et al. Pediatric maxillofacial injuries in madinah - a retrospective study. J Public Health Policy Plann. 2018;2(2):73-80.
Abstract
Objective: The objective of this retrospective study was to analyze the incidence, etiology and distribution pattern of maxillofacial injuries in the pediatric patients of King Fahad Hospital, Madinah. Method: Medical records of 865 pediatric patients were reviewed from 2014 to 2017. Relevant data in relation to demographics, age and sex, etiology/mechanism of injury, pattern and distribution of injuries were collected. The data was analyzed and results were compared with other studies. Results: The 0 to 6 years age group was commonly involved; peak incidence was at the age of five years. 360 soft tissue injuries were found in pediatric males and 178 in females whereas, 153 hard tissue injuries were documented in males and 69 in female patients. Laceration was the most common maxillofacial soft tissue injury (507) with a high frequency of 94% followed by Contusion 4% (20) and Dermabrasion 2%. Majority of lacerations were of the lips followed by those of the tongue, gingiva and face. Dental injuries constituted 59.45% of hard tissue injuries and 17.36% of the overall maxillofacial trauma in 132 pediatric patients. Avulsion injury in 56 children was most frequent and a majority of the affected teeth were lost. Dento-alveolar #'s were found in 5 cases (m: 4; f: 1) and Maxillo- Facial bone fractures in 85 (m: 6l; f: 24) children. Fractures of the Mandible were most common and majority of these were condylar fractures. Conclusion: There is a need at a national level for a public, parent and teacher education program on childcare and safety. Ambulance personnel and school teachers should be trained and licensed for basic 'On site' first aid procedures in dental and maxillofacial trauma.
Keywords
Pediatric, Maxillofacial injuries, Fall, Laceration, Avulsion, Mandible, Fracture.
Introduction
Trauma is the leading cause of morbidity and mortality due to craniofacial trauma among children because of their greater cranial-mass-to-body ratio: 8:1 at birth compared to 2.5:1 in adulthood [1]. Pediatric maxillofacial injuries are frequent and trauma can occur either with low velocity (fall, sport, violence) or high velocity (MVA, Pellet). The occurrence of both hard and soft tissue maxillofacial injuries is often attributed to the children’s high level of physical activity, decreased supervision and tendency towards risk-taking behavior and other factors.
Soft tissue injuries are more common than fractures in children who have sustained facial trauma, particularly in younger children whose facial skeletons are resistant to fracture. Dento-alveolar and soft tissue injuries account for majority of the pediatric maxillofacial injuries but the frequency of facial fractures is considerably low accounting for 1% to 14.7% of all facial fractures. They are less common, more often undisplaced or minimally displaced than in adults [2-4].
The reduced incidence of facial fractures in children when compared to adults is probably due to the flexibility of the facial bone, lack of pneumatization of the paranasal sinuses and protection of the malar region by the prominent buccal pad of fat in infants [5]. Facial fractures in children may be complicated by a disturbance of normal dental development, especially during the deciduous and mixed dentition phases. However, a spontaneous correction of occlusal malalignment may occur in children as the deciduous teeth are shed and replaced by permanent teeth [6]. Causes of fracture are closely linked with age-related levels of activity and vary depending on the data source [7].
The diagnosis of facial fractures in children is difficult and such fractures are frequently underreported. Plain radiographs are difficult to interpret in children and therefore CT which provides diagnostic details is commonly utilized [8].
There is a paucity of information regarding maxillofacial injuries in pediatric patients of Saudi Arabia and none so far from the holy city of Madinah, which in addition to the local population receives a huge number of pilgrims with their children from across the world.
The aim of this research was to perform a retrospective study to analyze the incidence, pattern and distribution of maxillofacial injuries in pediatric patients seen by the Department of Oral and Maxillofacial surgery, King Fahad Hospital, Madinah Kingdom of Saudi Arabia.
Materials and Methods
The pediatric age group in various countries has been taken to range from 0 to 21 years with infancy, between birth and 2 years, childhood from 2 to 12 years and adolescents from 12-21 years [9]. The age limit of pediatric medicine, in Saudi Arabia, is from 0 to 12 years of age in most of the pediatric hospitals and clinics [10] and hence the pediatric age in this study was defined as 12 years and below.
This study included 865 Pediatric patients aged 12 years or below including 531 male and 334 females brought with maxillofacial injuries to the King Fahad Hospital, Madinah in the retrospective period of three years from 2014 to 2017. There were 790 Saudis and 75 Non Saudi children. The patients were subdivided into two age groups namely 0 to 6 and 6 to 12 years of age for ease of study and comparison. There were 490 children in 0-6 age group and 375 in the 6 to 12 years age group.
Their Medical records, Plain radiographs including OPG and CT scan were reviewed.
Relevant data was collected in relation to the following:
1) Demographics, Age and Sex
2) Etiology/ mechanism of injury – MVA, fall, sport, violence
3) Type of injuries:
A) Soft tissue injuries – Dermabrasion, Contusion, Laceration, Skin loss
B) Hard tissue injuries –
1) Tooth injury – Avulsion, Crown #, Root #, Intrusion, Extrusion, Displacement, Subluxation
2) Dentoalveolar #’s
3) Facial bone #’s:
• Mandible
• Maxilla
• Zygoma
• Frontal
• Nasoethmoid
• Orbital
• Nasal bone
4. Site pattern and distribution of injuries
5. Associated injuries
The data was statistically analyzed using SPSS version 19. Relevant tables and graphs were made using Microsoft word.
Results
Age
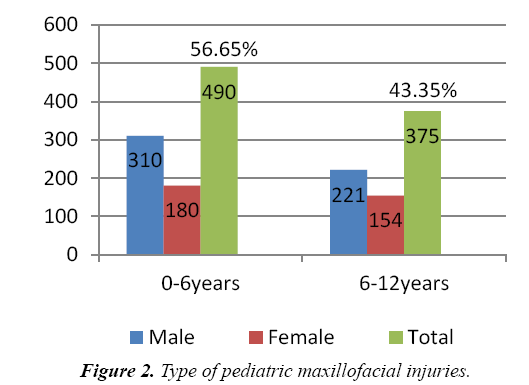
There were 531 males and 334 girls with an M: F ratio of 1.6:1. 490 patients were in the age group of 0-6 years and 375 patients in 6-12 years age group. Children in the 0 to 6 age group were frequently involved. The highest incidence was seen at the age of five years and commonly in boys.
Etiology
The most common cause for the pediatric maxillofacial injuries in this study was due to fall with a very high frequency of 89.71% (776). Only 8.20% (71) of the trauma was due to MVA followed by violence/abuse in 1.38% (12) and sport 0.46% (4). One child had a dog bite injury to the cheek and another sustained a pellet injury to the forehead.
A highly significant correlation was found between the Age group of 0-6 years and fall as the etiology whereas, no significance was seen between this age group and MVA. The Age Group of 6-12 years demonstrated a highly significant correlation with both MVA as well as fall in the etiology of pediatric maxillofacial injuries in this study. (P=0.001)
A significant correlation was found between Male gender and MVA followed by fall and Violence whereas; a highly significant correlation was seen between Female gender and fall followed by RTA in the etiology of pediatric maxillofacial injuries in this study (P=0.001).
Type of MF injury
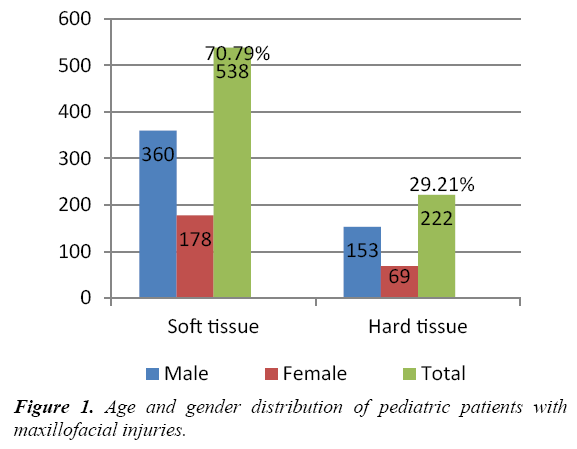
There were a total of 760 pediatric oral and maxillofacial injuries with 538 soft tissue injuries (71%) and 222 (29%) of the hard tissue injuries. 360 soft tissue injuries were found in pediatric males and 178 in females whereas, 153 hard tissue injuries were documented in males and 69 in female patients.
Hard tissue injuries
A total of 222 hard tissue injuries of teeth and facial bones were seen; 153 injuries in males and 69 in female patients.
I) Pediatric Dental Injuries: 132 Pediatric Dental Injuries (PDI) were found in our study; 88 in boys and 44 in girls. The PDI constituted 59.45% of the hard tissue injuries and 17.36% of the overall maxillofacial trauma.
II) Dento-alveolar Fracture – 5 cases (m: 4; f: 1) – 2.25% of hard tissue injuries
III) Facial bone fractures – 85 (m: 6l; f: 24) - 38.28% of hard tissue trauma and 11.18% of the overall pediatric maxillofacial injuries:
1) Mandible fractures – 60 fractures of mandible were found in 24 patients (m: 17; f: 7) 43 fractures in males and 17 mandible fractures in female children.
IV) Associated Injury
Discussion
Age
The first peak in frequency of pediatric facial fractures is reported to occur at 6-7 years, associated with school attendance. The second peak noted at 12-14 years, is related to increased physical activity and participation in sports during puberty and adolescence [5,6]. The highest incidence of pediatric maxillofacial injury was noted by us at the age of five years
In this study, pediatric oral maxillofacial injuries were most commonly found in the 0 to 6 years age group with 490 patients (56.64%) compared to 375 (43.35%) in the 6 to 12 years age group (Table 1 and Figure 1). In contrast to our observation, many studies have reported majority of maxillofacial injuries in the 6 to 12 years and above age [11,12]. Soft tissue injuries were more numerous in the younger age group compared to those of hard tissue trauma and facial fractures in the older patients which is in concurrence with other authors [13-16].
| Age Group | Males | Females | Total | Percentage |
|---|---|---|---|---|
| 0-6 years | 310 | 180 | 490 | 56.64% |
| 6-12 years | 221 | 154 | 375 | 43.35% |
| 531 | 334 | 865 | 100 |
Table 1: Age and gender distribution of pediatric patients with maxillofacial injuries.
Gender
Pediatric maxillofacial injuries were found to occur in a large number of boys (531) compared to girls (334) (Table 2) with an M: F ratio of 1. 6:1.The literature from other countries presents a varying male-to-female ratio ranging from 1.1:1 to 8.5:1, depending on the series. The preponderance of boys is attributed mainly to the fact that their physical activity is more intense and more hazardous than that of girls [2,3,5,7]. The lesser number of girls in this study may be due to a largely conservative sociocultural environment in the kingdom where girls are protected and under careful supervision more than boys. There is little opportunity for the female children to indulge in sports and physical activities which may put them at a risk of injury. It is well established in the case of facial fractures, that, the male patients outnumber their female counterparts in all age groups worldwide. Differences in gender-related fracture incidence are often attributed to more frequent involvement in sports, physical activity and dangerous behavior among boys [17,18].
| Etiology | Male | Female | Total | Frequency | |
|---|---|---|---|---|---|
| 1. | Fall | 455 | 321 | 776 | 89.71 % |
| 2. | MVA/RTA | 062 | 009 | 71 | 08.20% |
| 3. | Violence/Abuse | 009 | 003 | 12 | 01.38% |
| 4. | Sport/Games | 003 | 001 | 04 | 00.46% |
| 5. | Animal Bite | 001 | 000 | 01 | 00.11% |
| 6. | Pellet Injury | 001 | 000 | 001 | 00.11% |
| Grand Total | 531 | 334 | 865 | 100 |
Table 2: Etiology of pediatric maxillofacial injuries.
Etiology
Oral and maxillofacial soft and hard tissue injuries can occur due to a spectrum of causes ranging from fall, motor vehicle accidents, sports, abuse, animal bites and other incidents. Causes of pediatric facial fracture vary, depending on the data source and are closely linked with age-related levels of activity [5-7].
The most common cause for the pediatric maxillofacial injuries in this study was due to fall with a very large frequency of 89.71% (776). Our results are in agreement with several other studies from across the world. [2,5,17,18]. Only 8.20% (71) of the trauma in our study was due to MVA, second ranking to falls which is at variance from many reports that found MVA as the most common cause for pediatric maxillofacial injury [19,20]. Falls and MVA were followed by violence/abuse in 1.38% (12) and sport 0.46% (4) as the causes of maxillofacial injuries amongst the patients in our study (Table 3). The progressive maturation of motor coordination and balance as the young child grows, learns to walk and run results in more falls on the ground or from height. Patients below 6 years of age are subject to low velocity trauma such as from fall and are likely to sustain soft tissue injuries to the lips, tongue and face whereas older children are more prone to high velocity injury from MVA and sustain facial fractures [16].
| Type of OMF Injury | Male | Female | Number | Percentage |
|---|---|---|---|---|
| Soft tissue injuries | 360 | 178 | 538 | 71% |
| Hard tissue injuries | 153 | 069 | 222 | 29% |
| Total | 513 | 187 | 760 | 100 |
Table 3: Type of pediatric maxillofacial injuries.
A significant number of falls documented in our study, seem to occur and patients brought to the Emergency in the late hours of night at a time when children are ideally required to be asleep. This reflects a faulty habit and lack of consideration on this aspect by the parents who often are out at night along with their young children.
Half of all injuries in battered children (especially in infants and children younger than 5 years) are injuries to the head and neck [2,7]. Facial fractures have been reported to occur in 2.3% of child-abuse victims [21]. Repeated injuries, multiple injury sites, or questionable circumstances surrounding the injury should raise suspicion of possible abuse [22]. Violence/Abuse injury cases found in 1.38% (12) of patients in our study was more than those with sport injury. The figure in our study may be underreported because of cultural and family restraints, fear of law and reprisal in Saudi Arabia. There is a need for monitoring home environment, family counseling, child welfare and legal reprimand.
Type of maxillofacial injuries
In our study 360 soft tissue injuries were found in pediatric males and 178 in females whereas; 153 hard tissue injuries were documented in males and 69 in female patients. Soft tissue injuries – A wide variety of pediatric injuries represent a combination of mechanism, force and anatomic features unique to the child's stage of development [23]. Soft tissue injuries are more common than fractures in children who have sustained facial trauma, particularly in younger children whose facial skeletons are resistant to fracture [24,25] (Figure 2). Dentoalveolar and soft injuries account for majority of the pediatric maxillofacial injuries but the frequency of facial fractures is considerably low [2,19,23,25]. Soares et al. [26] have reported a high prevalence of soft tissue injury (STI) in their study sample; the lesions were more common in boys and in patients aged 0-3 years.
Our study has revealed that maxillofacial soft tissue injuries were most common with 538 (71%) soft tissue injuries compared to those of the teeth and facial bones 222 (29%). Out of 865 pediatric patients, 360 pediatric soft tissue injuries were found in males and 178 in females whereas, 127 hard tissue injuries were documented in males and 107 in female patients (Table 4). Laceration constituted the largest number of soft tissue injury in this study and was found in 507 patients with a high frequency of 94.23% followed by Contusion (20) 3.71% and Dermabrasion (10) 1.85%. This is in concurrence with the findings of other authors [19,27].
| Type of Injury | Male | Female | Total | Frequency | |
|---|---|---|---|---|---|
| 1. | Dermabrasion of Face | 009 | 001 | 010 | 1.85% |
| 2. | Contusion of the Face | 014 | 006 | 020 | 3.71% |
| 3. | Laceration of the Face | 034 | 012 | 046 | 8.55% |
| 4. | Laceration of cheek inner | 007 | 003 | 010 | 1.85 % |
| 5. | Laceration of the Lips Upper Lip Lower Lip Commissure |
059 062 004 |
024 039 001 |
189 083 001 005 |
35.13% |
| 6. | Laceration of the Tongue | 098 | 057 | 155 | 28.81% |
| 7. | Laceration of Gingiva | 039 | 019 | 058 | 10.78% |
| 8. | Laceration of Palate | 016 | 007 | 023 | 4.27% |
| 9. | Laceration of Vestibule | 017 | 009 | 026 | 4.83% |
| 10. | Puncture (pellet) injury | 001 | 000 | 001 | 0.18% |
| Grand Total | 360 | 178 | 538 | 100 |
Table 4: Type of pediatric maxillofacial soft tissue injuries. Lacerations were highest in frequency - 507 patients (94.23%).
The Lips were most frequently lacerated and more commonly involved the lower lip in 101 patients (m: 62; f: 39) compared to the upper lip seen 83 (m: 59; f: 24) Laceration at the Commissure was found in 5 children (m: 4; f: 1).
Intra-orally, Laceration injury of the Tongue was most frequently found affecting 155 children (m: 98; f: 57) followed by Gingival laceration seen in 58 patients (m: 39; f: 19); Laceration of the Vestibule was noted in 26 patients (m: 17; f: 9) and that of the palate (hard/soft) in 23patients (m: 16; f: 7).
Laceration of the face was found in 33 patients (m: 25; F: 8). One child had a dog bite to the cheek while another had a single puncture (pellet entry wound) in the forehead. Neither injury of the parotid duct or facial nerve nor any avulsive skin loss was seen with the facial lacerations.
Early diagnosis of pediatric soft tissue injuries, definitive treatment and good postoperative wound care is necessary for proper healing which helps to decrease adverse scars. Animal bites require confirmation of rabies status, thorough wound exploration and irrigation and prompt closure of the linear aspects of the wound. Puncture wounds should be irrigated to their depths, kept open and seen frequently to detect infection [28].
Dental Hard tissue injuries – In this study, pediatric patients suffered 132 Dental injuries (m: 88; f: 44) (Table 5). A majority 56 (42.42%) of these were permanent tooth avulsion in 39 male and 17 female children who were in the 6-12 years age group. One tooth was found avulsed in 45 patients, two teeth in 8 and three teeth in 3 pediatric patients.
| Dental Injury | Male | Female | Total | Frequency | |
|---|---|---|---|---|---|
| 1. | Tooth Avulsion | 39 | 17 | 56 | 42.42% |
| 2. | Crown Fracture | 11 | 3 | 14 | 10.60% |
| 3. | Intrusion | 15 | 06 | 21 | 15.90% |
| 4. | Subluxation | 23 | 18 | 41 | 31.06% |
| Total | 88 | 44 | 132 | 100 |
Table 5: Type of pediatric dental injuries.
Avulsion is a serious dental injury due sudden trauma causing dislodgement of the tooth out of the socket and injuring its supporting tissues. The child is liable for esthetic and functional impairment with psychological implications. Fall was the most common cause of dental avulsion in our study and more frequently seen in boys compared to girls. This is consistent with other reports even though literature data on the relationship between dental avulsion and gender/age are divergent [29]. Proclined maxillary incisors and incompetent lips increase their vulnerability to traumatic injury and avulsion. The upper permanent central incisors were more frequently found avulsed in this study and total mean number of teeth avulsed was 1.25. Most of the pediatric patients with dental avulsion injury were between 9-11 years of age. Our findings are in agreement with those reported by other authors [30-32].
Unfortunately, 52 (92.85%) of the pediatric patients with dental avulsion injury or the parents/attenders did not bring the avulsed tooth/teeth. This revealed a sad lack of awareness in a majority or inability to locate/retrieve the avulsed tooth from the scene of injury. Only 4 patients had their avulsed tooth/teeth replanted.
Avulsion injury can occur at home, road, school or elsewhere with witnesses and ‘near or on site’ replantation and atleast early transport would be beneficial. However, Lack of awareness, insufficient knowledge regarding the method or means of transport of the tooth, panic from bleeding and urgency to shift injured child to hospital are some reasons given by patients/ parents in our study for not replanting or retrieving the avulsed tooth/teeth from the site of injury. According to literature, abandoned attempt of replantation is more common, ranging between 48.38% up to 70%. [33,34]. As per IADT guidelines, immediate replantation already at the scene of the injury is the best treatment strategy, although it does not guarantee a longterm maintenance of the tooth in the oral cavity [35].
Subluxation is defined as an injury to the tooth's supporting structures with abnormal loosening without tooth displacement. Traumatic subluxation with mobility of teeth was seen in 41 children (31.06%) with 23 males and 18 females. This was followed by Intrusion injury in 21 (15.90%) patients including 16 male and 5 females. Crown fractures without exposure of pulp was noted in 14 patients (10.60%) with 11 male and 3 females. Dentoalveolar fractures were diagnosed in only 5 patients (m: 4; f: 1).
Facial bone fractures
A total of 85 fractures of the pediatric facial bones were diagnosed in this retrospective study constituting (9.26%) of the total children (865) with maxillofacial injuries. Most of the fractures were in boys 71.76% (61) compared to females 28.23% (24) Majority of fractures was that of the mandible found in 60 patients (70.58%) (Table 6).
| Facial Bone | Male | Female | Total | Percentage |
|---|---|---|---|---|
| Mandible | 43 | 17 | 60 | 70.58% |
| Maxilla | 03 | 01 | 04 | 4.70% |
| Orbital fractures | 08 | 02 | 10 | 11.76% |
| Zygoma | 04 | 02 | 06 | 7.05% |
| Frontal bone | 02 | 01 | 03 | 3.52% |
| Nasal fractures | 02 | 00 | 02 | 2.35% |
| Total | 62 | 23 | 85 | 100 |
Table 6: Pediatric maxillofacial facial bone fractures. Most of the fractures were in boys 72.94% (62) compared to females 28.23% [23].
Pediatric Maxillofacial fractures are relatively uncommon and constitute 1% to 15% of all facial bone fractures showing different clinical features when compared with adult patients. The flexibility of the facial skeleton in children, relative protection offered by lack of pneumatization of paranasal sinus and the protection of malar region by prominent buccal fat pad contribute to reduce the frequency of these fractures [36].
Fractures of the mandible
In this retrospective study, out of 85 facial bone fractures in 24 pediatric patients (m: 17; f: 7), 60 fractures were those of the mandible, being the most common accounting for 70.58% of the facial bone fractures. This is in accordance with other reports in the literature [37-39]. Our finding is in disagreement with studies wherein mid face fractures were reported as being more common or nasal fractures as being the most prevalent type of facial fracture among children of all ages [2,5]. The highest frequency of fracture of the mandible was at the Condylar site (50%) which was followed by that of the Parasymphysis (21.6%); Symphysis (13.3%); Body (10%) and Angle (3.3%). There was only one case of fracture of the Ramus and no Coronoid fractures (Table 7).
| Anatomical Site | Male | Female | Total | Frequency | |
|---|---|---|---|---|---|
| 1 | Symphysis | 06 | 02 | 08 | 13.33% |
| 2 | Parasymphysis | 08 | 05 | 13 | 21.66% |
| 3 | Body of the mandible | 04 | 02 | 06 | 10% |
| 4 | Angle of the mandible | 01 | 01 | 02 | 3.33% |
| 5 | Ramus | 01 | -- | 01 | 1.66% |
| 6 | Condylar site | 23 | 07 | 30 | 50% |
| Total | 43 | 17 | 60 | 100 |
Table 7: Site of pediatric mandible fractures.
Condylar fractures
The condylar site was the most common mandibular fractured site found in our study; seen in 30 children with a frequency of 50% comparable to 14.5%-60% reported in the literature [2,5,6,37]. The highly vascularized pediatric condyle and thin neck are poorly resistant to impact during fall which results in the condylar region to be the most commonly fractured site of the mandible. Fracture of the condylar head, medial pole and compression injury is more common in children unlike lower condylar neck fractures seen in the adults [40].
Condylar site injuries have serious implications for the TMJ and normal growth of mandible. Undiagnosed condylar fractures may lead to TMD, Ankylosis and contribute up to 10% of skeletal dentofacial deformities later in the child. Panoramic radiographs or a Towne view will be useful for initial diagnosis while CT helps to determine whether the condyle is dislocated from the TMJ fossa, to evaluate the degree of displacement, and to locate fragments [5]. There were 12 isolated condylar fractures and 18 combined with a fracture site elsewhere in the mandible. Among the combined condylar fractures eleven were unilateral and only seven were bilateral condylar #’s which have been reported to occur more often by other authors [8].
Fracture of maxilla
Maxillary fractures occur infrequently in the pediatric population: They account for only 1.2 to 20% of pediatric facial fractures, and they virtually do not occur in children younger than 2 years. Le Fort fractures (at all levels) are almost never seen before the age of two years. Their prevalence increases as the maxillary sinuses develop and the permanent teeth erupt, usually around the age of 5 years and it peaks at the age of 13 to 15 years. Four patients in our study had fracture of maxilla with Leforte-3 # in only one patient and anterolateral wall fracture of the maxillary sinus in three cases reflecting fewer incidences which is in accordance to that cited in the literature. [17,18,20].
Fracture zygoma
It was found in 6 (m: 4; f: 2) patients with a frequency of 7.05% in our study. This differs from the observation of Adams et al. who mention that amongst the midface fractures which although rare in children, zygomatic complex fractures are reported to be most frequent [18]. In children, zygomatic complex fractures often are greenstick fractures involving the lateral wall and floor of the orbit without displacement or functional defect, such as diplopia.
Orbital fractures
10 orbital fractures were found, mostly in boys. Fracture of the orbital roof was found in six, while fracture in the floor of the orbit was noted in four patients. Orbital fractures occurred with a frequency of 11.76% in our study whereas in other reports they constituted 20% of pediatric facial fractures. The orbital fractures result from transmission of force either directly from the orbital ring to the thin orbital walls or due to indirect, hydraulic pressure effect of displaced orbital soft tissues. Orbital roof fractures are comparatively more frequent in the very young below the age of 6 years before frontal sinus development. However, due to maxillary sinus expansion beyond the equator of the globe, orbital floor fractures are more common in older children. The age at which the probability of an orbital floor fracture exceeds that of orbital roof fracture is 7 years [2,18,41,42].
Frontal bone fractures
Below age 2, infants more commonly sustain injuries to the frontal region which are usually isolated, non-displaced fractures caused by low-impact/low-velocity forces [2,18,21,23]. Fractures of the frontal bone in young children are common because of the prominence of the forehead, which overhangs the face [2,18,42]. In addition to the durability of this bone, the infrequency of frontal sinus injury in children is due to the fact that full sinus development does not occur until age 5 or 6 and the incidence of frontal sinus fractures increase after puberty. Until the age of 6, children rarely sustain injury penetrating into the frontal sinus. Posterior wall fractures of the frontal sinus are associated with leakage of CSF and a high risk of brain injury and neurosurgical intervention.
Nasal bone fractures
The nasal bones are the least resistant and most prominent bones in the facial skeleton and often fractured although the nasal cartilage is compliant. The nasal fracture may be easily missed because of significant local edema and poor patient compliance during initial examination. The pediatric septum is more prone to injury than the nasal bones because it is more rigid, held very tightly in place by the perichondrium and surrounding bone. Undiagnosed and untreated Nasal septal injuries and septal hematoma can lead to airway obstruction and midfacial growth abnormalities in pediatric patients [2,5,7].
Nasal fractures are reported to be the most common type accounting for approximately half of all pediatric facial fractures [2,5] but we found only two patients with nasal bone fractures in total contrast to that reported in the literature. This could be due to the fact that in the city of Madinah, dedicated ENT services are available in another hospital facility. Patients with isolated ENT related injuries and epistaxis are taken there directly. Secondly, many nasal fractures are diagnosed and treated in an outpatient setting or a private clinic which possibly explains a low frequency (2.35%) of nasal fractures in our study.
Associated injuries
390 patients (45.08%) from a total of 865 in this study were documented to have associated injuries. Most of these were in boys (306) compared to girls (84) (Table 8). Associated injuries with pediatric facial fractures reported in the literature vary widely in the range of 10%-88% depending on the type of facial fracture [2,3,5,6]. The most common associated injuries in cases of midfacial and mandibular fractures are reported to be neurocranial injuries [5,6]. In our study also a majority of associated injuries were head injuries (310) with mild to moderate degree head injury in 269 patients associated more with fall and 41 patients had severe head injury associated more with an etiology of MVA.
| Type of Associated Injury | Number | Percentage |
|---|---|---|
| Neurocranial (Head) injuries | 310 | 79.48% |
|
||
|
||
| Fracture Clavicle | 14 | 3.58 |
| Fracture radius | 09 | 2.30 |
| Fracture Ulna | 07 | 1.79 |
| Fracture Femur | 12 | 3.07 |
| Fracture Tibia | 05 | 1.29 |
| Hand injuries | 11 | 2.82 |
| Blunt Abdominal trauma | 13 | 3.33 |
| Chest Injury | 09 | 2.30 |
| Total | 390 | 100 |
N - 390 (45.08%) m: 306; f: 84
Table 8: Type of pediatric associated injuries.
Conclusion
Pediatric Maxillofacial injuries were seen in a large number of boys compared to girls with an M: F ratio of 6.1: 1. Fall was the main cause of traumatic injuries in 90% of the patients. Soft tissue injuries were more common compared to those of the hard tissues.
Lacerations occurred with the highest frequency and the lips were most commonly affected. Dental hard tissue injuries were more in frequency than fractures of the facial bones. Tooth Avulsion injury was most frequent and a majority of the affected teeth were lost. Fractures of the Mandible were vey frequent among facial bone fractures and majority of these were condylar fractures.
There is a need at a national level for a public, parent and teacher education program on child care and safety. Ambulance personnel and school teachers should be trained and licensed for basic ‘On site’ first aid procedures in dental and maxillofacial trauma.
This study is done in one of the holiest cities that are recognized by around 1.6 billion Muslims all over the world. according to the National Transformation Program in Saudi Arabia, the number of Haj pilgrims from both inside and outside the Kingdom, is expected to go up by 2020 to 2.5 million, an annual increase of up to 13 percent and 15 million Umrah visitors will reach the Kingdom, a 30 percent increase over the current 6 million this year. This expansion can increase pediatric trauma in this city can be considered a good model for other cities.
References
- Wymann NE, Holzle A, Izuka T. Pediatric craniofacial trauma. J Oral Maxillofac Surg. 2008;66:58-64.
- Haug RH, Foss J. Maxillofacial injuries in the pediatric patient. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;90(2):126-34.
- Holland AJ, Broome C, Steinberg A, et al. Facial fractures in children. Pediatr Emerg Care. 2001;17:157-60.
- Kambalimath HV, Agarwal SM, Deepashri H, et al. Maxillofacial injuries in children: A 10 year retrospective study. J Maxillofac Oral Surg. 2013;12(2):140-4.
- ZimmermannCE, Troulis MJ, Kaban LB. Pediatric facial fractures: Recent advances in prevention, diagnosis and management. Int J Oral Maxillofac Surg 2006;35(1):2-13.
- Ferreira PC, Amarante JM, Silva PN (2005) Retrospective study of 1251 maxillofacial fractures in children and adolescents. Plast Reconstr Surg 115(6):1500-8.
- Faust RA, Younes AA, Gottlieb W, et al. Maxillary fractures in children. WebMD. 2006.
- Mukherjee CG, Mukherjee U. Maxillofacial trauma in children. Int J Clin Pediatr Dent 2012;5(3):231-6.
- Hardin AP, Hackell JM. AAP committee on practice and ambulatory medicine. Age limit of pediatrics. Pediatrics. 2017;140(3):e2017-51.
- Al-Mobaireek KF. Pediatric pulmonology services in Saudi Arabia: Past, present and future. Ann Thorac Med. 2013;8(4):181-2.
- Alcalá-Galiano A, Arribas-García IJ, Martín-Pérez MA, et al. Pediatric facial fractures: Children are not just small adults. Radiographics. 2008;28(2):441-61.
- Rahman RA, Ramli R, Rahman NA, et al. Maxillofacial trauma of pediatric patients in Malaysia: A retrospective study from 1999 to 2001 in three hospitals. Int J Pediatr Otorhinolaryngol. 2007;71(6):929-36.
- Roslan A, Roszalina R, Normastura A, et al. A maxillofacial trauma of pediatric patients in Malaysia: A retrospective study from 1999 to 2001 in three hospitals. Int J Pediatr Otorhinolaryngol. 2007;71:929-36.
- Rafaela S, Ingrid O, Luis P, et al. Maxillofacial injuries in a group of Brazilian subjects under 18 years of age. J Appl Oral Sci. 2009;17(3):195-8.
- Ogunlewe M, James O, Ladeinde A, et al. Pattern of pediatric maxillofacial fractures in Lagos, Nigeria. Int J Paediatr Dent. 2006;16:358-62.
- Hawramy FA. Maxillofacial trauma among children below 15 years in Sulaimani city/Iraq. Kufa Med J. 2011;14(1):225-30.
- Baumann A, Troulis MJ, Kaban LB, et al. Pediatric oral and maxillofacial surgery, Philadelphia, PA: Saunders. 2004;425-40.
- Adams CD, Januszkiewcz JS, Judson J, et al. Changing patterns of severe craniomaxillofacial trauma in Auckland over eight years. Aust N Z J Surg. 2000;70:401-4.
- Verma S, Verma RK, Shukla B, et al. Maxillofacial trauma in paediatric and adolescent patients. J Dent Med Sci (IOSR-JDMS). 2016;15(4):80-6.
- Muraoka M, Nakai Y, Nakagawa K, et al. Fifteen year statistics and observation of facial bone fracture. Osaka City Med J. 1995;41:49-61
- Kaban LB. Diagnosis and treatment of fractures of the facial bones in children. J Oral Maxillofac Surg. 1993;51:722-9.
- Cole P, Kaufman Y, Hollier LH, et al. Craniomaxillofac trauma reconstr. 2009;2(2):77-83.
- Gassner R, Tuli T, Hachl O, et al. Craniomaxillofacial trauma in children: A review of 3,385 cases with 6,060 injuries in 10 years. J Oral Maxillofac Surg. 2004;62(4):399-407.
- Oginni F, Fagade J, Akinwande, et al. Pattern of soft tissue injuries to the oro-facial region in Nigerian children attending a teaching hospital. Int J Paediatr Dent 2002;12:201-6.
- Idia S, Matsuya T. Pediatric maxillofacial fractures: Their aetiological characters and fracture patterns. J Craniomaxillofac Surg. 2002;30:237.
- Soares TR, Barbosa AC, Oliveira SN, et al. Prevalence of soft tissue injuries in pediatric patients and its relationship with the quest for treatment. Dent Traumatol. 2016;32(1):48-51.
- Bankole OO, Fasola AO, Denloye OO. Oro-facial soft tissue injuries in Nigerian children: A five year review. Afr J Med Sci. 2004;33(2):93-7.
- Hogg NJV, Horswell BB. Soft tissue pediatric facial trauma: A review. J Can Dent Assoc. 2006;72(6):549-52.
- Karayilmaz H, Kirzioglu Z, Gungor OE, et al. Aetiology, treatment patterns and long-term outcomes of tooth avulsion in children and adolescents. Pak J Med Sci. 2013;29(2):464-8.
- Tzigkounakis V, Merglova V, Hecová H, et al. Retrospective clinical study of 90 avulsed permanent teeth in 58 children. Dent Traumatol. 2008;24(6):598-602.
- Ade JS, Gomes BP, Zaia AA, et al. Relationship between clinical-radiographic evaluation and outcome of teeth replantation. Dent Traumatol. 2008;24:83-188.
- Andreasen JO, Borum MK, Jacobsen HL, et al. Replantation of 400 avulsed permanent incisors: Factors related to pulpal healing. Endod Dent Traumatol. 1995;11(2):59-68.
- Petrovic B, Marković D, Peric T, et al. Factors related to the treatment and outcomes of avulsed teeth. Dent Traumatol. 2010;26:52-9.
- Kinoshita S, Kojima R, Taguchi Y, et al. Tooth replantation after traumatic avulsion: A report of 10 cases. Dent Traumatol. 2002;18:153-6.
- [No Authors Listed]. Guidelines for the management of traumatic dental injuries. Int Assoc Dent Traumatol. 2007.
- Cardenas JLM, Olate S, Asprino L, et al. Pattern and treatment of facial trauma in pediatric and adolescent patients J Craniofac Surg. 2011;22:1251-5.
- Karim T, Khan AH, Ahmed SS. Trauma of facial skeleton in children: An Indian perspective. Indian J Surg. 2010;72: 232-5.
- Qudah MA, Bataineh AB. A retrospective study of selected oral and maxillofacial fractures in a group of Jordanian children. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;94:310.
- Imahara SD, Hopper RA, Wang J, et al. Patterns and outcomes of pediatric facial fractures in United States: A survey of the National Trauma Data Bank. J Am Coll Surg. 2008;207:710-6.
- Tiwana PS, Vickers A. In current therapy in oral and maxillofacial surgery. Mandibular Condyle Fractures. 2012.
- Gussack GS, Luterman A, Powell RW, et al. Pediatric maxillofacial trauma: Unique features in diagnosis and treatment. Laryngoscope. 1987;97:925-30.
- Dodson TB, Kaban LB. California mandatory seat belt law: The effect of recent legislation on motor vehicle accident related maxillofacial injuries. J Oral Maxillofac Surg.1988;46:875-80.