Research Article - Current Pediatric Research (2018) Volume 22, Issue 3
Parental perception of cleft lip in Kuwait.
Abdulaziz AlRashid*, Hisham BurezqIbn Sina Hospital, Kuwait
- Corresponding Author:
- Abdulaziz AlRashid
Plastic Surgery, Al-Babtain Centre for Burns and Plastic Surgery Ibn Sina Hospital
Sabah Health Region, Kuwait
Tel: 0096594426640
Email: a.alrashid@hotmail.co.uk
Accepted date: September 12th, 2018
Abstract
Background: Cleft Lip (CL) and Cleft Palate (CP) are one of the most common and immediately recognizable craniofacial malformations worldwide, forming the fourth most common congenital anomalies among newborns. Current research evidence suggests that cleft lip/palate CL/CP is caused by a combination of both environmental and genetic risk factors. CL is repaired at 3 months of age in most centers, including the one used for the study, Al-Babtain Centre for Burns and Plastic Surgery, where the infant is of an appropriate size and weight. Cleft palate (CP) is repaired at a later time, often between 9 and 12 months of age. The country of Kuwait was the focus of this research study, where the mean incidence of CL at the time was established to be 1.48 per 1,000 births. The incidence of CL/CP confers significant financial burden and psychological pressure on patients’ families. A survey was conducted to assess levels of public knowledge and awareness regarding CP and CL, its management and associated risk factors. Method: A retrospective cross-sectional survey of CL +/- CP patients (CL(P)) under the age of 8 who have undergone CL surgical repair between the ages of 3 and 6 months during 2010 until 2017, at Al-Babtain Centre for Burns and Plastic Surgery in Kuwait. All participants have received full orthodontic treatment prior to undergoing CL surgical repair. A total of 261 participants were surveyed. The response rate was 38% (100/261). The survey was of an open-ended nature. Results were tabulated according to preconceived questions and later expressed as percentages. Results: More than half of the participants (54/100) have not heard of CL/CP prior to having an affected child. Quarter of parents (25/100) felt it was appropriate to have CL surgically repaired between the ages of 1 and 3 months; more than half of parents (63/100) felt it was best to operate between the ages of 3 and 6 months; and only 12% of parents (12/100) thought it was best to operate between the ages of 6 and 12 month. Almost all patients (91/100) were satisfied with the aesthetic outcome of CL surgery. More than three-quarter of parents (81/100) demonstrated an understanding for the need for feeding support via specialized feeding bottles and correct positioning whilst feeding a child affected with an orofacial cleft. 82% of patients (82/100) were actively engaged in post-operative follow-up. Over half of the participants (54/100) were aware that their children may require subsequent operations to CL repair as part of CL sequelae treatment, whilst 37% of parents (37/100) felt that CL was a heritable condition that could be passed onto offspring. Conclusion: The present survey showcased key knowledge gaps about CL/CP amongst caregivers, limiting the standard of care to CL patients. Such limitation could be addressed by media campaigns aimed at increasing public awareness of orofacial clefts. This could be delivered via conventional routes such as: television; radio; billboards; and leaflets, or through social media, a more contemporary platform with a high adoption rate amongst teenagers in Kuwait. The establishment of specialized antenatal cleft clinics could overcome any uncertainty amongst caregivers, thus raising the general level of orofacial cleft awareness.
Keywords
Cleft lip; Parental perception; Kuwait.
Introduction
Cleft Lip (CL) and Cleft Palate (CP) are the most common and immediately recognizable craniofacial malformations in the world, being the fourth most common congenital anomalies among newborns. It is a multi-factorial condition, thought to be a result of genetic and environmental factors. CL +/- CP (CL(P)) incidence varies by ethnicity, affecting approximately 1 per 500 births in those with Asian, Latin American, and Native American ancestry, but only 1 in 2,500 people of African ancestry [1,2]. In Europe, the mean incidence is 1.36 in 1,000 whilst in Kuwait the incidence is 1.48 in 1,000 [3]. Most centers, including the one used for the study, Al- Babtain Center for Burns and Plastic Surgery, follow the conventional 3-month mark repair time for Cleft Lip (CL), whereas cleft palate (CP) is corrected at a later time, often between 9 and 12 months of age [4,5]. The traditional 3 months CL repair time is based on the “rule of 10” principle designed to act as a safety buffer for patients. The said rule was originally created in 1966 by Wilhelmsen and Musgrave, and was later modified by Millard in 1976. Rule of Ten is based on a number of cutoff criteria that include age; weight; leucocyte count; and hemoglobin [6]. At 3 months of age, a baby is generally of adequate weight to be anaesthetized safely and has higher probability of undergoing reconstructive surgical procedures more accurately and successfully [7,8]. Caring for children with CL significantly reduces the quality of life for parents in all aspects especially financially and socially. (CL(P)) has a direct effect on hearing, speech, feeding, and general appearance that could impact negatively on the mother– infant relationship. As a result, affected children are at an increased risk of language development deficit, thus negatively affecting the child’s social integration skills as well as leading to poorer infant development and cognitive function [7]. It has been reported that surgical intervention drastically improves the quality of life for both patients and parents [9,10]. Caring for a child with CL can cause parental anxiety or depressive symptoms. Surgical repair of an obvious orofacial cleft would have a positive psychological impact on the infant-mother relationship, allowing for better child integration within a family [4,8]. In utero intervention for CL repair has been suggested as a potential interventional alternative that could pave the way for scarless healing without disrupting the nasomaxillary growth. This remains to be merely an experimental surgery for the time being, as such intervention carries considerable risks for both, fetus and mother [9].
Method
The present study was a retrospective cross-sectional survey of 100 CL +/- CP patients under the age of 8 that were born between 2010 and 2017 and operated in Al- Babtain Centre for Burns and Plastic Surgery. All patients have received orthodontic care prior to undergoing CL repair. Al-Babtain Centre for Burns and Plastic Surgery is the only specialized burn center in Kuwait, serving 4.5 million people across the country. Study data was collected from surgical logbooks belonging to various reconstructive plastic surgery teams operating in the center between the 2010 and 2017. Patients diagnosed with CL +/- CP and operated between the ages of 3 and 6 months were the primary participants included in this study, with a total of 261 patients meeting the inclusion criteria. All the 261 patient participants were contacted via telephone, and out of the 261 patients, responses were received from 100 patients granting us informed consent to participate in the research study. In addition to gaining a generalized understanding regarding the perception and awareness of CL/CP in Kuwait, the results would demonstrate aspects that would need further improvement and bring it to the attention of relevant healthcare professionals.
Aims
1. Assess the level of patient knowledge regarding multi-disciplinary approach to CL management.
2. Assess cleft lip/palate risk factors and run a comparative study with currently available data in literature. Risk Factors Reviewed: Smoking/ antenatal medication/family or relatives with CL/ CP.
Data Analysis
Data was compiled into a Microsoft Excel Spreadsheet and all responses were pooled into specified categories to achieve a more meaningful outcome. Since the statistical analysis was open-ended in nature, Microsoft Excel and Microsoft Word were used for data analysis and illustrations. Results were tabulated according to preconceived questions and were later expressed as percentages. Data analysis procedures were carried out as illustrated in Figure 1.
Results
Response rate was established to be at 38% from which data was collected over a period of 6 months. A total of 100 participants out of 261 patients who were diagnosed with (CL(P)) and had undergone CL reconstructive surgery between the ages of 3 and 6 months during the period between 2010 and 2017, agreed to take part in this study. As many as 56% (n=56/100) of the participants were male whilst 44% (n=44/100) were female. The mean age for (CL(P)) reconstructive surgery was 5.2 months. The median age for fathers and mothers of (CL(P)) patients at the time of birth was 34.3 and 29.3 respectively. Out of the 100 patients who took part in this survey, 91% (n=91/100) were satisfied with the aesthetic outcome of CL surgery, whereas 9% (n=9/100) of patients were not satisfied with the post-operative outcome.
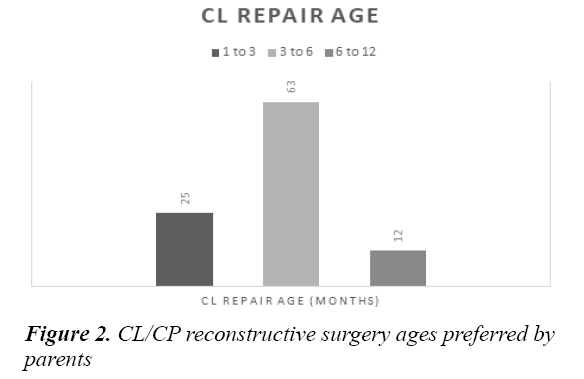
It was noted that 94% of study participants (n=94/100) had CL and no CP, compared with 6% of respondents (n=6/100) who had CL and CP. Considering the quotation of 3 to 6 months of age being the standard surgical time protocol that the medical center follows, 100% of patients (n=100/100) agreed that it was more appropriate for the treating surgeon to decide on the timing of surgery. When parents were asked about their perspective towards the ideal age for CL surgical repair: 25% (n=25/100) felt it was best to operate between the age of 1 and 3 months; 65% (n=63/100) felt it was best to operate between the age of 3 and 6 months; and 12% (n=12/100) felt it was best to operate between the age of 6 and 12 months, as illustrated in the bar graph in Figure 2 below.
Out of the 100 patients surveyed, 39 had at least 1 member of their family diagnosed with CL, while 4 participants had a sibling with CL; 2 participants had a father with CL; none of the participants had a mother identified with CL; 21 participants had a paternal cousin distressed with CL; 11 patients had a maternal cousin with CL; and 1 patient had both paternal and maternal cousins diagnosed with CL as illustrated in Table 1.
| Relative with CL | Number |
|---|---|
| Father | 2 |
| Mother | 0 |
| Sibling | 4 |
| Paternal Cousin | 21 |
| Maternal Cousin | 11 |
| Paternal & Maternal Cousins | 1 |
Table 1: Relatives previously diagnosed with cleft lip
Two mothers (n=2/100) were active smokers during pregnancy, whilst 46 mothers (n=46/100) were passive smokers.
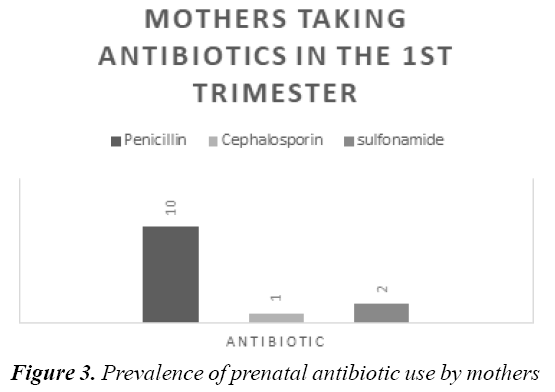
It was noted that 30% (n=30/100) of mothers were taking folic acid by the end of the 1st trimester, while 13 mothers took a course of antibiotics during the 1st trimester. All antibiotics were dispensed from primary care settings. It was also noted that 10% (n=10/100) of mothers were on a penicillin class antibiotic; 2% (n=2/100) were taking a sulfonamide class antibiotic (Trimethoprim); and 1% (n=1/100) were on a cephalosporin-class antibiotic (cefuroxime) in the 1st trimester as depicted by the graph in Figure 3 below.
Majority of the participating parents at a rate of 81% (n=81/100) demonstrated an understanding for the need for feeding support via specialized feeding bottles and correct positioning; while 80% (n=80/100) of parents realized that there was an increased risk for middle ear infection (otitis media). A significant portion of parents at a rate of 82% (n=82/100) followed up the reconstructive surgery of their children with speech and language therapist.
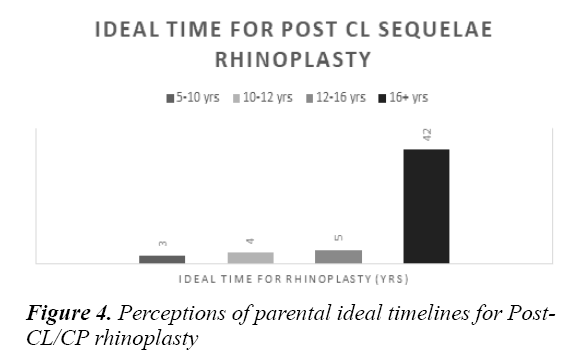
Only 37% of parents thought that (CL(P)) was a hereditary condition and could be passed on to offspring. In addition, 46% of parents stated that their children would not need any subsequent operations, whilst 54% were aware that their children might need subsequent operations, including rhinoplasty as part of post-cleft sequelae. Amongst the 54 parents who recognized the possibility of needing a rhinoplasty at a subsequent stage: majority of parents at a rate of 77.7% (n=42/54) opted for a rhinoplasty when their child turns 16 years old or older; 9.2% of parents (n=5/54) thought it was best to operate between the ages of 12-16 years old; 7.4% of parents (n=4/54) opined that the best age to operate was between 10 and 12 years; and 5.5% of parents (n=3/54) regarded 5-10 years as the correct age for the operation as illustrated by the bar graph in Figure 4 depicted below.
Discussion
CL/CP represents some of the most common orofacial clefts, forming approximately 60% of total head and neck anomalies [10]. Since (CL(P)) is a common congenital malformation, it was important to check patient awareness on (CL(P)) in Kuwait. To the best of our knowledge, no similar study has been previously conducted in the Middle East. Caring for a child with an orofacial cleft can cause negative and mixed feelings amongst parents characterized by: embarrassment; anxiety; guilt; depression; rejection; disappointment; and anger, in addition to imposing additional financial strains on a family [11]. Adult gaze has been previously studied and it was demonstrated that adults were more likely to stare for longer durations at the face of (CL(P)) infants when compared to healthy infants. (CL(P)) infants were also perceived to be less ‘cute’ compared to infants with no (CL(P)) [12]. Since health is defined as a state of physical, mental, and social wellbeing, such perceptions will deteriorate the quality of life for those who are caring for an infant with an orofacial cleft [13]. Data obtained from the research study established that 46% of the total parents were previously aware of CL/ CP. The figure was lower than the 81% reported by a Saudi Arabian study [14].
The discrepancy noted above in awareness rates between the two Middle East countries might be attributed to the existence of public awareness programs in Saudi Arabia and other countries with similar health care systems. Despite significant advancements in science and technology applications in healthcare, there still exists a deficiency of well-established antenatal orofacial cleft clinic in Kuwait aimed at addressing any queries parents might have. The absence of such clinics could heighten caregivers’ reliance on information from sources such as the internet or even superstitious beliefs [15].
The research study established that 81% of parents (n=81/100) were aware of the need for a specialized orofacial cleft feeding bottle placed in an upright feeding position and the possibility of speech disturbance if reconstructive surgery was delayed excessively. Most or 54% participating parents (n=54/100) were aware of the possibility of needing a rhinoplasty in adulthood as part of CL sequelae treatment. Unfortunately, due to the lack of available data of similar nature, it was not possible to evaluate these figures by means of a comparison. Patient speech perception has been correlated with the level of quality of life. Parents and patients often have different perceptions of the quality of speech. Therefore, speech and language input are necessary when evaluating the speech of a child with an orofacial cleft [16]. As per Al-Babtain Centre for Burns and Plastic Surgery protocol, all CL/CP patients were referred post-operatively to speech clinic for speech assessment and Ear, Nose and Throat (ENT) clinic for potential grommet insertion. In our survey, 82% of patients (n=82/100) attended the ENT clinic and 81% (n=81/100) were following up with a speech and language therapist. The following risk factors were identified as being significant contributors to increasing the risk of developing CL/CP in infants.
Smoking
Current data shows that there is a statistically significant association between smoking in early pregnancy and increased incidence of orofacial clefts [17]. It has been reported that maternal passive smoking and active smoking equally result in a 1.5-fold increase in the risk of (CL(P)) [18]. 46% of the surveyed mothers (n=46/100) were passive smokers whilst only 2% were active smokers (n=2/100). These findings are consistent with other studies that reported a positive correlation between passive smoking and orofacial cleft development [19].
Genetics & Consanguinity
Multiple studies have concluded that there was a positive correlation between orofacial clefts and a family with a history of the same disorder. A parent who had an orofacial cleft has a 3-5% risk of having an affected child compared to one that did not manifest the condition at birth [20]. The said risk would reach up to 40% once the first child is diagnosed with CL/CP [21]. A positive family history of a first cousin or a niece/nephew with (CL(P)) increases the risk to the person’s offspring to 0.5% and 1% respectively [22]. Out of the 100 patients surveyed, 39% (n=39/100) had first- or second-degree relatives with the same disorder, suggesting a possible positive heritable factor. None of the patients in our survey had a mother affected with CL, unlike data in the current literature which states that sons of CL/CP mothers have a significantly greater risk of CL/CP compared to daughters of CL/CP mothers [22].
Folic Acid
Both Wilcox et al. [22] and Butali et al. [4] reported that the maternal use of folic acid was found to significantly reduce the risk of (CL(P)) via affecting the proliferative embryonic and fetal cells of the neural crest and tube, but interestingly has no effect on isolated CP/ CL incidences [23,24]. The research study established that 30% of mothers surveyed (n=30/100) were found to have used folic acid regularly in the pre-conceptual period and during the first trimester [25]. The small number of women taking pre-conceptual folic acid could be attributed to unplanned pregnancies, whereas folic acid ingestion needs to be commenced at an early phase of the embryogenesis process [26].
Antibiotics
Certain classes of antibiotics are contraindicated in pregnancy, especially during the first trimester. The research study identified a total of 13 mothers of CL/CP patients who took an antibiotic during the first trimester of their pregnancies, all of which were obtained from primary care service centers. Among the mothers participating in the study, 10 took a penicillin-based antibiotic during the first trimester, 1 mother consumed cefuroxime, and 2 mothers took trimethoprim. Lin et al. (2013) [27], and Merrit (2005) [22] found that taking penicillin in the first trimester increases the risk of developing (CL(P)). On the other hand, Mølgaard et al. [28] found no link between the use of penicillin and CL, with the exception of pivmecillinam which was found to increase the risk of CP. Mølgaard et al. [28] also observed that the use of trimethoprim in the first month of pregnancy significantly increased the risk of (CL(P)). To our knowledge, no association between cephalosporin and (CL(P)) has been established.
Conclusion
The present survey showcased key knowledge gaps about CL/CP amongst caregivers. Additionally, 91% of the patients surveyed indicated that they were satisfied with the aesthetic outcome of the surgery with their family members expressing the same sentiments. Such results could be interpreted as an indicator that most CL patients view surgery as a tool that helps improve their social lives, thus helping to minimize the stigma associated with CL. The existence of such knowledge gaps limits the ideal standard of care to CL patients. Such limitation could be addressed through media campaigns aimed at increasing public awareness, emphasizing the importance of regular post-operative follow up, and promoting health education. It is recommended that government and other professional organizations initiate local media campaigns on social media, a platform with a high adoption rate amongst teenagers in Kuwait. Social media campaigns should be conducted in collaboration with conventional media such as television, radio, billboards and leaflets aimed at raising awareness on (CL(P)). A multi-platform campaign would, in turn, help in developing a more positive attitude towards infants with orofacial clefts. Such campaigns may also highlight the importance of smoking cessation and regular use of folic acid in the pre-conceptual and antenatal phase. A stricter policy on dispensing antibiotics in primary healthcare centers as well as better knowledge on safe antibiotic prescribing in pregnancy is also recommended as a way of limiting (CL(P)) risk factors. The establishment of specialized antenatal cleft clinics could as well overcome such limitations by raising the level of awareness amongst caregivers, in addition to providing a reliable source of information and education opportunities.
References
- Mossey PA, Modell B. Epidemiology of oral clefts: An international perspective. Front Oral Biol 2012; 16: 1-18.
- Emeka CI, Adeyemo WL, Ladeinde AL, et al. A comparative study of quality of life of families with children born with cleft lip and/or palate before and after surgical treatment. J Korean Assoc Oral Maxillofac Surg 2017; 43: 247-255.
- Srivastava S, Bang RL. Facial clefting in Kuwait and England: A comparative study. Brit J Plast Surg 1990; 43: 457-462.
- Slade P, Emerson DM, Freedlander E. A longitudinal comparison of the psychological impact on mothers of neonatal and 3 month repair of cleft lip. Brit J Plast Surg 1999; 52: 1-5.
- Kobus K, Kobus-Zaleśna K. Timing of cleft lip and palate repair. Devel Per Med 2014; 18: 79-83.
- Chow I, Purnell CA, Hanwright PJ, et al. Evaluating the rule of 10s in cleft lip repair: do data support dogma? Plast Reconstr Surg 2016; 138: 670-679.
- Kapp-Simon KA. Psychological issues in cleft lip and palate. Clin Plast Surg 2004; 31: 347-352.
- Jiri B, Jana V, Michal J, et al. Successful early neonatal repair of cleft lip within first 8 days of life. Int J Pediatr Otorhinolaryngol 2012; 76: 1616-1626.
- Lorenz HP, Longaker MT. In utero surgery for cleft lip/palate: Minimizing the ‘‘Ripple Effect’’ of scarring. J Craniofac Surg 2003; 14: 504-511.
- Manyama M, Rolian C, Gilyoma J, et al. An assessment of orofacial clefts in Tanzania. BMC Oral Health 2011; 11: 5.
- Turner SR, Rumsey N, Sandy JR. Psychological aspects of cleft lip and palate. Eur J Orthod 1998; 20: 407-415.
- Rayson H, Parsons CE, Young KS, et al. Effects of infant cleft lip on adult gaze and perceptions of “cuteness”. Cleft Palate Craniofac J 2016; 10: 15.
- World Health Organization. Constitution of the World Health Organization. Geneva: World Health Organization. 2006.
- Alnujaim NH, Albedaie ES, Alyahya LS, et al. Awareness, knowledge and attitudes of Saudi pregnant women towards cleft lip and palate. Curr Pediatr Res 2017; 21: 595-603.
- Oginni FO, Asuku ME, Oladele AO, et al. Knowledge and cultural beliefs about the etiology and management of orofacial clefts in Nigeria's major ethnic groups. Cleft Palate Craniofac J 2010; 47: 327-334
- Bickham RS, Ranganathan K, Wombacher NR, et al. Speech perceptions and health-related quality of life among children with cleft lip and palate. J Craniofac Surg 2017; 28: 1264-1268.
- Little J, Arslan MT, Mossey PA. Smoking and orofacial clefts. A United Kingdom–based case-control study. Cleft Palate Craniofac J 2004; 41: 383-386.
- Sabbagh HJ, Innes NP, Sallout BI, et al. Birth prevalence of non-syndromic orofacial clefts in Saudi Arabia and the effects of parental consanguinity. Saudi Med J 2015; 36: 1076-1083.
- Xuan Z, Zhongpeng Y, Yanjun G, et al. Maternal active smoking and risk of oral clefts: a meta-analysis. Oral Surg Oral Med Oral Pathol Oral Radiol 2016; 122: 680-690.
- Bender PL. Genetics of cleft lip and palate. J Pediatr Nurs 2000; 15: 149.
- Sandberg DJ, Magee WP, Denk MJ. Neonatal cleft lip and cleft palate repair. AORN Journal 2002; 75: 490-498.
- Merrit L. Understanding the embryology and genetics of cleft lip and palate, Advances in Neonatal Care. Adv Neo Care 2005; 5: 64-71.
- Wilcox AJ, Lie RT, Solvoll K, et al. Folic acid supplements and risk of facial clefts: National population based case-control study. BMJ 2007; 334: 464.
- Butali A, Little J, Chevrier C, et al. Folic acid supplementation use and the MTHFR C677T polymorphism in orofacial clefts etiology: An individual participant data pooled-analysis. Birth Defects Res A Clin Mol Teratol 2013; 97: 509-514.
- Lettieri J. Lips and oral cavity. InRE Stevenson, JG Hall, & RM Goodman (Eds.), Human malformations and related anomalies 1993; 367-381.
- Lammer J, Shaw M, Iovannisci M, et al. Maternal smoking and the risk of orofacial clefts: Susceptibility with NAT1 and NAT2 polymorphisms. Epidemiology 2004; 15: 150-156.
- Lin KJ, Mitchell AA, Yau WP, et al. Safety of macrolides during pregnancy. Am J Obstet Gynecol 2013; 208: 221.
- Mølgaard-Nielsen D, Hviid A. Maternal use of antibiotics and the risk of orofacial clefts: A nationwide cohort study. Pharmacoepidemiol Drug Saf 2012; 21: 246-253.