Research Article - Current Pediatric Research (2018) Volume 22, Issue 2
Initial serum level of TNF- α as an outcome predictor in pediatric patient with sepsis
Idham Jaya Ganda*, Yustin Andriani, St. Aizah Lawang, Dasril DaudDepartment of Pediatrics, Faculty of Medicine, Hasanuddin University, Makassar, South Sulawesi, Indonesia.
- Corresponding Author:
- Idham Jaya Ganda
Departement of Pediatrics, Faculty of Medicine, Hasanuddin University
Makassar, South Sulawesi, Jl. Perintis Kemerdekaan Km. 11 Tamalanrea Makassar, 90245
Indonesia
Tel: 62411- 584461
Fax: 62411- 590629
E-mail: unhaspediatrics.hi@gmail.com; dhamjaya_spa@yahoo.com
Accepted date: May 22, 2018
Abstract
Background: Sepsis is the leading causes of morbidity and mortality in critical patients in many intensive care units. TNF-α was the first circulating proinflamatory cytokine to be widely evaluated in sepsis patients. Objective: The aim of this study was to determine the role of TNF-α as an outcome predictor in pediatric sepsis patient. Methods: This prospective cohort study was conducted in Pediatric Intensive Care Unit Wahidin Sudirohusodo hospital from December 2015 until May 2016. A total of 70 sepsis patients were included. Plasma specimens were collected at admission, then the patients were being followed up if the patients develop septic shock or not. The diagnosis of sepsis is using the International Pediatric Sepsis Consensus 2005 criteria. Serum TNF-α was measured using Enzyme Linked Immunosorbent Assay technique. Results: The initial serum levels of TNF-α was significantly increased in both groups, but higher in the septic shock group. Cut off point ≥ 400pg/ml was obtained through the ROC, with the sensitivity 100%, specificity 100%, positive predictive value 100%, and negative predictive value 100%. Conclusion: The initial serum level of TNF-α can be used as a predictor outcome of sepsis patient in children and the limit of level ≥ 400 pg/ml is the most optimal cut off point as a prognostic value.
Keywords
GTNF-α, Sepsis, Predictor
Introduction
Sepsis is a clinical syndrome that triggered by infection which is characterized by a number of clinical symptoms including fever or hypothermia, leukocytosis or leukopenia, tachycardia and tachypnea. Various microorganisms act as infectious agents including bacteria, viruses, fungi, protozoa. Various internal and external factors also determine the occurrence of sepsis. Internal factors that also influential are immune factors and apoptosis. If there is something causes the immune system under pressure, then the individual becomes susceptible to infections. This situation will develop into sepsis or septic shock [1-5].
In a recent study recognized that various proinflammatory cytokines, particularly TNF-α effect on the response to severe infection and sepsis. TNF-α stimulates leukocytes and vascular endothelium to release other cytokines. It also increased the expression of surface molecules and strengthens the neutrophil-endothelial adhesion at the site of infection, increasing the production of prostaglandins and leukotrienes. TNF-α levels are increased in patients with severe sepsis or septic shock [1,6-13]. It is proved by previous studies in other countries which reported that the levels of TNF-α in the serum is more increased in patients with sepsis non survival than in patients with sepsis survival [14-16].
TNF-α production in large quantities can cause intravascular thrombosis, inhibit muscle contractility of heart, lowers blood pressure (shock), vascular dilation, and plasma leakage which then lead to septic shock [17-19]. If the expression of TNF-α occur continuously, mortality of patients with sepsis cannot be avoid. It means that if we can figure out cytokines that influence sepsis, hopefully we can predict the occurrence of shock in a patient. Therefore, it is important to investigate the effects of cytokines as the prognostic value in patients with sepsis.
The management of sepsis by using only anti-microbial was not entirely successful. It have to be noted that just by eliminating microorganisms that cause sepsis was not sufficient and it was proved by the death rate because of sepsis still high [1,20]. TNF-α in moderation plays a role in systemic inflammation, while high amounts are vital to the occurrence of septic shock [17].
Previous study by Kocabas et al. [15] and Bozza et al. [14] state that TNF-α is a good marker for diagnosing sepsis and also to determine prognosis in sepsis patients. If we can predict the outcome of patients with sepsis earlier, the patient can be treated more progressively, so the mortality rate in patients with sepsis can be reduced. Based on the fact above, it needs an approach from biological parameter to identify the role and prognostic value, in this case is TNF-α, which is correlative with sepsis patient’s outcome. Research on biological parameters in sepsis is still rare; study of TNF-α to predict the outcome (shock or no shock) of patients with sepsis in children has not been done before. In addition, research to find the point of intersection levels of TNF-α baseline between patients with sepsis in children who become septic shock and who did not become septic shock has not been done before. So this research is expected to enhance our knowledge to better clinical applications in the future.
Material and Methods
Subjects
This study included children aged 1 month to 18 years who were diagnosed with sepsis during December 2015 to May 2016. Sepsis was defined based on the criteria of the International Pediatric Sepsis Consensus of 2005, which was treated in the Pediatric Intensive Care Unit (PICU) Wahidin Sudirohusodo Hospital [21]. Samples are the entire population that meets the criteria of inclusion and exclusion. Inclusion criteria were patients with sepsis, age 1 month to 18 years, was willing to sign an informed consent agreement. Exclusion criteria were patients with trauma, burns, malnutrition, malignancy, being received corticosteroid treatment and patients with immune deficiency.
Children who meet the inclusion and exclusion criteria and is willing to be a sample (obtain permission from parents) and signed an informed consent agreement. After diagnosis of sepsis, the patient's blood sample is immediately taken within the first 24 h.
The Ethics Committee of Hasanuddin University approved this study and written informed consent was obtained from all parents.
TNF-α measurement
After blood extraction, experiment should be conducted immediately as well. Samples to be used within 5 days may be stored at 2-8°C, otherwise sample must be stored at -20°C (≤ 1 month) or -80°C (≤ 2 months) to avoid loss of bioactivity and contamination. Allow the serum to clot for 10-20 minutes at room temperature and centrifuge (at 2000-3000 RPM) for 20 minutes. Collect the supernatant carefully. When sediments occurred during storage, centrifugation should be performed again. Sample hemolysis will influence the result. When performing the assay, bring samples to room temperature. First, add prepared sample 40 μl, standards, and ELISA solutions. Let them react for 60 minutes at 37°C. Wash the plate five times. Add chromogen solution A and B. Incubate for 10 minutes at 37°C for color development. Then add stop solution. Read the value within 10 minutes.
Statistical analysis
The data obtained are grouped into two groups of patients; septic shock and sepsis without shock. Then, suitable statistic method was chosen to analyze the data, which was univariate and bivariate analysis, power=80%, α=0.05. Mann Whitney test is used to compare the median initial serum TNF-α level of the sepsis patient to the outcome of septic shock or not septic shock. For normality test, Kolmogorov-Smirnov test was used. Chi square was used to determine the significance of predictor factor relationship with the outcome of septic shock and not septic shock. Receiver Operator Curve (ROC) was used in order to determine the best cut-off point levels of TNF-α in determining the outcome. The Data analysis was processed by using SPSS 23.
Results
An observational study with prospective cohort approach to determine the role of TNF-α as a predictor of outcome in sepsis patients in children has been conducted in Dr.Wahidin Sudirohusodo Hospital Makassar from December 2015 until May 2016.
Patients with sepsis shock group consisted of 76% boys and 24% girls while in sepsis without shock group consisted of 60% boys and 40% girls. Statistical analysis showed no significant difference between the two groups with p=0.2. Septic shock group nutritional status consisted of 44% good nutritional status, 52% malnutrition, and 4% overnourished. Meanwhile, sepsis without shock group good nutritional status was 53.3%, malnutrition 44.4%, and overnourished 2.2%. Statistical analysis showed no significant difference with p = 0.72. The age of patients with septic shock was 16% 1-3 months, 28% 3-23 months, 16% 24-59 months, 40% >5 years. Sepsis without shock age’s was 15.5% 1-3 months, 33.3% 3-23 months, 13.3% 24-59 months, 37.7% >5 years. Chi square test results showed that there was no significant difference between the two groups with p=0.6 (Table 1).
| Sample Characteristic | Sepsis | P Value | |
|---|---|---|---|
| Shock n=25 (%) |
Not Shock n=45 (%) |
||
| Gender | |||
| Boy | 19 (76 %) | 27 (60 %) | 0.2* |
| Girl | 6 (24%) | 18 (40 %) | - |
| Nutritional status | |||
| Good | 11 (44%) | 24 (53.33%) | 0.72* |
| Undernourished | 13 (52%) | 20 (44.44%) | - |
| Overnourished | 1 (4%) | 1 (2.22%) | - |
| Age | |||
| 1-3 months | 4 (16%) | 7 (15.56%) | 0.6* |
| 3-23 months | 7 (28%) | 15 (33.33%) | - |
|
4 (16%) | 6 (13.33%) | - |
| >5 years | 10 (40%) | 17 (37.78%) | - |
*Chi-square test
Nutritional status based on WHO for children ≤ 5 years, CDC for children >5 years.
Table 1: Sample characteristic
Kind of infection that most common in this study was respiratory tract infections, followed by central nervous system infections, rheumatic heart disease, diarrhea, urinary tract infections, and infections of dengue (Table 2).
| TNF-α (pg/ml) | Sepsis | |
|---|---|---|
| Shock n=25(%) |
Not shock n=45(%) |
|
| Respiratory | 18 (72%) | 30 (66.6%) |
| Central nervous system | 7 (28%) | 10 (22.2%) |
| Rheumatic heart disease | 0 | 2(4.4%) |
| Diarrhea | 0 | 1(2.2%) |
| Urinary tract infection | 0 | 1(2.2%) |
| Dengue infection | 0 | 1(2.2%) |
Table 2: Focus Infection of sepsis patients
Initial serum level of TNF-α in septic shock group’s median was 544.83 pg/ml and range 405.08 to 1177.91 pg/ ml. While in sepsis without shock group was 345.88 pg/ ml and range 188.01 to 399.44 pg/ml. Mann Whitney test results showed that there were very significant differences between the two groups with p=0.00 (Table 3).
| TNF-α (pg/ml) | Sepsis | |
|---|---|---|
| Shock n=25 |
Not shock n=45 |
|
| Mean | 672.62 | 332.48 |
| Median | 544.83 | 345.88 |
| Standard Deviation | 271.29 | 52.95 |
| coefficient of variation | 40.3% | 15.9% |
| Minimum-Maximum | 405.08-1177,91 pg/mL | 188.01-399,44 pg/mL |
Mann Whitney test p=0.05 (<0.05)
Table 3: Initial serum level of TNF-α in sepsis patient who become shock and not shock
The result of blood culture test of patients with sepsis in not shock group consisted of 8 no growth, 2 staphylococcus aureus, 1 staphylococcus epidermidis, 2 Acinetobacter baumani. Meanwhile, patients in shock group consisted of 7 no growth, 2 E. Cloacae and Burkhoderia cepacia, 2 Acinetobacter baumani (Table 4).
| Sepsis | ||
|---|---|---|
| Shock | Not shock | |
| No growth | 7 | 8 |
| E. Cloacae, Burkhoderia Cepacia | 2 | 0 |
| Staphylococcus aureus | 0 | 2 |
| Staphylococcus epidermidis | 0 | 1 |
| Acinetobacter baumani | 2 | 2 |
| Achromobacter xylosoxidans | 1 | 0 |
Table 4: Causative pathogens
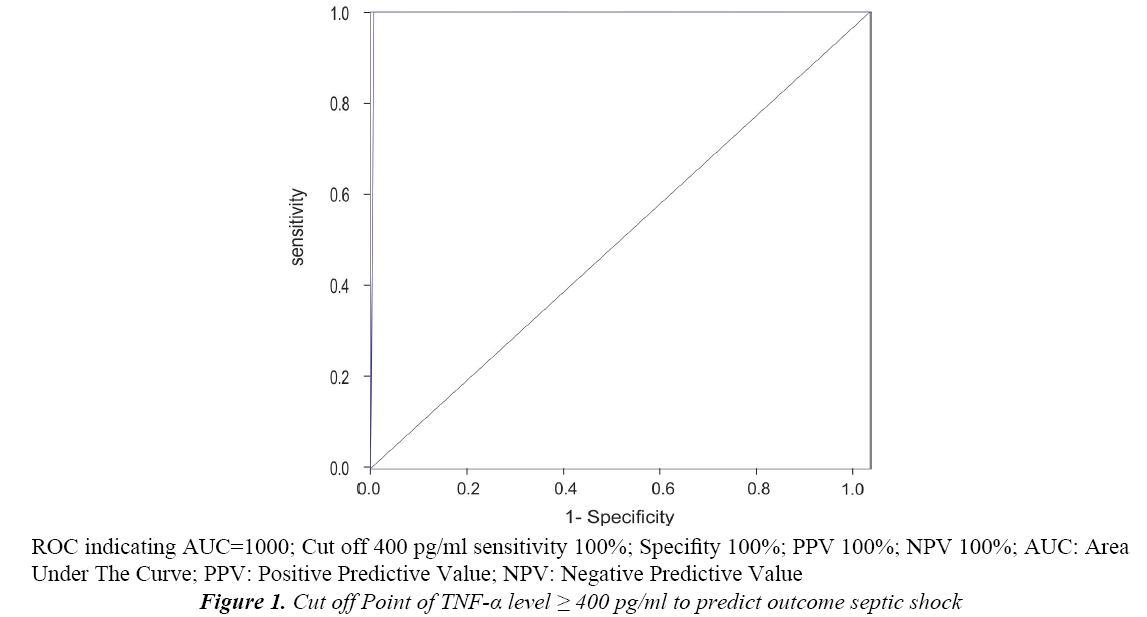
In order to assess the best cut-off point levels of TNF-α in determining the outcome, it can be seen in the Receiver Operator Curve (ROC). Sensitivity depicted on the ordinate Y, while the 1-specificity depicted on the axis X. The value on this cut-off point is the most optimal value as prognostic value in determining the outcome. The prognostic value of initial serum levels of TNF-α ≥ 400 pg/ml had sensitivity 100%, specificity 100%, positive predictive value 100%, negative predictive value 100% with 95% CI, and area under curve (AUC) 1 (Figure 1).
The initial serum levels of TNF-α was significantly increased in both groups, but higher in the septic shock group. Cut off point ≥ 400 pg/ml was obtained through the ROC, with the sensitivity 100%, specificity 100%, positive predictive value 100%, and negative predictive value 100%.
Discussion
This study used the 2005 Goldstein criteria to diagnose sepsis. Sepsis is Systemic Inflammatory Response Syndrome (SIRS) with suspicion or evidence of infection. The SIRS criteria must meet at least 2 of the following four criteria and one of them should be temperature instability or abnormal leukocyte count: Body temperature >38.5°C or <36°C. Tachycardia, (heart rate mean was >2 SD above normal by age, the absence of external stimuli, chronic medications, or pain stimuli; or persistent increase in 0.5 to 4 hours unknown or in children <1 year), bradycardia (mean heart rate <10th percentile by age without external vagal stimuli, β blocker, or congenital heart disease; or persistent depression that occurs> 0.5 hours without any known cause. The rate of respiration >2 SD above normal by age or the use of mechanical ventilation for acute processes not associated with neuromuscular disease or under the influence of general anesthesia. Increase or decrease in leukocyte counts by age (not secondary to chemotherapyinduced leukopenia) or immature neutrophils >10%. Suspicion or evidence of infection (positive culture, tissue staining or PCR test) associated with high probability of infection. Evidence of infection includes findings on physical, imaging, or laboratory examinations (eg found leucocyte cells in sterile body fluids, viscous perforations, pneumonia in thorax radiation, petechial or purpuric rash, or fulminant purpura).
This study showed that the serum levels of TNF-α can be used as an early predictor of outcome in sepsis patients in children and limit levels ≥ 400 pg/ml is the most optimal as a prognostic value. The influence of sex factor, nutritional status, and age to initial serum levels of TNF-α was also analyzed.
The concentration of TNF-α in the circulation is generally low and undetected in healthy subjects (not more than 3 pg/mL) [23]. This study shows that the serum levels of TNF-α had increased since the beginning of disease. The invasion of pathogenic microorganisms and/or its products will stimulate the proinflammatory cytokines. The main proinflammatory cytokines that play an important role in pathogenesis of sepsis is TNF-α, IL-1, IL-6 and IL-8. Tumor necrosis factor alpha which can work in hypothalamus causes fever. It also activates various types of cells such as monocytes, macrophages, dendritic cells and neutrophils, and together with IL-6 induces an acute phase response. Tumor necrosis factor alpha can also induce a procoagulant activity and endothelial cell damage that interfere with blood flow to the organ system and oxygen supply [4].
The function of TNF-α cytokine is to stimulate the expression of adhesion molecules on vascular endothelium and leukocytes which will lead to increasing of vascular permeability and inflammatory reactions. At high levels, TNF-α induce pathologic abnormality of septic shock [17]. Results of previous studies have shown that TNF-α is a good marker for the diagnosis of sepsis, to assess the effectiveness of therapy, and prognosis of sepsis disease. A research by Dinata et al. [16] reported that mean of TNF-α was higher in septic shock than in not septic shock group. Logistic regression analysis showed a positive correlation between the levels of TNF-α and the possibility of shock in patients with sepsis in children (P=0.002, r=0.78). A research conducted by Kumar et al. [23] found that average levels of TNF-α was higher in septic shock patients (59 pg/mL, range 5-2720 pg/ml) than in severe sepsis patients (47 pg/ml, range 5-3310 pg/ ml), so it can be concluded that TNF-α can be used as a marker of sepsis and initial aggressive therapy in patients with increasing levels of TNF-α. In a study conducted by Heper et al. [24], it obtained higher mean serum level of TNF-α at the beginning of admission in patients who died of sepsis (761.9 ± 933.12 pg/ml) than in patients who were improved (137 ± 317.9 pg/ml) (p=0.032). after 24 h of treatment, it obtained serum level of TNF-α mean in patients who died sepsis is 528.4 ± 829.3 pg/ml and 104.96 ± 156.32 pg/ml (p=0.032) in improved patients.
Initial serum level of TNF-α ≥ 400 pg/ml had a sensitivity 100%, specificity 100%, positive predictive value 100%, negative predictive value 100% (p ≤ 0.05), and area under curve (AUC) 1. Limit 400 pg/ml of initial serum level of TNF-α is the best cut-off point determining the outcome of patients. In the study conducted by Heper et al. [24], it obtained the cut-off point of TNF-α ≥ 65 pg/ml to predict the patients will die of sepsis or improves with sensitivity 100%, specificity 60.6%, positive predictive value 27.8%, negative predictive value of 100%, and AUC 0.8. In a study conducted by Kocabas et al. [15] which examined proinflammatory cytokines procalcitonin, TNF-α, IL- 6, IL-8, it found that procalcitonin and TNF-α is a best marker in the diagnosis of neonatal sepsis, determine the effectiveness of therapy, and prognosis of sepsis. In this study, the cut-off point of the levels of TNF-α ≥ 7.5 pg/ ml for diagnosing sepsis in neonates with a sensitivity 100%, specificity 96.6%, positive predictive value 96.2%, negative predictive value 98.3%, and AUC 1. The cut-off point of TNF-α level in this study is higher than other studies with ≥ 400 pg/ml. Probably it due to genetic polymorphisms, or different underlying disease, or people who are frequently exposed to skin infections, worms, or other infections, the levels of TNF-α in the population in Makassar is higher than in other regions. Clinical significance in this study is if we use a cut-off point of another study, all the patients in this study will get an excessive therapy because the lowest levels of TNF-α in this study is 188.01 pg/ml, while the cut-off point on the research by Heper et al. [24], the levels of TNF-α was ≥ 65 pg/ml. Based on the result of this study, supported by some previous studies, initial serum levels of TNF-α can be used as a prognostic factor in determining outcome, but it have to be noted that TNF-α is not the only prognostic factor in determining the outcome, there are also proinflammatory cytokines and other inflammatory risk factors.
Limitations of this study were including; not all patients were examined for blood cultures, blood culture of some patients were not successfully drawn, because the blood is too little, the laboratory cannot analyse viral infection, and the research only conducted in one place, so that the sample population was not reflect the population of Makassar city in general. While the strength of this study is a prospective cohort design is used so that we can follow the effects of these prognostic factors simultaneously, and also determine the cut-off point of serum levels of TNF-α early as prognostic factors using a Receiver Operator Curve (ROC).
Conclusion
The initial serum levels of TNF-α as the prognostic value of the outcome of patients with sepsis hopefully can be an additional reference of a more comprehensive sepsis treatment to prevent complications and deaths. Sepsis patients with initial serum levels of TNF-α ≥ 400 pg/ ml require a close supervision. Further research needs to be done with the involvement of other factors are also associated with sepsis outcomes such as genetic polymorphisms associated with TNF-α, TNF-α levels in the normal population in Makassar, and serial examination of TNF-α in patients with sepsis.
References
- Nasronuddin. Infectious Diseases in Indonesia Current and Future Solutions. 2nd ed. Surabaya: Airlangga University Press. 2011.
- Carcillo JA. Pediatric septic shock and multiple organ failure. Crit Care Clin 2003; 19: 413-440.
- Robbins. 2007. Diseases of the Immune System. Basic Pathology. 8th ed. WB Saunders
- Sriskandan S, Altmann DM. The immunology of sepsis. J Pathol. 2008; 214: 211-223.
- Russell JA, Rush B, Boyd J. Pathophysiology of Septic Shock. Crit Care Clin 2018; 34: 43-61.
- Abbas AK, Lichtman AH. Cellular and Molecular Immunology. 8th edn. WB Saunders Comp. 2015.
- Angus DC, Poll TVD. Severe sepsis and septic shock. The New England Journal of Medicine 2013; 369: 840-849.
- Chan, T., Gu, F., 2011. Early Diagnosis of Sepsis Using Serum Biomarkers. Expert Rev Mol Diagn 2011; 11: 487-496.
- Delves PJ, Roitt IM. The immune system. N Engl J Med 2000; 13: 108-116.
- Makhija P, Yadav S, Thakur A. Tumor necrosis factor alpha and interleukin-6 in infants with sepsis. Indian Pediatrics 2005; 42: 1024-1028.
- Peters K, Unger RE, Brunner J, et al. Molecular basis of endothelial dysfunction in sepsis. Cardiovasc Res 2003; 60: 49-57.
- Spronk PE, Zandstra DF, Ince C. Bench-to-bedside review: Sepsis is a disease of microcirculation. Crit Care 2004; 8: 462-468.
- Wong HR, Salisbury S, Xiao Q, et al. The pediatric sepsis biomarker risk model. Critical Care 2012; 16: R174.
- Bozza FA, Salluh JI, Japiassu AM, et al. Cytokine profiles as markers of disease severity in sepsis: A multiplex analysis. Crit Care 2007; 11: 1-8.
- Kocabas E, Sarickliogu A, Aksaray N, et al. Role of procalcitonin C reactive protein, interleukin-6, interleukin-8, and tumor necrosis factor α in the diagnosis of neonatal sepsis. Turk J Pediatr 2007; 49: 7-20.
- Dinata K, Runtunuwu AL, Mandei JM, et al. Correlation between tumor necrosis factor alpha and septic shock in children. Paediatrica Indonesiana 2013; 53: 1-5.
- Abbas A, Lichtman AH, Pillai S. Cellular and molecular immunology. 8th Ed. Philadelphia: Saunders Comp. 2014.
- Baratawidjaja KG. Basic Immunology. 11th ed, Jakarta: Balai Penerbit FKUI. 2014.
- Parrillo JE. Pathogenetic mechanisms of septic shock. The New England journal of medicine 1993; 328: 1471-1477.
- Duma D, Fernandes D, Bonini MG, et al. NOS-1 derived is an essensial triggering signal for the develpoment of systemic inflammatory responses. Eur J pharmacol 2011; 668: 285-292.
- Brahm G. International pediatric sepsis consensus conference: Definitions for sepsis and organ dysfunction in pediatrics. Pediatr Crit Care Med 2005; 6: 2-8.
- Runtunuwu AL. Roles and prognostic values of tumor necrosis factor alpha, interleukin-1 antagonist receptors, and nitric oxides in child sepsis. Makassar: Universitas Hasanuddin. 2014.
- Kumar S, Rizvi M. Prognostic serum tumor necrosis factor-α in paediatric patients with sepsis. J Infect Dev Ctries 2009; 3: 437-441.
- Heper Y, Akalın EH, Mıstık R, et al. Helvacı evaluation of serum c reactive protein, procalcitonin, tumor necrosis factor alpha, and interleukin-10 Levels as diagnostic and prognostic parameters in patients with community acquired sepsis, severe sepsis, and septic shock. Eur J Clin Microbiol Infect Dis 2006; 25: 481-491.