Research Article - Current Pediatric Research (2017) Volume 21, Issue 4
Epidemiology of goiter and its predictors among school age children in Leku town, Southern Ethiopia.
Desalegn Tsegaw Hibstu1* and Dawit Jember Tesfaye21Department of Reproductive Health, School of Public Health, College of Medicine and Health Sciences, Hawassa University, Ethiopia
2Department of Epidemiology, School of Public Health, College of Medicine and Health Sciences, Hawassa University, Ethiopia.
- *Corresponding Author:
- Desalegn Tsegaw Hibstu
Department of Reproductive Health
School of Public Health, College of Medicine and Health Sciences
Hawassa University, Ethiopia
. Tel: +251917187974
E-mail: desuethiopia@yahoo.com
Accepted date: November 23rd, 2017
Abstract
Background: A goiter prevalence of 5% or more in school age children is an indication of iodine deficiency in a population. So, school age children can be used to determine the severity of iodine deficiency in the population since they are easily susceptible to iodine deficiency. The study aimed to assess the epidemiology of goiter and associated factors among school aged children in Leku town, Southern Ethiopia. Method: Community-based cross-sectional study was employed from July 15-30/2017. A total of 358 children were selected using simple random sampling technique. Data on school age children were collected from their mothers/caretakers using a pre-tested and interviewer administered structured questionnaire. The presence or absence of goiter was confirmed by physical examination using world health organization guide line. Logistic regression was carried out using SPSS version 20.0 software. Results: The overall magnitude of goiter among school age children was 35.2% (CI: 30.4- 40.5%). Maternal education (AOR=2.50, CI: 1.37, 4.57), family monthly income (AOR=2.19, CI=1.09, 4.36), type of salt used (AOR=2.66, CI: 1.15, 6.17), timing of adding salt into food (AOR=2.20, CI: 1.27, 3.82) and using cassava as a food (AOR=2.19, CI: 1.30, 3.68) were identified predictors of goiter. Conclusion: The observed magnitude of goiter is considered as a public health problem in the study area. Women education, adding salt after cooking food, ensuring iodized salt consumption and increasing public awareness on consequences of goiter need to be given emphasis.
Keywords
School age children, Leku town, Ethiopia.
Abbreviations
AOR: Adjusted Odd Ratio; CI: Confidence Interval; COR: Crude Odd Ratio; EDHS: Ethiopian Demography and Health Survey; FMOH: Federal Ministry of Health; IDDs: Iodine Deficiency Disorders; ID: Iodine Deficiency; SD: Standard Deviation; SNNPR: Southern Nation Nationalities and People Region; SPSS: Statistical Package for Social Science; TV: Television; UNICEF: United Nations Children’s Fund; WHO: World Health Organization
Background
The term goiter refers to the abnormal growth of the thyroid gland [1]. It is the most observable indication of Iodine Deficiency Disorders (IDDs) [2]. Population consequences of severe iodine deficiency, named iodine deficiency disorders include endemic goiter, hypothyroidism, and cretinism, reduced fertility rate, increased infant mortality, and mental retardation [3]. Twenty-nine percent of the world’s population, living in approximately 130 countries, is estimated to live in areas of iodine deficiency [4].
Globally, about 600 million people had goiter and 230 million have some degree of brain damage due to iodine deficiency during maternity [5]. In the 2011 estimate of the Iodine Global Network, close to 2 billion people had inadequate iodine intake in the globe, where 30% were school aged children. Iodine deficiency (ID) in childhood and adolescence is linked with endemic goiter [6].
Pregnant mothers and school age children are the most vulnerable groups for ID compared to other segment of the population [7]. ID, worldwide public health problem, is not uncommon in mountainous regions of Europe, Asia, South and Central America, and Eastern Africa [8]. Globally, 241 million school children are suffering from IDDs while more than 1.5 billion people are at increased risk of ID and IDD is noticed in 57 million African children [9-11].
In Ethiopia, more or less 28 million people suffer from goiter, and more than 35 million people are at risk of ID [12]. Study on prevalence of goiter among children 6 to 12 years of age in Ethiopia in 2005 was 39.9%; 27.7% palpable and 12.2% visible goiter [13]. In the 2011 Ethiopia Demographic and Health Survey (EDHS) report, only 4 among 25 children live in households that utilized iodized salt. The proportion is higher in urban areas (24%) than rural areas (14%) [14].
Besides to the intake of goiterogenic substance containing food items like cassava and millet and coexistent deficiency of micronutrients (like iron and selenium deficiency), poor socio-economic status, maternal education, advanced age of the mother, age and sex of the child were some of the identified factors associated with ID [15-18].
Realizing the problem, the Ethiopian government planned to avert ID and to achieve the utilization of adequately iodized salt to 90% by the year 2015. Hence, in order to achieve the set plan, the government designed a national nutrition program and micronutrient guideline, and endorsed a resolution to ensure the availability of iodized salt [19].
A goiter prevalence of 5% or more in school-age children is an indication of iodine deficiency in a population. As a result the goiter rate in school-age children can be used to determine the severity of iodine deficiency in the population since they are easily susceptible to iodine deficiency, accessible as a study group and representativeness of society as a whole [1,20]. Therefore, this study is aimed to determine the magnitude of goiter and its predictors among school age children in Leku town, Southern Ethiopia.
Methods
Study Design, Setting and Populations
Community-based cross-sectional study was conducted from July15-30/2017 in Leku town, Sidama Zone, Southern Ethiopia. The town is found at a distance of 27 kilometer (km) from Hawassa; capital city of Southern Nation and Nationalities and People Region, Ethiopia and 299kmsouth of from Addis Ababa; capital city of Ethiopia. The town has five kebeles (kebele is the smallest administrative unit in Ethiopia) with a total population of 30,668, of which 15,828 are males, 5374 and 1012 are under 15 and under five children.
The town has five governmental health facilities (one primary hospital and four health posts) and five private clinics rendering preventive, promotive and curative and rehabilitation services for the community of the town and its surrounding community. The study populations were all school age children (6-12 years old) with their parents/ caretakers living in Leku town. Children diagnosed by physicians as mentally and physically not capable for physical examination procedures and interview, and living in the study area for less than six months were excluded.
Sample Size Determination and Sampling Procedure
Sample size was determined using single population proportion formula considering the following assumption: 95% confidence level, 5% margin of error and proportion of goiter among school age children (37.6%) [21].

From the total five kebeles, two kebeles were selected using simple random sampling technique. Complete enumeration of households found in the two kebeles of the town was carried out and unique identifier was assigned for each household. The team employed simple random sampling technique to identify the study subjects using the unique identifier of the households as a sampling frame. In the selected household if more than one eligible child was found, only one child was taken by lottery method. In case if no eligible study participant identified in the selected household, the data collectors went to the next household until they got eligible child.
Measurement of the Study Variable
In this study, the presence or absence of goiter was diagnosed clinically using physical examination of thyroid by trained bachelor degree holder nurses. The degree of goiter was graded by using WHO grading system (Grade 0: No palpable or visible goiter/no goiter, grade 1: a mass in the neck that is consistent with an enlarged thyroid which is palpable but not visible when the neck is in normal position and it moves upward as the subject swallows and grade 2: swelling in the neck that is visible when the neck is in normal position and consistent with an enlarged thyroid when the neck is palpated).
Data Collection Tools and Procedure
Pre-tested and interviewer administered structured questionnaire was used to collect quantitative data. The questionnaire was prepared in English language and translated to Amharic language and back to English language. Physical examination of the thyroid was performed to identify the presence of goiter. Six registered female nurses were participated to collect the data. Training on diagnosis of goiter and data collection procedures was given to data collectors for two days. One medical doctor and the investigators supervised the data collection process and checked filled questionnaire for consistency and completeness.
Statistical Analysis
After data collection, data were edited and cleaned; each questionnaire was checked for completeness and coded. Data were entered into computer using EPI Info version 3.5.4 and the analysis was done using SPSS version 20.0.
Categorical variables were described using frequency, percentage and figures. Simple binary logistic regression analysis for each independent variable against the dependent variable was executed to observe the impact of each factor on the occurrence of goiter among school age children.
Independent variables found to be significant in the simple binary logistic regression analysis at a cut-off p-value ≤ 0.2 with their 95% confidence interval (CI) were included in the multiple binary logistic regressions model. In the multiple binary logistic regressions, the effects of each independent variable on presence of goiter were assessed by controlling possible confounders using stepwise backward logistic regression. Adjusted odds ratios (AOR) with 95% CI and p-value of less than 0.05 were considered to have significant association between the dependent and independent variables.
Results
Socio Demographic and Economic Characteristics
In the present study, 358 (99.4%) children aged 6-12 were included. The mean age of the study participants was 8.94 years (± 1.96) standard deviation (SD) with average family size of 5.43 ± 1.63 SD and 188 (52.5%) were females. More than three in five, 227(63.4) parents/caretakers of the children were protestant by religion.
Two hundred fifty eight (72.1%) children were grade one to four and 180 (50.3%) and 188 (52.5%) of their mothers and fathers attended primary and secondary and above education. More than half 194 (54.2%) mothers and 147 (41.1%) of their husbands were house wife and governmental employed by occupation. One hundred sixty eight (46.9%) family members obtained monthly income of 1001 to 2000 Ethiopian birr (≈ 43-87 USD) and three among five 221 (61.7%) family members possessed television (TV) (Table 1).
| Variables | Category | Frequency (n) | Percentage (%) |
|---|---|---|---|
| Child age (years) | 6-10 | 267 | 74.6 |
| >10 | 91 | 25.4 | |
| Sex of child | Male | 170 | 47.5 |
| Female | 188 | 52.5 | |
| Religion | Protestant | 227 | 63.4 |
| Orthodox | 76 | 21.2 | |
| Muslim | 55 | 15.4 | |
| Child education | Kindergarten | 73 | 20.4 |
| 1-4 grade | 258 | 72.1 | |
| 5-8 grade | 27 | 7.5 | |
| Family size | = 4 | 115 | 32.1 |
| >4 | 243 | 67.9 | |
| Maternal education | No formal education | 89 | 24.9 |
| Primary education | 180 | 50.2 | |
| Secondary & above | 89 | 24.9 | |
| Husband education | No formal education | 17 | 4.7 |
| Primary education | 153 | 42.7 | |
| Secondary & above | 188 | 52.5 | |
| Maternal occupation | Farmer | 22 | 6.1 |
| Merchant | 81 | 22.6 | |
| Governmental employee | 61 | 17.0 | |
| Housewife | 194 | 54.2 | |
| Husband occupation | Farmer | 50 | 14.0 |
| Merchant | 136 | 38.0 | |
| Governmental employee | 147 | 41.1 | |
| Others* | 25 | 7 | |
| Monthly income | = 1000 | 41 | 11.5 |
| 1001-2000 | 66 | 18.4 | |
| 2001-3000 | 83 | 23.2 | |
| >3000 | 168 | 46.9 | |
| Possession of radio | Yes | 255 | 71.2 |
| No | 103 | 28.8 | |
| Possession of TV | Yes | 221 | 61.7 |
| No | 137 | 38.3 |
Others * include daily laborers, temporary workers with payment.
Dietary and Goiter Related Characteristics
Among the total study participants, 135 (37.7%) utilized iodized salt in their diet and 340 (95%) store the dietary salt kept closed, and only 51 (14.2%) put the salt near to fire. Two hundred forty three (67.9%) added the salt while cooking food, 341 (95.3%), 32 (8.9%), 323 (90.2%) used cabbage, millet and ‘habesha’ (local) cabbage in their diet as food, respectively. Nearly, nine in ten respondents, 312 (87.2%) heard about goiter, 24 (6.7%) had familial history of goiter and 128 (35.8%) perceived that the cause of goiter was iodine deficiency (Table 2).
| Dietary characteristics | Category | Frequency (n) | Percentage (%) | |
|---|---|---|---|---|
| Salt type used | Non-Iodized | 193 | 53.9 | |
| Iodized | 135 | 37.7 | ||
| Both | 30 | 8.4 | ||
| Method of storing salt | Kept opened | 18 | 5.0 | |
| Kept closed | 340 | 95.0 | ||
| Place of storing | Near to fire | 51 | 14.2 | |
| Away from fire | 307 | 85.8 | ||
| Timing of adding salt into food | During cooking | 243 | 67.9 | |
| After cooking | 115 | 32.1 | ||
| Foods included in the diet | Cabbage | Yes | 341 | 95.3 |
| No | 17 | 4.7 | ||
| Millet | Yes | 32 | 8.9 | |
| No | 326 | 91.1 | ||
| Soya bean | Yes | 16 | 4.5 | |
| No | 342 | 95.5 | ||
| Boyina’ (Cassava) | Yes | 75 | 20.9 | |
| No | 283 | 79.1 | ||
| ‘Habesha’ Cabbage* | Yes | 323 | 90.2 | |
| No | 35 | 9.8 | ||
| Hamicho’ (False banana) | Yes | 57 | 15.9 | |
| No | 301 | 84.1 | ||
| Heard of goiter | Yes | 312 | 87.2 | |
| No | 46 | 12.8 | ||
| Familial history of goiter | Yes | 24 | 6.7 | |
| No | 334 | 93.3 | ||
| Perceived cause of goiter | Iodine deficiency | 128 | 35.8 | |
| Rain water | 96 | 26.8 | ||
| Don’t know | 134 | 37.4 | ||
Habesha? Cabbage* (local cabbage).
Table 2. Dietary and goiter related characteristics of the study subjects in Leku town, Southern Ethiopia, 2017
Magnitude and Predictors of Goiter
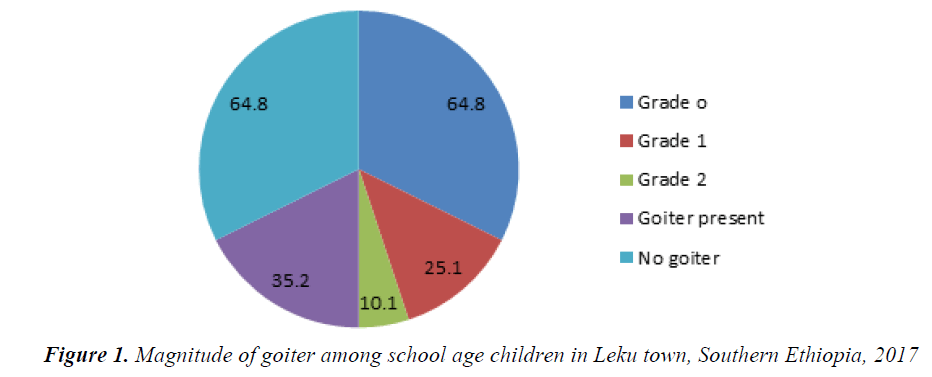
The overall magnitude of goiter among school age children was 126 (35.2%, CI: 30.4-40.5%). The magnitude of grade one goiter was 90 (25.1%) while grade two was 36 (10.1%) (Figure 1).
In the multiple binary logistic regressions: maternal education, family income, type of salt used, timing of adding salt into the food and using ‘boyina’ (cassava) as food were identified as independent predictors of goiter among school age children.
The present study revealed that children whose mothers did not attend formal education were nearly three times more likely to develop goiter (AOR=2.50, CI: 1.37, 4.57). The study showed that the odds of goiter was two times higher among children whose family monthly income was below ≤ 1000 Ethiopian birr 43 USD) compared with family monthly income of >3000 Ethiopian birr (AOR=2.19, CI=1.09, 4.36).
On the other hand, type of salt used, timing of adding salt into food and using ‘boyina’(cassava) as a food were other important predictors. The occurrence of goiter was nearly three times higher among children using non-iodized salt (AOR=2.66, CI: 1.15, 6.17). It was observed that adding salt into food while cooking contributed to two times increase in goiter prevalence among school age children (AOR=2.20, CI: 1.27, 3.82). School age children using ‘boyina’ (cassava) as a food were two times more likely to develop goiter (AOR=2.19, CI: 1.30, 3.68) (Table 3).
| Variables | Category | Presence of goiter | COR (95% CI) | AOR (95% CI) | P-value | |
|---|---|---|---|---|---|---|
| No | Yes | |||||
| Maternal education | No formal education | 51 | 38 | 1.58 (0.75,3.32) | 2.50 (1.37,4.57) | 0.012 |
| Primary education | 121 | 59 | 1.33 (0.79,2.24) | 1.16 (0.65,2.08) | 0.085 | |
| Secondary & above | 60 | 29 | 1.00 | 1.00 | ||
| Paternal education | No formal education | 6 | 11 | 3.46 (1.17,10.22) | 1.54 (0.72,3.25) | 0.26 |
| Primary education | 101 | 52 | 1.42 (0.93, 2.19) | 1.14 (0.64,2.05) | 0.653 | |
| Secondary & above | 125 | 63 | 1.00 | 1.00 | ||
| Family income | = 1000 | 31 | 10 | 1.24 (0.93, 5.07) | 2.19 (1.09,4.36) | 0.027 |
| 1001-2000 | 53 | 13 | 2.22 (0.78, 4.2) | 2.05 (1.15,3.65) | 0.015 | |
| 2001-3000 | 42 | 41 | 0.73 (0.59,2.33) | 1.93 (1.13,3.29) | 0.016 | |
| >3000 | 106 | 62 | 1.00 | 1.00 | ||
| Presence of Radio | Yes | 166 | 89 | 0.63 (0.40,0.99) | 0.85 (0.50,1.43) | 0.125 |
| No | 66 | 37 | 1.00 | 1.00 | ||
| Type of salt used | Non-iodized | 116 | 77 | 2.97 (1.29,6.81) | 2.66 (1.15,6.17) | 0.023 |
| Iodized | 94 | 41 | 1.29 (0.55,3.03) | 1.79 (0.73,4.37) | 0.191 | |
| Both | 22 | 8 | 1.00 | 1.00 | ||
| Place of storing | Near to fire | 28 | 23 | 2.20 (1.20,4.06) | 1.72 (0.91,3.28) | 0.097 |
| Away from fire | 204 | 103 | 1.00 | 1.00 | ||
| Timing of adding salt into food | During cooking | 144 | 99 | 2.79 (1.74,4.47) | 2.20 (1.27,3.82) | 0.005 |
| After cooking | 88 | 27 | 1.00 | 1.00 | ||
| Using cassava as food | Yes | 43 | 32 | 1.78 (1.01,3.14) | 2.19 (1.30,3.68) | 0.003 |
| No | 189 | 94 | 1.00 | 1.00 | ||
Table 3. Multiple binary logistic regressions model predicting presence of goiter among school age children in Leku town, Southern Ethiopia, 2017
Discussion
In the present study, the magnitude of goiter was found to be 35.2% (CI: 30.4, 40.5%) and magnitude of grade one and grade two goiter was 25.1% and 10.1%.This finding was almost in adjacent with a study conducted in Northwest Ethiopia (37.6%) [21]. The current magnitude of goiter is a significant public health problem in the study area according to the WHO, UNICEF and ICCIDD assessment criteria for the severity of IDD [22]. The magnitude of goiter in this study (35.2%) was also nearly in line with the national total goiter prevalence among school age children in Ethiopia (39.9%) [13].
On the contrary, the magnitude of the current finding is lower than the findings in a study in ten villages of four administrative states of Ethiopia (53.3%) and Pakistan; Islamabad (71.6%) [23,24]. The observed magnitude of goiter in this study was higher than the research findings in northwestern India: Rajasthan (11.4%) [25], India: Gujarat (20.5%) [26], southern Blue Nile area of Sudan (22.3%) [27] and South Africa (25.5%) [28].
The study demonstrated that goiter was more likely to increase among school age children whose mothers did not attend formal education and family members with a monthly income below 1001 Ethiopian birr. This finding is similar the study done in other areas [15,17]. This might be due that educated mothers can have better access to information and awareness, on cause, consequences and prevention strategies of goiter among children. Family members with better monthly income would have an opportunity to buy iodized salt and include in their diet. In the present study, it was figured out that goiter was higher among school children using non-iodized salt. This finding is consistent with a study in northwest Ethiopia [21].
On the other hand, timing of adding salt into food and using boyina (cassava) as food were noticed as independent predictors of goiter occurrence among school age children. Adding iodized salt into food while cooking increased the probability of goiter among children. This could be explained as when the iodized salt is introduced into food while cooking, it will lose its iodine content through heat. It was also observed that using cassava as a food increased the occurrence of goiter among school age children. This study is in line with a study by Gaitan and the finding in Southwest and Southern Ethiopia [29].
Limitations
The following limitations need to be taken into account in the findings of this research. First, the findings of this study are only based on physical examination by palpation using World Health Organization grading system as a result the specificity and sensitivity are low due to interobserver variation and the level of urinary iodine excretion was not measured [30,31]. Second, the cross sectional nature of the data could not show the direct causality of goiter among school age children.
Conclusion
In general, the magnitude goiter among school age children was high. Maternal education, family income, type of salt used, timing of adding salt into food and using ‘boyina’ (cassava) as a food were independent predictors of goiter occurrence among school age children in Leku town, Southern Ethiopia. Women education, adding salt after cooking food, ensuring iodized salt consumption and increasing public awareness on consequences of goiter need to be given emphasis.
Declarations
Ethical Approval and Consent to Participate
Ethical clearance was obtained from the Institutional Review Board of Hawassa University, College of Medicine and Health Sciences. Supportive letter was taken from Leku town health office. Since the study participants are below age 18 years old, parental/care taker informed verbal and written consent was secured and the Institutional Review Board committee approved their participation. An assent was also taken from children prior to palpation of their thyroid gland. Children diagnosed as having goiter were referred to the nearby health facility to for further investigation.
Availability of Data and Materials
All the data that support the findings of this study will be available from the corresponding author on reasonable request.
Authors’ Contribution
DTH conceived the study, monitored the data collection process, analyzed the data and wrote the manuscript. DJT participated in designing the study, supervising data collection process and writing the manuscript. Both authors read and approved the manuscript.
Acknowledgement
The authors acknowledge Leku town health office for facilitating the data collection process. The study participants need to be given respect, without their consent and the provision of the demanded information; this research work would not have been come into existence.
References
- WHO/UNICEF/ICCIDD. Assessment of iodine deficiency disorders and monitoring their elimination. A Guide for Programme Managers 2001.
- WHO. Global database on iodine deficiency disorders. 2013.
- Zimmermann MB, Jooste PL, Pandav CS. Iodine-deficiency disorders. Lancet2008; 372: 1251-1262.
- Pearce EN, Andersson M, Zimmermann MB. Global iodine nutrition: Where do we stand in 2013? Thyroid 2013; 23: 523-528.
- World Health Organization. Micronutrient deficiency information system project global prevalence of iodine deficiency disorders. World health Organization, Geneva (MDIS working paper, No.1) 1993.
- Zimmermann M. The effects of iodine deficiency in pregnancy & infancy. Pediatr Perinatal Epi 2012.
- Benoist B, McLean E, Andersson M, et al. Iodine deficiency in 2007: Global progress since 2003. Food Nutr Bull 2008; 29: 195-202.
- Hofvander Y. Endemic goitre among children in the Ethiopian highlands. Effect of a supplementary food with iodized salt. Ethiop Med J 1970; 8:179-184.
- Molineoux L, Ayele T. Endemic goitre surveys in Begemidir province, Ethiopia. Ethiop Med J 1967; 1: 239.
- Wolde-Gebriel Z, Demeke T, West CE, et al. Goitre in Ethiopia. Br J Nutr 1993; 69: 257-268.
- Abuye C, Ayana G, Umeta M, et al. Thyroid responses to varying doses of oral iodized oil in school children in Awassa, Ethiopia. Ethiop J Health Dev 2000; 14: 49-55.
- Dawit S, Seifu H, Carl KL, et al. Post-production losses in iodine concentration of salt hamper the control of iodine deficiency disorders: A case study in northern Ethiopia. J Health Popul Nutr 2010; 28: 238-244.
- Abuye C, Berhane Y, Akalu G, et al. Prevalence of goiter in children 6 to 12 years of age in Ethiopia. Food Nutr Bull 2007; 28: 391-398.
- Central Statistical Agency [Ethiopia] and ICF International. Ethiopia Demographic and Health Survey 2011. Addis Ababa, Ethiopia and Calverton, Maryland, USA: Central Statistical Agency and ICF International 2012.
- Kebede DL, Adinew YM. Predictors of goiter among school children in southwest Ethiopia: Case-control study. J Nutr Food Sci 2015; 5: 368.
- Amin D, Rathod S, Doshi V, et al. Changing prevalence of iodine deficiency disorders in Amreli district, Gujarat, India. NJIRM 2011; 2: 77-80.
- Kapil U, Pandey RM, Prakash S, et al. Assessment of iodine deficiency in school age children in Nainital district, Uttarakhand state. Asia Pac J Clin Nutr 2014; 23: 278.
- Pushpa S, Harish BR, Aghunath HR, et al. Prevalence of iodine deficiency disorders among school children aged 6-12 years in Mandya district, Karnataka. Int J Sci Stud 1214; 2.
- Federal Ministry of Health, Ethiopia. Ethiopia National Nutrition Strategy. Review and Analysis of Progress and Gaps 2009.
- Zimmermann MB, Moretti D, Chaouki N, et al. Development of a dried whole-blood spot thyroglobulin assay and its evaluation as an indicator of thyroid status in goitrous children receiving iodized salt. Am J Clin Nutr 2003; 77: 1453-1458.
- Mesele M, Degu G, Gebrehiwot H. Prevalence and associated factors of goiter among rural children aged 6-12 years old in Northwest Ethiopia, cross-sectional study. BMC Public Health 2014; 14: 130.
- Joint WHO/UNICEF/ICCIDD Consultation. Indicators for assessing iodine deficiency disorders and their control programmes. Geneva: WHO 1992.
- Charinet AKU. Determinants of iodine deficiency in school children in different regions of Ethiopia. East Afr Med J 2000;77: 133-137.
- Ali TZ, Anis RA, Shami SA, et al. Prevalence of goiter in school-going children in a Union Council near Islamabad. Pak J Med Res 1999; 38: 3-6.
- Singh MB, Marwal R, Lakshminarayan J. Assessment of iodine deficiency disorders in school Age children in Jodhpur district of Rajasthan. J Hum Ecol 2010; 32: 79-83.
- Misra SLKJRD. Prevalence of goiter in 6-12 years school-going children of Panchmahal district in Gujarat, India. Indian J Med Res 2007; 126: 475-479.
- Elnour A, Hambraeus L, Eltom M, et al. Endemic goiter with iodine sufficiency: A possible role for the consumption of pearl millet in the etiology of endemic goiter. Am J Clin Nutr 2000; 71: 59-66.
- Jooste JWPL, Kriek JA. Iodine deficiency and endemic goiter in the Langkloof area of South Africa. SAMJ 1997; 8: 10.
- Gaitan E. Goitrogens in food and water. Ann Rev Nutr 1990; 10: 21-39.
- Wolka E, Shiferaw S, Biadgilign S. Epidemiological study of risk factors for goiter among primary school children in southern Ethiopia. Food Nutr Bull 2014; 35: 20-27.
- Zimmermann M, Saad A, Hess S, et al. Thyroid ultrasound compared with World Health Organization 1960 and 1994 palpation criteria for determination of goiter prevalence in regions of mild and severe iodine deficiency. Eur J Endocrinol 2000; 143: 727-731.