- Biomedical Research (2012) Volume 23, Issue 4
Effect of obesity on pulmonary functions among Saudi Children
Ahmad H. Alghadir1,2, Farag A. Aly1,3,*1Rehabilitation Research Chair, King Saud University, Riyadh 11433, Saudi Arabia
2Department of Rehabilitation Sciences, College of Applied Medical Sciences, King Saud University, Riyadh 11433, Saudi Arabia
3Faculty of Physical Therapy, Cairo University, Cairo, Egypt
- *Corresponding Author:
- Farag A. Aly
Rehabilitation Sciences Department
Faculty of Applied Medical Sciences
King Saud University
P.O Box, 10219 Riyadh 11433
Saudi Arabia
Accepted Date: March 10 2012
Abstract
The possible relationship between the severity of obesity and the ventilatory function parameters among Saudi male children has been investigated. In addition to comparing the ventilatory function of of Saudi male children with different body weights to their age matching Caucasian reference values. Healthy Saudi male school children participated in this study. Selected children were divided into three groups, group I (normal weight children), group II (overweight children), and group III (obese children). Ventilatory function tests were conducted using portable Spirometer. Comparing the ventilatory function of the three groups of Saudi children showed that increasing degree of obesity have negative effect on ventilatory function among Saudi children as the ventilatory function of the obese Saudi children were much lower, than their age matching overweight and normal weight Saudi children but with non statistically significant differences between the three groups. Statistical analysis of the data also showed that Saudi children have ventilatory function much lower than the predicted reference values based on the age/sex specific BMI percentiles. Conclusion: Over weight and obese Saudi male children have much lower ventilatory function compared to their age matched normal weight Saudi children and their age matchedreference predicted values in away that could restrict their lung expansion and affect their exercise capacity.
Keywords
Obesity, ventilatory functions, age/sex specific BMI percentiles
Introduction
Obesity is defined as an excessive accumulation of energy in the form of body fat, in a way that can cause much health impairments[1].Obesity in children may be defined as a maladaptive increase in the mass of somatic fat stores[2],and is one of the major risk factors for cardiovascular diseases that track well into the period of adulthood.[3,4]In 40 to 50 year follow-up studies of obesity in adolescents has shown that excessive body fat in adolescent was a powerful predictor of cardiovascular disease, colorectal cancer, gout, and arthritis irrespective of the degree of obesity at the time when the morbidity was diagnosed[5].
Body mass index (BMI), i.e. weight (kg)/height (m2), is one of the most common indirect methods used to measure obesity which correlates well with the direct measures of obesity within a population[6,7].Adult subjects with BMI between 25 and 30 Kg/m2 are sub-classified as overweight or at risk for obesity related morbidities, and those with BMI greater than 30 Kg/m2 are considered obese[8].However, these definitions cannot be used to estimate obesity among children, because normative values for BMI are highly age-dependent in children and BMI values in children are significantly lower compared to that of adults at the same level of obesity.[9]A classification system obese children, based on percentiles for BMI for age is used to classify obesity into four different categories .Children who are at an ideal weight have a BMI in the 5th percentile to less than the 85th percentile for children of their age. The BMI values in children with less than ideal weight or thin children lie below the 5th percentile. Two classifications can be used to identify children whose BMI is above the healthy weight rangeoverweight or at risk for obesity and obese children "Overweight" refers to children who's BMI-for-age is in the 85th to less than the 95th percentiles. Children in this range are comparable to adults with a BMI of 25 to 29.9. Obese children have a BMI-for-age equal to or greater than the 95th percentile. This is comparable to adults with a BMI of 30 or more.[10,11] Growth charts of age/sex specific BMI percentiles are now available and can be downloaded directly from the web page of Centre for Disease Control (http://www.cdc.gov/nchs/data/ad/ad314.pdf). Increased body fat has a serious effect on a child's life. It increases the risk of several health problems, especially the respiratory system disorders as obese children have more respiratory symptoms than normal weight children of the same age with linear relationship between the Respiratory pathology and the amount of body fatness and it can also cause emotional and social problems. Obese children are also more likely to be obese subject at his adulthood stage, increasing their risk of serious diseases such as heart disease and stroke [12,13].
Several studies has shown an association between pulmonary function abnormalities and obesity in adult, as it has shown that the forced expiratory volume the first second (FEV1) is inversely related to body mass index and increasing body weight lead to worsening of pulmonary function [14]. Obesity also affects lung function in away that it can reduce respiratory well-being, even in the absence of specific pulmonary disorder, and may also exaggerate the effects of existing airway disease [15].
Most of the studies evaluating the relationship between obesity and ventilatory function tests were done on adults, while similar investigations in obese children are limited [16]. To the best of our knowledge no previous study has been done on Saudi children to investigate the effect of different degree of obesity on ventilatory function. So the Aim of this study was to investigate the possible relationship between the severity of obesity and the ventilatory function parameters by comparing ventilatory function parameters of overweight and obese male Saudi children with the age matched Saudi children with normal weight. In addition to comparing the ventilatory function of the three groups of Saudi male childrento their age matching Caucasian reference values (the inbuilt references values in most of the Spirometer).
Material and Methods
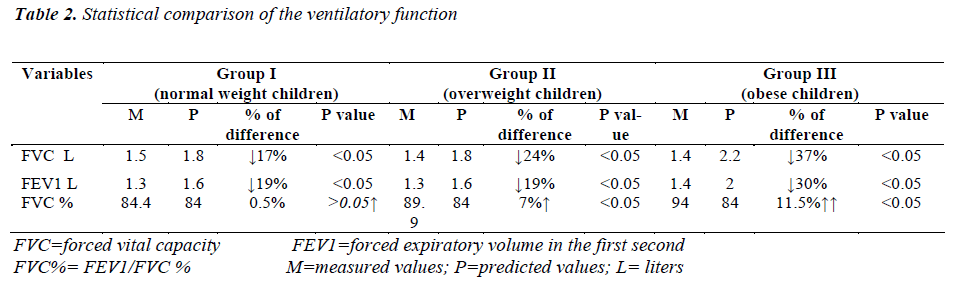
The past medical history of lung infection was collected from subject's family via face-to-face interview and a questionnaire. The investigation was approved by the ethics committee of Rehabilitation Research Chair, King Saud University. General characteristics of the subjects are shown in (Table I).
Anthropometric measurements and assessment of static ventilatory function had been conducted to all children. Forced vital capacity (FVC) and forced expiratory volume in the first second (FEV1) and the ratio between them were selected to be used as indices of static ventilatory function.
For each subject, height in centimetres during standing without shoes, weight in kilograms and age in years were noted. The body mass index (BMI) was calculated. Ventilatory function tests were conducted using portable Spirometer (Pony Fx (COSMED, Italy) by a trained lung function technician. The Spirometer was calibrated daily. The test procedures were in accordance with the ‘Guidelines for standardization of spirometry [17]. The test recordings were made at 20-25o C room temperatures, and between 9 am to 12 noon to minimize diurnal variation.[18]Tests were performed while subjects were seated comfortably in a chair. Subjects received detailed instruct tions about test procedures, and they practiced the manoeuvre before the test was recorded. The FVC, FEV1, and FEV1/FVC% were recorded. In order to obtain reproducible tests with technical acceptability according to the guidelines for standardization of spirometry, each subject repeated every manoeuvre for three to five times. The largest values for each parameter from acceptable tests were selected [19]. An automated feature of the Spirometer used in this study helped to discard tests with recorded parameters outside the acceptability criteria. On-screen evaluation of the spirograms for smoothness of curve, proper start, duration and end of test was also used to ensure that tests were within acceptability criteria.
Statistical Analysis
Data was expressed as mean and standard deviation(SD). ANOVA was used to detect the significant differences of the ventilatory function between the three groups of the study. Statistical analysis on baseline differences between Caucasian reference values of the ventilatory functions and that of each group under the study were performed using an unpaired student-t test..All P values less than 0.05 were considered statistically significant. The Soft ware package SPSS version 10 was used for all statistical analyses.
Results
This study showed that the more fatness the Saudi child has, the more reduction of ventilatory function he has, it showed also that ventilatory functions among Saudi children are lower the predicted values that requires further investigations to determine the reason behind this findings within each group and between three groups of the study value within the normal weight Saudi children >0.05.
ANOVA statistical analysis showed that increasing degree of obesity or body fatness have negative effect on ventilatory function among Saudi children as the ventilatory function of the obese Saudi children were much lower, than their age matching overweight and normal weight Saudi children but with non statistically significant differences between the three groups .Statistical analysis of the data showed that Saudi children have ventilatory function much lower than the predicted values based on the age/sex specific BMI percentiles (overweight, obese and even the normal weight children). The unpaired t test within group I (normal weight children)showed that the FVC, and FEV1(1.5 L, and 1.3 L respectively) are significantly lower than the predicted values that are supposed to be 1.8 L, and 1.6 L respectively <0.05. On the other hand the FVC % i.e. FEV1/FVC showed no significant difference between the measured and the predicted.
The ventilatory function among the overweight children (Group II) were much more lower than their predicted value, as the FVC was lower than the predicted value by 24 % compared to 17 % among group I ., while the FEV1 was lower than the predicted value by the same percentage as in group 1 (19%). The FVC % among the overweight children was significantly greater than the predicted value by 7 % <0.05 (Table II).
The ventilatory function among the obese children (Group III) showed highly significant difference between their measured valuesand the predicted values <0.05., as their FVC was lower than the predicted value by 37 % compared to 24% in group II and 17 % among group I, while the FEV1 was lower than the predicted value by 30 % compared to 19 %
Discussion
The present study aimed to investigate the effect of different degrees of obesity on ventilatory function among Saudi children by comparing ventilatory function of the overweight and obese Saudi children to their age matching normal weight Saudi children, in addition to comparing the spirometric values of three groups of Saudi children with the predicted values based on preprogrammed Caucasian reference values in standard spirometry. The results of the present study showed that increasing degree of obesity or body fatness have negative effect on ventilatory function as the ventilatory function of the obese Saudi children were much lower, than their age matching overweight and normal weight Saudi children but with non statistically significant differences between the three groups that might be related to the small sample and group size. The present results showed also that the observed values for studied ventilatory parameters of lung function tests (FVC, FEV1, and FEV1/FVC (%)in all Saudi children (normal weight, overweight and obese children were generally lower than the predicted values based on pre-programmed Caucasian reference values with negative correlation between the degree of body fatness and the ventilatory function .
The results showed that the normal weight healthy Saudi children have lower FVC, and FEV1 than the predicted values but only by a smaller percentage compared to the other two groups of obesity , this in addition to having non significant difference between their FVC% and the predicted reference. This means that the normal weight Saudi children do not show any obstructive or restrictive pathology in spite of their lower ventilatory functions that might be related other factors as physical inactivity and sedentary live among normal weight Saudichildren, as previous data suggest a positive relationship between levels of physical activity and pulmonary function [20].
.On the other hand the results show that the overweight and the obese Saudi children have higher FVC% (89.9, and 94 % respectively than the normal percentage the should be between 70% and 80 %, indicating that over weight and obese Saudi children are showing a restrictive lung feature [21].Such reduction in ventilatory function among overweight and obese children could be related to the Deposition of fat in the abdomen, on the diaphragm, and in intercostal muscles that restricts the respiratory system function and decreases lung expansion. These changes, along with the increased amount of fat on the chest wall, lead to decreased functional residual capacity, expiratory reserve volume, forced expiratory reserve volume, and minute ventilation.[22,23]. It has been also stated that Obesity can affect ventilatory function and reduce exercise capacity by its adverse effects on respiratory mechanics, resistance within the respiratory system, respiratory muscle function, lung volumes, work and energy cost of breathing, control of breathing, and gas exchange [24]. Therefore, parents should keep the weight of their children within healthy range, or at least prevent further weight gain if they are overweight [12].
References
- Himes JH, Dietz WH. Guidelines for overweight2 in adolescent preventive services: recommendations from an expert committee. Am J ClinNutr1994; 59: 307-316.
- Whitaker R, Wright J, Pepe M, Seidel K, Dietz W. Predicting obesity in young adulthood from childhood and parental obesity.N Eng J Med 1997; 337: 869-73.
- Vanhala M, Vanhala P, Keinanen-Kiukaanniemi S, Kumpusalo E, Takala J. Relative weight gain and obesity as a child predict metabolic syndrome as an adult. Int J ObesRelatMetabDisord 1999; 23: 656-659.
- Weiss R, Caprio S. The metabolic consequences of childhood obesity. Best Pract Res ClinEndocrinolMetab 2005; 19: 405-419.
- Must A, Jacques P, Dallai G, Bajema D, Dietz W. Long-term morbidity and mortality of overweight adolescents. N Eng J Med 1992; 327:1350-1355.
- Pietrobelli A, Faith M, Allison D, Gallagher D, Chiumello G, Heymsfield S. Body mass index as a measure of adiposity among children and adolescents: a validation study. J Pediatr 1998; 132: 204-210.
- Reilly J, Dorosty A, Emmet P, Study TA. Identification of the obese child: adequacy of the body mass index for clinical practice and epidemiology. Int J Obes2000; 24: 1623-1627.
- Expert panel on the identification, and treatment of overweight in adults. Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults: Executive Summary. Am J Clin- Nutr1998; 68: 899 917.
- Troiano R, Flegal K. Overweight children and adolescents: Description, epidemiology, and demographics. Pediatr1998; 101 (suppl): 497-504.
- Must A, Dallal G, Dietz W. Reference data for obesity: 85th and 95th percentiles of body mass index (wt/ht2) and triceps skinfold thickness. Am J ClinNutr 1991; 53: 839-846.
- http://www.weightwatchers.com
- Alemzadeh R, Rising R, Cedillo M, Lifshitz F. Pediatric obesity. In: Pediatric Endocrinology. 4th ed. Marcel Dekker, Inc., Monticello, NY 2003; 823-858.
- Deane S, Thomson A. Obesity and the pulmonologist. Arch Dis Child 2006;91: 188-191
- McClean KM, Kee F, Young IS, Elborn JS. Obesity and the lungEpidemiology Thorax 2008; 63: 649-654.
- Salome CM, King GG, Berend N. Physiology of obesity and effects on lung function. Journal of Applied Physiology 2010; 108: 206-211.
- Boran P, Tokuc G, Pisgin B, Oktem S, Yegin Z, Bostan O. .Impact of obesity on ventilatory function. Journal de Pediatria2007; 83: 171-176.
- American Thoracic Society. Standardization of Spirometry1994 Update. Am 278 J RespirCrit Care 279 Med 1995; 152: 1107-1136.
- Miller M, Navajas D, Pedersen O, Wanger J. Interpretative strategies for lung function tests. Eur 281 Respir J 2005; 26: 948-968.
- American Thoracic Society. Standardization of Spirometry, 1994 Update. Am J RespirCrit Care 283 Med1995; 152: 1107-1136.
- Cheng YJ, Macera CA, Addy CL, Sy FS, Wieland D, Blair S. Effects of physical activity onexercise tests and respiratory function. Br J Sports Med 2003; 37: 521-528.
- Pierce R. Spirometry: an essential clinical measurement. AustFamPhysician 2005; 34: 535-539.
- Marik P, Varon J. The obese patient in the ICU. Chest 1998; 113:492-498.
- Schunkert H. Obesity and target organ damage: the heart. Int J Obes 2002; 26 (S4): S15-S20.
- Koenig SM.Pulmonary complications of obesity.Am J Med Sci 2001; 321: 249-279.