Case Report - Research in Clinical Dermatology (2018) Volume 1, Issue 2
Double bipedicled fasciocutaneous flap for reconstruction of an extensive upper extremity defect: A case report.
Martain PJ Loonen1* and Jessica Konopka21Department of Plastic and Reconstructive Surgery, King’s College Hospital London, UAE.
2Aesthetic Private Medical Practice Krakow.
- Corresponding Author:
- Martain Pierre Jean Loonen, M.D., Ph.D., FCCP
Consultant Plastic Surgeon Department of Plastic and Reconstructive Surgery King’s College Hospital London Podium 2
Shining Towers, Mubarak Bin Mohammed Street، Al Khalidiyah Abu Dhabi - United Arab Emirates
Phone: + 971- 54- 3204135
E-mail: mloonen@yahoo.com
Accepted date: November 8, 2018
Citation: Loonen MPJ. Double bipedicled fasciocutaneous flap for reconstruction of an extensive upper extremity defect: A case report. Res Clin Dermatol. 2018;1(2):5-7
DOI: 10.35841/clinical-dermatology.1.2.5-7
Visit for more related articles at Research in Clinical DermatologyAbstract
Reconstruction of extensive upper extremity defects with local or regional flaps is challenging. This case report presents a patient with an enlarging and easily bleeding irregular mass at the right distal dorsal-radial upper arm since months. A MRI revealed a 11 × 10 cm ill-defined lobulated soft tissue mass. An ultrasound guided core biopsy of the right arm showed histological features favor of a high grade malignancy, suspicious for Merkel Cell carcinoma. A complete excision of the lesion was performed followed by a double bipedicled fasciocutaneos flap. The double bipedicled flap is a reproducible flap for extensive upper arm defects and no former publications were found using this type of flap for upper extremity defects.
Keywords
Reconstruction; Bipedicled flap; Upper extremity.
Introduction
Reconstruction of extensive upper extremity defects with local or regional flaps is challenging. Adipocutaneous defects around the shoulder can be reconstructed using a lateral arm flap [1]. Defects around the elbow can be reconstructed with the radial recurrent artery flap or a proximal based radial forearm flap [2].
Extensive defects between the shoulder and elbow area are technically challenging with limited reconstructive options. A pedicled latissimus dorsi muscle flap or musculocutaneous flap may cover such defects but with a donor side morbidity and degree of weakness with reduced mobility at the shoulder. Its use is further limited in extensive distal defects of the upper arm. Skin grafts have less tolerance to postoperative radiotherapy, lack volume and will not survive on exposed less vascularized tendon or bone areas [3-5].
The author (MPJ Loonen) describes a reconstruction of an extensive upper arm defect after excision of a Merkel Cell carcinoma using a double bipedicled fasciocutaneous flap.
Case Report
A 56 year old Pakistani man presented an enlarging and easily bleeding irregular mass at the right distal dorsal-radial upper arm for months. A MRI revealed a 11 × 10 cm ill-defined lobulated soft tissue mass. The lesion appeared close to the adjacent muscle in T1 with hyper intense foci and was heterogenously hyperintense in T2 with a feeding vessel (Figure 1).
An ultrasound guided core biopsy of the right arm showed histological features favor of a high grade malignancy, suspicious for Merkel Cell carcinoma. The PANCK, SYNAP, CD20 markers were positive.
Wide excision of the tumor was performed with superficial muscle fibers of the triceps brachii muscle by the oncology surgeon. Histopathological evaluation revealed tumor free margins with lymphovascular invasion (pT3NxMx). A Sentinel node biopsy showed no tumor cells. The final size of the defect was 12.5 × 11.5 cm.
The extensive defect (Figure 2) with exposed triceps brachii tendon was reconstructed using a double bipedicled fasciocutaneous flap design (Figure 3).
The width of each flap was 50% of the width of the defect. The height of each flap is 75% of the height of the defect. The vascular perfusion of the flap was maintained using this flap ratio. Increasing the flap height may be indicated in case tension is experienced during closing of the flap of both flaps in the middle part but may limit the vascular perfusion of the flap (Figure 4). The fascia was approximated at the medial part of both flaps using PDS 3-0® sutures. The skin was approximated using PDS 4/0® deep dermal sutures. A Monocryl 4-0® intradermal suture was used. The donor defects were reduced in size using a PDS 4/0 purse string deep dermal suture. The remaining defects were closed using non-meshed split-thickness skin grafts with drainage openings made in the grafts. The grafts were fixated using Vicryl Rapide 5-0® transcutaneous sutures. The small dog ears were not corrected at the cranial and caudal ends of the flaps to prevent interruption in the flap perfusion. Dog ear correction can be completed 4-6 months postoperative. A subcutaneous drain was placed and removed when the drainage was less than 25 cc/24 hours (Figure 5). A light compressive non-adhesive dressing was placed on the skin grafts and removed 5 days after the surgery. No pressure was applied on the bipedicled flaps.
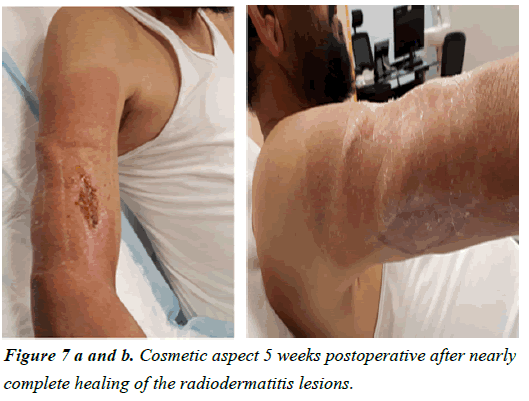
The initial postoperative course was uncomplicated. Adjuvant radiotheraphy was started several weeks postoperative. An extensive radio-dermatitis developed especially at the nonoperated skin areas probably due to asymmetrical radiation (Figure 6). The wounds healed by secondary intention using hydrogel wound dressings (Figure 7).
Discussion
Extensive defects between the shoulder and elbow area are technically challenging. A defect sized 12.5 × 11.5 cm was closed using a double bipedicled flap. The double bipedicled flap is able to closure large defects without significant donor side morbidity or functional morbidity as in the pedicled latissimus dorsi muscle or myocutaneous flap. The double bipedicled flap gives, in general, more flap mobility with more extensive transposition of the flaps compared with only one extensive bipedicled flap. The flap design is reproducible. Other reconstructive options like the pedicled latissiumus dorsi flap or a free flap are still available in case of flap failure. A comparable case report using the double bipedicled flap for upper extremity defects was not found using the National Center for Biotechnology Information (NCBI, Pubmed®) database.
Conclusion
The double bipedicled flap is a reproducible flap for extensive upper arm defects.
References
- Chang EI, Ibrahim A, Papazian N, et al. Perforator mapping and optimizing design of the lateral arm flap: Anatomy revisited and clinical experience. Plast Reconstr Surg. 2016;138:300e-6e.
- Devale MM, Munot RP, Bhansali CA, et al. Awkward defects around the elbow: The radial recurrent artery flap revisited. Indian J Plast Surg. 2016;49:357-361.
- Blackburn NE, Mc Veigh JG, Mc Caughan E, et al . The musculoskeletal consequences of breast reconstruction using the latissimus dorsi muscle for women following mastectomy for breast cancer: A critical review. Eur J Cancer Care (Engl). 2018;27:e12664.10.
- Tolhurst DE, Haeseker B, Zeeman RJ, et al. The development of the fasciocutaneous flap and its clinical applications. Plast Reconstr Surg. 1983;71:597-606.
- Hallock GG. Principles of fascia and fasciocutaneous flaps. Weinzweig J, ed. Plastic Surgery Secrets. Philadelphia, Pa: Hanley and Belfus, Inc; 1999.