Research Article - Biomedical Research (2017) Volume 28, Issue 11
Bortezomib in the initial treatment of inducing chemotherapy of multiple myeloma and autologous stem cell transplantation pre-treatment
Gang Zhang1, Lin-Lin Yang2, Jing Yu3, Qi-Yu Sheng4 and Li Li5*
1Department of Pain Management, Jinan Central Hospital Affiliated to Shandong University, Jinan, Shandong, PR China
2Department of Breast and Thyroid Surgery, Jinan Central Hospital Affiliated to Shandong University, Jinan, Shandong, PR China
3Operating Room, Jinan Central Hospital Affiliated to Shandong University, Jinan, Shandong, PR China
4Nursing Department, Jinan massage hospital, Jinan, Shandong, PR China
5Departement of Acupuncture and Massage, Jinan Massage Hospital, Jinan, Shandong, PR China
Accepted date: March 25, 2017
Abstract
Objective: This study investigates the effects of bortezomib on the initial treatment of inducing chemotherapy of multiple myeloma and autologous stem cell transplantation pre-treatment.
Methods: Eight cases of patients with multiple myeloma were treated with BDT chemotherapy regimen for four cycles (bortezomib 1.3 mg/m2 d 1, d 4, d 8, d 11, dexamethasone, 20 mg, d 1-4, d 9-12; 100-200 mg thalidomide for long term). Eight cases of patients with autologous peripheral blood stem cell transplantation pre-treatment were performed using bortezomib+Melphalan (bortezomib 1.0 mg/m2, -6 d, -3 d, +1 d +4 d; Melphalan 200 mg/m2, -2 d). The mobilization regimen was cyclophosphamide +bortezomib+dexamethasone+G-CSF5~10 μg/(kg/d-1).
Results: The partial or complete remission occurred in the eight cases of patients with multiple myeloma after BDT chemotherapy for four cycles. Stem cell collection was successful. Meanwhile, the hematopoietic functions of patients with autologous stem cell transplantation were successfully reconstructed.
Conclusion: The bortezomib combined with autologous stem cell transplantation is an effective method for the treatment of multiple myeloma. It is safe and reliable. Moreover, the maintenance therapy of bortezomib after transplantation may prolong the survival time of patients and improve the quality of life.
Keywords
Multiple myeloma, Multiple myeloma, Bortezomib
Introduction
Multiple myeloma is a common malignant plasmocyte dyscrasia. The main clinical symptoms include ostealgia, anemia, repeated infection, renal damage, and others [1]. In recent years, bortezomib has been widely used in chemotherapy and autologous stem cell transplantation induction to alleviate the condition and increase the survival rate [2]. However, limited studies are conducted on the pretreatment of bortezomib in autologous stem cell transplantation. Therefore, the effects of bortezomib in the initial treatment of inducing the chemotherapy of multiple myeloma and autologous stem cell transplantation pretreatment were investigated in this study to provide reference for clinical treatment. The report is shown as follows.
General Data and Methods
General data
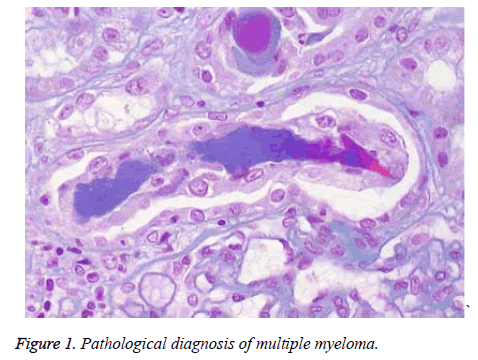
Eight cases of patients with initial myeloma were randomly selected from the Department of Hematology in our hospital from January 2014 to April 2016. All patients accorded with the diagnostic criteria of multiple myeloma after examination [3]. The pathological map is shown in Figure 1. Severe cardiovascular diseases, liver and kidney disorders, and serious lung diseases were excluded. A total of five male cases and three female cases aged 38-62 years old, with an average of 43.67 ± 8.29 years, were included. The following were considered: M protein type: three cases of IgG type, three cases of light chain type, one case of IgD type, and one case of IgA type. All patients suffered from multiple myeloma III. The study was approved by our hospital medical ethics committee and by the patients, who signed informed consents.
Therapeutic regimen
Pre-transplant chemotherapy: The autologous peripheral blood stem cell transplantation pre-treatment was performed in the eight cases of patients, with bortezomib+melphalan (bortezomib 1.0 mg/m2, -6 d, -3 d, +1 d, +4 d; melphalan 200 mg/m2, -2 d).
Mobilization regimen
The mobilization regimen was cyclophosphamide+bortezomib +dexamethasone G-CSF5~10 μg/(kg·d), bortezomib 1.3 mg/m2, d 1, d 4, d 8, d 11, d 1, dexamethasone 20 mg, d 4, d 8, d 1, cyclophosphamide 1.5 mg/m2, d 9. After chemotherapy, the hemogram was detected periodically. The PBSC of patients was collected after mobilization for 4 d. The patients took calcium orally to prevent hypocalcemia. The albumin, hematopoietic stem cells, and 706 dextran were proportionally mixed and stored in a -80°C refrigerator.
Pre-treatment regimen
The autologous peripheral blood stem cell transplantation pretreatment was performed in the eight cases of patients, with bortezomib+melphalan regimen (bortezomib 1.0 mg/m2, -6 d, -3 d, +1 d, +4 d; melphalan 200 mg/m2, -2 d).
Supportive treatment
The patients entered the 100 sterile laminar flow wards after undergoing medicated bath. The peripheral central venous catheter was retained. Meanwhile, norfloxacin and fluconazole were taken by the patients to prevent infection. The urine of the patients were alkalized and hydrated during the pre-treatment. If the temperature was above 38°C, then the broad-spectrum antibiotic should be intravenously dripped. If the neutrophils of patients were the fewest, then G-CSF5~10 μg/(kg·d) should be subcutaneously injected. If the patients appeared to be anemic, then red blood cell suspension should be infused. If the patients tended to bleed, then the single donor platelet should be infused.
Curative effect judgement
The clinical efficacy was measured according to the international standard set by the International Myeloma Working Group, including Complete Remission (CR), Partial Remission (VGPR), Tiny Remission (PR), and Stable Condition (SD) [4].
Results
Peripheral blood cell collection
The number of autologous peripheral blood stem cells in the eight cases of patients is shown in Table 1.
| Cases | MNC (× 108/kg) | CD34+cell (× 106/kg) |
|---|---|---|
| 1 | 9.48 | 3.46 |
| 2 | 5.07 | 6.21 |
| 3 | 5.15 | 3.08 |
| 4 | 6.26 | 3.43 |
| 5 | 5.87 | 3.86 |
| 6 | 5.61 | 4.24 |
| 7 | 6.27 | 4.43 |
| 8 | 6.44 | 3.67 |
Table 1. Peripheral blood cell collection.
Hematopoietic reconstitution time
The hematopoietic functions of the eight cases of patients recovered after they underwent the autologous peripheral blood hematopoietic stem cell transplantation. The clinical implantation times of neutrophils were 14 and 16 d. The clinical implantation times of the platelet were 25, 29, and 22 d.
Clinical efficacy
Among the eight cases of patients with multiple myeloma undergoing BDT chemotherapy for four cycles, one case had complete remission, and seven cases had partial remission (Table 2). The stem cell collection was successful. Meanwhile, the patients’ hematopoietic functions were successfully reconstructed after autologous stem cell transplantation.
| Cases | β2-microglobulin (mg•d L-1) | Myeloma cell (%) | M type | Immunoelectrophoresis |
|---|---|---|---|---|
| 1 | 0.278 | 0 | IgG type | Normal |
| 2 | 0.611 | 0 | light chain type | Normal |
| 3 | 0.275 | 0 | light chain type | Normal |
| 4 | 0.197 | 0 | IgG type | Normal |
| 5 | 0.208 | 0 | IgD type | Normal |
| 6 | 0.291 | 0 | light chain type | Normal |
| 7 | 0.314 | 0 | IgD type | Normal |
| 8 | 0.297 | 0 | IgA type | Normal |
Table 2. Re-examination result of autologous transplantation for 28 d.
Adverse reactions
During the inducing chemotherapy, two cases had fever, and one case had peripheral neuritis. The adverse reactions were improved in three cases after treatment. The patients could tolerate the inducing chemotherapy. During the mobilization chemotherapy, among the eight cases of patients, only cases of patients had mild diarrhea, and one case had slight hands and feet numbness. In addition, the adverse reactions were milder, and the patients could tolerate the mobilization regimen. During the autologous hematopoietic stem cell transplantation, two cases showed nausea and vomiting; three cases had diarrhea, fatigue, and other symptoms; and three cases had neutropenia and mild infection. The patients had no serious adverse reaction, which was improved after symptomatic treatment. Eight patients had no liver function lesion before and after autologous hematopoietic stem cell transplantation, which was not aggravated after transplantation.
Discussion
Multiple myeloma is the most common malignant plasmocyte dyscrasia, also known as myeloma, plasmocyte myeloma, or Kahler disease [5]. It is characterized by the malignant proliferation of monoclonal plasmocytes and a large amount of secretions of monoclonal immunoglobulins. The malignant plasmocytes can uncontrolledly proliferate and extensively infiltrate a large amount of monoclonal immunoglobulin deposits. Normal polyclonal plasmocytes proliferate, and the polyclonal immunoglobulin secretion is inhibited, so that the widespread bone destruction, repeated infections, anemia, hypercalcemia, hyperviscosity syndrome, renal insufficiency, and other clinical manifestations occur [6]. The incidence of multiple myeloma is about 1/30,000 and is higher in males. It frequently occurs around the 40-year-old population. Moreover, its incidence in melanoderm was higher in others than in Caucasians [7].
Traditional chemotherapy regimen has a lower remission rate for multiple myeloma. In addition, the disease cannot be completely remitted. The survival of patients is shorter. The therapeutic goal of multiple myeloma is to prolong the survival time of patients, induce and maintain the remission, prevent or delay the progression of disease, and reduce the symptoms and adverse reactions [8]. Bortezomib is a novel protease-like activity reversible inhibitor. It has cytotoxicity against many cancer cells and can delay tumor growth including multiple myeloma [9]. The effects of bortezomib in the initial treatment of inducing chemotherapy of multiple myeloma and autologous stem cell transplantation pre-treatment were investigated in this study. The results showed that eight cases of patients achieved partial or complete remission after BDT regimen chemotherapy. The stem cell collection was successfully conducted. The hematopoietic functions of patients were successfully reconstructed after autologous stem cell transplantation [10]. The results showed that bortezomib in the pre-treatment of autologous stem cell transplantation in the eight cases of patients with multiple myeloma III, the hematopoietic reconstitution, were successful. The disease could remit, and the patients could better tolerate the pretreatment. There were less transplantation-related complications, suggesting that bortezomib combined with autologous peripheral blood stem cell transplantation could effectively treat multiple myeloma.
Conclusion
In summary, bortezomib combined with autologous stem cell transplantation is an effective method in the treatment of patients with multiple myeloma. It is safe and reliable. Meanwhile, bortezomib maintenance therapy after transplantation may prolong the survival time of patients and improve the quality of life.
References
- Hideshima T, Chauhan D, Schlossman R, Richardson P, Anderson KC. The role of tumor necrosis factor alpha in the pathophysiology of human multiple myeloma: therapeutic applications. Oncogene 2001; 20: 4519-4527.
- San Miguel JF, Schlag R, Khuageva NK, Dimopoulos MA, Shpilberg O. Bortezomib plus melphalan and prednisone for initial treatment of multiple myeloma. N Engl J Med 2008; 359: 906-917.
- Hallek M, Bergsagel PL, Anderson KC. Multiple myeloma: increasing evidence for a multistep transformation process. Blood 1998; 91: 3-21.
- Kuehl WM, Bergsagel PL. Multiple myeloma: evolving genetic events and host interactions. Nat Rev Cancer 2002; 2: 175-187.
- Zhang W, Chen C, Zhang C, Duan J, Li Y, Ma H, Yao H, Meng A, Shi J. Probing the binding interaction of terbinafine with human serum albumin via multiple fluorescence spectroscopy and molecular modeling. Lat Am J Pharm 2016; 35: 1399-1406.
- Wang X. A novel pyran annulated heterocyclic compound: synthesis, crystal structure and activity against central nervous system multiple glioma. Lat Am J Pharm 2015; 34: 1446-1448.
- Han F, Li QW, Wang S, Deng J. Urination treatment drug corylifolinin exhibits influence towards therapeutic potential of multiple drugs. Lat Am J Pharm 2015; 34: 397-399.
- Zhou Y, Xu X, Sun Y, Wang H, Sun H, You Q. Synthesis, cytotoxicity and topoisomerase II inhibitory activity of lomefloxacin derivatives. Bioorg Med Chem Lett 2013; 23: 2974-2978.
- Sun Y, Wang HP, Zhou Y, You, QD. Recent advances in non-campto-thecin DNA topoisomerase I inhibitors as anticancer drugs. Prog Pharm Sci 2011; 35: 385-395.
- Kim SH, Sun Y, Kaplan JA, Grinstaff MW, Parquette JR. Photo-crosslinking of a self-assembled coumarin-dipeptide hydrogel. New J Chem 2015; 39: 3225-3228.