- Biomedical Research (2013) Volume 24, Issue 2
Blood glucose and lipids profile in non-diabetic patients taking propranolol.
Mohammad Ayatollahi1 and Golrasteh Kholasehzadeh21Department of Pharmacology, Schools of Medicine and Pharmacy, Yazd Shahid Sadoughi University of Medical Sciences,Yazd, Iran
2Department of Psychiatry, School of Medicine, Yazd Shahid Sadoughi University of Medical Sciences,Yazd, Iran
- *Corresponding Author:
- Mohammad Ayatollahi
Department of Pharmacology
Schools of Medicine and Pharmacy
Yazd Shahid Sadoughi University of Medical Sciences
Yazd, Iran
Accepted date: January 21, 2013
Abstract
This study investigated the effects of propranolol (P) as a non-selective b-adrenergic receptor blocker on blood glucose and lipid profile in non-diabetic patients. The results of this project will be a guide to prevent occurrence of hypoglycemic signs (tachycardia, palpitation, feeling hunger, blood pressure changes, anxiety and sweating) and its undesired consequences in P takers. Thirty seven patients chosen were without any serious cardiovascular complications and also without hearing, intellectual and visual defects. Fasting blood glucose and lipid profile of the patients were estimated by autoanalyser instrument, BT3000. Only comparison between blood HDL level before taking P and after an 8-week period of taking P became significant (Pv = 0.034) and the variable mentioned showed a reduction of level in most of the P takers. It is concluded that if a patient needs a beta adrenergic blocker, a selective beta 1 blocker should be considered cautiously.
Keywords
Propranolol, hypoglycemia, hyperglycemia, blood lipid
Introduction
Some studies showed that propranolol (P) causes hypoglycemia and/or hyperglycemia. Hypoglycemia is moreover hazardous for subjects using P (1, 2, 3). Therefore, to educate the patients who use P in controlling heart rate, hypertension, and for prevention of migraine attacks at Yazd city/Iran about the undesired consequences of chronic usage of P on blood glucose and lipid profile, the present investigation aimed to evaluate the effects of P as a non-selective b-adrenergic receptor blocker on blood glucose and lipid profile in non-diabetic patients. It will be a guide to prevent occurrence of hypoglycemic signs (tachycardia, palpitation, feeling hunger, blood pressure changes, anxiety, and sweating) and its undesired consequences in P takers.
Methodology and Sampling
Female patients aged 21–60 years without serious cardiovascular complications, and intellectual and visual defects were the candidates visited by the physician. Propranolol (P) was prescribed for them to control heart rate, and hypertension, and to prevent migraine attacks. After completing the questionnaires to obtain information for each patient and before taking P, patients were referred to clinical pathology laboratory of the university (following 10-12 hours of fasting) to measure the blood glucose and lipid profile (cholesterol, HDL, LDL, and triglyceride). Autoanalyser instrument BT3000 was used to measure levels of the above-mentioned parameters (the method of glucose oxidase for glucose level, cholesterol oxidase for cholesterol and HDL levels, triglyceride oxidase for triglyceride level and formula for LDL level considered). The patients were requested to revisit the laboratory after a 4- and a 8-week period of taking P. At the end, the results were subjected to statistical analysis and concluded.
Results
The results obtained for the blood glucose and lipids (cholesterol, triglyceride, HDL and LDL) profile of 23 female patients aged 21-60 years before taking P and after a 4-week period of taking P and 14 female patients aged 21-60 years before taking it , after a 4 and an 8 week period of taking P , in addition to between after a 4- and a 8-week period of taking P were compared. Changes in variables were not significant except in HDL level in comparison to before taking and after a 8 week period of taking P that showed a significant difference. The obtained data were statistically analyzed using SPSS and a paired T-test was done by the computer.
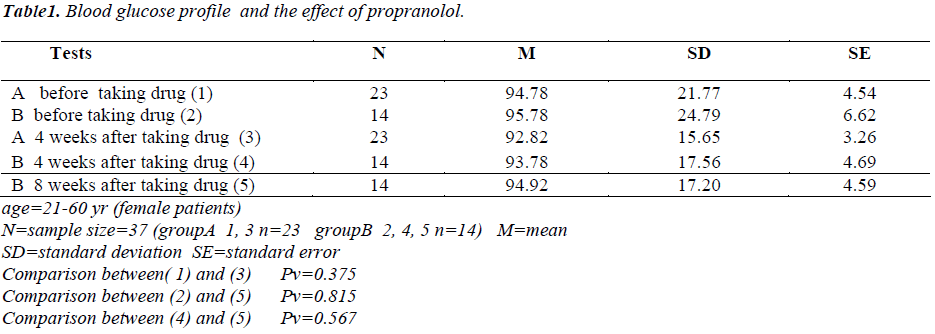
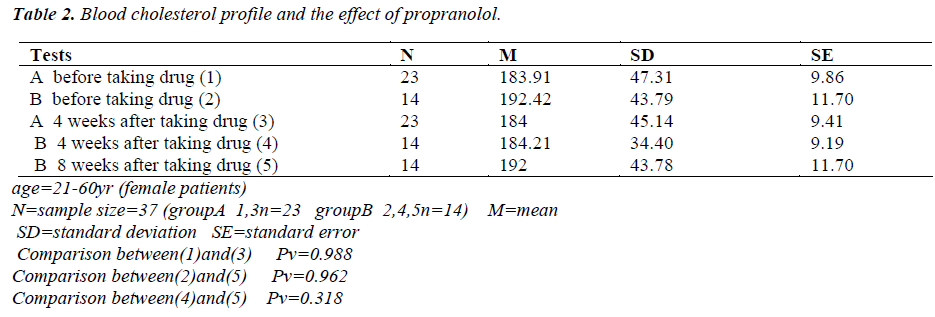
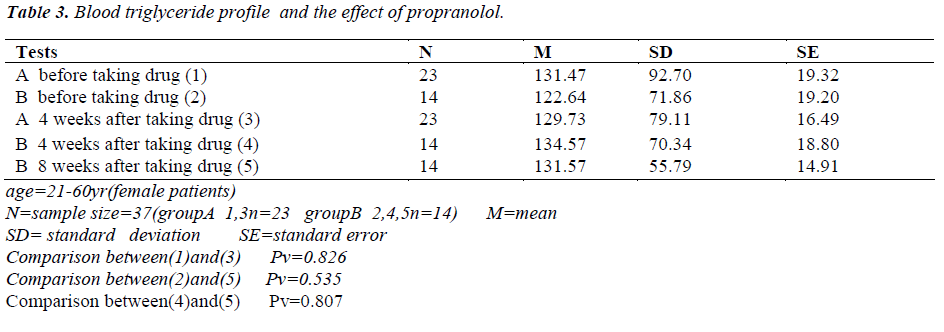
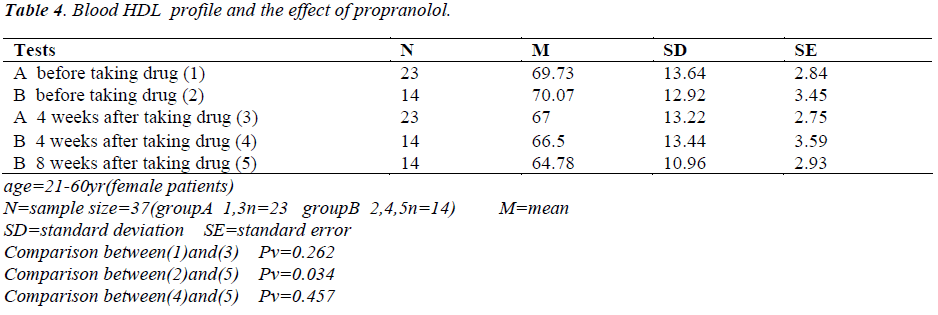
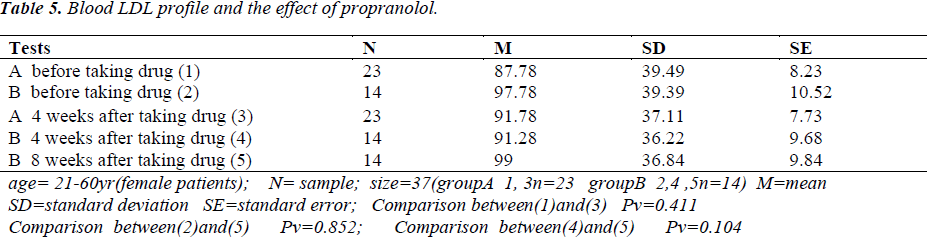
Tables 1-5 show the results of measured blood glucose and lipids profile in patients. N=37
Discussion and Conclusion
Comparison of the results before medication, after a 4- and a 8-week period of taking P did not show any significant differences (Tables 1, 2, 3, 5) except in the blood HDL level between before taking P and after a 8 week period of taking P (Pv = 0.034) and the variable mentioned above showed a reduction of level in most of the P takers (Table 4). One study showed that after a 4 and a 8- week period and more than one year of P taking affected the glucose tolerance and caused a significant reduction in blood glucose level [5,6]. Another study showed that after taking 10 mg/kg dl-Propranolol by gavage in 5- week-old rats (Wistar Kyoto) during a 10-week period, the total cholesterol, phospholipid and total fat levels in serum and liver were higher in the experimental group than in non-drug group. The serum glucose level in the drug group was higher than that in the non-drug group in the last weeks of the treatment [6]. The value of serum immunoreactive insulin in the drug group was lower than that in the non-drug group [6]. These results may suggest that P inhibits lipase activity sensitive to hormone in first weeks of treatment and affects the cholesterol biosynthesis and or catabolism [6]. P can be detrimental for the diabetic patients in two ways. Firstly, P can suppress glycogenolysis by blocking the b2-adrenergic receptors located in muscle and liver and thereby preventing an important mechanism to improve hypoglycemia (occurred when insulin dosage is excessive). Secondly, P can suppress the tachycardia as an early warning signal that of hypoglycemia. The patients should be educated for occurrence of sweating, hunger, fatigue and weak concentration that are felt in reduction of blood glucose level [7]. The comparison of the results of the project (Tables 1-5) with other studies suggest that the other studies can not be rejected but the experiments should be performed with doses higher than 40 mg to show whether P can cause a significant change in the abovementioned variables or not. An emphasized caution should be considered for the patients taking P with one or two hypoglycemic drugs and blood glucose level measured regularly [4]. It is concluded that if a patient needs a beta adrenergic blocker, a selective b1-blocker should be considered cautiously and the patient should be cared with frequent measurings of blood glucose level [1-3]. The patients should be educated for severe hypoglycemic signs (tachycardia, palpitation, feeling hunger, blood pressure changes, anxiety, weak concentration and sweating) that are extremely vital [7].
Acknowledgement
1-Deputy for Research of Yazd University of Medical Sciences for financial support, Yazd /Iran.
2-My colleague: Drs. Golrasteh Kholasehzadeh (psychiatrist) to present patients, Yazd /Iran.
3-My colleague: Dr. Hossein Fallahzadeh (statistician) to analyze data, Yazd /Iran.
4-My colleague: Dr. Mahmoud Akhavan Tafti and Staff from Central Clinical Pathology Laboratory of Yazd University of Medical Sciences to measure blood glucose and lipids levels, Yazd /Iran.
5-My wife and daughters: Mrs. Razieh Mashshaei, Drs. Shaghayegh (MD), Arghavan (MD) and Gelayol (Medical student) Ayatollahi to help me, Yazd /Iran.
References
- Mary Anne Koda–Kimble, LIoyd Yee Young. Applied Therapeutics: The clinical use of drugs. U. S .A, Lippincott Williams & Wilkins, 2001, 7th edition; pp.12-30.
- Patricia Clarkson, John skinner, Brenda Hughes, Chery Olsen, Lijla Brkic(Reviewed). Propranolol Pharmacology. No 1999; 1, p. 2.
- The P–I–E–N–O Parkinson’s List Drug Database. Propranolol / Inderal TM, Antihypertensive, Non–selective beta blockers, search or browse 11 years of Parkinson Email list messages (1993-2004).
- Gaafar K, Salama S, El Batran S. Studies on the glycemic and lipidemic effect of atenolol and propranolol in normal and diabetic rats. Arzneimittelforschung, 1994; 44(4): 496-501.
- Gautam VK., Vasavada JP., Khanijo SK. A study of oral glucose tolerance test in patients of hypertension receiving propranolol. Indian Heart J 1989; 41(4): 261-264.
- Tonooka M., Kawashima I., Sakashita M., Yasuhara H., Sakamoto K. Effect of chronic treatment of propranolol on lipid metabolism in spontaneously hypertensive rats (SHR). Jpn J Pharmacol 1985; 37(4): 335-344 .
- Lehne Richard A. Pharmacology for Nursing Care: W. B. Saunders Company. 2009. 7th Edition; p.169.