Research Article - Biomedical Research (2016) Volume 27, Issue 4
Application of one stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly in late kyphosis deformity
Jie Liu1*, Lei Cao2, Shifang Guo1, Hanguo Zhang1, Wen Xue1, Zongru He1 and Yaowen Qian11The Department of Orthopaedics, The People’s Hospital of Gansu, PR China
2Gansu Provincial Maternity and Child-Care Hospital, PR China
- *Corresponding Author:
- Jie Liu
The Department of Orthopaedics, The People’s Hospital of Gansu, PR China
Accepted on March 07, 2016.
Abstract
To determine the effectiveness of the application of one stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly in late kyphosis deformity. 39 cases of late kyphosis deformity treated with one stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly were retrospective reviewed. The height of anterior and posterior margin of vertebral body, local sagittal Cobb angle and vertebral wedge angle pre and post-operation were measured. All cases were followed up for 24-84 months (average of 32 months). The height of anterio margin of vertebral body pre-operation was 0.8575 ± 0.742 cm, while it was 2.675 ± 1.615 cm at latest follow up, which was significantly increased. The height of posterior margin of vertebral body was 2.878 ± 1.701 cm, while it was 2.805 ± 1.576 cm, at latest follow up, which was not significantly different compared with the results pre-operation. The Cobb angle of kyphosis at latest follow up post -operation was 11.988 ± 5.474°, which was significantly different compared with the results pre-operation. The average correction rate of kyphosis at latest follow up was 71.1%. The trauma vertebral wedge angle was 31 ± 9.899° pre-operation and significantly decreased at 6.062 ± 7.06° post-operation. 33 cases with spinal injury were classified according to Franke 1 value system. One stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly is an effective surgical procedure for the treatment of the late kyphosis deformity. The long-term effect is reliable.
Keywords
Late kyphosis deformity, Thoracolumbar spine, Vertebral wedge angle.
Introduction
The thoracolumbar spine is a common site of spinal fractures. The back pain, deformity and neurological dysfunction caused obsolete thoracolumbar vertebral kyphosis deformity were mainly induced by delayed treatment and malpractice on fracture, early infection. Surgical treatment is indicated for these patients with progressive deformity, refractory back pain, or deterioration of neurological status, and such operations are challenging for spine surgeons. Most researches demonstrated that the kyphosis more than 20° should be corrected by surgery [1]. 39 cases of thoracolumbar kyphosis deformity treated with one stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly from Feb 2007 to Feb 2011 at our department were retrospective reviewed. The treatment results are as follows.
Clinical Data
General information
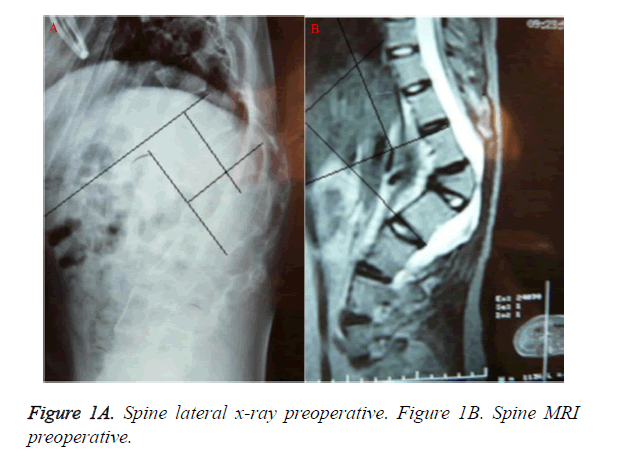
There were total 39 cases in this study, 24 cases of male, 15 cases of female, aged 17-68 years (average 41 years old). The medical history was 13-84 months (average of 47 months). The Cobb angle of kyphosis was 49.75+27.524° (Figure 1). 33 cases with spinal injury were classified according to Franke 1 value system.
There were 3 cases of grade A, 15 cases of grade B, 10 cases of grade C and 5 cases of grade D. 17 patients got obviouse waist and back pain, especially serious at the sit moment. 27 cases were diagnosed with lumbar vertebra fracture. 12 cases were patients with spinal tuberculosis. All patients were followed up for 24 to 84 months (average of 32 months).
Treatment
Patients were set in prone position with soft pillow underlying. According to the extent of apical vertebral pre operation, the rear structure was exposed. “C” type X-ray machine was used to locate the disease during the operation. Pedicle screws were placed in the 2 to 3 vertebral body around the diseased vertebral body. Temporary fixation with rod was put in the less compressed lateral of spinal cord to prevent spinal cord shear damage after vertebral body resection. The spinous process of apical vertebra, vertebral plate, transverse process and vertebral pedicle were resected. Vertebral body together with its upper lumbar disc and cartilage plate compressing spinal cord induced by apical vertebra kyphosis was resected through bilateral pedicles of apical vertebra using “eggshell” technology. After complete decompression, the anterior and lateral bony shell of the top vertebral body was broken in situ by curette. Parts of the vertebral plate of the upper and lower vertebral body of apical vertebra were bitted away to prevent the compression of the thecal sac and spinal cord by vertebral plate. Through temporarily channels after vertebral pedicle resection in fixtion lateral, distracter was put to brace anterior spinal column. Intervertebral bone graft was performed with a bite of the vertebral body cancellous bone or titanium cage with appropriate length. The rod with appropriate length was preflexed and connected to pedicle screw. Release the emporary fixation rod, fixed with preflexed rod and compressed the apical vertebra and high position disc. In the process of compression, spinal cord monitoring instrument would be used. The compression would be stopped, when spinal cord nerve potential is abnormal. After the recovery, the compression would be continued until the orthopedic effect was achieved.
Nerve stripping ion was used to explore whether there was broken bones retrusion in front of the dura mater. If there was, the broken bones would be put forward or resected to avoid the compression on the inferior part of dura mater. Antibiotics were routine used, the drainage tube would be pulled out 24 to 48 h after operation. The patients can do some physical activity with orthosis 1 week after operation. The wearing time with orthosis should be longer than 6 months.
Detection index
3.1 Height of anterior margin of vertebral body, which was the distance between the upper and lower end plates of the anterior margin of vertebral body. In some patients with severe lesions, the anterior margin was completely lost. The height of anterior margin of vertebral body was replaced by the distance between the upper and the lower endplates of the upper and lower vertebral body around the diseased vertebra.
3.2 Height of posterior margin of vertebral body, which was distance between the upper and lower end plates of the posterior margin of vertebral body. In some patients with severe lesions, the posterior margin could not be identified. The height of posterior margin of vertebral body was replaced by the distance between the upper and the lower endplates of the upper and lower vertebral body around the diseased vertebra.
3.3 Local sagittal Cobb angle, also known as kyphotic angle, which was the Cobb angle of the upper endplate of the upper vertebral body of the injured vertebral body and the lower endplate of the lower vertebral body of the injured vertebra. It indicated the severity of the kyphosis deformity.
3.4 Injured vertebral wedge angle, which was the cut angle of the cut angle of the upper and lower endplates of the injured vertebra. It reflexed compression of vertebral body, and the severity of the kyphosis deformity to a certain extent.
Statistical analysis
All statistical analysis was performed using SPSS11.0 software. The measurement data were shown as x ± s. The comparison between the groups before and after the operation was performed using t test. P<0.05 was considered as statistically significantly different.
Results
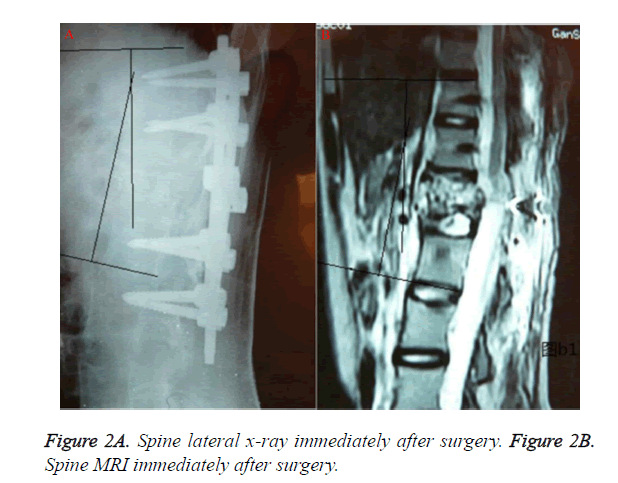
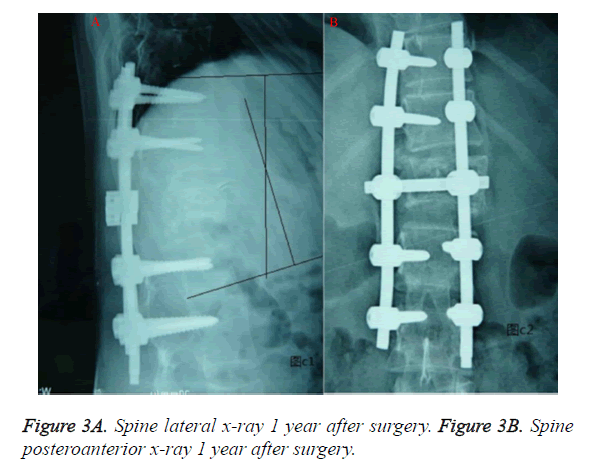
All patients were followed up for 24 to 84 months (average of 32 months). The height of anterio margin of vertebral body pre-operation was 0.8575 ± 0.742 cm, while it was 2.675 ± 1.615 cm at latest follow up, which was significantly increased. The height of posterior margin of vertebral body was 2.878 ± 1.701 cm, while it was 2.805 ± 1.576 cm at latest follow up, which was not significantly different compared with the results pre-operation. The average Cobb angle immediately after operation was 13° (4°-26°) (Figure 2). The Cobb angle of kyphosis at latest follow up post-operation was 11.988 ± 5.474°, which was significantly different compared with the results pre-operation. The average correction rate of kyphosis at latest follow up was 71.1%. (Figure 3) The trauma vertebral wedge angle was 31 ± 9.899° pre-operation and significantly decreased at 6.062 ± 7.06° post-operation (Table 1).
| Preoperative | The latest follow up | |
|---|---|---|
| Height of anterio margin of vertebral body (cm) | 0.8575±0.742 | 2.675±1.615* |
| Height of posterio margin of vertebral body (cm) | 2.878±1.701 | 2.805±1.576* |
| kyphotic angle(°) | 49.75±27.524° | 11.988±5.474°* |
| Wedge angle(°) | 31±9.899° | 6.062±7.06°* |
Table 1. The correction of the late kyphosis deformity post-operation.
The Frankel 1 grade of spinal cord injury at the latest followup were 2 cases of grade A, 7 cases of grade B, 17 cases of grade C, 7 cases of grade D. In 17 patients with significantly waist and back pain, the score of 14 cases were decreased from 10 points to 2 points, 2 cases were improved from 10 points to 2 points, and 1 case were improved to 4 points via operation. The perioperative complications included cerebrospinal fluid leakage in 1 cases, wound poor healing in 2 cases, and no neurological complications.
Discussion
For patients with late kyphosis deformity, the surgical indication includes nerve injury, spinal instability, local pain, kyphosis. The purpose of surgical treatment is that 1. relieve spinal cord compression; 2. restoring the spinal physiological curvature; 3. maintain the stability of the spine. For the posterior total vertebral osteotomy, the same degree of correction and simple shortening osteotomy indicate more shortening of middle column. It is demonstrated that the posterior osteotomy could be limited to 30°-40°, otherwise over shortening, distort and accumulate of spinal cord would be resulted [2,3]. Chen et al [1] found that if kyphosis Cobb angel was more than 45°, the spinal cord would appear obvious shortening and accumulation. Reconstruction with appropriate height was made on the anterior column of the osteotomy plane, the same degree correction could achieve smaller posterior column resection and reduce the spinal cord shortening compared with posterior total vertebral osteotomy, which would prevent the spinal cord injury caused by spinal cord shortening. In our study, all patients received reconstruction with bone graft block or titanium cage on anterior and middle columns, which properly restored and maintenance the height of the anterior and middle columns. The height of anterior marginal of the patients was 0.8575 ± 0.742 cm, 2.675 ± 1.615 cm pre and post-operation respectively (P<0.05). The height of the posterior marginal was 2.878 ± 1.701 cm, 2.805 ± 1.576 cm pre and post-operation respectively (P>0.05).
In this study, in the course of surgical correction of the deformity, bone graft block or titanium cage has played the role of leverage fulcrum to make the kyphosis correction more easy. Meanwhile, in the course of the posterior screw rod pressure correction, the degree of the spinal cord shortening was reduced, which effectively prevents the occurrence of complications of nerve injury. There were no symptoms of nerve injury or aggravation of symptoms in all cases. At the same time, in the reconstruction of anterior middle column of spine, the effective support by bone graft block or titanium cage could significantly reduce the load of the posterior screw rod fixation, which further reduced the occurrence rate of internal fixation fracture. The vertebral bone mass of the patients with late kyphosis deformity in the spinal segment which needs internal fixation was less due to long-term bedrest, activity decreased caused by spinal pain, spinal cord injury or other reasons, therefore, the holding capability on pedicle screw was less than normal.
The reconstruction and support of the anterior middle column reduced the risk of pull out of the pedicle screw. There were no internal fixation failure in the follow-up of the patients in this study.
The application of the posterior pedicle screw fixation plus anterior middle column mass bone and titanium cage filled with bone fragments provided good stability of diseased vertebra and upper vertebra immediately after operation. Moreover, it also provided good condition for diseased vertebra and upper vertebra in forward, which laid a solid foundation for a permanent solution to the kyphosis and the risk of internal fixation failure. It is reported that [4] the sagittal Cobb angle of combined anterior-posterior operation was 10.5°-22.2° (average 17.5°) pre-operation, -5°-12° (average 3.4°) immediately after operation, and 3.3°-18.5° (average 9.3°) at the last follow up. 5.9° was missed at the last follow up compared with the degree immediately after operation and the total kyphosis correction was 8.2°. In this study, the average Cobb angle pre-operation was 52°. The average follow-up was 17 months, and the post-operation average Cobb angle at the last follow up was 15°.
The average correction rate was 71.1%. The correction rate was not significantly decreased (2°decreased) compared with the degree immediately after operation (average kyphosis Cobb angle was 13°). The total degree of correction was 37°, which showed that the effect of this operation in the correction of deformity and the maintenance of stability are satisfactory. Therefore, the one stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly was superior compared with anterior posterior combined operation.
In conclusion, the treatment of one stage posterior approach osteotomy with screw rod fixation and cage inserting anteriorly on late thoracolumbar kyphosis deformity obtain satisfactory results on the deformity correction, integration, maintenance, decompression and trauma reduction.
Acknowledgements
None.
Conflicts of interest
None.
References
- Chen ZQ, Li WS, Guo ZQ, Qi Q, Dang GT. Surgical treatment on Post-traumatic Kyphosis of Thoracolumbar Spine. Chinese Journal of surgery 2005; 43: 201-204.
- Deng Q, Zhang Y, Sheng W. Stage I posterior osteotomy and instrumentation and stage II anterior debridement and bone grafting for lumbar spinal tuberculosis with severe kyphosis. Int J ClinExp Med 2015; 8: 20890-20896.
- Li X, Zhang J, Tang H, Lu Z, Chen S, Hong Y. Closing-opening wedge osteotomy for thoracolumbar traumatic kyphosis Eur J Med Res 2014; 19: 59.
- Verlaan JJ, Diekerhof CH, Buskens E, van der Tweel I, Verbout AJ, Dhert WJ, Oner FC. Surgical treatment of traumatic fractures of the thoracic and lumbar spine: a systematic review of the literature On techniques, complications, and outcome. Spine (Phila Pa 1976) 2004; 29: 803-814.