Research Article - Current Pediatric Research (2022) Volume 26, Issue 1
Anorectal biofeedback influence on encopresis resulting from sexual assault in school aged girls: A randomized controlled trial.
Hend Reda Sakr1*, Hanaa Mohsen Abd-Elfattah2, Mona Mohamed Abdelkhalek3, Mahmoud Ibrahim Elsayed Aly4, Mahmoud Kamal Mohamed Mousa5
1Department of Physical Therapy for Woman's Health, Badr University Cairo, Cairo, Egypt
2Department of Physical Therapy for Pediatrics and Pediatric Surgery, Badr University Cairo, Cairo, Egypt
3Department of Physical Therapy for Internal and Geriatric, Badr University Cairo, Cairo, Egypt
4Department of Basic Science, Badr University Cairo, Cairo, Egypt
5A Forensic Specialist at the Forensic Medicine Authority of the Egyptian Ministry of Justice, Cairo, Egypt
- Corresponding Author:
- Hend Reda Sakr
Department of Physical Therapy for Woman's Health, Badr University Cairo, Cairo, Egypt
E-mail: Hendsakr1986@gmail.com
Received: 06-Jan-2022, Manuscript No. AAJCP-22-51299; Editor assigned: 07-Jan-2022, PreQC No. AAJCP-22-51299(PQ); Reviewed: 14-Jan-2022, QC No. AAJCP-22-51299; Revised: 22-Jan-2022, Manuscript No. AAJCP-22-51299 (R); Published: 31-Jan-2022, DOI:10.35841/0971-9032.26.1.1215-1219.
Abstract
Objective: To investigate the efficacy of biofeedback on encopresis in school aged girls after sexual assault. Methods: Thirty girls with fecal incontinence, their age was ranging between 5 to 11 years were enrolled in this study and randomly divided into two groups of equal numbers (control and experimental). Both groups received exercises for pelvic floor muscles (kegel exercises) and daily home program. The experimental group received additionally anorectal manomerty biofeedback training program. Treatment for all patients lasted for three months (1 hr/session, 4 times/week). Anorectal manometric functions were assessed for all girls before and after treatment. Results: There was significant improvement in both groups that confirmed by comparing the mean values of all measured variables pre and post interventional treatment (P<0.05). There were significant differences between the control and experimental groups regarding all measured variables when comparing outcomes after interventional treatment (P<0.05). Conclusion: Anorectal biofeedback can be a successful interventional treatment that may remedy encopresis in school aged girls after sexual assault.
Keywords
Encopresis, Anorectal manometry, Kegel exercises, Sexual assault, Daily home program.
Introduction
Any threatening-life history might precede the incidence of bowel disorders. So, during assessment of females with gastrointestinal disturbances, it’s very common to find a history of sexual abuse [1]. Sexual abuse or sexual assault is any action characterized by sexual impression that is done by the abuser person on purpose against the desire of the victim and it starts from touching till reaching mouth, vaginal or anal penetration. The type of sexual abuse that can impact external anal sphincter can be produced by vigorous anal penetration either by an erected penis, suppository, enema, or thermometer [1,2].
Encopresis or fecal incontinence is defined as repeated involuntary transition of faeces to inappropriate locations" after mental age of 4 years old with no pathological cause resulting in leakage of soft liquid stool around stool mass in the rectum [3]. Fecal incontinence is caused by inappropriate functioning of sphincter muscles of the anus resulting from their damage. This damage can cause defect in sensory perception from the anal canal itself leading to weakness of these sphincteric muscles and the most common cause of this weakness is the trauma of the perineum [4].
Biofeedback treatment is one of the visual and sensory feedback techniques that indexed as a useful method in treating fecal incontinence through restoring normal pattern of bowel action. This is obtained by improving strength, coordination and isolation of levator ani muscle, improving the capability of the rectum to sense lower volumes of distensions and the capability of tolerating higher rectal distensions without non-controllable sensation of urgency [5,6].
On the other hand, Kegel exercises have an influence towards strengthening external anal sphincter and puborectalis muscle. They are efficient for prevention and cure of pelvic floor dysfunctions in females and this efficacy relies on the patient capability of voluntary contraction of the pelvic floor muscles on regular basis [6,7]. Also, they are very successful to perform them at home in order to strength muscles that support vagina, urethra and rectum [8].
Most studies were conducted to find the biofeedback effect on weakness of external anal sphincter in children suffering from fecal incontinence of neurogenic origin, while the traumatic cause especially the sexual abuse was neglected. So, the purpose of the current study was intended to find out biofeedback’s effect on external anal sphincter strength after sexual abuse in school aged girls.
Methods
Study design
A randomized, single-blind, controlled clinical trial was referred from forensic medicine authority of Egyptian ministry of justice and run the experiment in faculty of physical therapy outpatient clinic, Badr University in Cairo.
Participants
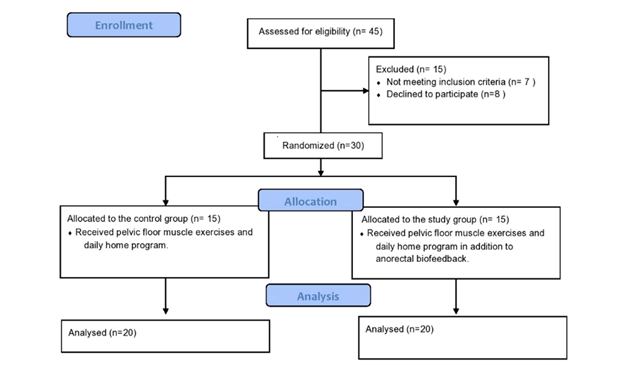
Thirty school-aged girls ranged from 5-11 years and all diagnosed with encopresis resulting from anal sexual abuse [9]. Seven girls did not fulfill the requirements for inclusion and eight girls' parents declined to participate in this study. Following the base line measurement, the girls were allocated randomly into two groups equal in number. We assumed that no confounding factor would have any effect. So, simple randomization technique was used. Girls were sequentially allotted a number from 1 to 30. At that point, online graph pad software used to randomly allocate 15 girls to each group. A flow chart depicts the experimental design in Figure 1.
Forty-five girls with encopresis were recruited for this study. The following factors were used to determine whether or not a girl was eligible to study: between the ages of 5 and 11 years, they have absent anal reflex, skin trifles around the anus, have funnel shaped anus, medically stable and were mature enough to comply with biofeedback. Girls whom have sexual transmitted disease or any medical condition that affect the anus potentially such as Crohn’s disease, severe chronic constipation, anorectal structural defects, anorectal surgical interference, Hirschsprung’s disease, myotonic dystrophy, metabolic and connective tissue disorders, and were excluded from study. The purpose, process and benefit were thoroughly clarified to parents of the included girls prior to data collection. In order to have their children involved in the study, parents were given written consent forms. Our study was carried out in compliance with the declaration of Helsinki criteria for human studies. The study was accepted by ethical review committee of the faculty of physical therapy, Cairo University. P.T.REC/012/002915.
Outcome measures
At baseline, all procedures were conducted before treatment and after three consecutive months of treatment in a warm and quiet space. All girls were evaluated clinically through history taking in details, rectal palpation, and general assessment of posture including mobility of spines, diaphragm, and positions of hips, knees, and feet. The examination includes voluntary and involuntary contractions that occur during increased intra-abdominal pressure [4].
Anorectal manometry was performed by using solar GI-HRAM device fabricated by medical measurements simple. Enschede, Netherlands was applied on all subjects. A water inflated, reusable HRM catheter with a channel of 20+1 pressure and inflating balloon free of latex connected to the distal portion (fabricated by mui scientific, Ontario, Canada).
This device measures the resting anal pressure (mmHg), squeeze anal pressure (mmHg), first sensation (ml) and maximum tolerable volume (ml). Anorectal manometry was applied at the primary evaluation to measure these parameters and was repeated after 3 months of treatment detecting the changes that were achieved.
Intervention
All participants received the same pelvic floor muscle exercise (Kegel exercise). At first, girls performed maximum pelvic floor muscle contractions (3 sets/8-10 repetitions) to hold contraction greater than 3 seconds. The exercise was progressed by increasing the hold period reaching 10 to 12 seconds, adding 3 fast contractions at the end of the contraction until they reach (10 sets/10 repetitions) starting from supine lying (to avoid substitution of hip adductor muscles, the patient's knees were manually supported) then sitting then standing then standing with legs apart till reach walking and jumping [7]. The program was applied for 30 minutes with 1-minute relaxation between the exercise sets, 4 days per week for 3 months.
The experimental group followed additionally anorectal biofeedback training with these procedures: The girl was positioned in lateral left position with flexion of hips and knees at 90 degrees, and then the probe was inserted rectally after lubrication with KY gel. A balloon made of rubber with dimensions 2.5 cm × 6 cm that can distend to 200 ml was connected to the probe. The distances to the base of the balloon were 5.5 cm and 4 cm from the distal and nearest side holes, respectively. By the station pull through method, sphincter recognition was achieved.
The catheter was gradually removed in 0.5 cm increments until the distal channel could record resting external anal sphincter pressure. The base of the balloon was located between 5.5 cm and 7 cm from the anus [10]. After insertion of the lubricated probe, the patient should be given 5 minutes’ relaxation prior to starting the session. Anal resting pressure was measured for 20 seconds. Participant girl was instructed to contract the anus as much as she could, to measure the squeeze anal pressure for a period of 30 seconds, and then she was given a rest for 1 minute. After that rectal sensations were measured. First, the balloon was blown up with 10 ml of water and held for at least 30 seconds before gas or fullness was felt by the patient, this is the (first sensation).
The balloon was then blown up with 400 ml of water (maximum volume) and the patient was instructed to measure the painful need to defecate (max tolerable volume). Every session, the patient was trained on lower volumes than those achieved in the previous session and is encouraged to achieve more anal squeeze pressure. Girls were taught to contract in different manners like maximum voluntary sustained contraction of sphincter, submaximal sustained contraction, fast twitch and quick flick contractions [11]. Each session takes approximately 30 minutes in addition to Kegel exercises.
Both groups followed daily home program that included diet control and pelvic floor exercise; the diet control was achieved at home by giving the patients diet rich in fibers to increase stool bulk like vegetable, fruits and whole grains. The dose for participating girls was two large tablespoons, two times daily [12] while the pelvic floor exercises were performed 20 repetitions of the mentioned exercise in home daily: maximum contraction and hold to reach 10 seconds (slow contraction) and maximal contraction with relaxation (quick flick fast contraction) [13].
Analysis of data
T-test was utilized to analyze subject characteristics between groups. The Shapiro-Wilk test was used to check the normal distribution of data, and Levene’s test for homogeneity was conducted to test the homogeneity between groups. An effect of anorectal manometry inside and between groups was tested by mixed MANOVA. Multiple post-hoc tests were utilized using Bonferroni correction. A p<0.05 was the level of significance. SPSS (IBM SPSS, Chicago, IL, United States of America) version 25 was utilized for all tests of statistics.
Results
Subject characteristics
There was no significant difference between both groups within the subject characteristics (p>0.05) Table 1.
| Control group | Experimental group | P-value | |
|---|---|---|---|
| Mean ± SD | Mean ± SD | ||
| Age (years) | 9.63 ± 1.74 | 9.88 ± 1.44 | 0.67a |
| Weight (kg) | 26.06 ± 2.01 | 27.10 ± 2.83 | 0.26a |
| Height (cm) | 125.30 ± 6.67 | 126.70 ± 6.83 | 0.57a |
Table 1. Basic characteristics of participants. SD: Standard Deviation; P-value: Level of significance; a : t-test.
Impact of treatment on anorectal manometry biofeedback: There was a significant interaction between treatment and time (Wilks’ Lambda=0.04; F=131.10, p=0.001, =0.95). There was a significant main effect of time (Wilks’ Lambda=0.00; F=2693.94, p=0.001, =0.99). There was a significant main effect of treatment (Wilks’ Lambda=0.12; F=42.43, p=0.001, =0.87).
Comparison within group: After treatment, there were significant improvements in the anorectal biofeedback parameters in both groups compared to the pretreatment results. There was a significant improvement in the parameters of anal resting, anal squeeze pressure, first rectal sensation and maximum tolerable rectal volume in control and experimental groups post treatment in comparison with that pretreatment (p<0.001)
Comparison between groups: There wasn’t significant difference between groups regarding all parameters before treatment (p>0.05). While after treatment, there was a significant decrease in findings of first rectal sensation and maximum tolerable rectal volume of the experimental group compared with the control (p<0.001); and a significant increase in the findings related to anal resting, anal squeeze pressure of experimental group compared with control group (p<0.001) (Table 2).
| Pre-treatment | Pa value | Post-treatment | Pa value | Pre vs. Post | ||||
|---|---|---|---|---|---|---|---|---|
| Control group | Experimental group | Control group | Experimental group | Control group | Experimental group | |||
| Mean ± SD | Mean ± SD | Mean ± SD | Mean ± SD | Pb value | Pb value | |||
| Anal resting pressure (mm Hg) | 18.20 ± 3.25 | 18.73 ± 2.31 | 0.61 | 29.80 ± 2.80 | 43.20 ± 5.15 | 0.001 | 0.001 | 0.001 |
| Anal squeeze pressure (mm Hg) | 61.93 ± 3.41 | 61.33 ± 3.24 | 0.62 | 81.60 ± 5.13 | 84.93 ± 2.81 | 0.036 | 0.001 | 0.001 |
| First rectal sensation (ml) | 11.00 ± 0.84 | 10.86 ± 0.83 | 0.66 | 8.60 ± 0.91 | 7.20 ± 0.77 | 0.001 | 0.001 | 0.001 |
| Maximal tolerable rectal volume(ml) | 77.06 ± 1.86 | 76.81 ± 1.90 | 0.92 | 63.86 ± 2.53 | 53.93 ± 1.28 | 0.001 | 0.001 | 0.001 |
Table 2. Comparison of anorectal manometry findings pre and post treatment. SD: Standard Deviation; P-value: Level of significance; a: Between group comparison, b: Within group comparison.
Discussion
The current study was conducted to find out the impact of anorectal manometry biofeedback on weakness of external anal sphincter after sexual trauma in school aged girls. Encopresis is a common condition that found in pediatric GIT setting that needs a combination of family education, pharmacological medications, a special balanced diet, and behavioral management to treat it successfully [14]. Children with encopresis/fecal incontinence have restrictions in their daily living that have a negative impact on their quality of life socially, suffering from fear, embarrassment of unexpected defecation and bad odor. This can affect their hygiene leading to anxiety, depression and poor self-confidence [15].
Weakness of external anal sphincter is the main cause of encopresis which can be resulted from many factors including sphincter damage plus weakness of puborectalis muscle. A previous study found that this weakness leads to decrease in the inward traction exerted by the puborectalis in patients with encopresis and is improved by biofeedback therapy [15,16]. The results of the experimental group showed at post-treatment period a significant improvement in the maximum squeeze pressure which agrees a previous study conducted by Munasinghe et al. who found that biofeedback improves maximum squeeze pressure in patients with fecal incontinence that accompanied by external anal sphincter damage, affecting quality of their lives [17]. In addition to the findings of a study conducted by Norton and Cody who found that biofeedback and pelvic floor exercises that strengthen external anal sphincter have a potent effect rather than exercises alone [18].
Biofeedback in our study shows significant improvement of the anorectal manometry outcomes which include first rectal sensation and maximal tolerable sensation as well as resting anal pressure and maximal squeeze pressure. The current results came in line with the results of a previous study conducted by Vaghar et al. who proved that biofeedback improved these outcomes suggesting that biofeedback therapy can be considered as a successful treatment for functional defecation disorders such as encopresis [19]. The significant improvement in the sensation outcomes including first rectal sensation and maximum tolerable volume may be attributed to increasing the contractility of external anal sphincter responding to rectal distension. Girls were trained to detect and react to weak rectal distension or to contract quickly responding to this distention of the rectum [20]. This interpretation agrees and illustrates the significant improvement in the sensory rectal outcomes of our study and was confirmed by a previous study conducted by Chiarioni et al. which proved that first rectal sensation thresholds and urge together were strong predictors responding to biofeedback treatment and sensory retraining suggesting that, the effectiveness of biofeedback could be more important than strength training [21].
Regarding effect of pelvic floor muscle exercise accompanied by biofeedback in managing encopresis; a previous research was conducted in 2019 for managing encopresis using pelvic floor muscle exercise and biofeedback above four months, every session lasted for 45 minutes and the results were that participants in the pelvic floor rehabilitation group had 5-fold higher likelihood of documenting symptom changes and a greater mean reduction in incontinence severity which supports results of our study [22] .
On the other hand, Ladi-Seyedian et al. conducted a comparative study between traditional biofeedback versus pelvic floor rehabilitation that managed pelvic floor disorders as fecal incontinence in all ages and stated that biofeedback alone, without pelvic floor exercises, is not an effective treatment which contradicts the results of our study.
A recent study review on biofeedback in addition to pelvic floor training for fecal incontinence found that there is no reason to judge from previous trials if these techniques are helpful or not and which component of these treatments are effective in managing such cases, which disagree with the results of the current study.
Limitation of this research includes a comparatively small sample size, and this was due to the restrictions of our Eastern Arabic society and their culture. The Egyptian society still blaming the females on the sexual abuse and put the total commitment and responsibility on her, so obtaining a large sample size and persuading the parents to treat their daughters physically and psychologically were very difficult although they were referred from forensic medicine authority of Egyptian ministry of justice.
Conclusion
It was concluded from the obtained results that, anorectal manometry bio feedback can be an effective, tolerable, and safe physical therapy modality to manage encopresis that resulted from anal sexual abuse in school aged girls.
Acknowledgements
The authors are grateful for all the children and their parents' cooperation and involvement in the current research.
Conflict of interest
Authors state no conflict of interest in the current research.
Funding
The current research did not receive special grants from any public, commercial, or non-profit funding organization.
Author contributions
Conceptualization: Reda HS, Abd-Elfattah HM, Abdelkhalek MM, Aly MI. Methodology: Reda HS, Abd-Elfattah HM. Formal analysis: Abd-Elfattah HM. Writing–original draft: Reda HS. Diagnosis: Kamal MM, Abdelkhalek MM, Aly MI. Referral: Kamal MM. Approval of final manuscript: All authors.
References
- Leroi AM, Berkelmans I, Denis P, et al. Anismus as a marker of sexual abuse. Dig Dis Sci 1995; 40(7): 1411-6. [Crossref][Google Scholar][Indexed]
- Leroi AM, Bernier C, Watier A, et al. Prevalence of sexual abuse among patients with functional disorders of the lower gastrointestinal tract. Int J Colorect Dis 1995; 10(4): 200-6. [Crossref][Google Scholar][Indexed]
- Colombo JM, Wassom MC, Rosen JM. Constipation and encopresis in childhood. Pediatr Rev 2015; 36(9): 392-401. [Crossref][Google Scholar][Indexed]
- Mazur-Bialy AI, Ko?oma?ska-Bogucka D, Op?awski M, et al. Physiotherapy for prevention and treatment of fecal incontinence in women systematic review of methods. J Clin Med 2020; 9(10): 3255. [Crossref][Google Scholar][Indexed]
- Jelovsek JE, Markland AD, Whitehead WE, et al. Controlling faecal incontinence in women by performing anal exercises with biofeedback or loperamide: A randomised clinical trial. J Gastroenterol Hepatol 2019; 4(9): 698-710. [Crossref][Google Scholar][Indexed]
- Rao SS, Benninga MA, Bharucha AE, et al. ANMS?ESNM position paper and consensus guidelines on biofeedback therapy for anorectal disorders. Neurogastroenterol Motil 2015; 27(5): 594-609. [Crossref][Google Scholar][Indexed]
- Johannessen HH, Wibe A, Stordahl A, et al. Do pelvic floor muscle exercises reduce postpartum anal incontinence? A randomised controlled trial. BJOG: Int J Gynaecol Obstet 2017; 124(4): 686-94. [Crossref][Google Scholar][Indexed]
- Xie M, Zhang X, Zhang X, et al. Can we evaluate the levator ani after Kegel exercise in women with pelvic organ prolapse by transperineal elastography? A preliminary study. J Med Ultra 2018; 45(3): 437-41. [Crossref][Google Scholar][Indexed]
- Iwai N, Iwata G, Kimura O, et al. Is a new biofeedback therapy effective for fecal incontinence in patients who have anorectal malformations? J Pediatr Surg 1997 ; 32(11): 1626-9. [Crossref][Google Scholar][Indexed]
- Nolan T, Catto-Smith T, Coffey C, et al. Randomised controlled trial of biofeedback training in persistent encopresis with anismus. Arch Dis Child 1998; 79(2): 131-5. [Crossref][Google Scholar][Indexed]
- Scott KM. Pelvic floor rehabilitation in the treatment of fecal incontinence. Clin Colon Rectal Sur 2014; 27(03): 99-105. [Crossref][Google Scholar][Indexed]
- Cinara Sacomori PT, Bary Berghmans PT, Rob de Bie PT. Predictors for adherence to a home-based pelvic floor muscle exercise program for treating female urinary incontinence in Brazil. Physiother Theory Pract 2018; 4: 26-30. [Crossref][Google Scholar][Indexed]
- Philichi L. When the going gets tough: Pediatric constipation and encopresis. Gastroenterol Nurs 2008; 31(2): 121-30. [Crossref][Google Scholar][Indexed]
- Rao SS, Bharucha AE, Chiarioni G, et al. Anorectal disorders. Gastroenterol 2016; 150(6): 1430-42. [Crossref][Google Scholar][Indexed]
- Fernández–Fraga X, Azpiroz F, Malagelada JR. Significance of pelvic floor muscles in anal incontinence. Gastroenterol 2002; 123(5): 1441-50. [Crossref][Google Scholar][Indexed]
- Norton C, Cody JD. Biofeedback and/or sphincter exercises for the treatment of faecal incontinence in adults. Cochrane Database Syst Rev 2012; 11(7): CD002111. [Crossref][Google Scholar][Indexed]
- Vaghar MI. An investigation into the effect of biofeedback on urinary and fecal incontinence in patients with anal sphincter dysfunction. J Family Med Prim Care 2019; 8(7): 2264. [Crossref][Google Scholar][Indexed]
- Miner PB, Donnelly TC, Read NW. Investigation of mode of action of biofeedback in treatment of fecal incontinence. Dig Dis Sci 1990; 35(10): 1291-8. [Crossref][Google Scholar][Indexed]
- Chiarioni G, Bassotti G, Stegagnini S, et al. Sensory retraining is key to biofeedback therapy for formed stool fecal incontinence. Am J Gastroenterol 2002; 97(1): 109-17. [Crossref][Google Scholar][Indexed]
- Ussing A, Dahn I, Due U, et al. Efficacy of supervised pelvic floor muscle training and biofeedback vs. attention-control treatment in adults with fecal incontinence. Clin Gastroenterol Hepatol 2019; 17(11): 2253-61. [Crossref][Google Scholar][Indexed]
- Ladi-Seyedian SS, Sharifi-Rad L, Nabavizadeh B, et al. Traditional biofeedback vs. pelvic floor physical therapy-is one clearly superior? Curr Urol Rep 2019; 20(7): 1-9. [Crossref][Google Scholar][Indexed]
- Norton C, Kamm MA. Anal sphincter biofeedback and pelvic floor exercises for faecal incontinence in adults: A systematic review. Aliment Pharmacol Ther 2001; 15(8): 1147-54. [Crossref][Google Scholar][Indexed]