- Biomedical Research (2012) Volume 23, Issue 4
An animal study on the effect of different classes of organic calcium channel blockers in wound healing
Naman Hirenkumar Shah, Aniket Kumar, N. Kaysina Vazhudhi, A. Blessed Winston, Kalpana Ernest, Margaret Shanthi FX*.Christian Medical College and Hospitals, Bagayam, Vellore 2, Tamil Nadu, India.
- *Corresponding Author:
- Margaret Shanthi FX
Department of Pharmacology and Clinical Pharmacology,
Christian Medical College and Hospitals
Vellore 632 002, TamilNadu
India.
Accepted date: July 25 2012
Abstract
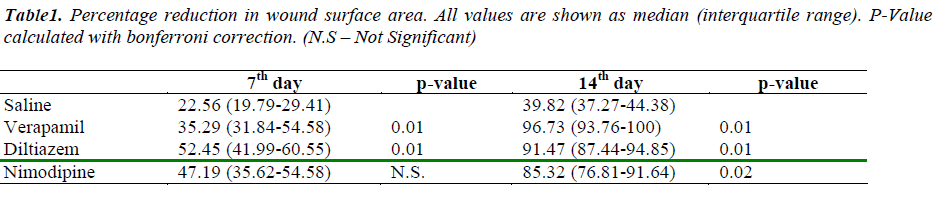
An animal study of the effect of different classes of organic calcium channel blockers in wound healing. Calcium channel blockers (CCB) have been shown experimentally to modulate cellular proliferation, maturation of keratinocytes and fibroblasts. We conducted this study to determine the effect of calcium channel blockers on an excision wound model. A total of 24 Wistar male rats were divided into four groups each of which were treated with one of the following drugs: verapamil, diltiazem nimodipine or normal saline after excision wound. Primary outcome was percentage reduction of the wound at 7th and 14th post-operative days. Compared to normal saline, CCB caused a highly significant percentage reduction of wound area on days 7 and 14. CCB enhanced the wound healing process compared to normal saline. The median percentage reduction of wound surface area at 7th day in the saline group with interquartile range was 22.56 (19.79-29.41) and that for the verapamil group 35.29 (31.84-54.58), diltiazem 52.45 (41.99-60.55) and nimodipine 47.19 (35.62-54.58) was statistically significant (p<.05) whereas on 14th day for saline it was 39.82 (37.27-44.38) and that for verapamil was 96.73 (93.76-100), diltiazem 91.47 (87.44-94.85) and nimodipine 85.32 (76.81-91.64). Day 14 showed better results when compared to day 7 with a higher level of significance. Topical CCB may be capable of promoting wound-healing activity. Hence, topical CCB may be a suitable alternative to saline in the treatment of wound healing
Keywords
Calcium channel blockers, Wound healing, Verapamil, Nimodipine, Diltiazem.
Introduction
Normal wound healing is a dynamic process characterized by organized inter-linked sequences of cellular and molecular events. These events include hemostasis by clot formation; inflammation; chemotaxis and adhesion of fibroblast, keratinocytes; angiogenesis by migrating endothelial cells; and collagen deposition and wound contraction [1].
Calcium plays an important role during the normal healing process. Patients with renal failure who have deranged calcium levels suffer from impaired and delayed wound healing [2]. In a study by Sank et al. [3] calcium dosedependently inhibited keratinocyte chemotaxis and adhesion. This effect of calcium was reversed by verapamil, an organic calcium channel blocker. In animal experiments, calcium impaired the wound contraction which was reversed by verapamil. Depletion of extracellular calcium as well as inorganic calcium channel blockers like Ni2+, Gd3+ block galavanotaxis of human keratinocyte but verapamil has shown to have no effect on it. Cellular calcium metabolism was also shown to regulate extracellular matrix production [4]. Verapamil, nifedipine and diltiazem may also inhibit FGF-induced fibroblastic and PDGF stimulated smooth muscle cell proliferation [5, 6]. Diltiazem and verapamil also inhibit matrix metalloproteinase (MMP) expression and collagenolytic activity in SMC but verapamil was shown to increase MMP activity in skin fibroblasts [6,7]. Verapamil also did not show any effect on production of VEFF and IL-6 by nonkeloid fibroblasts [8]. Verapamil, nimodipine and diltiazem have been utilized for the prevention and treatment of skin-flap necrosis in experimental animals by topical and systemic administration because of their vasodilatory action [9,10]. Almost all the studies mentioned above have used the doses in the range of 10 micromoles to 5 milimoles. Apart from being a L-type calcium channel blocker, verapamil is also an inhibitor of HERG K+ channels, neuronal and cardiac delayed rectifier K+ channels, KATPM, IKCa1, Kv1.3 but with higher IC-50 values. Diltiazem also inhibits HERG channels in cardiac myocytes.
Till date no study has been done to compare different organic calcium channel blockers (dose in range to inhibit only L-type of Ca2+ channels) with saline in an animal excision wound model. So, we decided to conduct the present study with the objective to compare (i) percentage reduction in wound surface area at day 7th and day 14th and (ii) median day of healing with three organic calcium channel blockers, namely verapamil, diltiazem and nimodipine with that of saline.
Materials and Methods
Animals: A total of 24 healthy Wistar rats of either sex, 12 weeks age and weighing 150–200 grams were procured from the Animal House of the institute. They were housed under controlled conditions of temperature of 23 ± 2°C, humidity of 50 ± 5% and 12 hours of light and dark cycle. Animals were kept individually in polypropylene cages containing sterile paddy husk as bedding throughout the experiment and had free access to food (rat chow) and water. There was no infection of the experimental wound in any animal. This animal study was approved by institutional Animal Ethics Committee. The study was done as per the guidelines set by CPCSEA, India.
Wound Model and Assessment
After two weeks of adaptation period, each animal was anesthetized with intraperitoneal ketamine 100 mg/kg followed by the creation of ~400 mm2 full thickness wound on a pre-determined area on the depilated back of the rat with excision wound method described earlier [11]. Immediately after wounding, photographs were taken by a fixed camera (Nikon Coolpix®). Wound boundaries for each wound were traced onto a transparency sheet every alternate day. After achieving hemostasis, the wound was covered with an occlusive dressing either soaked with drug or saline. This procedure was performed daily starting from day 0 (the day of wounding) and continued till complete healing of wound.
According to Wound Healing Society’s criteria, complete healing was defined as 100% re-epithelialization of the wound and no drainage from wound.
Treatment schedule
The animals were divided into 4 groups with 6 animals in each group to receive daily treatment with 0.5 mL of one of the following drugs: normal saline, 1 μM verapamil, 1 μM diltiazem, or 1μM nimodipine solution. Electrocardiogram was taken before and 1 hour after first application of drug to see any changes in heart rate due to systemic absorption of drug. The doses of drugs were chosen on the basis of the drugs’ inhibitory concentration 50 (IC50) values for L-type calcium channels.
Statistical Analysis
Percentage reduction in the wound surface area was calculated from the original wound size for 7th and 14th day. Kruskal-Wallis test with significance value of < 0.05 was used to assess the difference between groups. Multiple comparisons between the groups were done by Bonferroni’s post-hoc test for multiple comparisons. Analysis was done by R: A Language and Environment for Statistical Computing (version 2.12.2) [12].
Results
Descriptive statistics for all groups is given in Table 1. There was no trend toward decreased rate of wound healing with larger wound size
Percentage reduction in wound surface area
At day 7: There was a statistically significant difference between all groups as detected by Kruskal-Wallis method. In post-hoc comparisons, wound healing was significantly better in all three calcium channel blockers compare to saline. Although there was no significant difference evident between all three calcium channel blocker groups, diltiazem group had a higher percentage reduction in wound area. Effect size was calculated with multiple comparisons.
At day 14: Difference between saline and other three calcium channel blocker groups was increased at day 14. Effect of verapamil was apparently better at day 14. Percentage reduction in wound area in verapamil group was significantly higher compared to nimodipine group but no such difference was found in comparison between both verapamil and diltiazem groups or between diltiazem and nimodipine groups.
Effect on weight
Periodic estimation of weight was done as part of the study. There was a trend of marginal weight loss during first two days after creation of wound which was not significant. Similarly no significant difference in weight of animal was evident between all groups at either day 7 or day 14.
Effect on heart rate
As the doses of calcium channel blockers used in this study were very small compared to the usual doses, no significant effect of these drugs was found on heart rate because of their inappropriate systemic absorption. Electrocardiogram taken 1 hour after application of the drug did not show any decrease in heart rate in the study animals.
Discussion
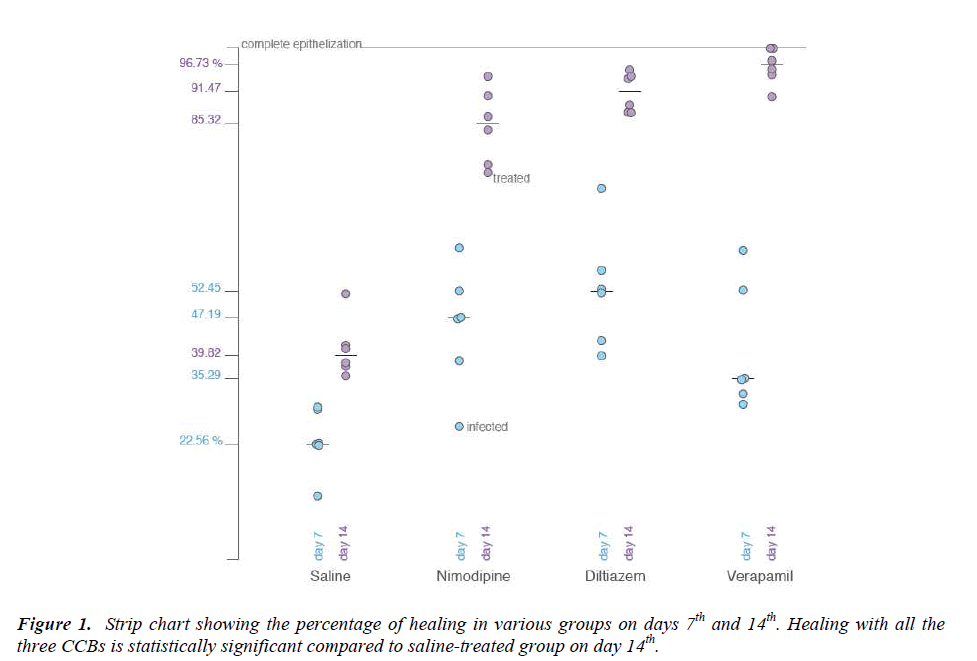
The present study has shown that organic calcium channel blocker have a better wound healing property compared to saline both at day 7 and day 14. There was no difference in wound healing process between the calcium channel blockers at seventh day. At day 14, verapamil was found to be significantly better than nimodipine. The results of the present study suggest that different classes of organic CCB enhance the wound healing process compared to normal saline. Organic CCB caused a highly significant percentage reduction of wound area compared with normal saline on days 7 and 14 (Table 1). The median of the percentage reduction of wound surface area at 7th day in the saline-treated group with interquartile range was 22.56 (19.79-29.41) and that for the verapamil group was 35.29 (31.84-54.58), diltiazem 52.45 (41.99-60.55) and nimodipine 47.19 (35.62-54.58) which was statistically significant (p < 0.05) whereas on 14th day for saline it was 39.82 (37.27-44.38) and that for verapamil was 96.73 (93.76-100), diltiazem 91.47 (87.44-94.85) and nimodipine 85.32 (76.81-91.64), respectively. Results of day 14 showed much improvement compared to day 7 with a higher level of significance (Figure 1).
Wound healing generally requires support at three levels. First is by improving general resistance and support mechanisms. Second is by stimulating the repair and regenerative mechanisms to prolong cell life, cell migration and cell binding and improving tensile strength or elasticity of the skin. Third is by therapeutic and nutritional activities including anti-inflammatory, antiseptic and antimicrobial actions, protein and collagen synthesis, and increased stability of bio-membranes. Antioxidants can interfere with the oxidation process by reacting with free radicals, chelating catalytic metals and also by acting as oxygen scavengers. Free radicals and other reactive oxygen species (ROS) are thought to play an important role in wound healing [13]. Verapamil has been shown to inhibit superoxide production by neutrophils and their adhesion, which can help hasten the anti-inflammatory stage. Some CCB (verapamil, diltiazem, and nicardipine) may possess analgesic properties that are useful in the treatment of post-herpetic neuralgia when administered alone or in combination with lidocaine by iontophoresis [14].
Intralesional verapamil injection for the treatment of wound healing based on experimental findings showed that CCB may significantly affect fibroblast function. CCB inhibit collagen gene expression and thereby collagen synthesis, increase matrix metalloprotease activity, inhibit transcription of tissue inhibitor of matrix metalloprotease, and thus affect cell proliferation, extracellular matrix protein synthesis and secretion, as well as collagen degradation [15].
Our study demonstrates that the three organic CCB when topically administered are capable of promoting woundhealing activity. The study also supports the role of calcium in regulating wound healing. CCB enhanced wound contraction rate. CCB are also known to cause vasodilatation, which increases blood supply to the wounded region and hence cause promotion of wound healing [4, 16].The present study suggests that CCB can be used to hasten the recovery of wounds clinically in patients. Economically also, use of CCB is beneficial since CCB are relatively cheap drugs. Many protocols have been formulated for their use pre-operatively and post-operatively before completion of scar maturation [4] will make CCB attractive candidates for use in the wound healing process. Further studies using different animal models, topical CCB preparations and different durations of treatment may be worthwhile.
In this study we have found that organic CCB significantly improved all clinical parameters of wound healing so far investigated. The improvement was observed after 7th day from the baseline till 14th post-operative day (< 0.05). Dressing of the wound area with all three CCB achieved overall better and faster healing rate compared to standard normal saline dressing of the wound area.
In conclusion, our study demonstrates that topical CCB may be capable of promoting wound-healing activity. Hence, topical CCB may be a suitable alternative to saline in the treatment of wound area. However, the use of CCB needs further evaluation in clinical settings before being recommended for the treatment of wound healing.
References
- Broughton G 2nd, Janis JE, Attinger CE. The basic science of wound healing. Plast Reconstr Surg 2006;117(7 Suppl): 12S-34S.
- Broughton G 2nd, Janis JE, Attinger CE. Wound healing: an overview. Plast Reconstr Surg 2006;117(7 Suppl):1e-S-32e-S.
- Sank A, Chi M, Shima T, Reich R, Martin GR. Increased calcium levels alter cellular and molecular events in wound healing. Surgery. 1989; 106:1141.
- Lee RC, Ping J. Calcium antagonists retard extracellular matrix production in connective tissue equivalent. J Surg Res 1990; 49: 463-466.
- UK PubMed Central (UKPMC). Cell-cycle arrest in G0/G1 phase of growth factor-induced endothelial cell proliferation by... - Abstract - UK PubMed Central [Internet]. 1997 Jan [cited 2011 Jul 28]; Available from: http://ukpmc.ac.uk/abstract/MED/9232324/reload=0
- Wada Y, Kato S, Okamoto K, Izumaru S, Aoyagi S, Morimatsu M. Diltiazem, a calcium antagonist, inhibits matrix metalloproteinase-1 (tissue collagenase) production and collagenolytic activity in human vascular smooth muscle cells. Int J Mol Med 2001; 8: 561-566.
- Boggio RF, Freitas VM, Cassiola FM, Urabayashi M, Machado-Santelli GM. Effect of a calcium-channel blocker (verapamil) on the morphology, cytoskeleton and collagenase activity of human skin fibroblasts. Burns. 2011; 37: 616-625.
- Giugliano G, Pasquali D, Notaro A, Brongo S, Nicoletti G, D’Andrea F, et al. Verapamil inhibits interleukin-6 and vascular endothelial growth factor production in primary cultures of keloid fibroblasts. Brit J Plast Surg 2003; 56: 804-809.
- Kawabata H, Knight KR, Coe SA, Angus JA, O’Brien BM. Experience with calcium antagonists nitrendipine, diltiazem, and verapamil and beta 2-agonist salbutamol in salvaging ischemic skin flaps in rabbits. Microsurgery. 1991; 12: 160-163.
- Stark GB, Dorer A, Jaeger K, Narayanan K. The influence of the calcium channel blocker nimodipine on flap survival. Ann Plast Surg 1989; 23: 306-309.
- Wong VW, Sorkin M, Glotzbach JP, Longaker MT, Gurtner GC. Surgical approaches to create murine models of human wound healing. J Biomed Biotechnol 2011; 2011: 969618.
- R Development Core Team. R: A Language and Environment for Statistical Computing [Internet]. R Foundation for Statistical Computing, Vienna, Austria. 2011. Available from: http://www.R-project.org Weinzweig N, Lukash F, Weinzweig J. Topical and systemic calcium channel blockers in the prevention and treatment of microvascular spasm in a rat epigastric island skin flap model, Ann Plast Surg 1999; 42: 320- 326.
- Lee RC, Doong H, Jellena AF. Response of burn scar to intralesional verapamil: Report of five cases. Arch. Surg 1994; 129: 107-111.
- Margaret Shanthi FX, Ernest K, Dhanraj P. Comparison of intralesional verapamil with intralesional triamcinolone in the treatment of hypertrophic scars and keloids. Indian J Dermatol Venereol Leprol 2008; 74: 343-348.
- Grzesiak JJ, Pierschbacher. Shifts in the concentrations of magnesium and calcium in early porcine and rat wound fluids activate the cell migratory response. J Clin Invest 1995; 95: 227-230.Huang S, Maher VM,
- McCormick J. Involvement of intermediary metabolites in the pathway of extracellular Ca2+-induced mitogenactivated protein kinase activation in human fibroblasts: Cell Signal 1999; 11: 263-274.