Research Article - Biomedical Research (2017) Volume 28, Issue 8
Ultrasonography and fluoroscopy guided implantable chest ports in pediatric oncology patients: single center experience
?smail Okan Y?ld?r?m* and Kaya Sarac
Department of Radiology, Inonu University School of Medicine, Malatya, Turkey
- *Corresponding Author:
- ?smail Okan Y?ld?r?m
Department of Radiology, Inonu University School of Medicine
Turgut Ozal Medical Center, Turkey
Accepted date: February 08, 2017
Abstract
Objective: To evaluate the long term outcomes of implantable chest ports in pediatric oncology patients.
Material and Methods: The study includes chest port insertion procedures performed in a total of 68 pediatric oncology patients (31 girls and 37 boys) at Department of Interventional Radiology between October 2014 and October 2016. Mean age of the patients was 6.28 years (range 6 months-16 years). All procedures were performed under ultrasonography and fluoroscopy guidance. All data were analyzed restrospectively.
Results: Technical success of all procedures was 100%. Duration of use is mean 199 days for chest port catheter (range 1-302 day). Perioperative complications developed in 4 patients (n=2 jugular vein and port pocket site hemorrhage, n=2 catheter malposition) and long-term complications developed in 9 (n=2 catheter malposition, n=1 insertion site infection, n=3 catheter-related blood stream infection, n=3 skin dehiscense). Premature catheter removal occurred in 8 patients.
Conclusion: Insertion of ultrasonography and fluoroscopy-guided implantable port devices results in high technical success and low complication rates. This condition suggests that interventional radiologists would come in the foreground in this field.
Keywords
Implantable port devices, Interventional radiology.
Introduction
Chemotherapy agents may be harmful and toxic for peripheral vessels in children with oncologic diseases who need long term medical treatment. However increased number of punctures may lead to pain and anxiety in pediatric patients. Therefore implantable chest port device which is a safe method that could tolerate the effects of chemotherapy agents has become an integral part of venous access [1]. Chest port insertion may lead to perioperative, technical problems like pneumothorax, hemorrhage or long term effects like infection (exit site, tunnel, pocket site, blood stream infection), catheter dysfunction, mechanic problems (catheter fracture or catheter displacement, catheter thrombosis) [2,3]. In this study, we aimed to present our experience about implantable chest port insertion performed at Department of Interventional Radiology in pediatric cancer patients.
Materials and Methods
Patients
This study includes chest port procedures performed in 68 pediatric hematology-oncology patients at Department of Interventional Radiology between October 2014-August 2016. This retrospective study was approved by the institutional Review Board of our institution. A written informed consent was obtained from each patient.
Of the patients, 31 were girls and 37 were boys, mean age was 6.28 years (range 6 months-16 years). 39 patients had acute lymphoblastic leukemia, 15 patients had acute myeloblastic leukemia, 5 patients had lymphoma, 5 patients had Wilm’s tumor, and 4 patients had hemophagocytic lymphohistiocytosis.
Procedure
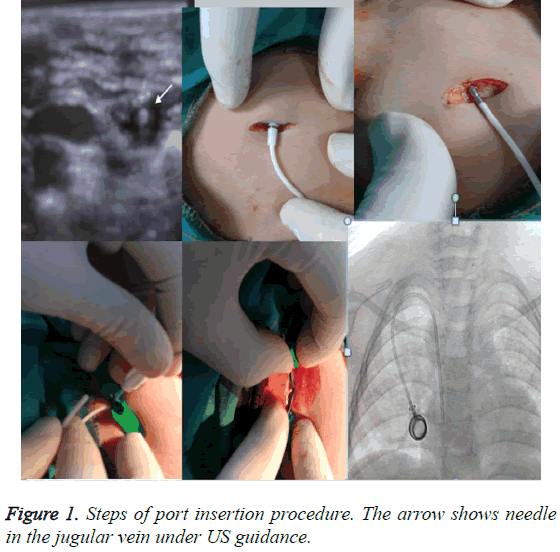
All procedures were performed under general anesthesia, anesthesia consultation was made prior to the procedure. Prothrombin time and platelet values of the patients were checked after approval had been obtained from the anesthetist (PT>17 Sec, PLT>50000/mm3). All patients had been using broad spectrum antibiotics, therefore prophylactic antibiotic was not needed to use. The whole chest and neck regions were stained with povidone-iodine up to mandible after the patients had been taken to supine position. Thereafter the patient was covered with sterile drapes. The interventional radiologist conducted the procedure in accordance with sterilization rules. 8-10 F low profile single lumen port catheter was used for older children and 6F (Polysite, Vygon, Italy) catheter was used for infants or smaller children. All venous interventions were performed from the right internal jugular vein under ultrasonography and fluoroscopy. The incision was done from 2 cm caudal part of clavicle. 21 gauge needles were used for all jugular punctures. Subcutaneous port pocket was opened with blunt dissection so as to be sufficient for port. Afterwards a tunnel was opened subcutaneously using a tunnel device up to jugular puncture site. Peel-away sheath was placed over the guide-wire. The catheter was placed after the guide-wire had been removed using a dilator within the peel-away sheath. While the peel-away sheath was being removed from one side, the catheter was preceded into the sheath in another side. After catheter tip was ensured to be at vena cava superior junction through fluoroscopy, subcutaneous tissue was closed with 3.0 vicryl suture, skin was closed with 3.0 ethilon suture. Port reservoir was checked through making a sufficient aspiration with Huber needle. The procedure was terminated after washing with heparinized saline (Figure 1).
Results
Port insertion procedure was performed with 100% success in all patients. Port catheter was removed in the ratio of 72% (49/68) during the study period, 27.9% (19/68) are still being used. Mean duration of use is 199 days for port catheter. Dysfunction was detected in the aspiration done from port reservoir in 3 patients in perioperative period (Table 1). In fluoroscopy control, port catheter was detected to have an angulation at jugular entrance point. So port catheter was revised using guide-wires. A control CT was obtained as haemoglobin values were seen to decrease within the same day in 2 patients. CT results did not reveal a significant hematoma. However a leakage was detected at jugular entrance point in one patient and from port pocket in another. The first patient was revised with 8F catheter through over-sizing the 6 F catheter and the leakage stopped. Port catheter had to be removed totally in the latter. Hemorrhage site was detected and cauterized. One patient was diagnosed with early catheter related infection due to Enterococcus spp. growing 13 days after catheter insertion and the port catheter had to be removed.
| Perioperative and long-term complication rates | ||
|---|---|---|
| Perioprerative complication | ||
| Jugular vein site and port pocket site hemorrhage |
n=2 | 2.94% |
| Catheter malposition | n=2 | 2.94% |
| Long-term complication | ||
| Catheter malposition | n=2 | 2.94% |
| Insertion site infection | n=1 | 1.47% |
| Catheter- related blood stream infection | n=3 | 4.40% |
| Skin dehiscence | n=3 | 4.40% |
| Premature catheter removal | n=8 | 11.76% |
Table 1: Perioperative and long term complications of implantable chest port procedures.
Late catheter infection was detected 95,142,203 days after port catheter insertion. Coagulase negative Staphylococcus aureus was detected in one of these patients and he/she had significant edema, erythema and cellulitis findings at port site. So port catheter was removed. Pseudomonas aeruginosa was detected at port site in 2 patients, one patient had skin dehiscence. Port catheter was removed in these two patients. Skin dehiscence was observed in 3 patients in whom no clinical or laboratory findings of infection were detected. Skin and port pocket was revised and port reservoir was placed again.
Catheter malposition-related catheter dysfunction was detected in 2 patients 150 and 183 days after port catheter insertion. Chest port catheter was placed again in these patients. Perioperative pneumothorax, hemothorax, air embolism were seen in no patients. Also venous thrombosis and fibrin sheath were not encountered.
Discussion
Chest port device is an indispensable venous access in pediatric oncology patients. Port reservoir’s staying beneath the skin and forming a natural barrier provide great advantages in patients who are already immune-compromised. However some complications may develop after port insertion. While publications about port insertion are available reported by pediatric surgeons and interventional radiologists, papers are also available comparing data of both groups [4-6].
In this study, outcomes of paediatric oncology patients who were inserted port at Department of Interventional Radiology during recent 2 years are discussed. Because port insertion had been performed by paediatric surgeons before this period.
Paediatric surgeons usually insert port catheter with anatomic landmark technique. Many studies have reported that imageguided percutaneous techniques reduce procedure-related complications [4,5,7].
Detection of jugular vein may be difficult particularly in infants. USG-guided puncture is an easy and safe method. Use of fluoroscopy provides great advantages with regard to detect perioperative catheter dysfunctions immediately. Dysfunction developed in 2 of our patients due to angulation at jugular vein entrance. We could correct this through guide wires under fluoroscopy in the course of the procedure. Technical success rate was 100% in our study. Premature catheter removal rates are 13% (8% due to infection and 5% due to blockage) in Munro et al. study. Also in Ross et al. study prematüre catheter removal rate is 12%. These results are closing similar to our study [8,9]. In this study, early complications developed in a total of 3 patients including haemorrhage at port catheter entrance, at port reservoir localization in 2 patients, early portrelated infection in one patient. In the late period, catheter malposition-related infection was observed in 2 patients and catheter-related infection developed in 3 patients, these rates are consistent with the other series [2,3,6,10,11].
The limitation of our study is that we could not reach detailed data about port catheters inserted by pediatric surgeons when we analyzed data retrospectively. Therefore we could not make a comparison.
In conclusion, vast majority of port devices were being inserted by paediatric surgeons before. We consider that interventional radiologists come in the foreground in that field while the importance of imaging-assisted insertion of port devices is gradually increasing.
References
- Biffi R, Toro A, Pozzi S, Di Carlo I. Totally implantable vascular access devices 30 years after the first procedure. What has changed and what is still unsolved. Support Care Cancer 2014; 22: 1705-1714.
- Jonge RC, Polderman KH, Gemke RJ. Central venous catheter use in the pediatric patient: mechanical and infectious complications. Pediatr Crit Care Med 2005; 6: 329-339.
- Crowley JJ, Pereira JK, Harris LS, Becker CJ. Radiologic placement of long-term subcutaneous venous access ports in children. AJR Am Roentgenol. 1998; 171: 257-260.
- Cil BE. Radiological placement of chest ports in pediatric oncology patients. Eur Radiol 2004; 14: 2015-2019.
- Lorenz JM, FFunaki B, Van Ha T, Leef JA. Radiologic Placement of Implantable Chest Ports in Pediatric Patients. AJR Am Roentgenol 2001; 176: 991-994.
- Shetty PC, Mody MK, Kastan DJ. Outcomes of 350 implanted chest ports placed by interven- tional radiologists. J Vasc Interv Radiol 1997; 8: 991-995.
- Lameris JS, Post PJ, Zonderland HM. Percutaneous placement of Hickman catheters: comparison of sonographically guided and blind techniques. AJR Am Roentgenol 1990; 155: 1097-1099.
- MunroFD, GillettPM, Wratten JC. Totallyim-plantable central venous access devices for paediat- ric oncology patients. Med Pediatr Oncol 1999; 33: 377-381.
- Ross MN, Haase GM, Poole M. Comparison of totally implanted reservoirs with external catheters as venous access de- vices in pediatric oncologic patients. Surg Gynecol Obstet 1988; 167: 141-144.
- Viana Taveira MR, Lima LS, de Araujo CC, de Mello MJ. Risk factors for central line–associated bloodstream infection in pediatric oncology patients with a totally implantable venous access port: A cohort study. Pediatr Blood Cancer 2016.
- Tsai HL, Liu CS, Chang JW. Totally Implantable Venous Access Ports via the External Jugular Vein: Safety and Effectiveness for Young Pediatric Patients. J Pediatr Hematol Oncol 2008; 30: 366-368.