- Biomedical Research (2016) Volume 27, Issue 2
The prognosis factors research on the 172 non-hodgkin lymphoma cases.
| Jia Ning Jiang, Xiu Hua Sun* Department of Medical Oncology, The Second Affiliated Hospital of Dalian Medical University, Dalian 116027, Liaoning Province, PR. China |
| Corresponding Author: Xiu Hua Sun Department of Medical Oncology The Second Affiliated Hospital of Dalian Medical University 467 Zhongshan Road Shahekou District, Dalian 116027, Liaoning Province PR. China |
| Accepted: January 20, 2016 |
Abstract
Objective: To make a research on the prognosis factors of non-hodgkin lymphoma (NHL) cases, and discuss how to improve the prognosis as far as possible.
Methods: To collect 200 cases of NHL in The Second Affiliated Hospital of Dalian Medical University from January 1st 2008 to January 1st 2013, except for the withdraw and the untreated, 172 cases were in the study with the follow-up visit information. To analyse the data by SPSS17.0 and compare the survival rate by Kaplan-Meier. To analyse the effects of different factors on the patients’ prognosis. To use Cox model to analysis the single factor into multi-factor.
Results: Except for the withdraw and the patients untreated, there were 172 cases in our research. The survival rate of 1 year, 3 years, 5 years is 72.7%, 50.6% and 36.0%. Analysed by single factor, the factors had an influence on the prognosis were age, Ann Arbor-Cotswold’s, IPI, LDH, general symptom, pathological type and therapy scheme. There was no evidence confirming sex, first zone, bone marrow puncture, extracapsular extension were the prognosis factors. Results: (1) Age: Patients below 60 years obviously had a better prognosis than them at or after 60. (2) Ann Arbor-Cotswold’s: Patients at 1st or 2nd stage had a better prognosis than those at 3rd or 4th stage. (3) IPI: low risk (0-1 score), lowintermediate risk (2 scores), high high intermediate risk (3 scores) and high risk (4-5 scores). The higher IPI was the worse prognosis would be. (4) The level of serum LDH: patients with a higher level would have a worse prognosis than the ones with it normal. (5) General symptom: Patients without general symptoms had a better prognosis. (6) Pathological type: NHL from B lymphocyte had a better prognosis than those from NK/T. To make a further analysis on B cell subgroups, there was a statistic difference among them. On the contrary, there was no statistic difference among the NK/T’s. (7) Therapy scheme: In the 1st or 2nd stage group, the therapy scheme didn’t affect the prognosis much, but comprehensive therapy was much better than chemotherapy or radiotherapy alone in the 3rd of 4th stage.
Conclusion:
- Age, Ann Arbor-Cotswolds, IPI, LDH, general syptom, pathological type and therapy scheme were related to the prognosis of NHL. Except for the last, all the factors were independent prognosis factors.
- Our study hadn’t testified gender, 1st zone, bone marrow puncture or involvement outside could affect the prognosis of NHL, so more researches needed to be done.
Keywords |
||||||||||
| Non-hodgkin lymphoma(NHL), Clinical features, Prognosis factors. | ||||||||||
Introduction |
||||||||||
| Lymphoma includes Hodgkin Lymphoma (HL) and non- Hodgkin Lymphoma (NHL) by WHO, the American Cancer Society has issued that HL accounts for 11 percent and NHL 89 percent [1]. HL has a better prognosis, but NHL’s prognosis is different. At present, a great number researchers have found NHL’s prognosis seems related to age, pathology, tumor load, staging, international prognosis index (IPI) [2], treatment and so on [3]. So it has been very important for therapeutic schedule to confirm prognosis factors and estimate effect. This was a retrospective study of NHL cases in our hospital during the last five years, which has analysed the prognosis factors and different therapeutic schedules. | ||||||||||
Materials and Methods |
||||||||||
Clinical material |
||||||||||
| 200 NHL cases in the Second Affiliated Hospital of Dalian Medical University from January 2008 to January 2013, 197 cases have been testified by pathology (98.5%), 3 by cytology (1.5%). 118 cases were males (59.0%), and 82 were females (41.0%). 98 patients were after 60 years old (49.0%), with the median age 48 years old. 87 cases had general symptoms (43.5%). The deadline of the follow-up visit was January 2014, 6 years in total, with the median time 3 years. 172 patients of all had completely clinical information. | ||||||||||
| All the subjects in this study have signed the informed consent form, and this study was approved by the Ethics Committee of The Second Affiliated Hospital of Dalian Medical University. | ||||||||||
Method |
||||||||||
First symptom and position |
||||||||||
| Among the 200 patients, painless superficial lymph node enlargement as the 1st symptom came to 94 cases (47.0%), gastrointestinal symptoms with its mass to 27 cases (13.5%), deep lymph nodes enlargement in viscera or mediastinum to 17 cases (8.5%), tonsil enlargement to 14 cases (7.0%), goitre in nasal cavity with rhinobyon to 13 cases (6.5%), personality change or nervous system disorder to 6 cases (3.0%), testicle goitre to 4 cases (2.0%), bone pain to 4 cases (2.0%), back pain of kidney diseases to 3 cases (1.5%), skin pricking with neoplasm to 3 cases (1.5%), thyroid goitre to 3 cases (1.5%), breast goitre to 3 cases (1.5%), menestration change with ovary mass to 2 cases (1.0%), spleen enlargement to 2 cases (1.0%), sore gums to 1 case (0.5%), hilar disorder with respiratory symptoms to 1 case (0.5%), abnormal vaginal discharge of endometrium disorder to 1 case (0.5%), eyelid goitre to 1 case (0.5%), appendiceal disorder to 1 case (0.5%). | ||||||||||
Clinical stage |
||||||||||
| According to Ann Arbor-Cotswolds, 21 cases were as stage for I (10.5%), and 19 cases were IA (90.5%), 2 cases were IB (9.5%). 22 cases were as stage for II (11.0%), 15 cases were IIA (68.0%), and 7 cases were IIB (32.0%), 60 cases were as much stage for III (30.0%), 37 cases were IIIA (62.0%) and 23 cases IIIB (38.0%). 97 cases were as much stage for IV (48.5%), 43 cases were IVA (44.3%) and 54 cases IVB (55.7%). | ||||||||||
Pathological type |
||||||||||
| Among all the patients, 197 cases have been testified by pathology (98.5%) and 3 by cytology (1.5%). By pathology, 97 cases were diffuse large B cell (DLBC) (48.5%), 29 follicular lymphoma (FL) (14.5%), 23 peripheral T-cell lymphomaunspecific (11.5%), 14 small B-cell lymphoma (SLL) (7.0%), 8 mantle cell lymphoma (MCL) (4.0%), 8 angioimmunoblastic lymphadennopathy T cell lymphoma (4.0%), 5 anaplastic large cell lymphoma (ALCL) (2.5%), 4 marginal zone lymphoma (MZL) (2.0%), 4 nasal NK/T lymphoma (2.0%), 3 Burkitt (1.5%) and 2 mucosa-associated lymphoid tissue (MALT) (1.0%). | ||||||||||
Whether bone marrow puncture befor first treatment |
||||||||||
| Among all the definite cases, 96 cases hadn’t bone marrow puncture (48.0%) and 104 had (52.0%) with positive result 16 cases (15.4%), negative result 88 cases (84.6%). | ||||||||||
Intenational Prognostic Indes (IPI) |
||||||||||
| IPI was consist of age after 60 years old, Ann Arbor-Cotswolds (III and IV), PS more than 1 ,more than 1 entensive infiltration and LDH in serum when diagnosed first. Each factor occupied 1 point, low risk (0-1), lowintermedi-aterisk(2), highintermediaterisk( 3) and high risk(4-5). Among all the patients, 45 patients were in low risk (22.5%), 30 in lowintermedi-aterisk (15.0%), 75 in highintermedi-aterisk (37.5%) and 50 in high risk (25.0%). | ||||||||||
Treatment |
||||||||||
| Among all the cases, 19 were withdraw (9.5%) and 9 died without treatment (4.5%). In the studied 172 cases, 4 cases accepted radiotherapy only (2.3%) and 85 did chemotherapy only (49.4%). 83 accepted associated comprehensive treatment, 19 of them did chemotherapy with molecular targeting treatment (22.9%), 37 did chemoradiotherapy alone or with molecular targeting treatment (44.6%), 22 had surgery, adjuvant chemotherapy with or without molecular targeting treatment (26.5%), 5 did surgery, radiotherapy and chemotherapy (13.2%). | ||||||||||
Chemotherapy alone |
||||||||||
| Among the cases with chemotherapy alone, CHOP (CTX +ADM+VCR+PDN) was the first line for 59 cases (69.4%), CHOPE (CTX+ADM+VCR+PDN+VP-16) for 10 cases (11.8%), COP (CTX+VCR+PDN) for 8 cases (9.4%), COPE (CTX+VCR+PDN+VP-16) for 2 cases (2.4%), FDM (FLU +DXM+MTT) for 2 cases (2.4%), CHO (CTX+ADM+VCR) for 1 case (1.2%), VP (VCR+PDN) for 1 case (1.2%), CVP (CTX+VCR+PDN) for 1 case (1.2%), COPP (CTX+ADM +VCR+PDN+PCB) for 1 case (1.2%). | ||||||||||
Comprehensive treatment |
||||||||||
| 83 cases accepted associated comprehensive treatment. 19 of them did chemotherapy with rituximab (22.9%). 28 did radiochemotherapy (33.7%), 23 of them had CHOP (82.1%), 3 had COPE (10.7%), 1 had COP (4.3%), 1 had MTX intrathecal injection (4.3%). 9 cases accepted radiochemotherapy with molecular targeting treatment (10.8%). 16 cases did surgery with adjuvant chemotherapy, 14 of them had CHOP (87.5%) and 2 had COP (12.5%). 6 cases accepted surgery with adjuvant treatment R-chop. 5 cases did surgery and adjuvant radiochemotherapy, 2 of them did CHOP+MTX (40.0%), 1 did CHOP (20.0%), 1 did COMP (20.0%) and 1 did VP+MTX (20%). | ||||||||||
Statistical analysis |
||||||||||
| Overall survival was from the beginning of treatment to the death or the last follow-up visit. The follow-up visit began in January 2008, ended in January 2014. Survival rate was calculated by Kaplan-Meier, and Cox was applied for the evaluation of clinical factors to prognosis. χ2 test was applied for group comparison, P<0.05 had statistical significance. | ||||||||||
Results |
||||||||||
Survival rate |
||||||||||
| 19 cases lost to follow up, to make withdraw rate 9.5%. 181 cases had been followed-up during the 5 years, 119 died (65.7%), and 9 died of rejecting any treatment, so 172 cases were studied by us. Its 1-year survival was 50.6%, 3-year survival 72.7% and 5-year survival 36.0%. All kinds of prognostic factors were showed in Table 1. Univariate analysis found that the prognosis factors were age, Ann Arbor- Cotswolds, B symptoms, serum LDH, pathological type, treatment. Sex, first region, extranodal invaded, marrow puncture or not before treatment might make little difference to the prognosis. | ||||||||||
Gender and prognosis |
||||||||||
| 101 male patients were studied, its 1-year, 3-year, 5-year survival was 72.3%, 44.6% and 40.6%. The 71 females’ was 83.1%, 56.3% and 46.5%. Statistic analysed (χ2=0.783, P>0.05), with no significance. So sex couldn’t be confirmed as a prognostic factor, and more researches were needed (Table 1). | ||||||||||
Age and prognosis |
||||||||||
| 89 cases were before 60 years old, whose 1-year, 3-year, 5-year survival was 83.1%, 52.8% and 41.6%. 83 cases were after 60 whose 1-year, 3-year, 5-year survival was 65.1%, 42.2% and 32.5%. Statistic analysed (χ2=7.813, P<0.05), showing evident difference that the prognosis of cases before 60 was much better than those after 60 (Table 1). | ||||||||||
Extranodal invaded and prognosis |
||||||||||
| 85 cases were without extranodal invaded, whose 1-year, 3- year,5-year survival was 58.5%, 49.6% and 24.2%. 87 cases were extranodal invaded whose was 54.0%, 42.1% and 25.3%. Statistic analysed (χ2=1.451, P>0.05), showing no statistical significance that extranodal invaded couldn’t be testified (Table 1). | ||||||||||
Serum LDH and prognosis |
||||||||||
| Serum LDH was measured at the beginning, 58 cases were in high level, whose 1-year, 3-year, 5-year survival was 53,2%, 37.1% and 22.0%. 114 cases were in normal, with it 58.7%, 48.2% and 38.3%. Statistic analysed (χ2=6.357, P<0.05), showing statistical difference that serum LDH contributed to the prognosis. Patients in normal had a better prognosis (Table 1). | ||||||||||
Marrow puncture before treatment and prognosis |
||||||||||
| 90 cases had marrow puncture before treatment, whose 1-year, 3-year, 5-year survival was 91.6%, 48.9% and 34,4%. 82 cases hadn’t with it 73.2%, 43.9% and 36.6%. Statistic analysed (χ2=0.03, P>0.05), showing no statistical difference that marrow puncture before treatment might contribute little to the prognosis (Table 1). | ||||||||||
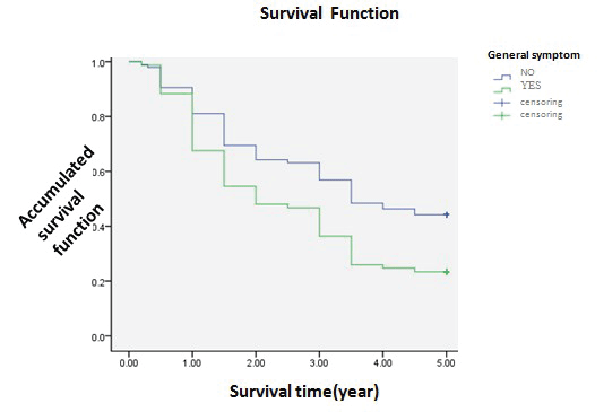
B symptoms and prognosis |
||||||||||
| According to the general symptoms, group A means no the symptoms and B means the opposite. 95 cases were in group A whose 1-year, 3-year, 5-year survival was 81.8%, 69.5% and 48.4%. 77 cases were in group B with it 67.5%, 36.4% and 23.4%. Statistic analyzed (χ2=8.724, P<0.05), with the picture showing the overall survival of the former better than the latter. We found cases in group A had a better prognosis (Table 1 and Figure 1). | ||||||||||
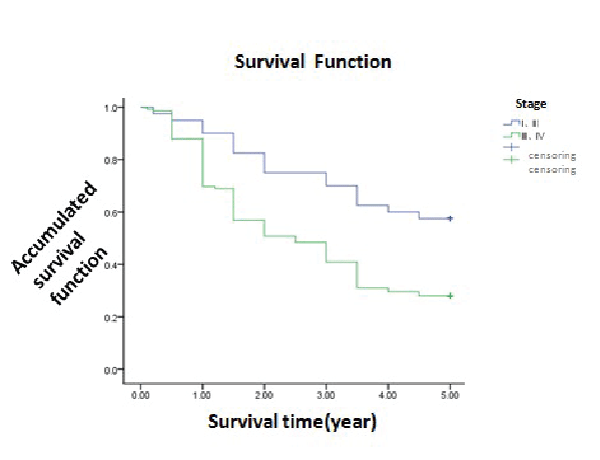
Ann Arbor-Coswolds and prognosis |
||||||||||
| 1-year, 3-year, 5-year survival of patients at stage I or II was 90.0%, 70.0% and 57.5%. And was 69.7%, 40.9% and 28.0%. From the picture, the survival curve of the former was much better than the latter. Statistic analysed (χ2=11.483, P<0.05), showing statistical difference that the earlier stage, the better prognosis (Table 1 and Figure 2). | ||||||||||
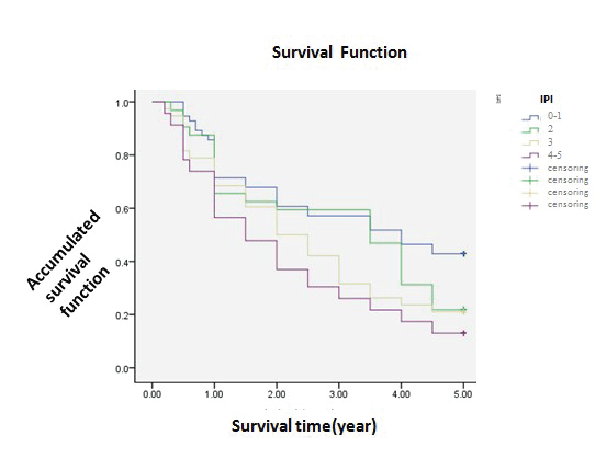
IPI and prognosis |
||||||||||
| 56 cases were in low risk (0-1), 22 cases in lowintermediaterisk (2), 38 cases in highintermedi-aterisk (3) and 46 cases in high risk (4-5). The 1-year survival was 71.4%, 65.6%, 68.4% and 56.5%. The 3-year survival was 57.1%, 59.4%, 31.6% and 26.1%. The 5-year survival was 42.9%, 21.9%, 21.1% and 13.0%. Bonding to the picture, the low risk had a better survival than the others. Statistic analysed (χ2=13.816, P<0.05), showing statistical difference that the lower IPI, the better prognosis (Table 1 and Figure 3). | ||||||||||
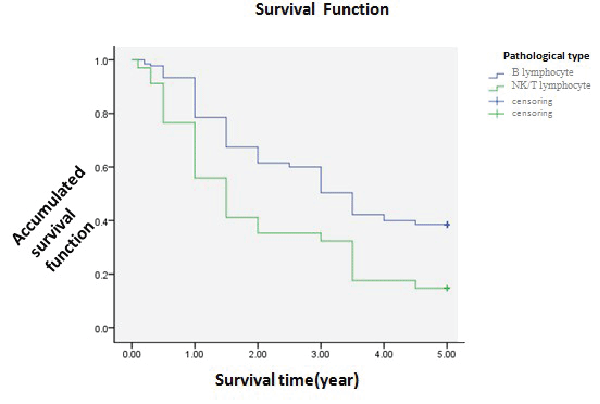
Pathological and prognosis |
||||||||||
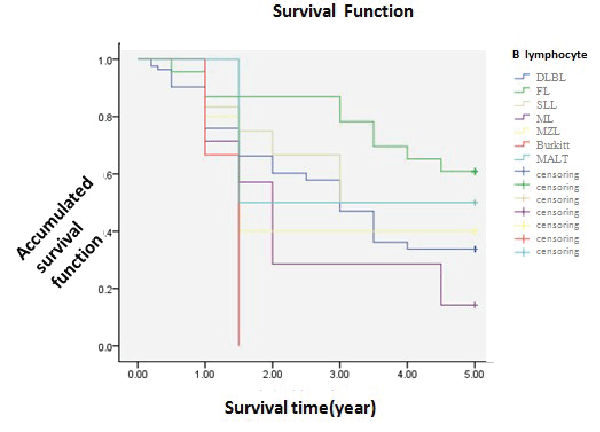
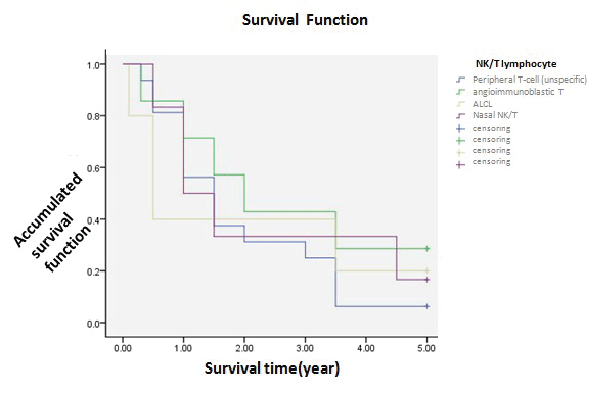
| But for the withdraw and untreated cases, 172 cases had been testified as NHL by pathology. 137 cases of those were from B cells, 35 from NK/T cells. The 1-year survival was 78.5% and 55.9%. The 3-year survival was 50.4% and 32.4%. The 5-year survival was 38.5% and 14.7%. Bonding to the picture, the former had a better survival than the latter. Statistic analysed (χ2=11.174, P<0.05), showing statistical difference that B cell lymphoma had a better prognosis. To further analyse, different subtypes from B cell including DLBC, FL, SLL, MCL, MZL, Burkitt, MALT, showed as the picture that each subgroup had different survival. The 1-year was 75.9%, 87.0%, 83.3%, 71.4% 80.0%, 66.7% and 100.0%. The 3-year survival was 47.0%, 78.3%, 50.0%, 28.6%, 40.0%, 0 and 50.0%. The 5-year survival was 33.7%, 60.9%, 50.0%, 14.3%, 40.0%, 0 and 50.0%. Statistic analysed (χ2=13.375, P<0.05), showing different subtypes had different prognosis. NK/T lymphoma including peripheral T-cell lymphoma- unspecific, angioimmunoblastic lymphadennopathy T cell lymphoma, nasal NK/T lymphoma. Just as the picture showed, though the survival was not the same, the curve was coinciding a little. The 1-year survival was 56.3%, 71.4%, 40.0% and 50.0%. The 3-year survival was 25.0%, 42.9%, 20.0% and 16.7%. The 5- year survival was 6.3%, 28.6%, 20.0%, 16.7%. Statistic analysed (χ2=1.22, P>0.05), showing no evident difference that the prognosis of different NK/T subtypes was nearly the same (Table 1 and Figures 4, 5, 6). | ||||||||||
First region and prognosis |
||||||||||
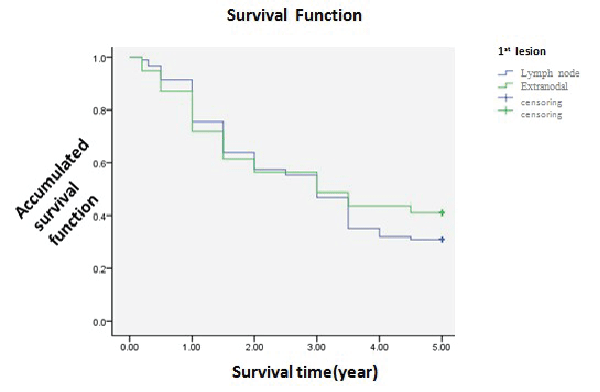
| We divided the cases into two groups, lymph node as the first region and the extranodal as the first. 94 cases were in the former, whose 1-year, 3-year, 5-year survival was 75.5%. 46.8% amd 30.9%. 78 cases were in the latter, whose was 71.8%, 48.7% and 41.0%. Showed by the picture, the two survival curve was almost coincided within 3 years. Bonding to the statistic analysis (χ2=0.737, P>0.05), showing no difference that first region might contribute little to the prognosis (Table 1 and Figure 7). | ||||||||||
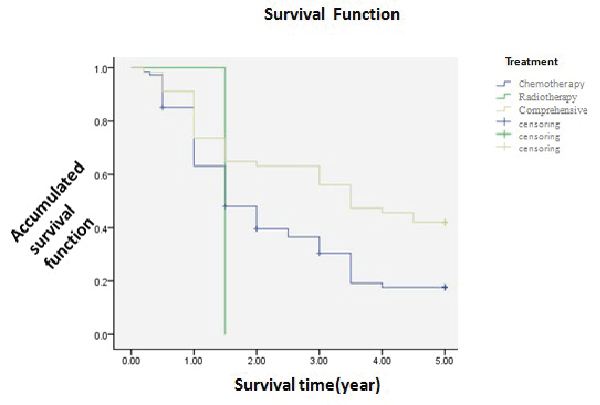
Treatment of different stages and prognosis |
||||||||||
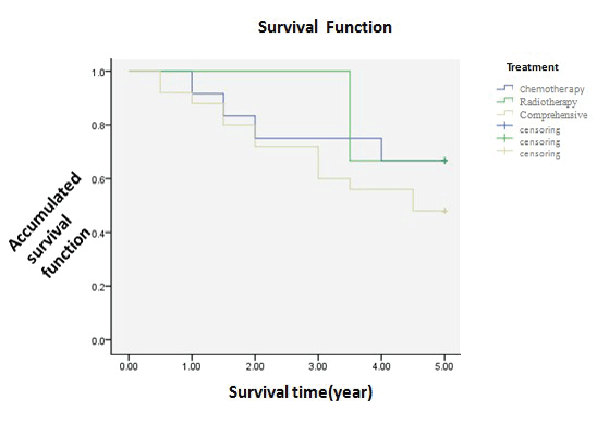
| Patients as stage for I or II was 40 cases, 11 of them had chemotherapy only, 3 had radiotherapy only and 26 had associated comprehensive treatment. The 5-year survival was 66.7%, 0 and 48.0%. Statistic analysed (χ2=1.121, P>0.05), showing no difference that the way of treatment contributed little to the prognosis. Patients as much stage for III or IV was 132 cases, 74 cases had surgery only, 1 case had chemotherapy only and 57 cases had comprehensive treatment. The 5-year survival was 17.6%, 0 and 42.1%. As showed as the picture, their survival curves were obviously different, and the comprehensive was better than the other two. Statistic analysed (χ2=10.075, P<0.05), showing difference that comprehensive treatment could improve the survival of patients as late stage (Table 1 and Figures 8, 9). | ||||||||||
Multi-factor analysis |
||||||||||
| Kaplan-Meier was applied as the single factor analysis, to find that age, Ann Arbor-Cotswolds, IPI, serum LDH, B symptoms, pathological type and treatment were the prognostic factors. Cox was applied to analyse the single factor to find except for the treatment, all the factor were the independent prognostic factors (Table 2). | ||||||||||
Discussion |
||||||||||
| NHL originates from lymphoid tissue, a rapid disseminated tumor of immune system that is the most common malignant tumor of blood system. The latest data collected by American Cancer Society has showed it occupies 89% [1]. The prognosis is heterogeneity. Judging it correctly has great value in making right treatment schedule, improving effect, decreasing adverse reactions. In the past 10 years, some scholars found some prognostic parameters, such as age, nodule size, the number of lesions, marrow infiltration, B symptoms, serum LDH. Then IPI [2] was setted out by the 16 institute of America, Canada and European countries. At present, large numbers of studies have found that the prognosis of NHL may relate to age, pathological type, tumor load, clinical stage and treatment [3]. Our study has make single factor analysis to find it related to age, Ann Arbor-Cotswolds, IPI, serum LDH, B symptoms, pathological type and treatment. Multi-factor analysis has showed age, Ann Arbor-Cotswolds, IPI, serum LDH, B ymptoms, pathological type are the independent factors, which conforms to the past literatures. | ||||||||||
| In the 172 cases, patients before 60 years old have a better prognosis, which testifies age is an independent factor and conforms to the reports at home and abroad. Because of the low-immunity, some organs’poor function which increases the marrow suppression of chemotherapy and radiotherapy, elder has a worse prognosis. But age is a uncontrolled factor that we can do nothing to. Ann Arbor-Cotswolds has been used by NHL, large numbers of clinical information have testified patients at stage for I and II have a better prognosis, and our study has received the approximated result. So early discovery, early diagnosis and early treatment contribute a lot [4]. The treatment schedule is always different between patients at early stage (I and II) and those at late (III and IV). More and more late patients improve more or less after conventional therapy and high dose of radiochemotherapy [5]. Serum LDH can react tuomor load, proliferation and the immune recognition, so it can be a prognostic factor which is negative related [6]. Our study conforms to the points above. IPI is according to age, ECOG, Ann Arbor-Cotswolds, extranodal number and serum LDH, which is divided into low risk(0-1), lowintermediaterisk( 2), highintermedi-aterisk(3) and high risk(4-5). IPI has been applied to low, mediate and high malignant [7,8]. This study has showed with the IPI increasing, the risk increasing, the survival lowing and prognosis falling, which conforms to the home and aborad. | ||||||||||
| Dependent on the general symptoms, it can divide into group A which has none and B which has the symptoms. B symptoms includes fever, night sweet and losing weight more than 10%, which have except for diagnosed reasons within 6 months. Finsen Institute studied 602 cases of NHL and compares the risk of group A with B, to find the statistic result P<0.0001 which showed group B had a worse prognosis. And our study has received the same result. | ||||||||||
| Pathological type is an independent prognosis factor. NHL originates from B lymphocyte, NK/T lymphocyte or the mixture. According to REAL/WHO, B lymphoma occupies 65.3% and NK/T 34.7%. And prognosis of the former is better than the latter by associated researches. Our study has got the same result. Then we compare the common subtypes of B lymphoma with NK/T, to find the prognosis is different in different subtypes of B lymphoma. The order better-to-worse is MALT, FL, BLL, MZL, DLBL, ML and Burkitt. Some studies showed indolent lymphoma such as FL had a better prognosis; invasive lymphoma such as DLCL had a worse one. And monocyte B lymphoma, MALT and lympho-plasmacytic lymphoma were in the middle. Our study is a little different, which may relate to insufficient samples, so more studies can be done under the sufficient ones. There is no difference among the 35 NK/T samples, which is disaccordance with reports at home and abroad [9]. Insufficient samples may cause it, so enlarging samples is necessary. | ||||||||||
| Our study has showed treatment isn’t an independent prognostic factor, which is controversial. It may be caused by the treatment of patients at early stage which shows the prognosis is not related to the treatment. Treatment schedules are chemotherapy, radiotherapy or comprehensive treatment such as radiotherapy, chemotherapy and molecular targeting treatment. Most NHL is invasive, such as DLBL and angioimmunoblastic lymphadennopathy T cell. CHOP was recommended in the past, but it trended to relapse and had a bad effect of saving treatment. Indolent lymphoma including FL and SLL, CHOP was recommended as the first line in the past, which early effect could get CR but ease to relapse. 98 percentage of B NHL express CD20, rituximab [10] combines with CD20 and induces the cytotoxicity mediated by antibody and complement, dissolve B cells to inhibit proliferating, induce apoptosis and evaluate the sensitiveness to chemotherapy. Rituximab combined with CHOP has been a better schedule than conventional chemotherapy in effect, prognosis and survival [11]. High invasive NHL, including lymphoblastic lymphoma and Burkitt. Obviously, CHOP alone cannot achieve a satisfying effect, so the chemotherapy schedule of acute lymphocytic leukemia is recommended. It needs high dose, long course and to pay attention to the invading of central nervous system. As for high invasive NHL, high dose chemotherapy, radiotherapy with autologous or allogeneic transplantation [12,13]. | ||||||||||
| Our study has showed the 5-year survival of I and II stage is 66.7% in chemotherapy, 0% in radiotherapy and 48.0% in comprehensive treatment (P>0.05), which prompts chemotherapy may be better than comprehensive in early stage. But the 5-year survival decreases to 17.6%, 0% and 42.1% at late (P<0.05), which prompts the comprehensive and chemotherapy is better than chemotherapy. At present, CHOP can be used as the first line for low malignant patients as stage for I and II. To mediate malignant patients as stage for I and II, srong combined chemotherapy is recommended. To patients as much stage for III and IV, high-level chemotherapy should be used for more than 6 to 8 courses. And hemopoietic stem cell transplantation is best. To mediate, high malignant of refractory lymphoma, high-dose radiochemotherapy combined with hemopoietic stem cell transplantation should be done as early as possible. Neither autologous nor allogeneic transplantation is common, which can be studied in future. | ||||||||||
| Our study has showed gender, marrow puncture before treatment, first region and extranodal invading affect the prognosis. Danish Finsen Institute collected 602 adults suffering NHL, to find that the prognosis of males was worse than females. It might result from the marrow function, because some studies showed females have it better [14]. But most studies showed, there’s no statistical difference among the 1-year, 3-year and 5-year survival (P>0.05) [15]. Our study supports the latter opinion, which conforms to most reports. So whether gender is a prognostic factor is controversial, more studies need to be done. If marrow infiltration occurs, it has been as much for IV stage, which has a bad prognosis. Marrow puncture contributes to diagnosis, to make a treatment schedule and to improve the prognosis [16]. But our study showed the opposite. Because most cases in our study are late stage, having marrow puncture or not does little to prognosis, so there is no difference in choosing the treatment schedule. We can enlarge the samples diagnosed as early age without marrow puncture and study. Our study has explored the affection of first lesion on prognosis, to find lymph or extranodal tissue does little. But associated results have testified when the first region is superficial lymph node, gastrointestinal track, spleen, lung, testis and ovary, the prognosis is good after comprehensive treatment such as surgery, chemotherapy, radiotherapy and molecular targeting treatment [17]. On the contrary, when the first lesion is liver, breast, central nervous system, nasopharynx, bone and skin, the prognosis is worse [18-22]. When the first lesion is spleen which conforms two or more items, including evaluated LDH, the size of tumor larger than 9 centimeters, with general symptoms and in high proliferated [23]. According to the international extranodal lymphoma study group (IELSG), there are mainly 5 dangerous factors. They are patients at or after 60 years old, Karnofsky (KPS) more than 70, evaluated serum LDH and cerebrospinal fluid, lesion in deep [24]. Our study doesn’t conform to the points above. We due to the insufficient of cases, so more cases should be collected to guarantee the samples of each subgroup. | ||||||||||
| Above all, for all the NHL patients, confirming bad factors, comprehensive analysis, considering the clinical feature pathological type of patients, confirming staging, accurate IPI can help choose the ideal treatment schedule, prolong the survival and improve the life quantity. Our study brings in more factors, and the balance among the groups is poor. The samples are not sufficient enough, and the study is retrospective. So we should enlarge the samples or make foresight study, and devise more reasonable statistical analysis to confirm the prognostic factors of NHL, to supply more accurate and reasonable evidence-based proof for patients. | ||||||||||
Conclusion |
||||||||||
| The prognosis of NHL is affected by many factors such as age, Ann Arbor-Cotswolds, IPI, serum LDH, B symptoms, pathological type and treatment, except for treatment, they are independent prognostic factors. | ||||||||||
| Our study has testified age, first region, marrow puncture before treatment and extra nodal invading affect the prognosis, so more samples need to be done in future. | ||||||||||
Tables at a glance |
||||||||||
|
||||||||||
Figures at a glance |
||||||||||
|
||||||||||
|
||||||||||
References |
||||||||||
|