Research Article - Journal of Psychology and Cognition (2017) Volume 2, Issue 1
Screening for speech-language development in Emirati toddlers.
Lolowa A Almekaini*, Taoufik Zoubeidi, Yusuf Albustanji, Hassib Narchi, Omer Al Jabri, Abdul-Kader Souid
Departments of Pediatrics, UAE University, Al-Ain, UAE
- *Corresponding Author:
- Lolowa A Almekaini
Departments of Pediatrics
UAE University Al-Ain, UAE
Tel: +971-3-713-7335
Fax +971-3-767-2022
E-mail: lolwa.mukini@uaeu.ac.ae
Accepted date: January 26, 2017
Citation: Almekaini LA, Zoubeidi T, Albustanji Y, et al. Screening for speech-language development in Emirati toddlers. J Psychol Cognition. 2017;2(1):26-31
DOI: 10.35841/psychology-cognition.2.1.26-31
Visit for more related articles at Journal of Psychology and CognitionAbstract
Background: The normal development of speech-language is especially challenging for Emirati toddlers, as they are frequently raised by live-in multilingual caretakers.
Methods: In this community-based study, we screened preschool Emirati children for delayed expressive language and associated socio-emotional/behavioral problems. Arabic versions of the Language Development Survey and Child Behavior Checklist for ages 1.5-5 years were validated before being used in this study. The data collection instruments (questionnaires) were completed by primary caregivers in the presence of trained staff. Delayed language was defined as a vocabulary size fewer than 20 words at 18-23 months or fewer than 50 words at 24-35 months.
Results: One hundred fifty two children (median-age, 26 months; 53% females) were enrolled in this study. Fifty-six percent of 18-23 month-old children had vocabulary size ≥ 20 words, 48% of the 24-29 month-old had vocabulary size ≥ 50 words and 46% of the 30-35 month-old had vocabulary size ≥ 50 words. Fifty four percent of 24-34 month-old children used combining words; with an average (SD) length-of-phrases of 3.9 (1.1), median=4.0; range=2.0-6.0. Household words (e.g. bed) were most common and exterior words (e.g. flowers) were least common. Vocabulary size was not significantly associated with gender, socioemotional variables or behavioral problems.
Conclusion: Many toddlers with potential delayed speech-language were identified. They require further assessment and intervention, when indicated. Appropriate language screening strategies should be implemented in the childhood health supervision visits. Comprehensive studies of functional use of language for communication, discrimination and production of speech sounds and acquisition of reading and writing skills are greatly needed in our region.
Keywords
Childhood vocabularies, Language-rich interactions, Social interactions, Neurodevelopment, Language disorders.
Introduction
The United Arab Emirates (UAE) is a rapidly developing country, with most families having foreign caretakers who are heavily involved in their children’s care. With most parents working full-time and, as a result, employing foreign helpers, the Arabic mother tongue-language might be conveyed less efficiently to infants and toddlers. Thus, for many of these preschool children, the first language is obscured and the sociolinguistic identity is unclear [1]. Furthermore, language screening is not routinely implemented in the childhood health supervision visits. Consequently, environmental influences on language development and specific language disorders are usually not discovered until children enter school.
Language development in Emirati toddlers has previously been investigated [2].
About 10% of the studied children had delays in the language domain of the Denver Developmental Screening Test. Language delay was associated with rural living, noninvolvement of child caretakers, family history of language delay, perinatal complications and Behavioral problems in the child [2].
Verbal communicative disabilities may impair learning and predispose affected children to later socioemotional and behavioral problems such as anxiety, social withdrawal, aggression, attention deficit/hyperactivity and emotional dysfunction [3,4]. Although clinicians are responsible for early surveillance, assessment and management of language delays and disorders, a comprehensive speech-language assessment is expensive and requires special expertise. Therefore, preschool children screening tools for language acquisition, based on caregivers’ input, are currently commonly used. The Language Development Survey (LDS), an instrument based on parent reports of acquired vocabularies and word combinations, serves as a quick and reliable measure of vocabulary size and length-of-phrases for 18-35 month-old children [5-7].
In this study, we used the LDS to report on these variables (vocabulary size and length-of-phrases) in toddlers and correlate them with socioemotional and behavioral outcomes. The primary aim was to screen for early speech-language delays in the community. The secondary aim was to validate the LDS by examining its psychometric properties on linguistically-specific and culturally-appropriate receptive and expressive Arabic language scales. Our hypothesis was that local environmental factors, such as cultural characteristics, exposure to several languages, adversely influence the language development in infants and toddlers.
Methods
In this cross-sectional, community-based study, we used validated Arabic versions of the Language Development Survey (LDS) and Child Behavior Checklist for ages 1.5-5 (CBCL/1.5-5) screening tools (completed by parents in the presence of trained staff) [5-7]. The English questionnaires were translated into Arabic and back-translated to English to verify the accuracy of the conversion (Appendix 1). The Arabic version was slightly modified to reduce dialect variations. It included 310 words (arranged in 14 semantic categories).
Emirati families with children between 18 and 35 months of age who presented to the Ambulatory Health Services (Abu Dhabi) for a health supervision visit between October 2015 and June 2016 were recruited. With an estimated prevalence of delayed language in Emirati children of about 10%, a sample size of at least 140 participants was calculated to give the study adequate power with a 95% confidence level (Open Epi version 3.0). The study was approved by the Medical Ethics Committees for Human Research of the Al Ain Medical District (College of Medicine and Health Sciences) and the Ambulatory Health Services (Health Authority of Abu Dhabi). Written, informed consent was obtained from the primary caregivers and anonymity was assured.
Parents documented each word and phrase that the child said spontaneously. The five longest and best phrases or sentences pronounced by the child were recorded. Parents also reported the birthweight, any history of prematurity, ear infection, number of languages spoken at home, family language delay and any concern they had about their child’s language.
Children were evaluated for word size (number of expressive vocabularies), length of phrases (word combinations) and problem behaviors. The approach taken in developing the adapted LDS and its corresponding cutoff scores was the same as in previous studies. A vocabulary size fewer than 20 words at 18-23 months or fewer than 50 words at 24-35 months was defined as delayed language. Less than 2 word spontaneous phrases at 24-35 months were also considered abnormal [5-7].
Statistical analysis
Negative binomial regression with log link and the child’s age as an offset variable was used to investigate the relationship between vocabulary scores (response), CBCL syndromes and other characteristics (predictors), while controlling for the effects of age on vocabulary scores. Differences between mean word counts in males and females within each semantic category and age group were tested using the Mann- Whitney test because of the small sample sizes and lack of normality (Shapiro-Wilk test). The Pearson chi-square test was used to study relationships between language delays and risk factors, as well as with CBCL syndromes. For all statistical analysis, significance was defined by a 2-tailed p<0.05. All factors associated with language delay with a p-value <0.1 were subsequently entered in a logistic regression model. Only the associations with a p-value<0.05 in that model were considered statistically significant and their odds ratio (OR) with 95% confidence intervals (ci) were calculated.
Results
One hundred eighty-four 18-35 month-old children were enrolled in this study.
Eighteen (9.9%) children were excluded because of missing essential data (e.g., age) and 14 (7.6%) for being non-UAE citizens. All remaining 152 (82.6%) children were included in the analysis; their characteristics are shown in Table 1. Sixty-nine (45%) children were living in urban, 56 (43%) in semi-urban and 18 (12%) in rural areas. The mothers of 69 children (45%) were homemakers and those of 83 (55%) children were employed. As the majority of the families had one or more caretakers, it was not possible to ascertain the proportion of children raised exclusively by their mother. There was no significant difference in the vocabulary size according to the source of information (p=0.4). Three or more bouts of ear infections were associated with lower vocabulary size (p=0.066). Otherwise, gender (p=0.3), history of prematurity, or family history of delayed language had insignificant effects on the vocabulary size.
| Gender, No. of children (%) Females Males |
80 (53) 72 (47) |
|---|---|
| Age in months, mean ± SD (range) | 26.0 ± 4.9 (18-35) |
| Age groups, No. of children (%) 18-23 mo 24-29 mo 30-35 mo |
54 (35.5) 50 (32.9) 48 (31.6) |
| Informants Mothers Fathers Other primary caregivers |
71% 3% 26% |
| History of prematurity, No. of children (%) No Yes |
126 (85.1) 22 (14.9) |
| Birthweight, No. of children (%) <2000 g 2000-2400 g =2500 g Unspecified |
5 (3.3) 33 (21.7) 85 (55.9) 29 (19.1) |
| History of ear infection, No. of children (%) One Two Three |
111 (81.0) 19 (13.9) 7 (5.1) |
| Problem behavior, No. of children (%) Any symptoms Internalizing symptoms Externalizing symptoms |
43 (28.3) 26 (17.1) 10 (6.6) |
| Family history of language delay, No. of children (%) No Yes |
126 (84.0) 24 (16.0) |
| Mothers’ employment status, No. of mother (%) Homemakers Teachers Students Healthcare Unspecified workforce |
69 (45.4) 13 (8.6) 6 (3.9) 4 (2.6) 60 (39.5) |
| Fathers’ employment status, No. of father (%) Police Government sectors Engineers Retirements Unspecified workforces |
48 (31.6) 35 (23.0) 5 (3.3) 2 (1.3) |
Table 1. Sample characteristics (N=152).
Distribution of the vocabulary size by age group is shown in Table 2. For 18-23 month old children, the prevalence of a vocabulary size ≥ 20 words was 56% and for ≥ 50 words 28%. For 24-29 month old children, the prevalence of a vocabulary size ≥ 20 words was 76% and for ≥ 50 words 48%. For 30-35 month old children, the prevalence of a vocabulary size ≥ 20 words was 75% and for ≥ 50 words 46% (Table 2).
| Â = 20 words | = 50 words | |
|---|---|---|
| 18?23 mo (n=54) | 30 (56) | 15 (28) |
| 24?29 mo (n=50) | 38 (76) | 24 (48) |
| 30?35 mo (n=48) | 36 (75) | 22 (46) |
Values are number (%) of children.
Table 2. Distribution of the vocabulary size by age group (N=152).
| Vocabulary size <50 words ONLY | 18 (36) |
|---|---|
| Less than 2-word phrases ONLY | 2 (4) |
| Vocabulary size <50 words PLUS <2-word phrases | 3 (6) |
| Total | 23 (46) ** |
Values are number (%) of children
* These children had data on both vocabulary size and average length-of-phrases; their mean (SD) age was 29 (3) mo
** The remaining 27 (54%) children spoke = 50 words and had an average (SD) length-of-phrases of 3.9 (1.1), median = 4.0 and range=2.0-6.0.
Table 3. Prevalence of delayed language in children 24-34 mo (N=50)*
Fifty 24-34 month old children had available data on both vocabulary size and average length-of-phrases; their mean (SD) age was 29 (3) months. The prevalence of delayed language in these children is shown in Table 3. Eighteen children (36%) had a vocabulary size <50 words, two (4%) were not combining words and three (6%) had both limitations (Table 3). These 23 (46%) children require further assessment and possible intervention. The remaining 27 (54%) children spoke ≥ 50 words and had an average (SD) length-of-phrases of 3.9 (1.1), median=4.0 and range=2.0-6.0.
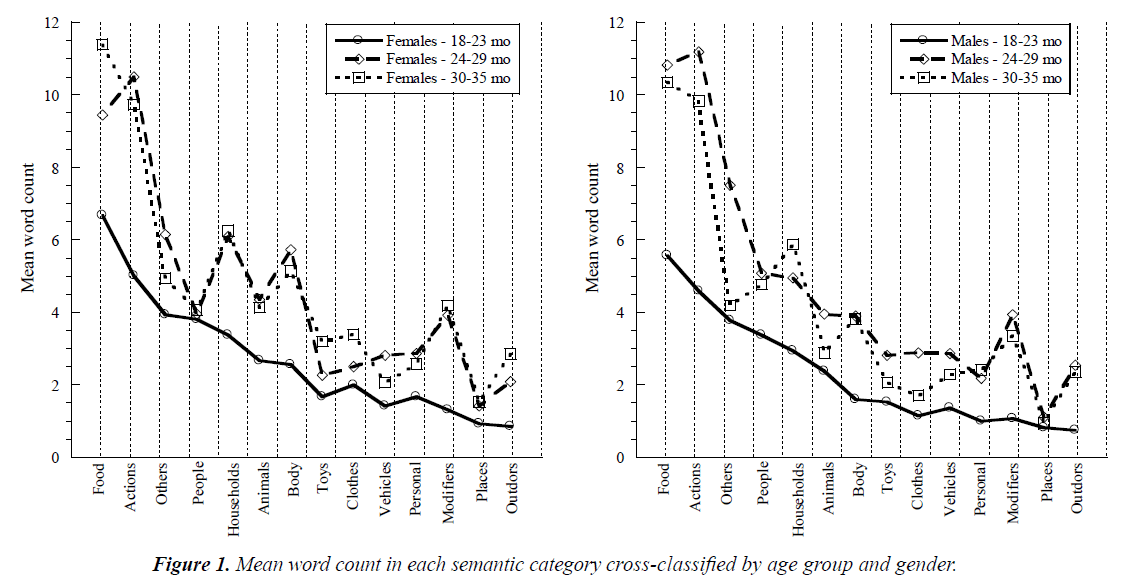
Most children used limited word types with only 22% using all 14 tested semantic categories. In all age groups, and in both genders, the highest number of words related to nonliving (inanimate) objects and the lowest related to outdoor items (Table 4 and Figure 1). In the 24-29 month age group all word counts were increased, with no significant differences between males and females. In all age groups, the vocabulary size was significantly higher in females than in males for body parts (p=0.05), places (p=0.064) and clothes (p=0.08).
Twenty-nine percent of children were exposed at home to languages other than Arabic. The proportion of children with delayed language decreased with exposure to more foreign languages but the difference was not statistically significant (Table 5). Delayed language was significantly more prevalent (p=0.007) in children living in semi-urban areas (64%) or rural (55%) than in those living in an urban environment. In the multivariate logistic model, living outside an urban environment (OR 1.98, 95% ci 1.16, 3.38, p<0.01) and exposure to fewer languages spoken at home (OR 2.3, 95% ci 1.05, 5.05, p<0.03) remained significant independent factors for language delay. There were no significant relationships between problem behaviors and vocabulary size (Tables 6-8), although borderline and abnormal cases had higher vocabulary size than normal cases in all syndromes, except in the autism spectrum.
| Non-living names | Living names | Verb actions | Others | Body parts | Modifiers | Outdoors | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Â F | M | F | M | F | M | F | M | F | M | F | M | F | M | |||||||||
| 18?23 mo (N=54) |
17.7 | 14.3 | 6.5 | 5.7 | 5.0 | 4.6 | 3.9 | 3.8 | 2.6 | 1.6 | 1.3 | 1.1 | 0.9 | 0.7 | ||||||||
| 24?29 mo (N=50) |
27.4 | 27.6 | 8.3 | 9.0 | 10.5 | 11.2 | 6.1 | 7.5 | 5.7 | 3.9 | 3.9 | 3.9 | 2.1 | 2.5 | ||||||||
| 30?35 mo (N=48) |
30.4 | 25.6 | 8.2 | 7.6 | 9.7 | 9.8 | 4.9 | 4.2 | 5.1 | 3.8 | 4.2 | 3.4 | 2.8 | 2.4 | ||||||||
Table 4. Mean word count in each semantic category cross-classified by age group and gender (N=152).
| Number of languages other than Arabic | Normal language | Delayed language | Total |
|---|---|---|---|
| 0 | 56 (75.7) | 52 (66.7) | 108 (71.0) |
| 1 | 15 (20.3) | 25 (32.0) | 40 (26.3) |
| 2 | 3 (4.0) | 1 (1.3) | 4 (2.6) |
p=0.17 (Chi square test).
Table 5. Number (percentage) of children with delayed language as a function of number of spoken languages at home in the 152 surveyed children.
| Behavior Syndromes | Females | Males | P (1) | |||
|---|---|---|---|---|---|---|
| N (%) | Mean (SD) | N (%) | Mean (SD) | |||
| Oppositional Defiant | Normal | 77 (96.3) | 56.2 (51.8) | 70 (97.2) | 50.3 (50.0) | 0.790 |
| Borderline/Abnormal | 3 (3.8) | 49.3 (51.7) | 2 (2.8) | 75.5 (2.1) | ||
| Externalizing | Normal | 75 (93.8) | 56.5 (52.3) | 67 (93.1) | 47.9 (45.8) | 0.458 |
| Borderline/Abnormal | 5 (6.2) | 45.0 (40.4) | 5 (6.9) | 92.6 (80.4) | ||
| Attention Deficit/Hyperactivity | Normal | 75 (93.8) | 54.6 (51.1) | 68 (94.4) | 49.9 (47.6) | 0.471 |
| Borderline/ Abnormal | 5 (6.2) | 74.2 (58.9) | 4 (5.6) | 70.0 (82.9) | ||
| Internalizing | Normal | 66 (82.5) | 54.5 (49.1) | 60 (83.3) | 49.9 (49.8) | 0.664 |
| Borderline/Abnormal | 14 (17.5) | 62.2 (63.1) | 12 (16.7) | 56.7 (49.4) | ||
| Depressive | Normal | 72 (90.0) | 56.4 (52.1) | 64 (88.9) | 46.8 (46.9) | 0.355 |
| Borderline/Abnormal | 8 (10.0) | 50.6 (48.5) | 8 (11.1) | 84.9 (59.7) | ||
| Anxiety | Normal | 67 (83.8) | 53.9 (49.0) | 57 (79.2) | 47.6 (47.2) | 0.329 |
| Borderline/Abnormal | 13 (16.2) | 65.9 (63.9) | 15 (20.8) | 64.1 (57.0) | ||
| Autism Spectrum | Normal | 66 (82.5) | 57.4 (50.4) | 64 (88.9) | 50.5 (48.7) | 0.796 |
| Borderline/Abnormal | 14 (17.5) | 48.2 (57.6) | 8 (11.1) | 54.8 (58.8) | ||
| Any Syndrome | Normal | 56 (70.0) | 56.8 (50.1) | 53 (73.6) | 46.8 (46.1) | 0.644 |
| Borderline/Abnormal | 24 (30.0) | 53.6 (55.5) | 19 (26.4) | 62.8 (57.5) | ||
Table 6. Relationship between problem behavior and gender (factors) vs. vocabulary size (response).
(1) Likelihood ratio test from the negative binomial regression with log link and age as offset and where the total vocabulary count is the response and behavior syndrome and genders the factors
| 18-23 mo | Age Groups 24-29 mo | 30-35 mo | P (2) | |||||
|---|---|---|---|---|---|---|---|---|
| N (%) | Mean (SD) | N (%) | Mean (SD) | N (%) | Mean (SD) | |||
| Oppositional Defiant | Normal | 51 (94.4) | 34.7 (32.8) | 48 (96.0) | 63.8 (57.3) | 48 (100.0) | 62.6 (55.0) | 0.278 |
| Borderline/Abnormal | 3 (5.6) | 37.7 (31.6) | 2 (4.0) | 93.0 (22.6) | 0 (0.0) | - | ||
| Externalizing | Normal | 51 (94.4) | 35.3 (33.3) | 45 (90.0) | 60.2 (53.3) | 46 (95.8) | 63.9 (55.6) | 0.299 |
| Borderline/Abnormal | 3 (5.6) | 27.3 (9.0) | 5 (10.0) | 107.8 (73.2) | 2 (4.2) | 33.5 (34.6) | ||
| Attention Deficit/Hyperactivity | Normal | 53 (98.1) | 34.8 (32.8) | 46 (92.0) | 63.4 (54.5) | 44 (91.7) | 62.0 (55.1) | 0.377 |
| Borderline/Abnormal | 1 (1.9) | 38.0 (-) | 4 (8.0) | 83.3 (84.1) | 4 (8.3) | 70.0 (62.3) | ||
Internalizing |
Normal | 44 (81.5) | 33.0 (30.4) | 40 (80.0) | 62.4 (53.4) | 42 (87.5) | 62.9 (56.7) | 0.378 |
| Borderline/Abnormal | 10 (18.5) | 43.2 (41.1) | 10 (20.0) | 75.4 (73.0) | 6 (12.5) | 60.8 (45.7) | ||
| Depressive | Normal | 49 (90.7) | 34.1 (33.1) | 46 (92.0) | 60.0 (53.2) | 41 (85.4) | 64.0 (56.9) | 0.233 |
| Borderline/Abnormal | 5 (9.3) | 42.6 (26.9) | 4 (8.0) | 122.5 (69.6) | 7 (14.6) | 54.4 (45.3) | ||
| Anxiety | Normal | 46 (85.2) | 32.0 (30.1) | 40 (80.0) | 58.9 (49.4) | 38 (79.2) | 65.7 (57.3) | 0.185 |
| Borderline/Abnormal | 8 (14.8) | 51.5 (42.1) | 10 (20.0) | 89.6 (77.3) | 10 (20.8) | 51.0 (45.7) | ||
| Autism Spectrum | Normal | 44 (81.5) | 34.8 (34.6) | 42 (84.0) | 63.6 (51.8) | 44 (91.7) | 64.2 (55.0) | 0.959 |
| Borderline/Abnormal | 10 (18.5) | 35.3 (21.9) | 8 (16.0) | 72.4 (81.1) | 4 (8.3) | 45.3 (60.5) | ||
| Any Syndrome | Normal | 39 (72.2) | 32.9 (32.1) | 35 (70.0) | 59.3 (48.7) | 35 (72.9) | 65.8 (56.5) | 0.493 |
| Borderline/Abnormal | 15 (27.8) | 40.0 (33.9) | 15 (30.0) | 78.4 (71.6) | 13 (27.1) | 54.2 (51.8) | ||
Table 7. Relationship between problem behaviors (factor) vs. vocabulary size (response) in the studied age groups.
Discussion
In this screening survey of toddlers for a spoken language delay, there were no significant differences between females and males with respect to most semantic categories (Table 4), vocabulary size, length-of-phrases or problem behaviors (Table 6). Many children ≥ 24 months had a vocabulary size <50 words and were not using word combinations (Tables 2 and 3). These potential linguistic delays were not significantly related to problem behaviors (Table 8); this probably reflects yet undetermined environmental variables. Nevertheless, the results justify implementing routine language screening in all childhood clinic visits [8-10]. Language development predicts the child’s intellect, while language difficulty correlates with learning problems [11]. These essential receptive (comprehension) and expressive (production) skills rely on information collected from hearing and other vital commands.
| Language Development | P (2) | ||||
|---|---|---|---|---|---|
| Delayed N (%) |
Normal (1) Â N (%) |
Both Groups N (%) | |||
| Oppositional Defiant | Normal | 67 (53.2) | 59 (46.8) | 126 (100.0) | 0.390 |
| Borderline/Abnormal | 11 (42.3) | 15 (57.7) | 26 (100.0) | ||
| Externalizing | Normal | 75 (52.8) | 67 (47.2) | 142 (100.0) | 0.201 |
| Borderline/Abnormal | 3 (30.0) | 7 (70.0) | 10 (100.0) | ||
| Attention Deficit/Hyperactivity | Normal | 73 (53.7) | 63 (46.3) | 136 (100.0) | 0.115 |
| Borderline/Abnormal | 5 (31.2) | 11 (68.8) | 16 (100.0) | ||
| Internalizing | Normal | 67 (54.0) | 57 (46.0) | 124 (100.0) | 0.209 |
| Borderline/Abnormal | 11 (39.3) | 17 (60.7) | 28 (100.0) | ||
| Depressive | Normal | 75 (52.4) | 68 (47.6) | 143 (100.0) | 0.318 |
| Borderline/ Abnormal | 3 (33.3) | 6 (66.7) | 9 (100.0) | ||
| Anxiety | Normal | 77 (52.4) | 70 (47.6) | 147 (100.0) | 0.201 |
| Borderline/Abnormal | 1 (20.0) | 4 (80.0) | 5 (100.0) | ||
| Autism Spectrum | Normal | 67 (51.5) | 63 (48.5) | 130 (100.0) | 1.000 |
| Borderline/Abnormal | 11 (50.0) | 11 (50.0) | 22 (100.0) | ||
| Any Syndrome | Normal | 59 (54.1) | 50 (45.9) | 109 (100.0) | 0.285 |
| Borderline/Abnormal | 19 (44.2) | 24 (55.8) | 43 (100.0) | ||
(1) >20 words for 18-23 mo and >50 words for 24-35 mo
(2) Pearson chi-square test .
Table 8. Language development vs. problem behaviors.
Our results also show a higher prevalence of language delay than other reports. Differences between the original survey in English and the validated Arabic translation that we used might explain this. Using a concurrent survey in English would have helped clarify this possibility but unfortunately, this was not possible as none of the toddlers and a significant proportion of their parents/carers did not speak English. Another possible reason for the observed prevalence is the possible existence of a linguistically-specific environment in this community. For example, 71% of the enrolled children are exposed only to Arabic language spoken at home, a factor significantly associated with language delay. Contrary to our hypothesis, it seems, therefore, that exposing children to more than one language spoken at home results in a lower prevalence of language delay.
Epidemiologic studies in the United States have shown a prevalence of primary language delay in 18-23 month old children of 13% and in that 30-36 month old of 17%. These frequencies were higher in males, preschool children, twins and in the presence of a family history of delayed language [5-6]. One Chinese study in preschool children identified a delay in verbal comprehension in 4.0%, expressive language in 2.8% and both domains in 3.3% [12].
Known risk factors associated with language impairment are numerous and include hearing deficit, ear infections, atopy, prematurity, problem behaviors and emotional disorders [11,13,14]. Children with these conditions require more frequent language assessment and perhaps referral to a speech-language specialist. This study identified frequent ear infections, an easily treatable condition, as a risk factor associated with lower vocabulary size (p=0.066). Children with recurrent or chronic ear infections may, therefore, require more frequent hearing assessments.
We found no significant effect on the vocabulary size of gender, problem behaviors, prematurity or family history of language delay. This could be explained by the limited number of children who were premature or had family members with language delay (Table 1). In contrast, the lack of a significant association between problem behavior and vocabulary size could be attributed to difficulties in diagnosing these disorders, such as autism, in preschool children. Future studies with much larger sample sizes and wider age limits are needed to explore the effects of these important variables, including gender, on early language acquisition in Emirati toddlers.
Unfortunately, the percentage of children having >50 words did not adequately increase with age (Table 2). The expected language development may have been halted in these growing children, resulting in a lack of improved vocabulary size with increasing age. Another pattern of language delay was observed in the types of acquired vocabularies (Table 4). Spontaneous phrases, involving word combinations of genuine meaning, is a pivotal ‘syntax’ function which emerges in children ≥ 24 months of age, when they acquire >50 words in their memory [15]. Thereafter, language acquisition accelerates more rapidly and serves to describe effectively objects and people (Figure 1). In this study, most children used limited types of words and only 22% used all 14 tested semantic categories. Names for inanimate objects were more common than those for outdoor items, which might reflect the community’s preference for an indoor lifestyle due to the outdoor elevated temperature and humidity.
We recognize that recurrent ear infections may impair language development in young children if complicated by hearing impairment. Although all the children had normal neonatal hearing screen results, the hearing status of children who had ear infections was not routinely tested. This weakness in our study needs to be addressed in future similar surveys. Another limitation of this study is that the data were derived from a questionnaire (CBCL/1.5-5). Direct assessment of children’s language by a professional, such as a speech or language therapist would, undoubtedly [16]; have been preferable and more reliable. However, this option is very time- and resource-consuming for such a survey. Using a validated questionnaire which has been used extensively in many studies was, therefore, the optimal option for this study. Furthermore, this method allows comparison with the majority of previous studies that have used the same instrument.
Conclusion
Variations in childhood language acquisition are usually minimal and mostly reflect the complexity of individual languages. This study identified potentially significant early language problems in the UAE community. The implication of these findings on childhood learning requires thorough investigation. Our results justify establishing communitybased programs aiming at early detection of language impairment. Such services provide opportunities to improve the outcome of children with a preschool language delay and prevent later learning and behavioral problems. Although parental support is an important first step, care manager nurses have been shown to be effective in increasing patients’ health knowledge, self-management skills and readiness to make changes in health behaviors in patients with heart failure and diabetes [17]. The feasibility of adding such extra expertise to the medical team, as a link between physicians, parents and children, would improve the detection and intervention of speech-language problems [18].
Acknowledgement
We thank the participating families and AHS staff for their support of this work. We are also grateful to Mrs. Sania Al- Hamad for staff training, Fatema Al-Shibli and Gaya Al Badi for collecting data.
Conflicts of Interest and Source of Funding
This work was supported by the United Arab Emirate University and the Ambulatory Health Services of Abu Dhabi. For the remaining authors none were declared.
References
- Lori AA, Al-Ansari SH. Relations of some sociocultural variables and attitudes and motivations of young Arab students learning English as a second language. Psychol Rep. 2001;88:91-101.
- Eapen V, Zoubeidi T, Yunis F. Screening for language delay in the United Arab Emirates. Child Care Health Development. 2004;30:541-9.
- Poll GH, Miller CA. Late talking, typical talking and weak language skills at middle childhood. Learn Individ Differ. 2013;26:177-84.
- Eapen V, Mabrouk AA, Zoubeidi T, et al. Prevalence of pervasive developmental disorders in preschool children in the UAE. J Trop Pediatr. 2007;53:202-5.
- Rescorla L. The Language Development Survey: a screening tool for delayed language in toddlers. J Speech Hear Disord. 1989;54:587-99.
- Rescorla L, Alley A. Validation of the language development survey (LDS): A parent report tool for identifying language delay in toddlers. J Speech Lang Hear Res. 2001;44:434-45.
- Ivanova MY, Achenbach TM, Rescorla LA, et al. Preschool psychopathology reported by parents in 23 societies: Testing the seven-syndrome model of the child behavior checklist for ages 1.5-5. J Am Acad Child Adolesc Psychiatry 2010;49:1215-24.
- Lousada M, Ramalho M, Marques C. Effectiveness of the language intervention programme for preschool children. Folia Phoniatr Logop. 2016;68:80-5.
- Lugo-Neris MJ, Peña ED, Bedore LM, et al. Utility of a language screening measure for predicting risk for language impairment in bilinguals. Am J Speech Lang Pathol. 2015;24:426-37.
- Klee T, Carson DK, Gavin WJ, et al. Concurrent and predictive validity of an early language screening program. J Speech Lang Hear Res. 1998;41:627-41.
- Duff FJ, Reen G, Plunkett K, et al. Do infant vocabulary skills predict school-age language and literacy outcomes? J Child Psychol Psychiatry. 2015;56:848-56.
- V, Lee PW, Lieh-Mak F, et al. Language screening in preschool Chinese children. Eur J Disord Commun. 1992;27:247-64.
- Beaulieu-Poulin C, Simard MN, Babakissa H, et al. Validity of the language development survey in infants born preterm. Early Hum Dev. 2016;98:11-6.
- Edmunds SR, Ibañez LV, Warren Z, et al. Longitudinal prediction of language emergence in infants at high and low risk for autism spectrum disorder. Dev Psychopathol. 2016;6:1-11.
- Patterson JL. Observed and reported expressive vocabulary and word combinations in bilingual toddlers. J Speech Lang Hear Res. 2000;43:121-8.
- Conti-Ramsden G, Durkin K. Language development and assessment in the preschool period. Neuropsychol Rev. 2012;22:384-401.
- Ciccone MM, Aquilino A, Cortese F, et al. Feasibility and effectiveness of a disease and care management model in the primary health care system for patients with heart failure and diabetes (Project Leonardo). Vasc Health Risk Manag. 2010;6:297-305.
- McQuiston S, Kloczko N. Speech and language development: Monitoring process and problems. Pediatr Rev. 2011;32:230-8.