- Biomedical Research (2010) Volume 21, Issue 2
Review: The Prion and its Potentiality
Dipendra Raj Pandeya1, Nimish K. Acharya2 and Seong-Tshool Hong1*
1Laboratory of Genetics, Department of Microbiology and Immunology, Institute for Medical Science, Chonbuk Na-tional University Medical School, Chonju, Chonbuk 561-756, South Korea.
2University of Medicine and Dentistry of New Jersey (UMDNJ) - Graduate School of Biomedical Sciences, 2 Medical Center Drive, Stratford, NJ 08084, USA.
- *Corresponding Author:
- Seong-Tshool Hong
Laboratory of Genetics
Department of Microbiology and Immunology
Institute for Medical Science, Chonbuk National Univer-sity Medical School
Chonju, Chonbuk 561-756, South Korea
Phone/Fax: 82-063-270-3105
E-mail: seonghong@chonbuk.ac.kr
Abstract
A great deal of effort during the past 27 years has been devoted to defining the chemical nature of prions, the infectious agents responsible for transmissible spongiform encepha-lopathies. Prion diseases are fatal neurodegenerative disorders that can arise spontane-ously, be inherited, or be acquired by infection in mammals. They are unique not only in terms of their biological features but also in terms of their impact on public health. It has been hypothesized that in addition to Creutzfeldt - Jakob disease (CJD) in humans and Bovine Spongiform Encephalopathy (BSE) in animals, prions may also play a role in sev-eral other neurodegenerative diseases such as Alzheimer’s disease, Parkinson’s disease, amyotrophic lateral sclerosis, and frontotemporal dementia; however, the precise mecha-nism underlying prion-mediated neurodegeneration still remains elusive. In this review, we outline the physico-chemical characteristics of prions and their impact on human and animal health.
Keywords
Prion, prion diseases, bovine spongiform encephalopathy, neurodegeneration
Introduction
Prion disease (PD) is an untreatable and fatal neurodegenerative disorder that affects both humans and animals. Since various aspects of PD pathogenesis have not been conclusively delineated, PD remains an intriguing puzzle waiting to be solved. Transmissible spongiform encephalopathy (TSE) is the general term assigned to all known prion diseases.
PD is the new designation of a group of spongiform encephalopathies because of the histological appearances of large vacuoles in the cortex and cerebellum and all invariably fatal, which show similar clinical and neuropathological changes. TSEs in sheep and goat is known as Scrapie; in humans, they are known as Kuru, CreutzfeldtJakob disease (CJD), Gerstmann-Straussler-Scheinker syndrome (GSS) and fatal familial insomnia (FFI). Kuru has been described only in the Fore population of New Guinea. For many years after its first recognition in 1957 [1], Kuru was the most common cause of death among women in the affected population, but it is disappearing because of the cessation of ritualistic cannibalism that had facilitated disease transmission [2]. The term chronic wasting disease is used in mules, deer [3] and Rocky Mountain elk [4], bovine spongiform encephalopathy (BSE) or mad cow disease is used in cattle and feline spongiform encephalopathy in cats, albino tigers, pumas and cheetahs. With the exception of FFI, all of these disorders have been experimentally transmitted to nonhuman primates and laboratory rodents. Severe loss of neurons is a key characteristic for all prion diseases, accompanied by strong astrogliosis and mild microglia activation. This results in a progressive spongiform degeneration of the central nervous system (CNS) which manifests itself in ataxia, behavioral and, in humans, a highly progressive loss of intellectual abilities changes [5]. Though it was initially gestated to explain elusive neurodegenerative diseases in mammals, it has now grown to encompass a number of non-Mendelian traits in fungi [6, 7, 8].
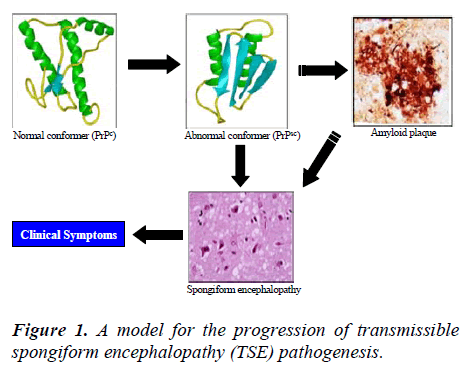
The mode of transmission appears to be novel; a protein agent rather than a particle containing nucleic acid is involved. However, the mechanism and propagation of PD still remain to be conclusively elucidated. Some key players associated with pathogenesis of the disease have been identified. The most important one is the protein agent that induces abnormal refolding of the normal prion protein. Aggregation of these misfolded proteins leads to the formation of dense plaques and fibers known as amyloid. The deposition of amyloid consequently results in cell death and tissue damage in the brain and spinal cord. Spongiform changes are associated with neuronal loss during amyloid plaque formation; failure to elicit inflammatory responses is a major characteristic of degenerative tissue damage due to prion diseases (Fig.1). Most prions identified so far are self polymerized amyloids that form highly ordered cross-β fibrous aggregates. The yeast prion [PSI+] is a self-perpetuating amyloid of Sup35 [9], an evolutionarily conserved eukaryotic release factor that is required for the termination of translation [10, 11]. This review provides a basic understanding of the nature of prion proteins and highlights the etiology, replication, transmission and other clinical and pathologic features of these debilitating interesting diseases.
Prion disease
Prion diseases are rare and unusual neurodegenerative disorders of the nervous system caused by the accumulation of a misfolded form of the endogenous PrP; these diseases present ongoing threats to humans and animals [12, 13]. Much about TSE diseases remain unknown. The diseases are characterized by certain misshapen protein molecules that appear in brain tissue. Prion diseases result in progressive cognitive and motor impairment and are characterized by the accumulation of proteinaceous brain lesions or plaques [14]. Sheep scrapie was the first of to be recognized, but subsequently a set of human diseases including Kuru and CJD was shown to have similar clinical and pathological features. TSEs have now been identified in a wide range of mammals, including cats, cows, mink, deer and elk [15]. These diseases affect the structure of brain tissue and are all fatal and untreatable. Some of the distinctive features of TSEs include neuronal vacuolation (spongiosis), neuronal death, and glial reactions. In addition, a defining characteristic is the deposition of PrPsc, mainly in the brain and lymphoreticular tissues. Also, no adaptive immune responses are elicited upon infection, most likely because the mammalian immune system is largely tolerant to PrP from the same species. This is not surprising, given that many cells in neural and extraneural compartments express PrPc. Although TSEs are by definition transmissible, a growing number of Prnp-associated non-infectious, neurodegenerative proteinopathies are now also being recognized [16]. The only molecules thus far associated with infections are isoforms of PrP. These transmissible agents appear to have a common mechanism of pathogenesis and possibly a common origin. Some have spread across species barriers (transmissible mink encephalopathy and possibly newvariant CJD); some have reached epidemic proportions by entering the food chain (transmissible mink encephalopathy, bovine spongiform encephalopathy, and Kuru); and others have been inherited due to mutations in the PrP gene (familial CJD, GSS and FFI) [17]. Recent evidences suggest a role for the ubiquitin proteasome system (UPS) in prion disease. Both wild-type PrPc and disease associated PrP isoforms accumulate in cells after proteasome inhibition leading to increased cell death and abnormal β-sheet-rich PrP isoforms have been shown to inhibit the catalytic activity of the proteasome [18]. The hallmark feature common to all prion diseases, whether sporadic, dominantly inherited or acquired by infection, is that they involve aberrant metabolism of the prion protein.
The Prion Hypothesis
The nature of the agents responsible for TSEs has been the focus of intense scrutiny and considerable debate over the last few years. Research on the molecular genetics of PrP protein has contributed greatly to our knowledge of these diseases [19]. The observation that the scrapie agent was resistant to procedures that inactivate or modify nucleic acids, but sensitive to treatments that denature proteins, led to speculation that the agent could be a self-replicating protein devoid of nucleic acids [20]. Based on these events, Stanley Prusiner in 1982 hypothesized the existence of a novel class of infectious agents, which he named prions [21]. Specifically, it was hypothesized that the scrapie agent was a proteinaceous infectious particle because infectivity was dependent on proteins and resistant to methods known to inactivate nucleic acids [22]. A similar proposal was presented more than a decade earlier by Gibbons and Hunter [23] and Griffith and Levine [24], who used irradiation to demonstrate that the scrapie agent was devoid of disease-specific nucleic acid. The alternative virion hypothesis is not a conventional viral hypothesis but rather addresses the diversity of biological properties of TSEs. This hypothesis states that TSEs are caused by a replicable, informational molecule (likely to be a nucleic acid) bound to PrP. Many TSEs, including scrapie and BSE, show strains with specific and distinct biological properties; this feature, according to supporters of the virion hypothesis, is not explained by prions.
No mechanism has yet been proposed that can satisfactorily explain how the PrP protein alone could specify and retain multifactorial TSE strain characteristics. On the other hand, the virino hypothesis [25, 26] proposes the existence of a small, host-independent, informational molecule encoding strain-specific information that is bound to and protected by a host protein, PrP. This fulfills the requirements of all biological experimental evidence obtained and is compatible with the biophysical and bio-chemical data [27].The molecular structure of the agent is still undetermined, but there is now enough evidence to formulate testable hypotheses. For example, de novo production of infectivity [28] in a test tube by experimental manipulation of recombinant or synthetic PrP has been clearly demonstrated. The absence of molecular structural data does not invalidate the prion hypothesis but simply underscores the difficulty of extracellularly reconstituting this remarkable molecular transformation. However, additional studies are required to substantiate these claims or explain the strain diversity of prions that can lead to variable phenotypic disease expression.
Prion Protein (PrPc- PrPsc)
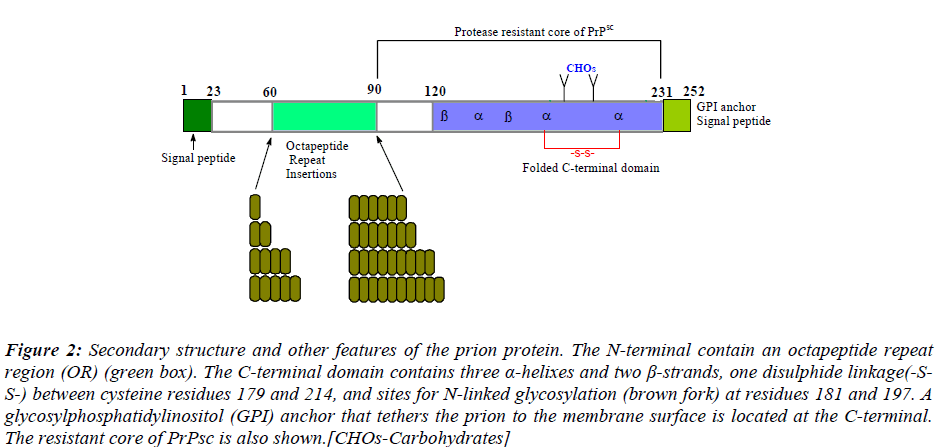
The prion protein is arguably one of the most extensively studied proteins. Prions are infectious pathogens that differ from bacteria, viruses and viriods in their structure and pathogenesis [29]. They contain information encoded in the shape of the prion protein molecule; this information is transmissible from one molecule to another. Studies of the scrapie agent, and more limited studies on prions in humans, indicate that these agents are resistant to treatments that inactivate nucleic acids and viruses (alcohol, formalin, ionizing radiation, proteases and nucleases) [30], but they are inactivated by treatments that disrupt proteins (autoclaving, phenol, detergents, and extremes of pH) [23]. From a broader view, prions are elements that impart and propagate variability through multiple conformations of a normal cellular protein. The cellular prion protein (PrPc) is a cell membrane bound glycoprotein with a molecular weight of 33-35 kDa present in various organs, it is especially abundant in the central nervous system (CNS). Little is known about the physiology of PrPc. The conformational counterpart of PrPc, PrPsc, is thought to be the cause of prion diseases, hence, by definition, standing for neurotoxicity and prion infectivity. This assumption has been challenged by several observations during the last decade. The disease-associated isoform of PrPsc is post-translationally derived from PrPc [31, 32]. PrPc is converted into PrPsc through a process in which a portion of its α-helical and coiled structure is refolded into a β-sheet [33]. PrPc is linked to the cell membrane by a glycosylphosphatidylinositol (GPI) anchor. It has either one or two sugar chains that are closely linked to the C-terminus; it also exists in an unglycosylated form (Fig. 2).
Figure 2: Secondary structure and other features of the prion protein. The N-terminal contain an octapeptide repeat region (OR) (green box). The C-terminal domain contains three a-helixes and two Ã-strands, one disulphide linkage(-S-S-) between cysteine residues 179 and 214, and sites for N-linked glycosylation (brown fork) at residues 181 and 197. A glycosylphosphatidylinositol (GPI) anchor that tethers the prion to the membrane surface is located at the C-terminal. The resistant core of PrPsc is also shown.[CHOs-Carbohydrates].
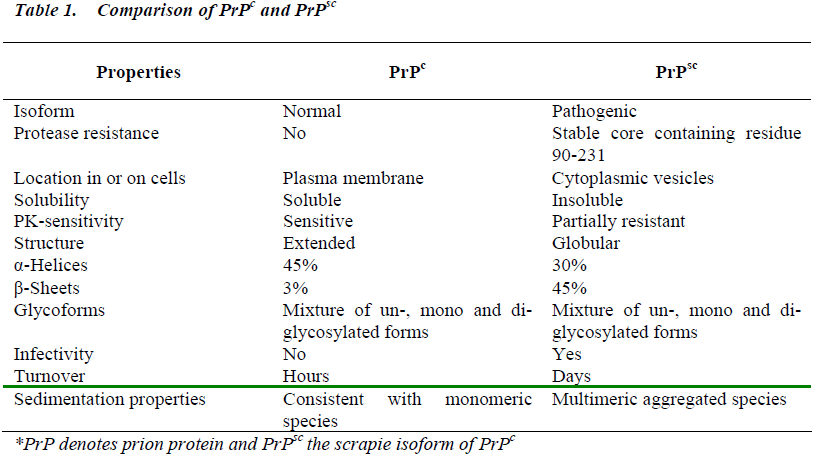
PrPc and PrPsc differ in their biochemical properties, with PrPsc being protease-resistant and detergent-insoluble (Table 1). Despite intensive investigation, no differences between the primary sequences or covalent modifications of these two isoforms have been found [34]. Rather, they are thought to differ in their three-dimensional conformation, with PrPsc having much higher β-sheet content than PrPc [35]. Circular dichroism spectrometry and infrared studies suggest that PrPc is composed of 42% α-helical and 3% β-sheet conformations, whereas PrPsc is composed of 30% α-helical and 43% β-sheet conformations [32]. The increased β-sheet content in PrPsc is due to the major conformational transition of the hydrophobic region (amino acid residues 90-140) and a portion of the helices in PrPc molecules. This molecular event makes the molecule hydrophobic and resistant to proteinase K (PK) digestion. The conformationally altered region in PrPsc is thought to form the repeated stretches of short β-sheets, and it can aggregate into multimers of PrPsc, which can become PrP amyloid fibrils [36]. A tertiary structure of PrPc, based on nuclear magnetic resonance spectroscopic analyses of recombinant PrP produced in bacteria, included a long, flexible N-terminal tail (residues 23 to 121), three α-helices, and two small antiparallel β-sheet strands that flanked the first α-helix [37, 38]. Molecular modeling studies predicted that PrPc is a four helix bundle protein containing four regions of secondary structure denoted by H1, H2, H3 and H4. The secondary structure is dominated by α-helices. Helices 2 and 3 are joined by a disulfide bond which maintains the original conformation. Although a tertiary structure of PrPsc has not yet been identified, current evidence suggests that generation of this iso-form involves primary changes in the N-terminal half of the protein, including folding of a portion of the N-terminal tail from residues 90 to 121 (and possibly part of the first α-helix) into a β-sheet. A key challenge in the field is now to obtain a complete structure of PrPsc by spectroscopic and crystallographic techniques that would allow atomic level specifications of the PrPc conformation.
Expression and physiological function of Prion
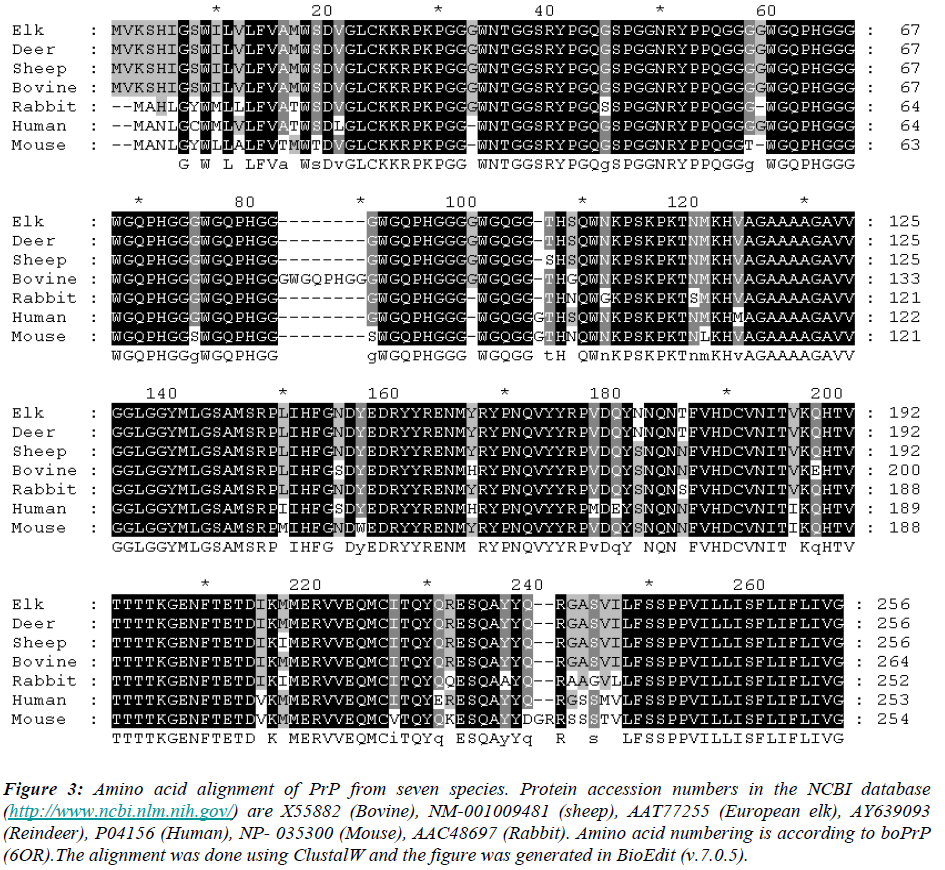
PrPc is a glycoprotein that is normally attached to the surface of neurons, especially to synaptic membranes, and glial cells of the brain and spinal cord in all mammals via a GPI anchor [39]. The expression pattern of PrPc is diverse and developmentally regulated in skeletal muscle, kidney, heart, secondary lymphoid organs and the CNS, suggesting a wide-ranging and conserved function of the protein [40, 41, 42, 43, 44]. Its expression in most tissues, together with its evolutionarily conserved amino acid sequence, supports a fundamental role for PrPc. As PrPc is most abundantly expressed in the brain, the loss of this protein is expected to result in substantial neurobehavioral modifications even though the specific role of PrPc in neural function and behaviour is still elusive [45]. The normal physiological role of PrPc remains enigmatic, although a number of roles have been proposed due to its remarkable conservation across species. However, studies of PrP-null mice have shown that it is not essential for viability, and various investigators have suggested that it may have a function in sleep regulation [46], cell adhesion [47], or Purkinje cell viability [48]. In vitro studies showing that PrP-/- neurons are extremely vulnerable to oxidative stress, and that PrPc has superoxide dismutase-1 (SOD-1)-like activity [49], have lead to the proposal that PrPc might have a role in cellular oxidative responses. It has been suggested that ablation of this antioxidant func-tion of PrPc might be associated with neurodegeneration in prion disease. There is evidence that the protein binds copper [50, 51] and may play roles in the trafficking of copper ions [52, 53] or protection from oxidative damage in the nervous system [54]. On the other hand, compelling evidence now suggests that PrPc has neuroprotective properties. It is upregulated upon ischemic brain damage [55], and in PrP deficient mice the infarct size is drasti-cally increased [56]. In addition, PrPc is able to protect against several proapoptotic stimuli [57], as well as longterm renewal in hematopoietic stem cells [58]. Besides its various functions, the amino acid sequences of human, bovine, sheep, deer, elk, rabbit and mouse prion proteins and found a great deal of similarity among them (Fig. 3). This homology across all mammalian prion protein sequences could facilitate the transmission of TSEs between species.
Figure 3: Amino acid alignment of PrP from seven species. Protein accession numbers in the NCBI database (http://www.ncbi.nlm.nih.gov/) are X55882 (Bovine), NM-001009481 (sheep), AAT77255 (European elk), AY639093 (Reindeer), P04156 (Human), NP- 035300 (Mouse), AAC48697 (Rabbit). Amino acid numbering is according to boPrP (6OR).The alignment was done using ClustalW and the figure was generated in BioEdit (v.7.0.5).
Prion Replication
The mechanism by which prion infectivity increases is still unknown, since the infectious agents do not contain nucleic acids. Information appears to be stored in the structure of the protein aggregates. Prion aggregates can grow by incorporating new prion protein and inducing a refolding into the pathological prion form. Growth of prion aggregates, however, is not enough for replication.
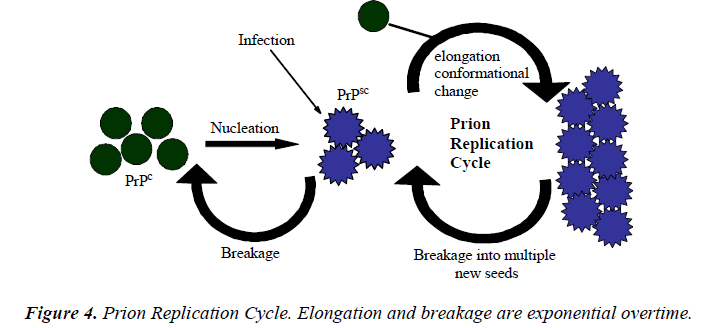
At some point, one prion must become two prions. The in vivo kinetics of elongation and breakage are exponential over time [59] and quite different from the in vitro kinetics of nucleation and growth (Fig. 4). Nucleation is a very rare process and can generally be ignored in vivo, since disease usually follows introduction of the infectious agent. Even if the disease arises spontaneously, intervention will always be too late to interfere with nucleation. Instead, we have focused on the exponential rate of growth. Since the process appears to be exponential, the posttranslational conversion of PrPc, or a precursor of PrPsc, may be obligatory [31]. A PrPsc molecule might combine with a PrPc molecule to produce a heterodimer that is subsequently transformed into other PrPsc molecules. In the next cycle, two PrPsc molecules combine with two PrPc molecules, giving rise to four PrPsc molecules, which then combine with four more PrPc molecules, creating an exponential process. Regarding the thermodynamic and kinetic analysis of prion replication and the replication cycle for the inherited, sporadic, and infectious scenarios, several inferences can be made about the bio-physical properties of the normal cellular and disease causing PrP isoforms.
PrPsc replication requires the presence of the gene in the host cell to direct PrPc synthesis. Although PrPsc replication requires a PrP gene in the host cell, this gene does not need to be carried by the infectious pathogen. Therefore, PrPsc must be more stable than PrPc, and a plausible origin for this distinction may be the extensive network of intramolecular interactions between PrP monomers in the PrPsc multimer. Protease resistance could be a corollary of this increased stability and not necessarily the cause of the increased metabolic stability of PrPsc [21].
Pathogenesis of prion disease
The pathogenesis of prion disease is also poorly understood. In peripheral infection, prions silently accumulate and replicate in peripheral organs or reservoirs and transit through at least one PrP-positive (PrP+) tissue before reaching the CNS. Prions indeed replicate in lymphoid organs during the early stages of infection [60]. Within the lymphoreticular system, follicular dendritic cells (FDCs) are a prominent site of PrPsc deposition [61], both in wild-type and nude mice (defective in T-cell responses).
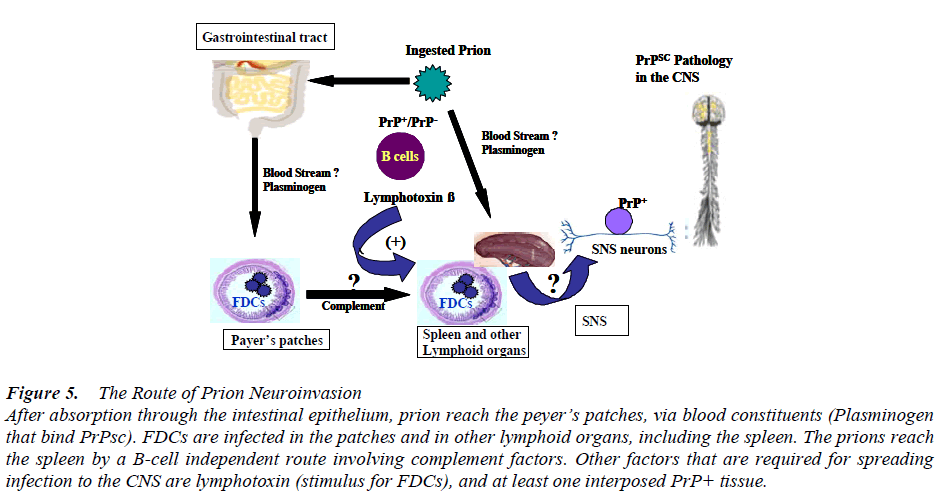
Thus, neuroinvasion typically begins upon ingestion of the TSE agent (Fig. 5). The pathogen must first cross the intestinal epithelium in a process that still remains elusive amid some data suggesting a mechanism involving transcytosis by microfold (M) cells [62]. Migratory dendritic cells are also known to directly capture antigens within the intestinal lumen and could also be responsible for initial uptake of the TSE agent. Once past the epithelial wall, PrP<sup>sc</sup> appears to be phagocytosed by antigen-displaying cells such as macrophages and dendritic cells. While macrophages appear to serve a more protective role [62], some experimental evidence suggests that dendritic cells deliver the TSE agent to follicular dendritic cells located in the germinal centers of B cell-rich follicles present in Peyer’s patches and other gut associated lymphoid tissue (GALT) underlying the intestinal epithelium. After incubation in lymphoid tissue such as the GALT and spleenthe TSE agent spreads to the central nervous system (CNS) via the enteric nervous system. A new study finds that tunneling nanotubes are important for the intracellular transfer of prion during neuroinvasion [63]. Prions gain access into and between neurons by hijacking tunneling nanotubes. Whereas previous studies have shown that prions can spread by other mechanisms, these are far less efficient. For example, transportation by exosomes re-quires 5 days of coculture, compared with 12 hours by nanotubes [64].
Figure 5: The Route of Prion Neuroinvasion After absorption through the intestinal epithelium, prion reach the peyer?s patches, via blood constituents (Plasminogen that bind PrPsc). FDCs are infected in the patches and in other lymphoid organs, including the spleen. The prions reach the spleen by a B-cell independent route involving complement factors. Other factors that are required for spreading infection to the CNS are lymphotoxin (stimulus for FDCs), and at least one interposed PrP+ tissue.
Although this is the most likely route for neuroinvasion, it has been suggested that blood may also play a role in the pathogenesis of prion diseases [65]. For example, a number of studies in animals have produced prion infections from inoculation of buffy coats and other blood components [66, 67]. These observations set the stage for a model of neuroimmune invasion that comprises two phases. The first phase is characterized by the widespread colonization of lymphoreticular organs by a mechanism that is dependent on B lymphocytes, follicular dendritic cells and additional factors such as complement [68]. The second phase requires expression of PrPc in peripheral sympathetic nervous system (SNS) nerves and results in prion dissemination in the CNS. Recently, the effectiveness of standard leukoreduction for removing TSE infectivity from whole blood was investigated [69]. The removal of all white cells reduced infectivity by only 42%, suggesting that other blood components, cells or plasma, could be infectious. These data, when considered together with animal studies of prion infectivity in blood, have highlighted both the significance of PrPc and the role of individual blood components in the pathogenesis of TSEs.
Etiology of prion diseases
Despite a lack of mechanistic knowledge, prion diseases are emerging as one of the best understood neurodegenerative disorders with respect to etiology and pathogenesis. The etiologic agent of TSEs was hypothesized to be a “slow virus” by Sigurdsson [70], in an effort to explain the transmissible nature and prolonged incubation period observed during experimental transmission studies [71]. The “slow virus” was indeed unconventional because it provoked no immune response in the host and was resistant to formalin, UV light and ionizing radiation treatments that normally destroy viruses [72]. Stanley Prusiner pursued this finding and eventually showed that a single protein, dubbed the prion protein, was consistently present in the infectious fraction and that surprisingly, this protein was encoded by a normal chromosomal gene of the host [73]. Sequencing of the prion protein gene (PRNP) was pivotal to understanding prion disease because it showed that mutations in this gene could give rise to CJD, as well as to two other conditions (GSS and FFI) not previously considered to be prion diseases. Subsequent studies by Prusiner et al. [74] demonstrated that a hydrophobic protein was an essential component of the scrapie agent, but no specific polypeptide was identified. To underscore the requirement of a protein for scrapie infectivity, Prusiner [21] introduced the term “prion” in 1982 to describe the proteinaceous infectious particle. In the same year, Prusiner et al. [75] and Bolton et al. [73] reported the purification of scrapie prion and demonstrated its relatively high resistance to PK treatment. Soon after the discovery of prions, a similarity with a normal cellular protein that is a structural component of cell membranes was identified. The neurotoxic form of PrP could represent distinct proteinaceous species, which is intermediate or byproduct of PrPc→PrPsc conversion pathway. The current understanding suggests a number of possible mechanisms to cell death in TSE diseases, including an increased level of NMDA receptor mediated excitation [76] and activation of Erk1/2 pathway [77].The generation of TSEs by prions in different species, or in some instances different disease phenotypes in the same species, suggested the existence of different prion “strains” [78]. Although neither the viral nor the protein only theory has been proven, evidence in favor of the protein-only hypothesis has overwhelmed the virus camp. Hence for better understanding of identity and structural characteristics of the neurotoxic form of PrP, more rigor-ous efforts are mandatory.
The Species Barrier
Passage of transmissible spongiform encephalopathies between species is often a stochastic process and may be limited by a species barrier. This barrier represents the decreased efficiency with which TSEs are passed from one animal to another animal of a different species, as compared to the efficiency of transmission among animals of the same species. In spite of centuries of exposure, sheep scrapie is not known to have been transmitted to humans, but bovine spongiform encephalopathy (BSE) has (fortunately only rarely) done so. The primary determinants of the species barrier are the sequences of the potential prion proteins of the two species. The transmis-sion of prions from one species to another requires prolonged incubation times, compared to intraspecies trans-mission; in some instances, the species barrier seems to confer complete resistance to transmission. Although transmission of a TSE from one species to another might be less efficient than transmission within the same species, once it occurs the TSE may become adapted to the new host. Following adaptation, it can be transmitted more efficiently among members of the new species, and the incubation period becomes shorter and less variable. For example, when scrapie is transmitted experimentally from one species to another, the incubation period is usually longer during the first passage than for subsequent pas-sages within the new species [79]. This is an important topic that is relevant to the debate over the possible transmission of BSE to man.
Species barriers in TSE diseases have been studied experimentally in several laboratory species including mice, rat, hamsters and non-human primates. From studies with transgenic mice, three factors have been identified that contribute to the species barrier: 1) the difference in PrP sequences between the prion donor and recipient, 2) the strain of prion, and 3) the species specificity of protein X, a factor that facilitates PrPsc formation by binding to PrPc. This factor is probably a protein, hence the provisional designation protein X [80, 81]. Even a single amino acid change in the PrP of the recipient can bring about a radical change in incubation times [82] or even result in resistance to disease. Since these classic studies were performed, several transgenic experiments have confirmed the intimate relationship between the sequence of the prion protein and specificity of transmission [83, 84]. None-theless, other studies established that in some contexts, it may not be the sole determinant.
Prion strains
One of the most puzzling phenomena in prion biology is the existence of prion “strains”. The prion “strain” concept originates from the multiple but distinct transmissible prion diseases that can be passed in the same inbred mouse lines despite their identical PrP-encoding genes. A remarkable feature of prion biology is the strain phenomenon, where prion particles apparently composed of the same protein lead to phenotypically distinct transmissible states. These strains have distinct neuropathologies, and differential rates of disease progression have provided evidence of discrete subtypes of TSEs [85]. The existence of prion strain was first discovered during the transmission of scrapie among goats [86]. Different prion strains are characterized by length of incubation period of disease, the distribution of CNS vacuolation that they produced, and whether or not prion deposits formed. Different strains frequently associated with PrPsc species show dis-tinct physical features such as susceptibility to PK digestion, stability toward denaturing agents, proportions of dimono-, and unglycosylated forms and differential electrophoretic mobility following PK treatment; this reflects diversity at the aminoterminus that results in multiple cleavage sites. These observations taken together begin to build an argument for PrPsc as the information molecule in which prion strain-specific information is encrypted. Deciphering the mechanisms by which PrPsc carries in-formation for prion diversity and passes it on to the nascent prions is a challenge. Whether PrPsc can adopt multiple conformations, each with a distinct incubation time and pattern of PrPsc deposition, remains to be determined [87]. The existence of different prion strains casts a shadow on the protein-only hypothesis. The prion strains and species barriers in prion transmissibility appear to be in-tricately related, representing two sides of the same coin. While cross-species transmission often results in faithful propagation of the inoculating strain, in some cases it can result in strain switching, as observed in animal studies [88], yeast prion systems [16], and other in vitro experiments [89]. The exact mechanism by which strain switching occurs is still not clear. The existence of the strain phenomenon is not only a scientific challenge, but it also represents a serious risk for public health. The dynamic nature and inter-relations between strains and the potential for the generation of many new prion strains depending on the polymorphisms and the crossing of species barrier is the perfect recipe for the emergence of extremely dangerous new infectious agents [90].
Interaction of PrPc with other proteins
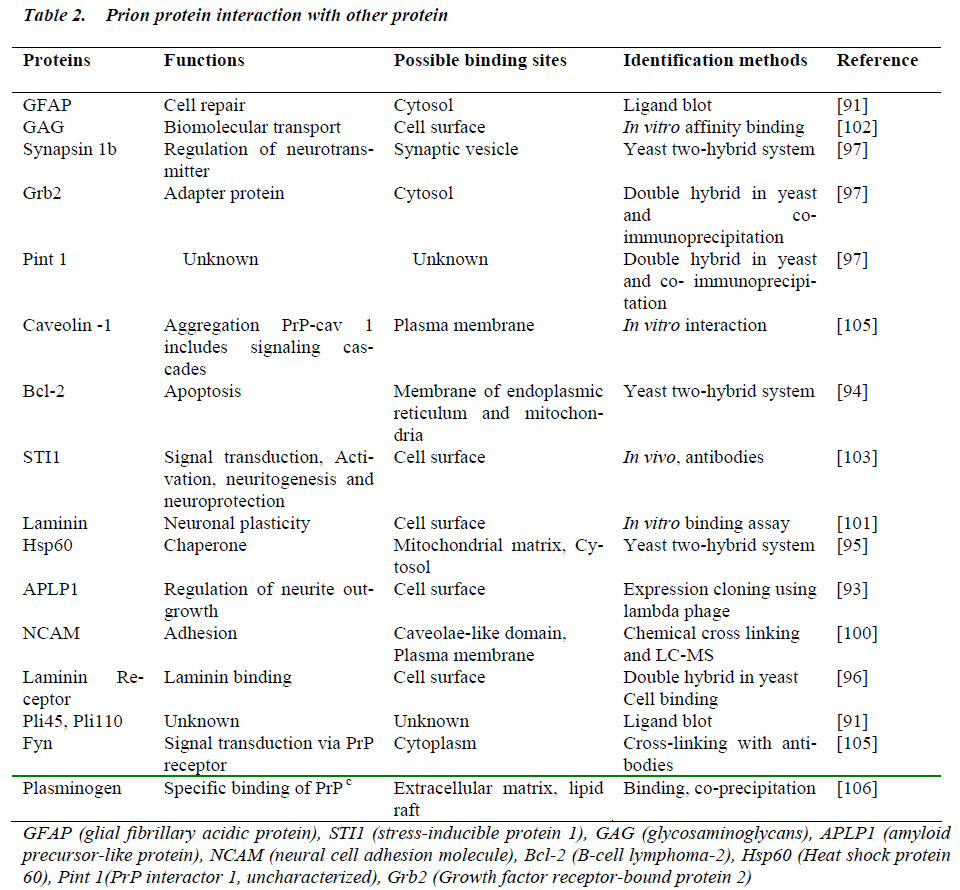
PrPc interacts with a large number of proteins. In order to investigate the transformation of PrPc into PrPsc, possible interactions with other protein candidates were identified (Table 2). The first interacting proteins identified were a pair of prion protein ligands, Pli45 and Pli110 [91]; the former is a glial fibrillary acidic protein (GFAP), a marker for astrocytes that proliferate in response to TSE infec-tions [92]. Later on, other prion protein ligands, including Pli3, Pli4, Pli5, Pli6, Pli7 and Pli8, were identified using the PrP-alkaline phosphatase screening method [93]. Sub-sequently, a number of PrPc -interacting proteins have been identified using a yeast two-hybrid system: these include the anti-apoptotic protein Bcl-2 [94], the cellular chaperone heat shock protein 60 (Hsp60) [95], the 37 KDa laminin receptor precursor [96], the synaptic vesicle marker synapsin1b, the adaptor protein Grb2 and the prion interaction protein, for which no function has been determined [97]. In addition to Hsp60, other chaperones such as Hsp73 and GroEL can interfere with α to β conversion of prion, while chaperones such as Hsp70 have no role in the PrP conversion [98]. PrPc also binds to laminin in PC12 cells and rodent primary neurons, and this interaction promotes neurite outgrowth in these cells [99]. A number of additional cell surface proteins interact with PrPc including neuronal cell adhesion molecules (N-CAMs) [100], apolipoprotein 1 (an amyloid precursor protein that has been implicated in Alzheimer’s disease), the 67 KDa laminin receptor [101] and Glycosaminogly-cans (GAGS) [102]. The complementary hydropathy, a technique in which cDNA is used to generate a complementary mirror image of the target protein, identified that the 66 KDa stress inducible protein STI-1 binds to PrPc and might be involved in neuroprotection [103].
The list of putative PrPc binding partners is equally long; some of these cellular cofactors have been suggested to contribute not only to normal PrPc function but also to the conformational conversion process [104].
Relationship to other diseases
Researchers of prion diseases believe that PrP may play important roles in other brain disorders. Ongoing studies may also help determine whether prions consisting of other proteins may play a part in more common neurodegenerative conditions, including Alzheimer's disease, Parkinson's disease and amyotrophic lateral sclerosis (ALS). Clinical studies also showed a striking similarity between TSE and common age-related conditions such as Alzheimer’s or Parkinson’s disease, both of which show symptoms of progressive dementia and loss of motor control, respectively. Both of these diseases are spontaneous, but they can sometimes be inherited. With regard to CJD and Alzheimer’s disease, DeArmond et al. [107] stated that “although there are obvious differences in the etiology and pathogenesis of both sets of disorders, a remarkable number of similarities exist.” In both cases, pathogenesis involves an abnormal form of a neuronal membrane protein. One feature that distinguishes the TSE diseases from other neurodegenerative diseases is the glycophosphatidylinositol membrane anchor on prion protein, the molecule that is corrupted in TSE diseases. The presence of this anchor profoundly affects TSE pathogenesis, which involves major membrane distortions in the brain, and may be a key reason for the greater neurovirulence of TSE prions relative to many other autocatalytic protein aggregates [108]. The abnormal buildup of amyloid-β (Aβ) peptides in the brain is regarded as the causes of Alzheimer’s disease. Lauren et al. [109] show that the prion protein might mediate the pathogenic effects of Aβ oligomers. Their groups find that, within PrPc, aminoacid residues 95–110 are crucial for Aβ binding. Interestingly, the enzyme α-secretase - which precludes Aβ production by cleaving the Aβ precursor protein APP within the Aβ domain - also cleaves PrPc between residues 111 and 112 [110], thus releasing from the membrane the portion of PrPc to which Aβ would otherwise bind. For instance, does PrPc mediate the effects of Aβ dimers isolated from brains of people with Alzheimer’s disease [111, 112], or of the Aβ*56 oligomer, which causes memory deficits in mouse models of this disease [113, 114]? Not withstanding these unresolved questions, the discovery that PrPc may be a mediator in the development of Alzheimer’s disease is fascinating, not least from a therapeutic perspective. There are still many researches are on the way to elucidate the relationship of prion protein with other neurodegenerative disorders.
Therapeutic approach to prion disease
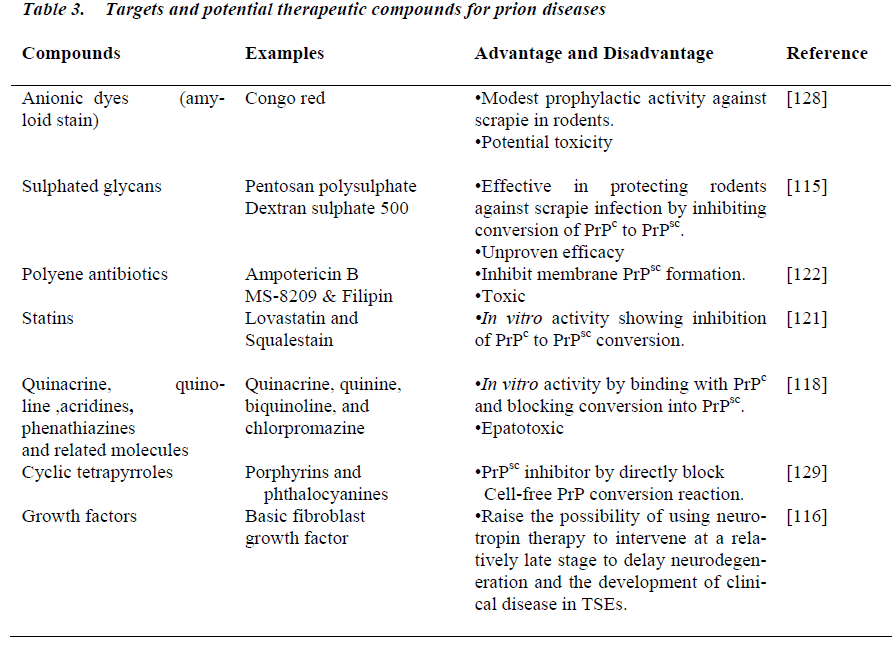
Prion diseases are always fatal, often not until months after the outbreak of the disease. According to studies conducted on mice suffering with scrapie, PrPc seems to have a protective effect in certain conditions such as stroke. Interestingly, mice that do not produce PrPc appear to be completely healthy. This property provided a starting point for a new therapeutic approach that has recently become a focal point: can the production of healthy PrPc be switched off in infected animals, thereby depriving the diseased PrPsc of its ability to spread? In this way, the chain reaction would be interrupted. Insights into prion research and techniques might also prove to be useful in laterstage treatment regimes for other diseases. Newly designed proteins might be able to convert viral or bacterial proteins into a disabled state. The unique biological features of the prion protein have encouraged investigation of new prophylactic strategies and therapeutics with multiple compounds aimed at a single target, i.e., PrP (Table 3) [115, 116, 117, 118, 119, 120, 121, 122] Over the past three decades, number of drugs has been isolated as active against mammalian prion [123]. These include polysulfate anions, dextrans, heparins, oligonucleotides, cyclic tetrapyrroles, anthrocyclines, porphyrins and diazo dyes.
However, none of these has proven to be an effective therapy for sick animals or patients, although there was some success using quinacrine and chlorpromazine in vitro. For most of these compounds, the mode of action and targets remain largely unknown. Mostly, two main modes of action for antiprion drugs can be imagined: either in cis, or in trans. Some compounds are thought to bind directly to PrPc or PrPsc like Congo Red (CR), Pentosan Polysulfate (PPS) or Glycosaminoglycans (GAGs) have cis action. Other compounds are thought to act in trans by affecting PrPc or PrPsc indirectly. Among these molecules are various lysosomotropic factors including the antimalarial drugs Quinacrine (QC) and Chloroquine. Indeed, the lysosome is a potential site of conversion of PrPc to PrPsc [124]. In addition, a recent report [28], proposes that QC’s antiprion activity is related to its ability to redistribute cholesterol from the plasma membrane to intracellular compartments, thereby destabilizing membrane domains. Other compounds like Curcumin and Di-methyl sulphoxide (DMSO) have been used for the therapeutic purposes. Curcumin is an efficient inhibitor of PrPsc propagation in RML-infected N2a cells (IC50 10 nM), and causes a decrease in detectable protease-resistant PrP in cell free conversion studies (40% decrease with 10 nM curcumin), but it has no effect on disease progression after i.c. prion infection in hamsters regardless of the treatment regime [125]. DMSO treatment decreases the amount of detectable PrPsc in ScN2a culture [126] and reduces the infectivity titre of scrapieinfected brain material [127] in prion propagation systems. It is uncertain whether these findings can be extrapolated to the clinical realm. Furthermore, results suggested that such drugs could adversely impact the health of the patients.
Most described therapeutic strategies target the infectious prion particles; some researchers are seeking methods of repairing the disease related structural damage to the brain. Others have reported that stem or fetal cell transplants can colonize damaged areas and restore some of the lost tissue in experimental animals. Intercepting disease progression in advance of debilitation and irreversible brain damage, however, could increase treatment options. Many researchers have emphasized the dire need for diagnostic tools that would permit widespread screening for carriers of the infectious agent. Such tools could indicate potential candidates for early treatment with therapeutic compounds that might prevent continued infection.
Closing remarks
Our understanding of prion diseases has advanced dramatically over the past half-century. It is now clear that these diseases, once thought to be medical and veterinary curiosities, exemplify novel principles of protein structure and transfer of biological information. Some of these principles may have applicability to other neurodegenerative disorders such as Alzheimer’s, Parkinson’s, and Amyotrophic lateral sclerosis (ALS) diseases, which all involve accumulation of conformationally altered proteins. In addition to their intrinsic scientific and medical significance, prion diseases have also assumed increasing public health importance. The emergence of BSE and variant CJD emphasizes the need for designing more sensitive procedures for detecting prions in food, blood products and donor organs. Although prion diseases currently affect a relatively small number of individuals, it is wise to take steps to prevent potential increases in their incidence. The knowledge gained from the study of prion diseases may provide effective strategies geared toward defining disease etiology and dissecting molecular pathogenesis of more common neurodegenerative disorders such as Alz-heimer’s disease, Parkinson’s disease and ALS. Since the risk from inherited disease is present decades before neurologic dysfunction is evident, development of effective therapies is imperative.
A critical issue is whether the phenomenon of propagation of biological information through transmission of protein conformation is exclusively associated with a small group of proteins, like PrP, or a more general process in biology. The discovery of proteins with prion-like behavior in yeast and fungi has provided some insight [130, 131]. Understanding prion multiplication and disease processes will certainly open up new vistas in biochemistry and genetics. As PDs are incurable and fatal, a continuous vigilance is needed to preempt outbreaks of prioninduced diseases.
Acknowledgements
This work was supported by the grant of the Korean Ministry of Education, Science and Technology
References
- Zigas V. Kuru in New Guinea: Discovery and Epidemiology. Am J Trop Med Hyg. 1970; 19:130-132.
- Liberski PP, Gajdusek DC. Kuru: forty years later, a historical note. Brain Pathol.1997; 7: 555-560.
- Williams ES, Youn S. Chronic wasting disease of captive mule deer; a spongiform encephalopathy. J Wildl. Dis 1980; 16: 89-98.
- Guiroy DC, Williams ES, Yanagihara R. Gajdusek, DC. Immunolocalization of scrapie amyloid (PrP27-30) in chronic wasting disease of Rocky Mountain elk and hybrids of captive mule deer and whitetailed deer. Neurosci Lett 1991; 27: 195-198.
- Aguzzi A, Polymenidou M. Mammalian prion biology: one century of evolving concepts. Cell 2004; 116:313-327.
- Ross ED, Minton A, Wickner RB. Prion domains: sequences, structures and interactions. Nat Cell Biol 2005b; 7: 1039-1044.
- Shkundina IS, TerAvanesyan MD. Prions. Biochemistry 2007; 72: 1519-1536.
- Shorter J, Lindquist S. Prions as adaptive conduits of memory and inheritance. Natl Rev 2005; 6: 435-450.
- Sparrer HE, Santoso A, Szoka FC, Weissman Jr, Weissman JS. Evidence for the prion hypothesis: induction of the yeast [PSI+] factor by in vitro converted Sup35 protein. Science 2000; 289: 595-599.
- IngeVechtomov SG, Zhouravleva GA, Chernoff YO. Biological roles of prion domains. Prion 2007; 1: 228-235.
- Wickner RB, Edskes HK, Shewmaker F, Nakayashiki T. Prions of fungi: inherited structures and biological roles. Nature Rev. Microbiol 2007; 5: 611-618.
- Prusiner SB. Prion diseases and the BSE crisis. Science 1997; 278: 245-251.
- Prusiner SB. Prion Biology and Diseases. Cold Spring Harbor Laboratory Press, New York Cold 2003; 6: pp. 1-800.
- Prusiner SB, Scott MR, DeArmond SJ, Cohen FE. Prion protein biology. Cell 1998; 93: 337-348.
- Collinge J. Prion diseases of humans and animals: their causes and molecular basis. Annu Rev Neurosc 2001; 24: 519-550.
- Tanaka M, Chien P, Yonekura K, Weissman JS. Mechanism of crossspecies prion transmission: An infectious conformation compatible with two highly divergent yeast prion proteins. Cell 2005; 121: 49-62.
- Medori R, Tritschler HJ, LeBlanc A, Villare F, Manetto V, Chen, HY. Fatal familial insomnia, a prion disease with a mutation at codon 178 of the prion protein gene. N Engl J Med 1992; 326: 444-449.
- Deriziotis P, Tabrizi SJ. Prions and the proteasome Biochim Biophys Acta 2008; 1782: 713-722.
- Aguzzi A, Weissmann C. Prion research: the next frontiers. Nature 1997; 389: 795-798.
- Alper T, Cramp WA, Haig DA, Clarke, MC. Does the agent of scrapie replicate without nucleic acid? Nature 1967; 214: 764-766.
- Prusiner SB. Novel proteinaceous infectious particles cause scrapie. Science 1982; 216: 136-144.
- Dickinson AG, Outram GW. The scrapie replicationsite hypothesis and its implications for pathogenesis. Academic Press, NY. In Slow transmissible diseases of the central nervous system 1979; 2: 13-31.
- Gibbs CJ Jr, Gajdusek DC, Latarjet R. Unusual resistance to ionizing radiation of the viruses of kuru, CreutzfeldtJakob disease. Proc. Natl. Acad. Sci. USA 1978; 75: 6268-6270.
- Levine P. Scrapie: an infective polypeptide? Lancet 1972; 1: 748-749.
- Anonymous. Scrapie: strategies, stalemates, and successes. Lancet 1982; 1: 1221-1223.
- Kimberlin R. Scrapie agent: Prions or virinos? Nature 1982; 297: 107-108.
- Somerville RA. The transmissible agent causing scrapie must contain more than protein. Rev Med Virol 1991; 1: 131-139.
- Kocisko DA, Come JH, Priola SA, Chesebro B, Raymond GJ, Lansbury PT, et al. Cellfree formation of proteaseresistant prion protein. Nature 1994 370: 471-474.
- Prusiner SB, Bolton DC, Groth DF, Bowman KA, Cochran P, McKinley MP. Further purification and characterization of scrapie prions. Biochemistry 1982; 21: 6942- 6950.
- Prusiner SB. Prions. Proc. Natl Acad Sci USA 1998; 95: 13363-13383.
- Borchelt DR, Scott M, Taraboulos A, Stahl N, Prusiner SB. Scrapie and cellular prion proteins differ in their kinetics of synthesis and topology in cultured cells. J Cell Biol 1990; 110: 743-752.
- Caughey B, Dong A, Bhat KS, Ernst D, Hayes SF, Caughey WS. Secondary structure analysis of the scrapieassociated protein PrP 27-30 in water by infrared spectroscopy. Biochemistry 1991; 30: 7672-7680.
- Pan KM, Baldwin M, Nguyen J, Gasset M, Serban A, Groth D, et al. Conversion of a-helices into Ã-sheets features in the formation of the scrapie prion proteins. Proc Natl Acad Sci USA 1993; 90: 10962-10966.
- Stahl N, Baldwin MA, Teplow DB, Hood L, Gibson GW, Burlingame AL, et al. Structural studies of the scrapie prion protein using mass spectrometry and amino acid sequencing. Biochemistry 1993; 32: 1991-2002.
- Safar J, Roller PP, Gajdusek DC, Gibbs CJ. Conformational transitions, dissociation, and unfolding of scrapie amyloid (prion) protein. J Biol Chem 1993; 268: 202-76-20284.
- Prusiner SB. Shattuck Lecture: Neurodegenerative diseases and prions. N Engl J Med 2001; 344: 1516-1526.
- Donne DG, Viles JH, Groth D, Mehlhorn I, James TL, Cohen FE, et al. Structure of the recombinant fulllength hamster prion protein PrP (29-231): the N terminus is highly flexible. Proc Natl Acad Sci USA 1997; 94: 13452-13457.
- Riek R, Hornemann S, Wider G, Billeter M, Glockshuber R, Wuthrich K. NMR structure of the mouse prion protein domain PrP (121?231). Nature 1996; 382: 180-182.
- Moser M, Colello RJ, Pott U, Oesch B. Developmental expression of the prion protein gene in glial cells. Neuron 1995, 14: 509-517.
- Caughey B, Race RE, Chesebro, B. Detection of prion protein mRNA in normal and scrapieinfected tissues and cell lines. J Gen Virol 1988; 69: 711-716.
- Dodelet VC, Cashman NR. Prion protein expression in human leukocyte differentiation. Blood 1998; 91: 1556-1561.
- Ford MJ, Burton LJ, Li H, Graham CH, Frobert Y, Grassi J, et al. A marked disparity between the expression of prion protein and its message by neurones of the CNS. Neuroscience 2002; 111: 533-551.
- Lasmezas CI. Putative functions of PrPC. Br. Med. Bull 2003; 66: 61-70.
- Manson J, West JD, Thomson V, McBride P, Kaufman MH, Hope J. The prion protein gene: a role in mouse embryogenesis? Development 1992; 115: 117-122.
- Aguzzi A, Baumann F, Bremer J. The prion's elusive reason for being. Annu Rev Neurosci 2008; 31: 439-477.
- Collinge J, Whittington MA, Sidle KC, Smith CJ, Palmer MS, Clarke AR, et al. Prion protein is necessary for normal synaptic function. Nature 1994; 370: 295- 297.
- Herms J, Tings T, Gall S, Madlung A, Giese A, Siebert H, et al. Evidence of presynaptic location and function of the prion protein. J Neurosci 1999; 19: 8866-8875.
- Moore RC, Lee IY, Silverman GL, Harrison PM, Strome R, Heinrich C, et al. Ataxia in prion protein deficient mice is associated with upregulation of the novel PrPlike protein doppel. J Mol Bio 1999; 292: 797-817.
- Brown DR, Besinger A. Prion protein and superoxide dismutase activity. Biochemical Journal 1998; 334: 423-429.
- Aronoff-Spencer E, Burns CS, Avdievich, NI, Gerfen, GJ, Peisach J, Antholine WE, et al. Identification of the Cu21 binding sites in the Nterminal domain of the prion protein by EPR and CD spectroscopy. Biochemistry 2000; 39: 13760-13771.
- Jackson GS, Murray I, Hosszu LL, Gibbs N, Waltho JP, Clarke AR, et al. Location and properties of metalbinding sites on the human prion protein. Proc Natl Acad Sci USA 2001; 98: 8531-8535.
- Pauly PC, Harris DA. Copper stimulates endocytosis of the prion protein. J Biol Chem 1998; 273: 33107-33110.
- Perera WS, Hooper NM. Ablation of the metal ion induced endocytosis of the prion protein by disease-associated mutation of the octarepeat region. Curr Biol 2001; 11: 519-523.
- Brown DR. Normal protein and the synapse. Trends Neurosci 2001; 24: 85-90.
- McLennan NF, Brennan PM, McNeill A, Davies I, Fotheringham A, Rennison KA, et al. Prion protein accumulation and neuroprotection in hypoxic brain damage. Am J Pathol 2004; 165: 227-235.
- Spudich A, Frigg R, Kilic E, Kilic U, Oesch B, Raeber A, et al. Aggravation of ischemic brain injury by prion protein deficiency: role of ERK-1/-2 and STAT-1. Neurobiol Dis 2005; 20: 442-449.
- Chiarini LB, Freitas AR, Zanata SM, Brentani RR, Martins VR, Linden R. Cellular prion protein transduces neuroprotective signals. EMBO J 2002; 21: 3317 -3326.
- Zhang CC, Steele AD, Lindquist S, Lodish HF. Prion protein is expressed on longterm repopulating hematopoietic stem cells and is important for their self renewal. Proc Natl Acad Sci USA 2006; 103: 2184-2189.
- Masel J, Jansen V AA, Nowak MA. Quantifying the kinetic parameters of prion replication. Biophys Chem 1999; 77: 139-152.
- Hill AF, Zeidler M, Ironside J, Collinge J. Diagnosis of new variant CreutzfeldtJakob disease by tonsil biopsy. Lancet 1997; 349: 99-100.
- Kitamoto T, Muramoto T, Mohri S, Dohura K, Tateishi J. Abnormal isoform of prion protein accumulates in follicular dendritic cells in mice with Creutzfeld?Jakob disease. J Virol 1991; 65: 6292-6295.
- Mabbott NA, MacPherson GG. Prions and th