Research Article - Biomedical Research (2018) Artificial Intelligent Techniques for Bio Medical Signal Processing: Edition-II
Nuclear factor E2-related factor expression and its relationship with oxidative stress in the placenta of pregnant diabetic rats
Hongping Zhang1, Jianqiong Zheng1*, Yehui Zhang1, Yeping Wang1, Jianxin Li2, Xiaomin Xu2, Min Lin2 and Xiaoqin Li2
1Department of Gynecology and Obstetrics, Wenzhou People’s Hospital, Wenzhou Maternal and Child Health Care Hospital, the Third Clinical Institute Affiliated To Wenzhou Medical University, Wenzhou, Zhejiang, PR China
2Wenzhou City Key Laboratory of Gynecology and Obstetrics, Wenzhou People’s Hospital, Wenzhou Maternal and Child Health Care Hospital, the Third Clinical Institute Affiliated to Wenzhou Medical University, Wenzhou, Zhejiang, PR China
- *Corresponding Author:
- Jianqiong Zheng
Department of Gynecology and Obstetrics
Wenzhou People’s Hospital
Wenzhou Maternal and Child Health Care Hospital, PR China
Accepted on March 14, 2017
DOI: 10.4066/biomedicalresearch.29-16-2217
Visit for more related articles at Biomedical ResearchAbstract
Objective: The aim of this study is to investigate Nrf2 expression in placenta of gestational diabetes mellitus rat (GDM) and the relationship between oxidative stress.
Methods: Thirty pregnancy SD rats were chosen in our study, and randomly divided into 3 groups: normal control group, GDM group and GDM+Oltipraz (5 mg/kg, via intragastric administration 1 hour before STZ treatment) group. GDM and GDM group were treatment with Streptozotocin (STZ) via intraperitoneal injection once a week, the control group was treatment with the same amount of citric acid buffer. On day 20 of pregnant period, anesthesia and dissect rats, placenta tissue and blood were prepared for experiment. The expression of Nrf2 in placenta was determined by western blotting. Insulin expression and Total antioxidative capability and MDA were detection by ELISA Kit.
Results: Blood glucose has been increased significantly when the GDM group and control group were compared with the difference was statistically significant. With the GDM group, the intervention group was compared so that the placental insulin levels were significantly increased and the difference was statistically significant. GDM group Nrf2 protein expression levels were significantly increased and the difference was statistically significant (P<0.05) when it is compared with normal group.
Conclusion: GDM is a problem of great clinical importance core for the development of numerous adverse maternal and perinatal outcomes. Through the placenta tissue of rat insulin levels, total antioxidant capacity (total antioxidant capacity, TAC), lipid peroxidation levels and protein expression of Nrf2, this study recognized a gestational diabetic rat model to explore the possible pathogenesis of gestational diabetes, and provided a theoretical basis for clinical treatment.
Introduction
Gestational diabetes (Gestational diabetes mellitus, GDM) refers to the occurrence or during pregnancy was first discovered impaired glucose tolerance caused by different degrees of abnormal glucose metabolism, is a common highrisk obstetrics pregnancy, the incidence rate is about 15% [1]. The disease hazards maternal-fetal safety, and even lifethreatening perinatal [2].
During pregnancy, the risk of preeclampsia was increased for women along with GDM that had high risks for type 2 diabetes and cardiovascular diseases in their later life in Chinese and other populations. The childhood obesity, impaired glucose tolerance and increased cardiovascular risk profile during adolescence and early adulthood was developed with more inclination by the offspring born to GDM-complicated pregnancy. In china, the GDM occurrence has been increasing globally. Occurrence has been increased from 2.3% in 1999 to 6.8% in the year 2008 at Tianjin, a cosmopolitan city near Beijing in North China. With the increase of prevalence, data was compared across regions/areas is vulnerable by differences in screening procedures and diagnostic criteria for GDM and lack of quality population-based studies [3]. Evidence of the landmark study of the Hyperglycaemia and Adverse Pregnancy Outcomes (HAPO) Survey recommended use of a new set of diagnostic criteria for GDM by one-step approach performing a 75 g, 2 h Oral Glucose Tolerance (OGTT) has been reviewed by the International Association of Diabetes and Pregnancy Study Group (IADPSG).
Older age (high maternal age), pre-pregnancy obesity, high parity, Family History of Diabetes (FHD) (especially in firstdegree relatives), previous delivery of a macrosomic infant and previous obstetric outcome history (e.g. previous history of GDM, congenital malformation, caesarean section) are some of the traditional and most often reported risk factors for GDM. Still some controversial potential risk factors are available such as low or high birth weight, short stature, smoking, multiparty, physical inactivity, excess weight gain in pregnancy and socioeconomic factors like education level, occupation and monthly household income. Occurrence of diabetes, obesity and metabolic syndrome is increased in turkey with growth of economy and the transition to a more sedentary lifestyle. Prevalence has increased from 7.2% to 13.7% in the last 12 years for the diabetes [4].
GDM occurrence varied based on race–ethnicity ranges from a low of 6.8% among non-Hispanic whites to 16.3% among Asians and Pacific Islanders. In Unites States, data have suggested that the incidence of GDM is increasing in all race– ethnicities with a trend paralleling the increase in prevalence of type 2 diabetes. Risk of fetal macrosomia, large-forgestationalage neonates, preeclampsia, perinatal mortality, and cesarean delivery was increased by associated with gestational diabetes mellitus along with long-term hazards, a higher risk of maternal type 2 diabetes and obesity, glucose intolerance, and metabolic syndrome in the offspring of women born to mothers diagnosed with GDM [5].
GDM risk factors are established by including the history of GDM in a prior pregnancy, history of delivering a macrosomic neonate, advanced maternal age, nonwhite race–ethnicity, and high parity. Family history of diabetes mellitus12 and maternal high or low birth weight is included with an additional nonmodifiable factors related to GDM risk. The GDM risk is increased with potentially modifiable factors being overweight or obese by having a body mass index [calculated as weight (kg)/[height (m)]2] of at least 25, being sedentary lifestyle, and by consuming a low-fiber and high glycemic-load diet.
In a clinical trial, to have cancer chemopreventive activity a prototype dithiolethione, oltipraz has been presented. Oltipraz enhances the binding activity of Nrf2 to the antioxidant response element and so production of phase II enzyme genes ware increased. Recent studies documented the beneficial effect of oltipraz on insulin action in some mouse models of insulin resistance where the investigators did not relate the insulin-sensitizing effect of oltipraz to Nrf2 activation directly [6]. Diabetic patients often appear oxidative stress, insulin resistance and chronic inflammation and other clinical manifestations, and these manifestations and nuclear factor E2- related factor (nuclear factor elytroid-derived factor 2-related factor, Nrf2) expression is closely related to [7]. Maternal-fetal placenta is linked endocrine organ, GDM placental tissue is affected Nrf2 expression levels of oxidative stress, not reported in the literature.
Literature Survey
Zhu et al. [8] collected peripheral blood samples from women at 16-19 weeks of pregnancy at a tertiary hospital in China between the year of 2010 and 2014. Samples collected from 10 women were subsequently diagnosed with GDM and constructed two small Ribo-Nucleic Acid (RNA) libraries. Quantitative Real-Time Polymerase Chain Reaction (qRTPCR) validates the differentially expressed miRNAs by performing high-throughput sequence, followed by target prediction, Gene Ontology analysis, and pathway identification. Results provide the insights into the molecular mechanisms that underlie GDM that contributes to the diagnosis and treatment of this disease.
Artal [9] documented the physical inactivity as an independent risk factor for obesity insulin resistance and type 2 diabetes. To magnify the risk, the physiological and hormonal changes related with pregnancy. On the other hand the evidence and accumulated experience indicate that antenatal lifestyle interventions includes physical activity and judicious dieting improved the pregnancy outcome and reduced the risk of gestational diabetes and has been an effective as an adjunctive therapy for diabetes in pregnancy. American Congress of Obstetricians and Gynecologists (ACOG), American Diabetes Association (ADA), Royal College of Obstetricians and Gynaecologists (RCOG), and Society of Obstetricians and Gynaecologists of Canada (SOGC) were the major professional organizations recommend the lifestyle interventions that include diet and exercise to prevent or manage gestational diabetes or diabetes mellitus.
Hernandez et al. [10] challenged on CONVentional Lowcarbohydrate/ higher-fat (LC/CONV) diet, hypothesizing that a higher-complex Carbohydrate/lower-fat (CHOICE) diet would improve the maternal Insulin Resistance (IR), Adipose Tissue (AT) lipolysis, and infant adiposity. 12 diet-controlled overweight/obese women with GDM at 31 weeks were randomized to an isocaloric LC/CONV with 40% carbohydrate/45% fat/15% protein; n=6 or CHOICE with 60%/25%/15%; n=6 diet. All meals were provided. At 37 weeks, AT was biopsied. Insulin suppression of AT lipolysis was improved on CHOICE versus LC/CONV (56 vs. 31%, P=0.005), consistent with improved IR. AT expression of multiple proinflammatory genes was lower on CHOICE (P & lt; 0.01). Infant adiposity trended lower with CHOICE (10.1 & plusmn; 1.4 vs. 12.6 & plusmn; 2%, respectively). A CHOICE diet improves the maternal IR and infant adiposity, challenge the recommendation for a LC/CONV diet.
Bhavadharini et al. [11] estimated the utility of Capillary Blood Glucose (CBG) to diagnose the GDM in resource-constrained settings where Venous Plasma Glucose (VPG) estimations may be impossible. In southern India, consecutive pregnant women (n=1031) attended an antenatal clinics underwent 75 g OGTT. Fasting were measured, 1 and 2 h VPG (AU2700 Beckman, Fullerton, CA) and CBG (One Touch Ultra-II, LifeScan). For different CBG cut points, sensitivity and specificity were estimated by using the International Association of Diabetes in Pregnancy Study Groups (IADPSG) criteria to diagnose the GDM as gold standard. Bland–Altman plots were drawn to look at the agreement between CBG and VPG. For CBG values, correlation and regression equation analysis were derived.
Loboda et al. [12] concise the knowledge about Nrf2 and HO-1 across different phyla by suggesting their conservative role as stress-protective and anti-aging factors. Expression of genes coding was regulated by the multifunctional regulator Nrf2 and a cytoprotective factor for anti-oxidant, anti-inflammatory and detoxifying proteins. The vertebrate Nrf2 belongs to Cap ‘n’ Collar (Cnc) bZIP family of transcription factors that shares a high homology with SKN-1 from Caenorhabditis elegans or CncC found in Drosophila melanogaster. Major characteristics of Nrf2 were to some extent represented by Nrf2-dependent genes and their proteins includes Heme Oxygenase-1 (HO-1), which besides removing toxic heme, produces biliverdin, iron ions and carbon monoxide. Through the protection against oxidative injury, regulation of apoptosis, modulation of inflammation and contribution to angiogenesis, HO-1 and their products used the beneficial effects. Disturbances in the proper HO-1 level were associated with the pathogenesis of some agedependent disorders that includes neurodegeneration, cancer or macular degeneration.
Materials and Methods
Animals
Female, male clean grade SD (Sprague-Dawley) 30 rats, weighing 200-250 g, were purchased from Chinese Academy of Sciences Shanghai Branch Experimental Experimental Animal Center. Experiments with male and female rats were placed in a well-ventilated, relative humidity of 40%-70% and a temperature of 22°C-25°C shielding system, free diet. Give lighting 12 h/d, and the timely replacement of feed, one week of accommodation. Adaptive feeding 1 week after fasting for 12 h, fast glucose oxidase test blood glucose intravenously, weighed. Excluding fasting blood glucose ≥ 11.1 mmol/L mice. The male and female rats at 1:2 ratio mated overnight, the next morning found that vaginal mucus examination or sperm are marked as pregnancy 0d, calculate pregnancy. This study was approved by the ethics committee of Wenzhou City People’s Hospital for approval.
Method
The establishment of gestational diabetic rat model [13,14]. Using a random number table, 30 SD rats were divided into normal group (control group), gestational diabetes mellitus (GDM group) and gestational diabetes+Oltipraz group (intervention group) equally. GDM group and the intervention was given streptozotocin (Streptozotocin, STZ) intraperitoneal injection in the dosage of 45 mg/kg (now with the current, saved ice bath) after the fasting 12h and return to normal diet after 4 h [15]. 5 days after STZ injection, the fasting blood glucose ≥ 11.1 mmol/L mice was determined as gestational diabetes successful model. Control group was given a normal diet and injected the same amount of citrate buffer. After successful modeling, the intervention group were given the body of Oltipraz orally, Oltipraz first dissolved in DMSO, and then dissolved in sodium carboxymethyl cellulose, according to 5 mg/kg administered concentration; control group and the GDM group was given the same amount of the sodium carboxymethylcellulose gavage. STZ, Oltipraz, sodium carboxymethyl cellulose purchased from sigma company; sodium citrate were purchased from Shanghai Biochemical Technology Co., Ltd. Aladdin.
The placental tissue samples and tissue preparation
Pregnant rats 20 d undelivered after fasting 12 h, intraperitoneal injection of chloral hydrate (3.5%) were anesthetized and sacrificed, caesarean section to remove the placental tissue. A placenta ultrasound (condition) treatment, 2000 rpm centrifugal 15 min, supernatant was used for insulin, total antioxidant capacity (total antioxidant capacity, TAC) and malondialdehyde (malondialdehyde, MDA) detection. TAC, MDA and insulin assay kit comes on Haixi Tang Biotechnology Limited. Another organization in accordance with 50 mg/500 μL lysis buffer ratio of placental tissue homogenates ice bath, sonication lysis solution 10 s after 60 min, lysate at 4°C, 12000 rpm centrifugal 20 min, the supernatant was measured Nrf2 protein content.
The measurement of insulin levels
Diabetes mellitus, a clinically and genetically heterogeneous group of disorders consists of one common feature which has high levels of glucose in the blood due either to insulin deficiency or to resistance of the body’s cells to the action of insulin. Over the past several decades, research led to the recognition that the different types of diabetes have different causes although their pathologic courses after onset of diabetes may be similar. Insulin-Dependent Diabetes Mellitus (IDDM) has low or absent levels of circulating endogenous insulin and to prevent ketosis and sustain life it is dependent on injected insulin. Onset mostly in youth but may occur at any age. It is associated with certain HLA and GAD antigens. During diagnosis, an abnormal immune response and islet cell antibodies are frequently presented. Etiology probably only partially genetic, as only ~35% of monozygotic twins are concordant for IDDM. Non-Insulin-Dependent Diabetes Mellitus (NIDDM) has Insulin levels as normal, elevated, or depressed. Most patients are characterized by hyperinsulinemia and insulin resistance. Like disease progresses insulinopenia is developed. For treatment of hyperglycemia, insulin may be used and not insulin-dependent or ketosis-prone under normal circumstances. Onset predominantly after age 40 years but can occur at any age. Around 50% of men and 70% of women are obese. Etiology probably strongly genetic as 60%-90% of monozygotic twins are concordant for NIDDM..Enzymelinked immunosorbent assay (ELISA) was utilized to detect placental insulin levels.
The measurement of TAC levels
Fe3+ can reduced to Fe2+ by TAC, and Fe2+ Philippines reacting morpholine can form a stable complex with the class by colorimetric measured antioxidant capacity in accordance with the level of under 520 nm in antioxidants. In accordance with the ELISA kit instructions, according to the standard curve equation to calculate the total antioxidant capacity of the placenta.
The measurement MDA Levels
The principle of Thiobarbituric acid (TBA) assay detecting MDA. A chemical reaction occurs producing a color change between MDA and TBA, which can detect changes in the relative content of MDA at 532 nm. In accordance with the ELISA kit instructions and according to the standard curve equation to calculate the total antioxidant capacity of the placenta.
Nrf2 protein expression by Western blot assay
Coomassie protein quantitative determination of the application standard quantitative methods. Optical density measured at 595 nm. Standard protein concentration standard curve of optical density values to calculate the sample protein concentration. Determination of Nrf2 expression levels by western blot method, and after scanning ChemiDoc XRS+ (BIO-RAD), with ImageStudioLite strip analysis software.
Statistical method
SPSS 17.0 software was used for statistical analysis. All measurement data were presented as mean ± standard deviation (x̅ ± S). For comparison between two groups, one-way ANOVA was used for measurement data. P<0.05 was considered statistically significant.
Result
Comparison of blood glucose and insulin levels in the placenta of rats
Comparing with GDM group and control group, blood glucose was significantly increased and the difference was statistically significant. Compared the intervention group with the GDM group, the placental insulin levels were significantly increased and the difference was statistically significant. The results are shown in Table 1.
| Number of cases | Glucose (mmol/L) | Insulin (ng/ml) | |
|---|---|---|---|
| Control | 10 | 6.40 ± 0.18 | 0.135 ± 0.007 |
| GDM group | 10 | 9.58 ± 0.70*** | 0.129 ± 0.007 |
| Intervention group | 10 | 8.06 ± 0.87 | 0.156 ± 0.009# |
Note: *Indicates GDM group and control group, P<0.001; #indicates the intervention group and the control group, P<0.05.
Table 1. Comparison of blood glucose and insulin levels in the placenta of rats.
Compare the placental oxidative stress parameters in rats TAC and MDA
Comparing with GDM group and control group, blood glucose was significantly increased and the difference was statistically significant. The results are shown in Table 2.
| Number of cases | TAC (mmol/ml) | MDA (μmol/mg) | |
|---|---|---|---|
| Control | 10 | 3.40 ± 0.16 | 26.97 ± 0.99 |
| GDM group | 10 | 3.90 ± 0.10 * | 29.94 ± 1.62 |
| Intervention group | 10 | 3.80 ± 0.25 | 28.18 ± 1.18 |
Note: *Indicates GDM group compared with the control group, P<0.05.
Table 2. Compares each group SD rat’s placenta TAC and MDA level.
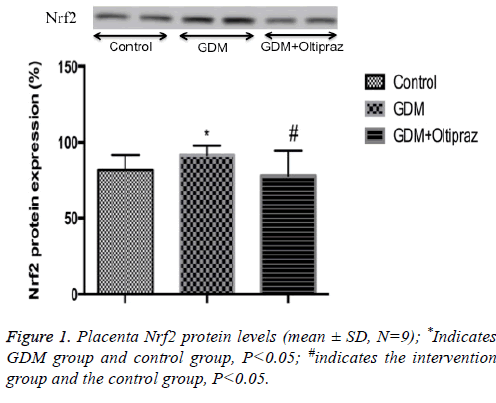
The groups were compared placenta Nrf2 protein levels
Compared with the normal group, GDM group Nrf2 protein expression levels were significantly increased and the difference was statistically significant (P<0.05); give the body of Oltipraz intervention, placenta Nrf2 protein expression decreased, the difference was statistically significant (P<0.05, Figure 1).
Discussion
Diabetes is considered to be induced by common genetic factors and environmental results, and reduced insulin secretion and oxidative stress are closely related [16]. When high glucose, endogenous reactive oxygen species exceeds the antioxidant defense system ability to eliminate reactive oxygen species, which will produce large amounts of free radicals [17]. Islet B cells reactive oxygen species and reactive nitrogen high sensitivity, and low antioxidant superoxide dismutase levels, islet B cells susceptible to injury [18], resulting in reduced insulin secretion. Studies suggest that oxidative stress related to the reduction the secretion of pancreatic B cells and insulin resistance phenomenon, which is the basic aspects and features of the pathogenesis of type 2 diabetes [19]. GDM is one of the common diseases in pregnancy, high blood sugar during pregnancy not only maternal health hazard, but also has an adverse effect on the fetus, such as excessive amniotic fluid, fetal growth restriction, premature birth, stillbirth, especially prone to huge children [20]. GDM pathogenesis is unknown, may be associated with insulin resistance [21,22] pancreatic B cell defects [23-25], genetic factors [26,27] and oxidative stress [28-30].
With the research of oxidative stress and gestational diabetes gradually deepening, some scholars have found that pregnancy hyperglycemia oxidative stress can occur in the placenta and the placenta plays an important role in the protection of offspring adversely affect maternal hyperglycemia in recent years [31]. Comparision with the adoption of Raman spectroscopy between normal pregnant women and patients with GDM placental tissue, content of amino acid residues, CO bond and H bond were selected as the observation. It is found that GDM placental tissue in patients subjected to oxidative stress hyperglycemia. There are siginicant different between GDM placental tissue in patients with normal placentas of pregnant women there are significant differences [32]. We found in the study that it was significantly higher compared to normal pregnant rat placenta of gestational diabetes in the total antioxidant capacity. Placenta lipid antioxidant capacity in gestational diabetes group is higher than the normal group, and total antioxidant capacity of this trend showed a high degree of consistency. We hypothesized that these variations are placenta placenta a protection against high glucose made by the reaction. GDM, the placenta forms, quality, microvilli, inflammatory states will change, and high glucose to a certain extent affect gas exchange placenta, supply nutrients, protein, fat, carbohydrate synthesis, transfer and exchange functions [32]. After the body of Oltipraz intervention, we found that mice GDM placental insulin levels were lower than normalins and the ulin levels rise. This may be because high glucose leads to oxidative stress, oxidative stress islet B cells, islet B cell injury affects the placenta insulin levels in the body, and after giving the body of Oltipraz, relieve oxidative stress state, reduce islet B cell damage, thus placenta insulin levels rise.
Nrf2 is important cellular antioxidant capacity of nuclear transcription factor-related, is the body against oxidative stress and cell damage in the central regulator, generally expressed in various tissues and cells. When oxidative stress occurs in cells, Nrf2 is activated into the nucleus. Nrf2 signaling network control is one of the body's main antioxidant defense system, the role of Nrf2 in maintaining glucose homeostasis in diabetes has been confirmed by numerous studies [6]. Researchers through Nrf2 knockout mice and Keap-1 knockout mice were tested and found lacking Nrf2 in vivo glucose balance had a positive effect, Nrf2 activation can be reduced insulin signaling, glucose uptake, which Tip Nrf2 may be associated with the promotion of insulin resistance [33-35]. We found that in animal studies, high gestational diabetes rat placenta Nrf2 protein expression compared with normal pregnancy, placenta Nrf2 description of hyperglycemia made protective response, which the placenta total antioxidant capacity and increased the same role. Oltipraz is Nrf2 activator, the body of Oltipraz in the intervention group placental protein expression of Nrf2 lower than the gestational diabetes group, we speculate that this may be related to the special role of the placental barrier and the expression of Nrf2 protein in different tissues is related in after the issue, we will discuss this in depth.
References
- Liying Z, Ling F, Yanhong D. The role of oral glucose tolerance test, fasting blood glucose levels in gestational diabetes diagnosis. J Perinatal Med 2012; 15: 660-663.
- Veeraswamy S, Vijayam B, Gupta VK, Kapur A. Gestational diabetes: the public health relevance and approach. Diabetes Res Clin Practice 2012; 97: 350-358.
- Leng J, Shao P, Zhang C, Tian H, Zhang F, Zhang S, Hu G. Prevalence of gestational diabetes mellitus and its risk factors in Chinese pregnant women: a prospective population-based study in Tianjin, China. PLoS One 2015; 10: e0121029.
- Erem C, Kuzu UB, Deger O, Can G. Prevalence of gestational diabetes mellitus and associated risk factors in Turkish women: the Trabzon GDM Study. Arch Med Sci 2015; 11: 724-735.
- Russo LM, Nobles C, Ertel KA, Chasan-Taber L, Whitcomb BW. Physical activity interventions in pregnancy and risk of gestational diabetes mellitus: a systematic review and meta-analysis. Obstet Gynecol 2015; 125: 576-582.
- Yu Z, ShaoW, Chiang Y. Oltipraz upregulates the nuclear respiratory factor 2 alpha subunit(NFR2) antioxidant system and prevents insulin resistance and obesity induced by a high-fat diet in C57BL/6J mice. Diabetologia 2011; 54: 922-934.
- Qiulan G, Ximei S, Liyong Y. Nrf2 relationship with diabetes pathogenesis. Fujian Medical University 2014; 48: 348-352.
- Zhu Y, Tian F, Li H, Zhou Y, Lu J, Ge Q. Profiling maternal plasma microRNA expression in early pregnancy to predict gestational diabetes mellitus. Int J Gynecol Obstet 2015; 130: 49-53.
- Artal R. The role of exercise in reducing the risks of gestational diabetes mellitus in obese women. Best Practice Res Clin Obstet Gynaecol 2015; 29: 123-132.
- Hernandez TL, Van Pelt RE, Anderson MA, Reece MS, Reynolds RM, de la Houssaye BA, Janssen RC. Women With Gestational Diabetes Mellitus Randomized to a Higher-Complex Carbohydrate/Low-Fat Diet Manifest Lower Adipose Tissue Insulin Resistance, Inflammation, Glucose, and Free Fatty Acids: A Pilot Study. Diabetes Care 2016; 39: 39-42.
- Bhavadharini B, Mahalakshmi MM, Maheswari K, Kalaiyarasi G, Anjana RM, Deepa M, Pastakia SD. Use of capillary blood glucose for screening for gestational diabetes mellitus in resource-constrained settings. Acta Diabetologica 2016; 53: 91-97.
- Loboda A, Damulewicz M, Pyza E, Jozkowicz A, Dulak J. Role of Nrf2/HO-1 system in development, oxidative stress response and diseases: an evolutionarily conserved mechanism. Cell Mol Life Sci 2016; 73: 3221-3247.
- John CM, Ranasamy R, NG Al, Al-Nuaimi AH, Adam A. Nicotinamide supplementation protects gestational diabetic rats by reducing oxidative stress and enhancing immune responses. Curr Med Chem 2012; 19: 5181-5186.
- Haider S, Ahmed S, Tabassum S, Memon Z, Ikram M, Haleem DJ. Streptozotocin-induced insulin deficiency leads to development of behavioral deficits in rats. Acta Neurologica Belgica 2013; 113: 35-41.
- Tian ZH, Miao FT, Zhang X, Wang QH, Lei N, Guo LC. Therapeutic effect of okra extract on gestational diabetes mellitus rats induced by streptozotocin. Asian Pacific J Tropical Med 2015; 8: 1038-1042.
- Zhang Y, Zhuang S, Li X. Oxidative stress in obese diabetic patients with nephropathy system and related factors. Chinese J General Pract 2013; 12: 820-823.
- Shen X, Li J, Yan Z. Relations selectin levels and oxidative stress in obese type 2 diabetic patients with serum E. Chinese J Pathophysiol 2006; 22: 2040-2043.
- Zhang H, Li R, Du X. Correlation of relevant factors and iron nutrition and oxidative stress in type 2 diabetes. Chinese General Practice 2013; 16: 2343-2346.
- Shi L. Oxidative stress associated with obesity and type 2 diabetes. Diabetes New World 2015.
- Emily J, Hannah J, Fraley E. Women Julianne Mazzawi. Appreciating Recent Motherhood and Culture: A Systematic Review of Multimodal Postpartum Lifestyle Interventions to Reduce Diabetes Risk in with Prior Gestational Diabetes. Maternal Child Health J 2016.
- Dutt A, Salvesen HB, Chen TH, Ramos AH, Onofrio RC, Hatton C, Nicoletti R, Winckler W, Grewal R, Hanna M, Wyhs N, Ziaugra L, Richter DJ, Trovik J, Engelsen IB, Stefansson IM, Fennell T, Cibulskis K, Zody MC, Akslen LA, Gabriel S, Wong KK, Sellers WR, Meyerson M, Greulich H. Drug-sensitive FGFR2 mutations in endometrial carcinoma. Proc Natl Acad Sci U S A 2008; 105: 8713-8717.
- Jung EJ. Fibroblast growth factor receptor 2 gene amplification status and its clinicopathologic significance in gastric carcinoma. Hum Pathol 2012; 43: 1559-1566.
- Ubeda M, Rukstalis JM, Habener JF. Inhibition of cyclin-dependent kinase 5 activity protects pancreatic beta cells from glucotoxicity. J Biol Chem 2006; 281: 28858-28864.
- Steinthorsdottir V, Thorleifsson G, Reynisdottir I, Benediktsson R, Jonsdottir T, Walters GB, Styrkarsdottir U, Gretarsdottir S, Emilsson V, Ghosh S, Baker A, Snorradottir S, Bjarnason H, Ng MC, Hansen T, Bagger Y, Wilensky RL, Reilly MP, Adeyemo A, Chen Y, Zhou J, Gudnason V, Chen G, Huang H, Lashley K, Doumatey A, So WY, Ma RC, Andersen G, Borch-Johnsen K, Jorgensen T, van Vliet-Ostaptchouk JV, Hofker MH, Wijmenga C, Christiansen C, Rader DJ, Rotimi C, Gurney M, Chan JC, Pedersen O, Sigurdsson G, Gulcher JR, Thorsteinsdottir U, Kong A, Stefansson K. A variant in CDKAL1 influences insulin response and risk of type 2 diabetes. Nat Genet 2007; 39: 770-775.
- Lauenborg J, Grarup N, Damm P, Borch-Johnsen K, Jørgensen T, Pedersen O, Hansen T. Common type 2 diabetes risk gene variants associate with gestational diabetes. J Clin Endocrinol Metabol 2009; 94: 145-150.
- Soronen J, Laurila PP, Naukkarinen J, Surakka I, Ripatti S, Jauhiainen M, Yki-Järvinen H. Adipose tissue gene expression analysis reveals changes in inflammatory, mitochondrial respiratory and lipid metabolic pathways in obese insulin-resistant subjects. BMC Med Genomics 2012; 5: 1.
- Pappa KI, Gazouli M, Economou K, Daskalakis G, Anastasiou E, Anagnou NP, Antsaklis A. Gestational diabetes mellitus shares polymorphisms of genes associated with insulin resistance and type 2 diabetes in the Greek population. Gynecol Endocrinol 2011; 27: 267-272.
- Wedekind L, Belkacemi L. Altered cytokine network in gestational diabetes mellitus affects maternal insulin and placental–fetal development. J Diabetes Complicat 2016.
- Kaneto H, Nakatani Y, Kawamori D, Miyatsuka T, Matsuoka TA, Matsuhisa M, Yamasaki Y. Role of oxidative stress, endoplasmic reticulum stress, and c-Jun N-terminal kinase in pancreatic beta-cell dysfunction and insulin resistance. Int J Biochem Cell Biol 2006; 38: 782-793.
- Houstis N1, Rosen ED, Lander ES. Reactive oxygen species have a causal role in multiple forms of insulin resistance. Nature 2006; 440: 944-948.
- Ma R, Chou X. The impact of gestational diabetes on offspring heart. Chinese Med Innovat 2014; 11: 150-153.
- Chang Y, Zhu X. Changes in Raman spectroscopy gestational diabetes placental tissue proteins contemplated use. Chinese J Diabetes 2008; 16: 294-296.
- Chartoumpekis DV, Ziros PG, Psyrogiannis AI, Papavassiliou AG, Kyriazopoulou VE, Sykiotis GP, Habeos IG. Nrf2 represses FGF21 during long-term high-fat diet-induced obesity in mice. Diabetes 2011; 60: 2465-2473.
- Shen C, Liu X. Gestational diabetes and placenta microvilli morphological and ultrastructural changes. Chinese J Pathol 2011; 40: 856-859.
- Russo LM, Nobles C, Ertel KA, Chasan-Taber L, Whitcomb BW. Physical activity interventions in pregnancy and risk of gestational diabetes mellitus: a systematic review and meta-analysis. Obstet Gynecol 2015; 125: 576-582.