Research Article - Current Pediatric Research (2017) Volume 21, Issue 1
Invasive neonatal Group B streptococcal infection, over a 10 year period, in West Hertfordshire, UK.
Charlene MC Rodrigues1,2, Sabita Parida3, Sankara Narayanan4*
1Department of Paediatric Immunology and Infectious Diseases, Great North Children’s Hospital, Newcastle Upon Tyne, UK.
2Department of Zoology, University of Oxford, South Parks Road, Oxford, UK.
3Department of Microbiology, Watford General Hospital, Watford, UK.
4Department of Paediatrics, Watford General Hospital, Watford, UK.
- *Corresponding Author:
- Sankara Narayanan
Department of Paediatrics
Watford General Hospital
Watford, United Kingdom.
Tel: +441923 217392
Email: cnarayanan@nhs.net
Accepted date: January 30, 2017
Abstract
Introduction: Group B Streptococcus (GBS) infection is the most important cause of neonatal infection in developed and developing countries. UK National guidance for the prevention of neonatal GBS infection was published in 2003. This surveillance study aimed to assess the burden of invasive neonatal GBS disease over a decade in a single UK county. Method: A retrospective analysis was done of GBS positive cultures from blood and cerebrospinal fluid in babies aged 0-89 days, from 1 January, 2004 to 1 January, 2014. Notes were reviewed and a standard proforma completed by a clinician to identify patient demographics, clinical features, clinical course, treatment and outcome. Results: There were 41 cases of GBS disease, with an overall incidence of 0.73 per 1000 live births and 17% (n=7) had GBS meningitis. Intrapartum antibiotic prophylaxis was given to 25% (n=4) of eligible mothers. Treatment was for appropriate duration, with exception for severe clinical features. Our outcome of GBS meningitis was favourable, with 14% mortality. Conclusion: The rates of early onset disease 0.46 per 1000 and late onset disease 0.27 per 1000 live births are in keeping with other national studies of UK incidence. However, this trend is increasing and improvements are needed for better prevention of GBS disease.
Keywords
Group B streptococcus, Intrapartum antibiotic prophylaxis, Neonatal infection, Streptococcus agalactiae, United Kingdom.
Abbreviations
CRP: C-Reactive Protein; CSF: Cerebrospinal Fluid; GBS: Group B Streptococcus; EOD: Early Onset Disease; IAP: Intrapartum Antibiotic Prophylaxis; LOD: Late Onset Disease; NICE: National Institute for Clinical Excellence; RCOG: Royal College of Obstetricians and Gynaecologists; UK: United Kingdom.
Introduction
Group B Streptococcus (GBS) remains the most significant pathogen causing early onset sepsis in neonates in both developed and developing countries. Early onset disease (EOD) is characterised by presentation between days 0-6 of life and late onset disease (LOD) from day 7-89. Rates of GBS infection in England and Wales have risen in the last decade, with EOD increasing from 0.28 to 0.41 per 1000 live births and LOD increasing from 0.11 to 0.29 per 1000 live births [1].
In the UK, it is estimated that 21% of women have vaginal GBS carriage [2]. The methods for risk reduction of invasive GBS disease in the industrialised countries include universal antenatal screening for maternal vaginal carriage of GBS between 35-37 weeks gestation and appropriate antibiotics therapy. Such screening methods are not employed in the UK on the basis of insufficient evidence that it would reduce the burden of disease in the UK [3]. The Royal College of Obstetricians and Gynaecologists (RCOG) recommend a risk-based approach with selective intrapartum antibiotic prophylaxis (IAP) published in 2003 and updated in 2012 [4].
This study sought to investigate the incidence, presentation, and maternal demographics of infants who develop invasive GBS disease within a district in UK.
Method
This retrospective surveillance study identified cases from 1 January 2004 to 1 January 2014. The RCOG guidance was introduced in 2003 so it was presumed that the data collected reflected practice adhering to this guidance in Watford General Hospital, West Hertfordshire. This district general hospital serves a population of 542,600, with between 5316-5947 live births per year and a total of 56,489 live births in ten years [5].
Microbiological records were interrogated to identify infants, aged 0-89 days, who had GBS positive cultures from sterile sources, i.e. blood, cerebrospinal fluid (CSF), urine, bone or joint aspirates. For each patient, relevant maternal and neonatal data was collected using a standardised template, notes were available for 35 infants (85.4%).
Microbiological records were interrogated to identify infants, aged 0-89 days, who had GBS positive cultures from sterile sources, i.e. blood, cerebrospinal fluid (CSF), urine, bone or joint aspirates. For each patient, relevant maternal and neonatal data was collected using a standardised template, notes were available for 35 infants (85.4%).
Socioeconomic background was assessed from maternal postcode at the time of birth through http://tools.npeu. ox.ac.uk/birthplace-imd/. Data was analysed using statistical software STATA version 11. Study was performed as a service evaluation tool and hence ethics committee approval was not required.
Results
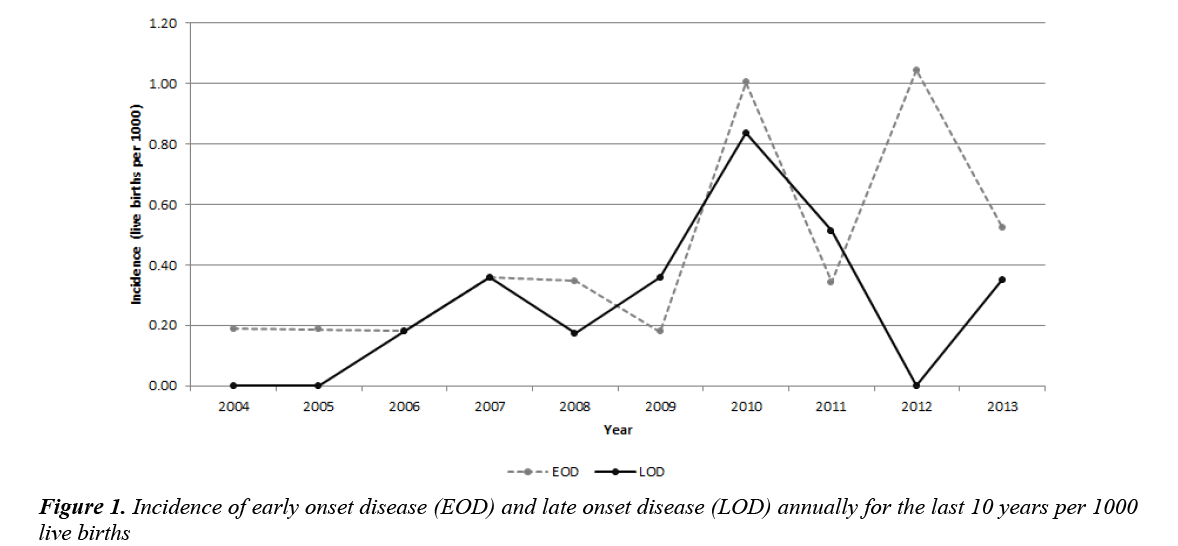
There were 41 cases of invasive GBS disease identified between 1st January, 2004 to 1st January, 2014. The overall incidence of GBS disease in West Hertfordshire was 0.73 per 1000 live births over this decade. The incidence of EOD increased from 2004 to 2014 with peaks in 2010 and 2012 to over 1 per 1000 live births (Figure 1). Mean birth weight in the whole cohort was 3.24 kg (± SD 0.92 kg). Of these births, 29.27% (n=12) were preterm (<37+0 weeks gestation). In all 41 cases, GBS septicaemia was diagnosed following positive blood cultures. For seven babies an additional diagnosis of GBS meningitis was made, four following identification of GBS in CSF culture and three with CSF pleocytosis and negative CSF culture, antibiotics had been commenced prior to lumbar puncture in these three children.
EOD and Risk Factors
Incidence of EOD was 0.44 per 1000 live births (Figure 1). In all cases of EOD, illness was identified and treatment commenced within the first two days of life. Prematurity was identified in 21.95% (n=9) of EOD cases. Other risk factors identified in these pregnancies included; GBS on vaginal swab in current pregnancy 14.63% (n=6, opportunistic screening due to lower urinary symptoms in pregnancy, not all women in this study were screened), maternal pyrexia >38°C 14.63% (n=6) but no women had GBS bacteriuria in current pregnancy or previously had a neonate with invasive GBS disease.
There were 17 mothers who were eligible for intrapartum antibiotic prophylaxis (IAP) according to the RCOG guidelines [4]. Adequate benzylpenicillin prophylaxis was given to four mothers (23.53%) only. Two mothers had oral erythromycin. Of the remaining 11 mothers who should have received IAP, seven had babies who developed EOD and four had LOD. Therefore, given the efficacy of IAP is estimated to be 80%, had the all the mothers had adequate and timely IAP, five to six cases of EOD could have potentially been prevented [6].
LOD
There were 16 babies who developed LOD from day 7-89 of life. The incidence of LOD was 0.28 per 1000 in this cohort (Figure 1).
Maternal Demographics
The mean maternal age was 30.45 years (SD ± 3.73). The ethnicity was predominantly white British (64.29%), with 17.86% of Indian origin. The remaining 17.85% were evenly distributed between the following ethnic groups: Bangladeshi, Jewish, European, Black African and Pakistani.
Analysis of Index of Multiple Deprivation (IMD) identified that the median score was 11.21 which is within the 2nd quintile (1st quintile represents the least deprived). The 25th and 75th percentile spanned the 1st to 3rd quintile suggesting the poverty was not a contributing factor to the development of maternal GBS carriage or neonatal disease in our cohort. No mothers in this study tested HIV positive when they booked with maternity services at the start of pregnancy.
The majority of babies were delivered vaginally, 17 by spontaneous vaginal delivery (51.52%) and four (12.12%) by instrumental assisted vaginal delivery (forceps or ventouse). There were 17 babies born by caesarean section, 48.48% by emergency caesarean section and 3.03% by elective caesarean section.
Presentation
Babies presented to a variety of different hospital settings. All EOD was identified within 24 hours of life. Five (12.20%) babies were screened asymptomatically at birth due to risk factors for infection identified at the delivery by the neonatal doctor. Another three babies (7.32%) were born in “poor” condition, requiring resuscitation disproportionate to the preceding history and information available. In these cases the clinicians started the baby on antibiotics suspecting that infection was, at least in part, responsible for the need for resuscitation. All other babies had been symptomatic and a neonatal doctor called to review them in the first 48 h of life.
All LOD presented to the children’s emergency department, as symptomatic babies seen by a paediatrician. Respiratory distress, temperature instability and poor feeding were the three most common presenting features of GBS disease in both EOD and LOD cohorts.
Investigations
All babies in this cohort were treated as “suspected sepsis” and had antibiotics commenced at the point the blood cultures were taken, therefore there was no delay starting therapy. A lumbar puncture was documented in 25 cases (60.98%). There were seven cases of GBS meningitis, four diagnosed with positive CSF cultures and three with CSF pleocytosis (white cell count 320, 440, 2288 × 109/ml respectively) and negative CSF cultures.
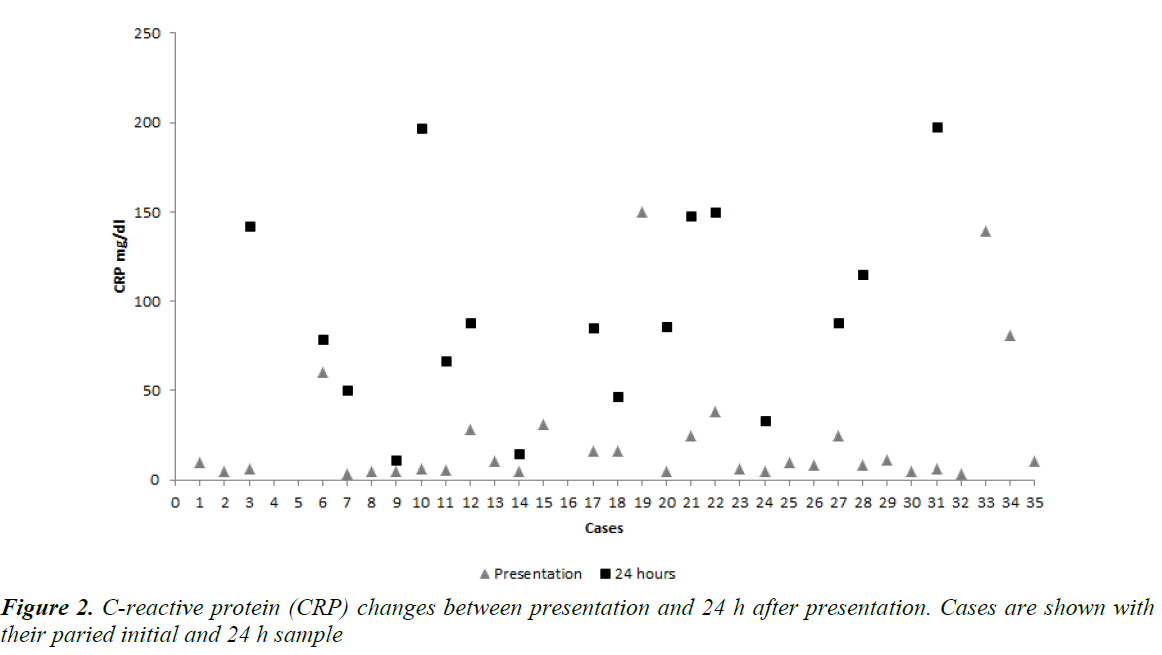
Inflammatory markers were measured in these babies as part of the initial work-up and ongoing assessment. The initial C-reactive protein (CRP) was compared to the paired value in the same patient 24 h later. Mean initial CRP was 23.43 mg/dl (SD ± 36.13mg/dl) increasing to 98.94 mg/dl (SD ± 59.85 mg/dl) 24 h later, p<0.0001, paired t-test (Figure 2).
The same process was followed for serum white cell count. The mean white cell count on presentation was 11.27 × 109/ml (SD ± 7.47 × 109/ml). There were only four patients who had a repeat in 24 h and the mean was 16.50 × 109/ml (SD ± 11.72 × 109/ml). The increase did not reach statistical significance, likely due to the small number of samples but increased white cell count has been shown not a reliable marker of infection in neonates [7,8].
Management
For all babies who were identified as being septicaemic, antibiotics were commenced immediately. Intravenous benzylpenicillin and gentamicin are administered as empirical antibiotics for neonatal sepsis. Thirty-five children were commenced on this regimen, with the remaining six given ceftriaxone (n=3) or cefotaxime (n=3). Duration of antibiotic treatment varied within this cohort, with almost half the children (n=20, 48.78%) receiving seven days of treatment. All children diagnosed with GBS meningitis and septicaemia were treated for a minimum of 14 days (n=3), the others received, 21 days (n=2) and 42 days (n=1, this child had infective subdural collections), respectively.
Additional strategies were needed to manage neonates with sepsis, including respiratory and cardiovascular support. In 25 babies, no respiratory support was needed, 11 (26.83%) required intubation and ventilation, three (7.32%) needed continuous positive airway pressure support and three (7.32%) received oxygen therapy. Inotropic support was required in 14.63% of babies.
Outcome
Information regarding short and long term outcomes for these children was obtained from the medical records and documentation of outpatient follow up. Information was located for 30 patients (73.71%), with the remaining 11 patients lost to follow up. Within our cohort, 24 were unaffected, with five babies having neurological sequelae and one baby who died a few hours after presenting in cardio-respiratory arrest on day 20 of life.
The five children with neurological complications had deficits that ranged from mild developmental delay to spastic quadriplegic cerebral palsy. It should be noted that only one of the children with neurological sequelae had GBS meningitis. The other four were premature infants with GBS septicaemia and other complications of prematurity.
Discussion
The incidence of invasive GBS disease has steadily increased over the last decade across West Hertfordshire. The rates of EOD, 0.44 per 1000 and LOD, 0.28 per 1000, live births reflect similar national levels of 0.41 per 1000 live births and 0.29 per 1000 live births for EOD and LOD, respectively [1]. This is in contrast to the most recent US incidence of EOD 0.24 per 1000 live births and LOD 0.32 per 1000 live births in 2012 [9]. It is of note that in 1996, the US introduced universal screening for GBS at 35-37 weeks into pregnancy and women offered antibiotic prophylaxis accordingly [10]. With the UK following a risk-based approach to targeted intrapartum antibiotic use, the incidence both locally and nationally of EOD remains higher. It is understood that IAP does not affect LOD and this may reflect other factors within the two populations. It is interesting to note that Northern Ireland has higher incidence of EOD of 0.57 per 1000 live births which may contribute to the higher overall UK incidence compared to the England and Wales alone [11]. It would be prudent to note that the true incidence of invasive GBS disease may indeed be higher than that reported in most studies due to the number of cases that fail to be microbiologically confirmed. We start treatment on many neonates whose cultures, although taken prior to antibiotic administration, show no bacterial growth, suggesting amount of blood sampled and culturing techniques could be implicated.
It is well understood that EOD can be prevented by identification of risk factors and IAP. In a study by Heath et al., 58% of mothers of babies with EOD were identified as having risk factors. We found 43.90% of mothers of babies with EOD had risk factors (including prolonged rupture of membranes, although this is no longer an indication for IAP in isolation) [4]. We also found suboptimal use of IAP for mothers at risk and a theoretical calculation of case prevention of five to six cases, had timely and appropriate IAP been given. Similar findings on a larger scale were reported by other UK units and highlight the need for improved prevention strategies in the UK [12].
Maternal GBS carriage rates are difficult to study in the UK as there is no national screening programme; estimates are ~20% [2,13,14]. The association between socioeconomic deprivation, maternal GBS vaginal carriage and subsequent neonatal GBS disease is unclear. In a study in South Bedfordshire, neonatal GBS surveillance was carried out between 1993 and 1998. Which noted the high incidence may be due to the relative deprivation of the cases compared to the local population [15]. In Our geographically adjacent study, found the IMD score to be in the three lowest quintiles (least deprived) for 75% of the cases.
CRP is a frequently used inflammatory marker in both adult and paediatric settings. Current National Institute of Clinical Excellence guidelines (NICE) suggests repeating the CRP at 18-24 h after starting antibiotics, and lumbar puncture is indicated if CRP >10 mg/l [16]. Our data supports the use of serial CRP monitoring to guide treatment in neonates with GBS infection and inform the need for lumbar puncture.
Treatment of neonatal sepsis is commenced empirically when a neonate is identified as unwell or risk factors are noted in an asymptomatic child. NICE guidance is for intravenous benzylpencillin (25 mg/kg) 12 hourly and gentamicin (5 mg/kg) 36 hourly [16]. Duration of antibiotics varies depending on the presence or absence of meningitis. GBS septicaemia should be treated for minimum seven days. GBS meningitis should be treated for minimum 14 days. All babies in our cohort fulfilled these criteria and if duration of antibiotics exceeded seven or 14 days, it was based on clinical judgement of incomplete resolution of infection.
Outcomes following GBS meningitis have remained relatively bleak for the last three decades. A contemporaneous study from the US reported that over half (56%) of GBS meningitis survivors demonstrated age-appropriate development [17]. Although development was not formally measured in the follow up of our patients, the paediatrician’s developmental assessment deemed five (71%) children to be unaffected. They report 19% severely impaired survivors compared to 14% in our study [17]. Mortality data for meningitis in <90 day olds in the UK identifies a case fatality ratio of 5% for GBS meningitis, in contrast to the case fatality ratio in our cohort of 14% (n=1) [18]. This may be due to the small number of GBS meningitis cases in our study (n=7). We await with anticipation the British Paediatric Surveillance Unit report on the UK surveillance of GBS disease which will no doubt have far reaching implications on antenatal care and GBS management in subsequent years. Preventative strategies including maternal vaccination remain an exciting opportunity to prevent this serious and life-threatening infection [19].
We acknowledge the limitation of this study, as a retrospective analysis over a decade, there may have been variation amongst clinicians practice based on other influences, training or informal guidelines. In addition, the obstetric adherence to the RCOG guidelines from 2003 has not been fully evaluated.
Source of Funding
All authors are employed by the NHS in England. CMCR was supported by Wellcome Trust (Grant 109031/Z15/Z).
Ethical Approval
Study was performed as a service evaluation tool and hence ethics committee approval was not required.
References
- Lamagni TL, Keshishian C, Efstratiou A, et al. Emerging trends in the epidemiology of invasive group B streptococcal disease in England and Wales, 1991-2010. Clinical Infectious Diseases: An Official Publication of the Infectious Diseases Society of America. 2013; 57: 682-688.
- Colbourn T, Gilbert R. An overview of the natural history of early onset group B streptococcal disease in the UK. Early human development. 2007; 83: 149-156.
- UK National Screening Committee. Group B Streptococcus: The UK NSC policy on Group B Streptococcus screening in pregnancy. London: 2008.
- Hughes RBP, Heath P. On behalf of the Guidelines and Audit Committee of the Royal College of Obstetrics and Gynaecology. Prevention of neonatal early onset group B streptococcal disease. RCOG Guideline No 36. London: Royal College of Obstetrics and Gynaecology 2003.
- Public Health England. Health Protection Profiles, Summary Information, East of England, West Hertfordshire 2016.
- Benitz WE, Gould JB, Druzin ML. Antimicrobial prevention of early-onset group B streptococcal sepsis: estimates of risk reduction based on a critical literature review. Pediatrics 1999; 103: e78.
- Hornik CP, Benjamin DK, Becker KC, et al. Use of the complete blood cell count in early-onset neonatal sepsis. Pediatric Infectious Diseases Journal 2012; 31: 799-802.
- Hornik CP, Benjamin DK, Becker KC, et al. Use of the complete blood cell count in late-onset neonatal sepsis. Pediatric Infectious Diseases Journal 2012; 31: 803-807.
- Centers for Disease Control and Prevention. ABCs Report: Group B Streptococcus [CDC web site]. 2012.
- Centers for Disease Control and Prevention. Prevention of perinatal group B streptococcal disease: a public health perspective. Centre for Disease Control and Prevention 1996.
- Eastwood KA, Craig S, Sidhu H, et al. Prevention of early-onset Group B Streptococcal disease - the Northern Ireland experience. BJOG: An International Journal of Obstetrics and Gynaecology 2015; 122: 361-367.
- Vergnano S, Embleton N, Collinson A, et al. Missed opportunities for preventing group B streptococcus infection. Archives of Disease in Childhood: Fetal and Neonatal edition 2010; 95: F72-73.
- Hassan IA, Onon TS, Weston D, et al. A quantitative descriptive study of the prevalence of carriage (colonisation) of haemolytic streptococci groups A, B, C and G in pregnancy. Journal of Obstetrics and Gynaecology: The Journal of the Institute of Obstetrics and Gynaecology 2011; 31: 207-209.
- Jones N, Oliver K, Jones Y, et al. Carriage of group B streptococcus in pregnant women from Oxford, UK. Journal of clinical pathology 2006; 59: 363-366.
- Beardsall K, Thompson MH, Mulla RJ. Neonatal group B streptococcal infection in South Bedfordshire, 1993-1998. Archives of Disease in Childhood Fetal and Neonatal Edition. 2000; 82: F205-207.
- National Institute for Clinical Excellence. Antibiotics for early-onset neonatal infection 2012.
- Libster R, Edwards KM, Levent F, et al. Long-term outcomes of group B streptococcal meningitis. Pediatrics 2012; 130: e8-15.
- Okike IO, Johnson AP, Henderson KL, et al. Incidence, etiology and outcome of bacterial meningitis in infants aged <90 days in the United kingdom and Republic of Ireland: Prospective, enhanced, national population-based surveillance. Clinical Infectious Diseases: An Official Publication of the Infectious Diseases Society of America 2014; 59: e150-157.
- Nuccitelli A, Rinaudo CD, Maione D. Group B Streptococcus vaccine: State of the art. Ther Adv Vaccines 2015; 3: 76-90.