- Biomedical Research (2014) Volume 25, Issue 1
Gynecological surgeries in patients with rheumatic diseases: A matched case control study of perioperative characteristics.
DongYan Li, Min Hao and XiaoFeng Li*Second Hospital, Shanxi Medical University, No. 382 Wuyi Road, Taiyuan 030001, China
- *Corresponding Author:
- XiaoFeng Li
Second Hospital, Shanxi Medical University
No. 382 Wuyi Road, Taiyuan, 030001, China
Accepted date: November 20 2013
Abstract
To analyze and evaluate perioperative characteristics in gynecological patients complicated with rheumatic diseases, 34 gynecological patients complicated with rheumatic diseases who received surgical treatment in the Second Hospital of Shanxi Medical University from January 2002 to October 2012 were selected as study group, and 34 patients with similar- gynecological diseases served as control group. Preoperative erythrocyte sedimentation rate (ESR), average operation time, average amount of intraoperative bleeding and postoperative complications in all patients were analyzed retrospectively. There were significant changes in the preoperative ESR in the study and control group(19.97±11.97 mm/H vs. 9.91±2.02 mm/H). There were no significant differences in the average operation time or average amount of intraoperative bleeding (P>0.05), but the incidence of postoperative complications was significantly higher in the study group (29.41%) than the control group (5.88%) (P < 0.05). Gynecological patients complicated with rheumatoid disease can tolerate gynecological surgery, but patients with increased preoperative ESR have a greater risk for postoperative infections.
Keywords
Rheumatic disease; Gynecological surgery; Perioperative period
Introduction
Most rheumatic diseases are more common in women during child-bearing period, perimenopausal period and postmenopausal period [1]. These autoimmune diseases affect multiple systems and organs with complex clinical features as well as repeated and delayed course of disease. With the progress in treatment means, rheumatic disease has been controlled effectively, and the life span of patients has been prolonged, and the requirement on living quality has been promoted, and patients with the need to adopt operative treatment are increasing [2]. However, due to autoimmune disorders in patients with rheumatic disease and use of hormone, immunosuppressor and non-steroid anti-inflammatory drug, intraoperative haemorrhage and postoperative infection occur easily in such patients, which is one of the contraindications in gynecological operation. In recent years, with improved technology of gynecological operation and occurrence of new narcotic, hemostatic and anti-infective drugs, operative treatment is also given to these patients; but how to deal with the perioperative period of these patients and what are clinical characteristics during perioperative period have not been reported yet. This article was to analyze clinical data of 34 gynecological patients complicated with rheumatic disease diagnosed and treated by our hospital and rheumatism immunity division accurately in the past 10 years and to investigate the treatment and clinical characteristics during perioperative period.
Materials and Methods
General data
A total of 34 patients, aged 26-73 years, were selected from Gynaecology Department of the Second Hospital of Shanxi Medical University from January 2002 to October 2012. They were diagnosed with rheumatic disease by doctors from Rheumatism Department. 34 patients (26-72 years) with similar gynaecological disease were served as control group. In 34 patients with rheumatic disease, there were 15 cases of rheumatoid arthritis, 4 dermatomyositis, 8 systemic lupus erythematosus, 2 primary Sjgren syndrome, 2 ankylosing spondylitis, 2 mixed connective tissue disease and 1 scleroderma. The gynecological disease involved uterine fibroid in 13 patients, ovary serous cystadenocarcinoma in 4 patients, pelvic organ prolapse in 3 patients, ectopic gestation in 5 patients, benign ovarian tumor in 4 patients, cervical squamous cell carcinoma in 1 patient, endometrial polyp in 1 patient, endometrioid adenocarcinoma in 1 patient and cervical intraepithelial neoplasias in 2 patients.
Treatment in perioperative period
1) Preoperative observations
All patients of the study group had suffered from rheumatic disease for 1-32 years. 8 patients took prednisone and methylprednisolone of glucocorticoid orally before operation, 5 patients took immunodepressant orally, 3 patients took non-steroid anti-inflammatory drug (celecoxib) orally, 2 patients took traditional Chinese medicine (TGP); the other patients did not receive medication. Blood routine, urine routine, hepatorenal function and erythrocyte sedimentation rate(ESR) were examined before operation.
2) Intra-operative findings
All patients received general anesthesia. No difference existed in medication for intra-operative anesthesia between the two groups. The operation time and intra- operative bleeding amount was retrospectively analyzed; the intra-operative bleeding amount was calculated as per the amount recorded by aspirator and the number of gauzes and rectal pads; and the blood wetted area of 10*10cm was calculated as per 10ml; each gauge (10 cm in side length) and rectal pad (composed of 10 gauges) was square [3]; and therefore, each wetted gauge and wetted rectal pad was calculated as per 10ml and 100ml bleeding, respectively.
3) Postoperative findings: intravenous drip of 1.5g cefuroxime, the second generation of cephalosporin was given routinely to all the patients after surgery, bid to prevent infection; and the patients who orally took drugs for rheumatic disease were given continuously the oral agents. Furthermore, the patients were conducted to exercise in the early period of postoperation. Complications including postoperative secondary infection and incision disruption were recorded, in which the infection was judged based on the absence and presence of fever which referred to the condition with postoperative body temperature > 38.5 for more than 3 days [2]. For the patients with postoperative body temperature > 38.5, blood culture was carried out for examination. Generally speaking, blood routine and urine routine examination were given within 3 days after operation.
4) Follow-up visit for checking whether rheumatic disease was worsened within 3 months after operation.
Statistical analysis
SPSS 13.0 statistical software was adopted to process the
data, and all measurement data were expressed as 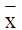 ±S;
χ2 test or Fisher exact probability was adopted for counting
data, and t test was employed for measurement data;
and the difference with P<0.05 was considered statistically
significant.
±S;
χ2 test or Fisher exact probability was adopted for counting
data, and t test was employed for measurement data;
and the difference with P<0.05 was considered statistically
significant.
Results
General comparison
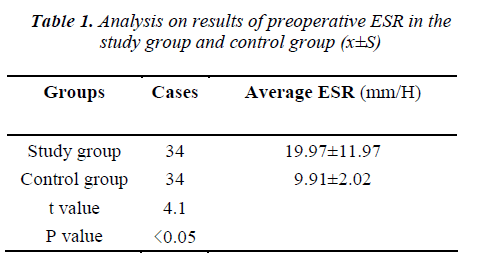
The average age (50.86±15.93) of the patients in the study group was not significantly different from that (51.06±15.37) in control group (P>0.05). There was also no difference in the constituent ratio of disease between the two groups (P>0.05). While a significant difference was found in preoperative ESR between the two groups (P<0.05), as shown in Table 1. No abnormal hepatorenal function, urine routine or blood routine was found in both groups before operation.
Analysis on intra-operative conditions
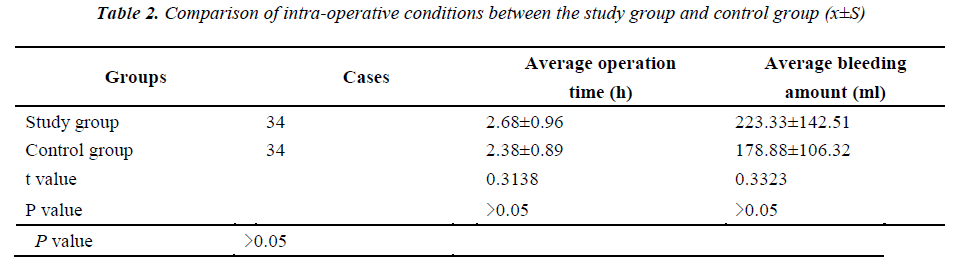
All intra-operative vital signs of the two groups were stable; and no significant difference was found in the average operation time and bleeding amount between the two groups (P>0.05); see Table 2.
Analysis on postoperative complications in patients with rheumatic disease
The main postoperative complication of both groups was postoperative fever; 10 of 34 patients with rheumatic disease had postoperative fever, and 2 patients receiving gynecological operation in the corresponding period got fever. They were all healed after operation and discharged from the hospital. The incidence of postoperative complications in the study group and control group was 29.41% and 5.88%, and the difference was considered statistically significant (P<0.05). See Table 3.
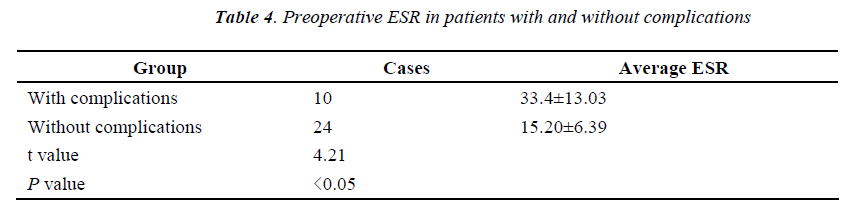
For the patients showing postoperative complications in the study group, the result of preoperative ESR rose obviously, and a significant difference can be observed compared with the patients without postoperative complications (P<0.05); see Table 4.
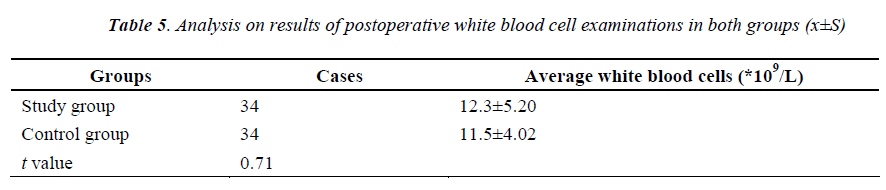
The postoperative blood routine re-examination showed that the average number of white cells in both study and control group increased compared with those before operation, but the difference was not statistically significant (P>0.05); see Table 5.
The postoperative urine routine re-examination showed that 8 patients had increased white blood cell count in patients with complications, including 6 patients from the study group and 2 patients from the control group. Blood culture was performed in patients exhibiting postoperative fever, among them, 4 patients showed positive findings.
Discussions
Prediction of infection after surgery for rheumatic disease
The onset of the rheumatic disease is relevant to environment, virus, heredity, sex hormone and mental state and is accompanied by various gynecological diseases such as cervical lesions, ovarian cancer and hysteromyoma, etc [4-6]. When gynecological disease needs the operative treatment in such patients, the probability of postoperative complications is increased due to the reduced autoimmunity and the use of immunosuppressant. It is worthy of studying how to predict the postoperative complications. ESR is normally lower than 20mm/h. It might rise in case of rheumatic disease and surgery and is relevant to the severity of the disease. The patient showing an increased ESR is at the active stage of the disease and is infected easily after surgery due to abnormal immunologic mechanism. In this study, ESR in patients of the study group increased significantly, especially the patients with postoperative complications, prompting that the patients with increased pre-operative ESR who were easily infected should be observed closely. ESR can become an indicator for preoperatively determining whether the postoperative infection occurs easily. Therefore, the surgery shall be conducted after ESR is lowered to normal as much as possible.
Impact on infective fever after surgery from treatment of rheumatic disease
Absorption fever may occur after surgery, which is non-infective fever from absorption of aseptic necrosis material in case of tissue damage and bleeding and a physiological change. Generally, the maximum body temperature should not be greater than 38.5oC., and fever should not last for more than 3 days. The abnormal condition occurs when the maximum body temperature is more than 38.5 oC and fever lasts for more than 3 days, which indicates infection may occur. The common complication is the infective fever when gynecological operation was performed after pelvic surgery, and the common types include urinary system infection, upper respiratory infection and deep pelvic infection, etc. For the patients with postoperative fever in this study, blood culture and urine routine examination were carried out correspondingly to support the diagnosis of the infection. The rise in body temperature is associated with increase rate of body metabolism and leukocyte infiltration as well as production of excitatory amino acid, free radicals and bradykinin which affect patients, rehabilitation by casing reduced immunity, increase in hospital stay and cost of care. Patients with rheumatic disease are infected easily after gynecologic operation [7]. Compared with the control group, the incidence of postoperative complications is increased in the study group, which is consistent to the above opinions. It is indicated that the incidence of postoperative infection was not affected by immunosuppressor for treating rheumatic disease [7], and use of immunosuppressor before and after the surgery is safe without stopping [8,9]. Among the patients receiving the immunosuppressor in the study group, 2 patients showed postoperative fever; considering few cases, the analysis cannot be carried out, and further observation and study is needed. In addition, improper use of glucocorticoid might lead to the infection, so the glucocorticoid shall be used as per the former dosage or increased dosage before and after surgery [10]. In the study group, 3 patients receiving glucocorticoid had postoperative fever, which might be related to the hormone dosage after surgery that was not increased. The infection risk in patients with thrombocytopenic purpura is increased if the glucocorticoid is used for more than 4 weeks [11]. Most patients with rheumatic disease need using glucocorticoid all year round [12]. However, the impact of preoperative medication time on postoperative infective fever has not been analyzed due to fewer cases, and further observation is needed. The patients with rheumatic disease and gynecological disease can tolerate regular operation and experience similar postoperative complications. Therefore, for such patients, it would be best to perform surgery during remittent stage of the disease; the emergency patients and those with malignant tumor who must be given the surgery as soon as possible are required to be observed and managed closely after surgery, thereby reducing the occurrence of complications.
References
- Oliver JE, Silman AJ. Why are women predisposed to autoimmune rheumatic diseases? Arthritis Res Ther. 2009; 11(5): 252.
- Lu ZY, Zhong NS. Internal medicine. 7th Ed People's Medical Publishing House 2008.
- Feng YJ, Shen K. Obstetrics and Gynecology. 2th Ed People's Medical Publishing House 2010.
- Dong JL, Yang NP. Study and development of rheumatoid arthritis and malignant tumor. China Medical Herald 2007; 4: 6-7.
- Rojo Contreras W, Montoya Fuentes H, Gámez Nava JI, Suárez Rincón AE, Vázquez Salcedo J, Padilla Rosas M, Baltazar Rodríguez LM, Trujillo X, Ramírez Flores M, Trujillo Hernández B, González López L. Prevalence and cervical human papilloma virus associated factors in patients with rheumatoid arthritis. Ginecol Obstet Mex 2008; 76: 9-17.
- Yang R. One report on ovarian cancer and dermatomyositis. J Oncol 2002; 8: 121.
- Joulie D, Girard J, Mares O, Beltrand E, Legout L, Dezeque H, Migaud H, Senneville E. Factors governing the healing of Staphylococcus aureus infections following hip and knee prosthesis implantation: a retrospective study of 95 patients. Orthop Traumatol Surg Res 2011; 97: 685-692.
- Scanzello CR, Figgie MP, Nestor BJ, Goodman SM. Perioperative management of medications used in the treatment of rheumatoid arthritis. HSS J 2006; 2: 141-147.
- Loza E, Martinez-Lopez JA, Carmona L. A systematic review on the optimum management of the use of methotrexate in rheumatoid arthritis patients in the perioperative period to minimize perioperative morbidity and maintain disease control. Clin Exp Rheumatol 2009; 27: 856-862.
- Pieringer H, Stuby U, Biesenbach G. Patients with rheumatoid arthritis undergoing surgery: how should we deal with antirheumatic treatment? Semin Arthritis Rheum 2007; 36: 278-286.
- Xu J, Zhao H, Su L, Ji BX, Hui WH. The risk factors of infection in patients with idiopathic thrombocytopenic purpura during treatment of glucocorticoids. Adv Drug React J 2006; 8: 252-254.
- James NG. Definition, diagnosis and treatment of immune thrombocytopenic purpura. Haematologica. 2009; 94(6): 759-762