Hyponatremia is an electrolyte imbalance common in clinical practice and is associated with impaired quality of life and survival. The aim of this study is to investigate hyponatremia-associated clinical characteristics in a hospitalized geriatric patient population. Hyponatremia was categorized as mild, moderate and severe based on serum Na levels. The relationships between severity of hyponatremia and patient age, sex, duration of hospital stay, time of hyponatremia onset and outcome were studied. A total of 978 patients aged 65 years and above were evaluated. Hyponatremia was detected in 176 patients (18%). Moderate (HR: 4.5, 95% Cl: 0.213-0.542, p<0.001) and severe hyponatremia (HR: 2.5, 95% Cl: 0.077-0.606, p<0.001) were significantly more frequent in patients with hyponatremia at the time of hospitalization. Of the etiological factors, the most common was acute renal damage and iatrogenic causes. The most common comorbidities were diabetes mellitus and hypertension. The impact of polypharmacy and impaired oral intake on hyponatremia in the geriatric population was clearly seen. We demonstrated that patients with diabetes and hypertension are at a higher risk of developing hyponatremia, and showed a significant relationship between severity of hyponatremia and the time that hyponatremia was diagnosed.
keywords |
| Hyponatremia, Geriatric patient, Etiology, Comorbidity, Hyponatremia severity. |
Introduction |
| Hyponatremia is one of the most frequent electrolyte
imbalances seen in clinical practice which is often defined as a
serum sodium (Na) measurements of <135 mEq/L [1, 2]. The
exact prevalence and incidence is not known. While it is seen
in 15-30% of hospitalized patients, more than 50% of the
overall hyponatremic population consists of hospitalized
patients [3, 4]. |
| In hyponatremia cases, it should first be established if the
patient is genuinely hyponatremic (hypo-osmolar
hyponatremia) or pseudo-hyponatremic (iso-osmolar
hyponatremia) which is observable in conditions such as
hyperlipidemia and hyperproteinemia [5]. |
| While hyponatremia can affect all age groups, its incidence
seems to be higher in the elderly due to the impaired response
of water and electrolyte homeostasis to dietary and
environmental alternations [6]. The higher frequency of
hyponatremia in the elderly population was also shown to be
associated with presence of comorbidities, physiological
changes in glomerular filtration rate, altered water metabolism
and polypharmacy [7-9]. |
| There are very few studies investigating the incidence and
prevalence of hyponatremia and addressing to risk factors
associated with hyponatremia and offering up-to-date information in our country. The objective of our study was to
determine the frequency and etiology of hyponatremia and
comorbidities in the hospitalized elderly and to investigate the
relationship between severity of hyponatremia and
demographic characteristics, hospitalization and mortality. |
Methods |
| A total of 978 patients aged 65 years and above was evaluated
in our study and included 176 geriatric patients, serum sodium
levels of whom were <135 mEq/L at the time they presented,
or dropped below 135 mEq/L over the period of hospital stay. |
| Patient files were reviewed retrospectively. Age, sex, the time
hyponatremia was diagnosed, regular medications and
medications given while the patient was hospitalized, chronic
condition history if present, diagnoses leading to hyponatremia
and volume status were documented. Duration of hospital stay
and outcome (improvement, death) were indicated. |
| Patients were identified from determined sodium values of
hospitalized patients, which were sent electronically from the
chemistry department. Sodium values were determined with
ion-selective electrodes (Hitachi 917, Roche, according to the
manufacturer's instructions) and in all of these samples plasma
osmolality and plasma glucose concentration were determined
simultaneously. In all patients the first step consisted of the
exclusion of pseudo-hyponatraemia, through analysis of plasma osmolality, total protein, triglyceride and cholesterol
concentrations. The patients were grouped according to the
severity of hyponatremia as follows: sodium levels of 126-135
mEq/L were considered mild hyponatremia, sodium levels of
116-125 mEq/L as moderate hyponatremia and sodium levels
of = 115 mEq/L as severe hyponatremia [10]. |
| The World Health Organization considers individuals aged 65
years and older within the psychogeriatric age group.
Gerontologists classify people aged 65 to 74 years as early old
age, people aged 75 to 84 years as old age and people aged 85
years older as late old age (senility) [11]. The patients were
distributed into three groups based on these data. The
frequency of hyponatremia for the internal medicine clinic of
our hospital, hyponatremia etiologies and comorbidities were
calculated as percentage rates. The relationships between
severity of hyponatremia and patient age, sex, duration of
hospital stay, time of hyponatremia onset and outcome were
studied. |
Statistical analysis |
| SPSS 22.0 software was used for statistical analyses of the
data. The data were summarized as percentages and means.
Hyponatremia prevalence in the hospitalized geriatric
population was calculated. The relationships between
hyponatremia severity and age groups, sex, duration of hospital
stay and outcome were studied using the chi-square,
independent student?s T test and Mann Whitney U tests.
Comorbidities and hospitalizations were presented as
percentages. The results were evaluated by hazard ratio and
95% confidence interval. In these analyses, p values <0.05
were considered statistically significant. |
Results |
| A total of 978 patients aged 65 years and older that admitted in
hospital were enrolled. Of the hospitalized patients, 530 (54%)
had one or more electrolyte imbalances. Hyponatremia was
detected in 176 (18%). The lowest and highest Na values were
98 mEq/L and 134 mEq/L, respectively, with a mean Na of
125.9 mEq/L. Mild, moderate and severe hyponatremia were
identified in 121 (68.7%), 41 (23.2%) and 14 (7.9%) of the
patients, respectively. Mean age of patients was 76.1 ± 7.2
years (65-95 years) overall, and was 75.8 ± 7.3 years (65-95
years) in women and 76.7 ± 7.2 years (65-92 years) in men.
Age range was 65-74 years for 84 patients (47.7%), 75-84
years for 66 (37.5%) and = 85 for 26 patients (14.8%).
Hyponatremia was considerably more common among females
(female/male: 109/67; 61.6% versus 38.4%). Duration of
hospital stay was ranging between one day and 50 days, with a
mean duration of hospital stay of 9.9 days. Hyponatremia was detected during hospital stay in 113 (64.2%) of the 176 patients
diagnosed with hyponatremia while 63 (35.8%) of the patients
developed hyponatremia between days 1 and 25 of
hospitalization (5.2 days on average). Hundred fourty four
(81.8%) patients were discharged from the internal medicine
clinical service and laboratory parameters with improvement,
while 15 (8.5%) died during stay the hospital?s internal
medicine clinical service. Seventeen (9.6%) patients required
intensive care during hospital stay. Of the patients treated in
the intensive care unit, one was discharged with improvement,
whereas 16 patients died. As a result, one hundred fourty five
(82.4%) patients were discharged from the hospital with
improvement, while thirty one (17.6%) patients were died.
There is not significant relationship between severity of
hyponatremia and mortality. But the mortality rate is
significantly high in patients who stay in intensive care unit
(p<0.001). |
| The relationships between severity of hyponatremia and
demographic characteristics, duration of hospital stay, time of
hyponatremia onset and outcome were examined: no
significant relationship observed between female and male
gender, age groups, duration of hospital stay or outcome, while
severity of hyponatremia and time of hyponatremia onset were
significantly related. Of the 113 (64.2%) patients diagnosed
with hyponatremia at the time of hospitalization, 64 (56.6%)
had mild hyponatremia, 37 (32.8%) had moderate
hyponatremia and 12 (10.6%) had severe hyponatremia. On the
other hand, of the 63 (35.8%) patients who developed
hyponatremia following hospitalization, 57 (90.4%) developed
mild hyponatremia, 4 (6.4%) moderate hyponatremia and 2
(3.2%) severe hyponatremia. Among the patients diagnosed
with hyponatremia at the time of hospitalization, moderate
hyponatremia (Hazard ratio: 4.5, 95% Cl: 0.213-0.542,
p<0.001) and severe hyponatremia (Hazard ratio: 2.5, 95% Cl:
0.077-0.606, p<0.001) was significantly more frequent (With
reference to patients diagnosed with hyponatremia after
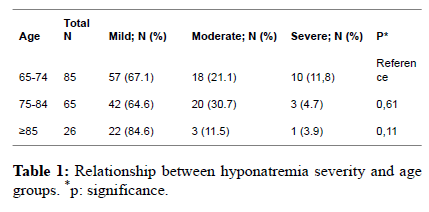
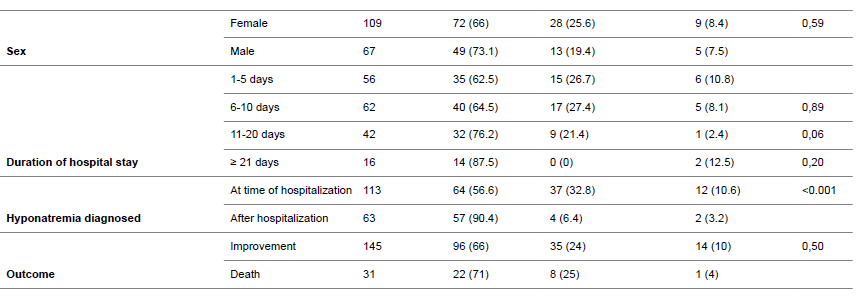
hospitalization). The relationship between hyponatremia
severity and age is shown in Table 1 and the relationship with
sex and duration of hospital stay is given in Table 2. |
 |
 |
 |
| The rates of etiology of hyponatremia were as follows; thirty
eight patients (23.3%) had infection, 87 (47.7%) had acute
renal damage (ARD), 22 (12.5%) had acute cardiac failure
(ACF), 3 (1.7%) had encephalopathy, 4 (2.2%) had hypovolemic shock, 7 (3.9%) had malignancies, 128 (72.7%)
had iatrogenic factors, 8 (4.5%) had chronic lung disease
(CLD) and 39 (22.2%) had impaired oral intake and
malnutrition (Figure 1). |
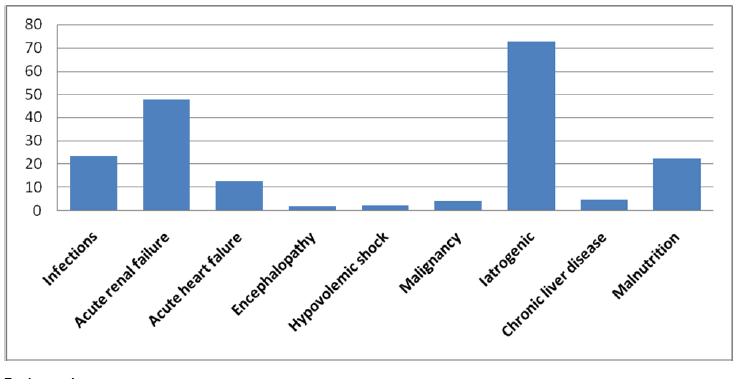 |
| Figure 1: Etiology in hyponatremia. |
| By volume status, 103 (58.5%) patients were hypervolemic, 30
(17%) were euvolemic and 43 (24.5%) had hypovolemic
hyponatremia. |
| Current comorbidities of the patients with hyponatremia were.
Ninety two patients (52.2%) had diabetes mellitus (DM), 130
(73.8%) had hypertension (HT), 30 (17%) had malignancies,
41 (23,3%) had coronary artery disease (CAD), 60 (34%) had
congestive heart failure (CHF), 87 (49.4%) had chronic kidney disease (CKD), 13 (7.4%) had CLD, 32 (18.1%) had chronic
obstructive pulmonary disease (COPD) or asthma, 10 (5.7%)
had psychiatric conditions, 12 (6.8%) had thyroid dysfunction,
23 (13%) had neurologic conditions, 15 (8.5%) had cardiac
arrhythmias, 11 (6.2%) had benign prostate hyperplasia (BPH)
and only one 1 (0.5%) patient had chronic skin disease (Figure
2). |
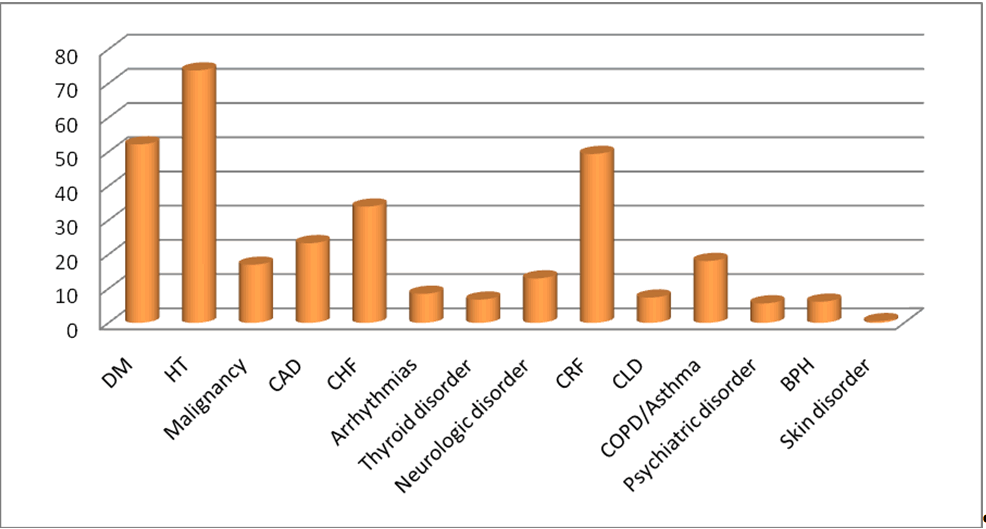 |
| Figure 2: Comorbidities in hyponatremic patients (DM: Diabetes Mellitus, HT: Hypertension, CAD: Coronary Artery Disease, CHF: Chronic
Heart Failure, CRF: Chronic Renal Failure, CLD: Chronic Liver Disease, COPD: Chronic Obstructive Lung Disease, BPH: Benign Prostatic
Hypertrophy). |
Discussion |
| The present study clearly indicated that hyponatremia in
elderly population is not uncommon. Also we demonstrated
that time of onset of hyponatremia is significantly related to the
severity of hyponatremia. Additionally the rate of mortality
among geriatric patients with hyponatremia in intensive care
unit is remarkable. |
| Hyponatremia is the most common electrolyte disorder,
particularly in the geriatric population and among hospitalized
patients [12]. Although there are conflicting reports on the
incidence and prevalence of hyponatremia due to the
differences in the considered criteria as well as in the age
ranges and populations studied, values ranging from 2.5 to
30% have been reported from the previous studies [3]. In their
3-year prospective study involving 98.411 adults hospitalized
patients, Waikar et al. (2009) identified hyponatremia in 14.290
(14.5%) patients at the time of hospitalization and noted further
5093 patients developing hyponatremia during hospital stay
(19.7% in total). Gosch et al. (2012) reported a value of 16.7%
in their study with 2280 hospitalized geriatric patients. In our
study, consistent with the literature, 530 (54%) of the 978
hospitalized patients aged 65 years and older had at least one
electrolyte disorder and 176 (18%) developed hyponatremia
[13, 14]. |
| There is a lack of consensus regarding the severity of
hyponatremia and different studies considered different ranges.
In the Singapore study, 36% of the patients had Na values of
126-135 mEq/L (mild hyponatremia), 5% had Na values of
116-125 mEq/L (moderate hyponatremia) and 1.2% had Na
values of <116 mEq/L (severe hyponatremia) [10]. Based on
the same values, mild hyponatremia was less common and moderate and severe hyponatremia were more common in our
study compared to the Singapore study. |
| We found out that the risk of moderate and severe
hyponatremia was significantly higher in the patients
diagnosed with hyponatremia at the time of hospitalization. In
a study by Hawkins (2003) and Anderson et al. (1985),
moderate and severe hyponatremia were significantly more
frequent among patients with hospital-acquired hyponatremia
[10, 15]. This suggests an impact of poor health care services,
irregular follow-up and multiple drug use in the geriatric
population. Also hyponatremia during hospital stay may be
detected in routine checks, therefore at an earlier stage. |
| Despite conflicting results have been reported from studies
investigating the relationships between risk of hyponatremia
development and severity of hyponatremia and age and sex, the
studies generally reported increased rates of hyponatremia with
increasing age [16]. Women are at a higher risk of developing
hyponatremia associated with psychotropic and the diuretic
drug was given the lower body weight as a characteristic of the
gender [17]. In our study, moderate and severe hyponatremia
was more common in the female compared to male gender,
although the relationship was not statistically significant. |
| While many studies have reported inappropriate antidiuretic
hormone (ADH) syndrome as the most common cause of
hyponatremia, multiple factors may cause hyponatremia in the
geriatric population. In their study, Padhi et al. (2014) reported
the most common cause of hyponatremia as the inappropriate
ADH syndrome (IADHS) (36.2%), followed by severe sepsis
(21.5%), trauma (21.1%) and ARD (5.9%) [18]. In a study by
Rao et al. (2010), the most common cause was IADHS (30%)
and the other factors were medications (24%) and renal losses (21%), respectively [19]. In contrast with other studies, druginduced
hyponatremia, impaired oral intake and malnutrition
and ARD-associated hyponatremia was significantly more
frequent in our study. |
| One of the leading reasons that hyponatremia is more common
in the geriatric population is the comorbidities. Mohan et al.
(2013) identified comorbidities in 73% of the patients who
developed hyponatremia. Of these patients, 51% had HT, 16%
had DM, 13% had thyroid disorders, 17% had COPD, 15% had
malignancies and 19% had psychiatric disorders while 27%
had no comorbidities [20]. Because of elderly age group in our
study, DM, HT, CAD, CKD and malignancies were more
frequent compared to the other studies. |
| Gray et al. (2014) found that patients with hyponatremia were
hospitalized for significantly longer durations compared to
normo-natremic patients, while Lim et al. (2001) did not
determine a significant relationship between sodium levels and
duration of hospital stay in their study in the geriatric
population [21, 22]. No significant relationship was determined
in our study. Even though previous studies have found out
longer durations of hospital stay for hyponatremic patients
compared to normo-natremic patients, the relationship between
hyponatremia severity and duration of hospital stay in
hyponatremic patients is not clear. This observation suggests
that underlying comorbidities rather than severity of
hyponatremia is the major determinant of hospital stay. |
| An increased risk of mortality has been demonstrated for
hyponatremic patients in previous studies. Mortality rate was
20% in a study by Clayton et al. (2006) enrolling 108 severely
hyponatremic patients, 27% in a study conducted in England
with 104 patients and 20% in a study by Rao et al. (2010) in
the geriatric population [19, 23, 24]. Consistent with the
available data, mortality rate was 17.6% in our study. |
| In addition to correcting the serum sodium, the management of
hyponatraemia must always include treatment of the
underlying cause. Severe or symptomatic hyponatraemia
should be treated as a medical emergency. While fluid
restriction is the initial treatment of choice in asymptomatic
patients, more active and urgent treatment is required in the
symptomatic patient with severe euvolaemic hyponatraemia.
Hypertonic saline should only be used in symptomatic patients
with very low serum sodium concentrations. Hypervolaemic
hyponatraemia should be easily recognizable by history,
clinical examination and the results of renal and liver function
tests. The management is to treat the underlying disease
process and will usually include fluid restriction and diuretic
therapy. The history and clinical examination will be supported
by biochemistry consistent with hypovolaemia with
hypovolaemic hyponatraemia. Treatment consists of volume
expansion with isotonic saline [25, 26]. |
| Conclusion |
| There is a growing geriatric population in our country and this
patient population is at higher risk of fluid electrolyte balance
due to organic and functional changes in the organism that occur with age. Because comorbidities and polypharmacy are
more common, and geriatric population; especially in intensive
care, is under remarkable risk of hyponatremia related
mortality, they require urgent and appropriate management. To
reduce hyponatremia-associated hospitalization, morbidity,
mortality and health care costs, older patients should be
monitored against hyponatremia at the time of hospitalization
as well as during the hospital stay. Further studies with larger
sample are essential to reach more precise conclusion. |
Conflict of Interest |
| The author has no conflict of interest. |
|
References |
- Smith MD, Mc Kenna K, Thompson JC. Hyponatremia. Clin Endocrinol 2000; 52: 667-678.
- Schrier R. The patient with hyponatremia or hypernatremia. In: Schrier RW, ed. Manual of Nephrology. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins 2000: 21-36.
- Upadhyay A, Jaber BL, Madias NE. Incidence and prevalence of hyponatremia. Am J Med 2006; 119: 30-35.
- Hoorn EJ, Lindemans J, Zietse R. Development of severe hyponatraemia in hospitalized patients: Treatment-related risk factors and inadequate management. Nephrol Dial Transplant 2006; 21: 70-76.
- Akman S, Guven AG. Hyponatremia: Clinical Evaluation and Treatment. The Journal of the Turkish Society of Nefrol 2001; 10: 68-72.
- Clayton JA, Le Jeune, IR, Hall IP. Severe hyponatraemia in medical in-patients: aetiology, assessment and outcome. QJ Med 2006; 99: 505-511.
- Fegan G, Begley J. Hyponatremia in the elderly. CME Geriatr Med 2005; 7: 76-85.
- Beck LH. The aging kidney: Defending a delicate balance of fluid and electrolyctes. Geriatrics 2000; 55: 26-28.
- Chua M, Hoyle GE, Soiza RL. Prognostic implications of hyponatremia in elderly hospitalized patients. Arc of Gerontol and Geriatricsm 2007; 45: 253-258.
- Hawkins, RC. Age and gender as risk factors for hyponatremia and hypernatremia. Clin Chim Acta 2003; 337: 169-172.
- WHO Theuses of epidemiology in the study of the elderly. WHO, Geneva, Technical Reports Series 1984; 706: 1-84.
- Thompson CJ. Hyponatraemia: new associations and new treatments. Eur J Endocrinol 2010; 162: 1-3.
- Waikar SS, Mount DB, Curhan GC. Mortality after Hospitalization with Mild, Moderate, and Severe Hyponatremia. Am J Med 2009; 122: 857-865.
- Gosch M, Gstrein BJ, Heppner HJ, Lechleitner M. Hyponatremia in Geriatric In hospital Patients: Effects on Results of a Comprehensive Geriatric Assessment. Gerontology 2012; 58: 430-440.
- Anderson RJ, Chung HM, Kluge R, Schrier RW. Hyponatremia: A prospective analysis of its epidemiology and the pathogenetic role of vasopressin. Ann Intern Med 1985; 102: 164-168.
- Liamis G, Rodenburg EM, Hofman A, Zietse R, Stricker BH, Hoorn EJ. Electrolyte Disorders in Community Subjects: Prevalence and Risk Factors. Am J Med 2013; 126: 256-263.
- Almond CSD, Shin AY, Fortescue EB, Mannix RC, Wypij D, Binstadt BA, et al., Hyponatremia among runners in the Boston Marathon. N Engl J Med 2005; 352: 1550-1556.
- Padhi R, Panda BN, Jagati S, Patra SC. Hyponatremia in critically ill patients. Indian J Crit Care Med 2014; 18: 83-87.
- Rao MY, Sudhir U, Anil Kumar T, Saravanan S, Mahesh E, Punith K. Hospital-Based Descriptive Study of Symptomatic Hyponatremia in Elderly Patients. J Assoc Physicians India 2010; 58: 667-669.
- Mohan S, Gu S, Radhakrishnan AP. Prevalence of Hyponatremia and Association with Mortality: Results from NHANES. Am J Med 2013; 126: 1127-1137.
- Gray JR, Morbitzer KA, Liu-DeRyke X, Parker D, Zimmerman LH, Rhoney DH. Hyponatremia in Patients with Spontaneous Intracerebral Hemorrhage. J Clin Med 2014 ; 3: 1322-1332.
- Lim KH, Yap KB. Hyponatremia in Hospitalised Elderly Patients. Med J Malaysia 2001;56: 232-235.
- Clayton JA, Le Jeune IR, Hall IP. Severe hyponatremia in medical in-patients: aetiology, assessment and outcome. Q J Med. 2006; 99: 505-511.
- Gill G, Huda B, Boyd A, Skagen K, Wile D, Watson I, et al. Characteristics and outcome of severe hyponatremia a case control study. Clin Endocrinol 2006; 65: 246-249.
- Sterns RH, Nigwekar SU, Hix JK. The treatment of hyponatremia. Semin Nephrol 2009; 29: 282-299.
- Verbalis JG, Goldsmith SR, Greenberg A, Schrier RW, Sterns RH. Hyponatremia treatment guidelines 2007: expert panel recommendations. Am J Med 2007; 120: 1-21.
|




