Keywords
|
| Obesity, Sleeve gastrectomy, Short-term. |
Introduction
|
| Type 2 diabetes mellitus (DM2) and its relationship with obesity have already been well-known. Twenty percent of patients who underwent bariatric surgery had DM2 and bariatric surgery has satisfying outcomes in these patients [1]. |
| Obesity is pandemic worldwide in all age groups. Although obesity and associated health problems are wellknown, it is hard to treat disease. Among treatment options are various pharmacological, non-pharmacological and surgical methods. Whereas a change in life style is the primary treatment method, surgical especially bariatric surgery methods are being used for refractory and selected cases. Both obesity and DM2 are related with many chronic diseases such as coronary heart disease, hypertension, mental disorders, hypovitaminosis of vitamin D and even cancer [2-5]. Thus, losing weight is essential to reduce lifethreatening risks [1]. Bariatric surgery helps patients to lose weight and to manage obesity-related health problems, especially type 2 diabetes mellitus, and helps them to maintain weight. The use of bariatric surgery, especially laparoscopic sleeve gastrectomy, becomes more common for the treatment of obesity-related health problems [6-7]. In this study, our aim is to evaluate the short-term (4 month follow-up) outcomes of sleeve gastrectomy in type 2 diabetic patients, comparing them with hypertensive ones and the patients without any known chronic condition, retrospectively. We evaluated the changes such as fasting blood glucose, glycated haemoglobin (HbA1c), diastolic and systolic blood pressure values, weight, body mass index (BMI), lipid profiles, glomerular filtration rate by using Modification of Diet in Renal Disease(MDRD) equation [8]. We also evaluated the rate of patients’ adherence to life-style changes such as physical activity, before and after the bariatric surgery. |
Materials and Method
|
| This study was conducted with three categories of subjects: 1) DM2 patients with minimum BMI of 40, 2) patients with isolated hypertension (HT) and 3) patients without any known chronic condition. The obesity diagnosis and treatment guidelines of the Turkish Society of Endocrinology and Metabolism were used for the planning of bariatric surgeries [9]. According to these guidelines, bariatric surgery is performed when: |
| • a patient has BMI>40 kg/m2 |
| • a patient has BMI>35 kg/m2 and co-morbidities associated with obesity, including type 2 diabetes, OSA, severe HT, cannot be controlled through medical treatment and changes in life style |
| • non-surgical methods were unsuccessful. |
| The guidelines list the contraindications of bariatric surgery as follows: |
| • untreatable major depression and psychosis |
| • drug and alcohol addiction |
| • binge eating disorder |
| • advanced heart failure |
| • severe coagulopathy |
| • lack of psychic and mental competence required to follow postoperative instructions |
| In sleeve gastrectomy, a large part of the curvature of stomach is removed and the stomach takes the form of a tube. For the purpose of this study, together with sleeve gastrectomy, perioperative control endoscopy was performed on patients to test whether there was any leakage. |
| After the patients consented to take part in the study, their age, gender and educational status were recorded. For the analysis, the values of following parameters were evaluated retrospectively before the operation and 4 months after the operation: fasting blood glucose, glycated haemoglobin (HbA1c), diastolic and systolic blood pressure, weight, body mass index (BMI), lipid profiles and glomerular filtration rate by using Modification of Diet in Renal Disease (MDRD) equation [8]. A GFR value higher than 120 ml/min is accepted as hyperfiltration [10]. |
| This study was approved by a local ethical committee according to the Helsinki Declaration. |
| We also evaluated whether there was a difference between the groups with regard to BMI, GFR and FPG values after the operation. |
Statistical Analysis
|
| The continuous data were presented in the form of Mean ± Standard Deviation, and the categorical data were presented in percentile values. Shapiro-Wilk test was used to check whether the data showed normal distribution. For the comparison of groups that did not have normal distribution, Kruskal-Wallis H test was used in cases where the number of groups was minimum three. For the comparison of values obtained in different measurement periods, Friedman’s test was used in cases where the number of groups was three. Two-way repeated measures ANOVA (One Factor Repetition) test was used for repeated measurements. Pearson’s Chi-Square and Pearson’s Exact Chi-Square tests were used for the analysis of cross tables. The software programs used for the analysis of data were IBM SPSS Statistics 21.0 and Sigma Stat 3.5. The p values less than 0.05 were reported as statistically significant. |
Results
|
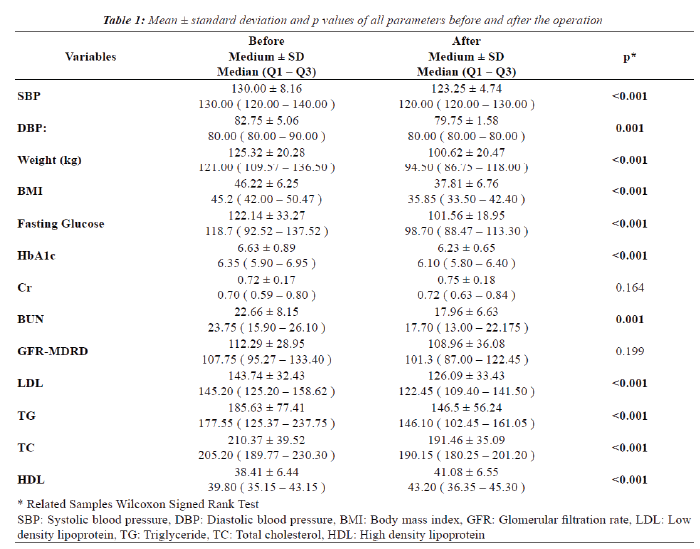
| The files of 40 participants with a BMI of 40 and over (11 men and 29 women with an average age of 38.20 ± 11.26 years) were scanned retrospectively for the purpose of this study. In this group, 8 people had isolated hypertension, 12 had DM2 and 20 had no known chronic disease. Evaluating the parameters before and after the operation, we first considered all groups together. The results indicate that, with regard to the values before the operation and four months after the operation, there were significant changes in SBP (systolic blood pressure), DBP (Diastolic blood pressure), weight, BMI, fasting glucose (FG), HbA1c, creatinine, blood urea nitrogen (BUN), LDL, TG, TC (total cholesterol) and HDL. The total weight loss according to mean values before and after the surgery was 19.71 kg. There was no significant difference in GFR values calculated using creatinine and MDRD. (Table 1 presents mean ± standard deviation and p values of all parameters before and after the operation). The average duration of operations was 115 minutes. |
| We then evaluated the difference before and after the operation individually each group i.e. the group of patients with no known chronic disease, the group of hypertensive patients and the group of diabetics. The changes in parameters of each group were compared with other groups. |
| There was a significant difference in SBP values before and after the operation in the group with no chronic disease, hypertensive group and diabetic group (the unadjusted p values were respectively 0.002, <0.001, <0.001). There is not a statistically interaction between groups and SBP parameters (p=0.065). |
 |
| When we considered the group with no chronic disease, the hypertensive group and the diabetic group individually, there was a significant difference in DBP values before and after the operation only in the group of hypertensive patients, and the difference in the diabetic group and the group with no chronic disease was not significant (the unadjusted p values were respectively <0.001, 0.059, 0.052).There is not a statistically significant interaction between groups and DBP parameters (p=0.079). |
| There was a significant difference in BMI values before and after the operation in all groups of participants (all unadjusted p values were <0.001). There is a statistically significant interaction between groups and BMI parameters (p=0.044). The change in BMI was less in the DM group compared to control and HT groups (p=0.044). |
| There was a significant difference in FG values before and after the operation in the groups of participants with no chronic disease, hypertensive and, diabetic patients (the unadjusted p values were respectively 0.023, <0.001, <0.001). There is a statistically significant interaction between groups and FG parameters (p=0.043). The change in FG was greater in the HT group compared to control and DM groups (p=0.043). |
| There was a significant difference in HbA1c values before and after the operation in all groups (all unadjusted p values were <0.001). There is a statistically significant interaction between groups and BMI parameters (p=0.044). There is not a statistically significant interaction between groups and HbA1c parameters (p=0.123). |
| There was not any significant differences in Cr, BUN, and MDRD values before and after the operation in all groups (all unadjusted p values were >0.05). A GFR value higher than 120 ml/min is accepted as hyperfiltration. While 40% of the participants had hyperfiltration before the obesity surgery, the rate decreased to 25% after the surgery (p=0.146) |
| There was a significant difference in LDL values before and after the operation in the groups of participants with no chronic disease and hypertensive patients (the unadjusted p values were respectively <0.001, =0.001). There was no difference in the diabetic group (p=0.063). There is not a statistically significant interaction between groups and LDL parameters (p=0.293). |
| There was a significant difference in TG values before and after the operation in the groups of participants with no chronic disease, hypertensive patients and diabetic patients (the unadjusted p values; <0.001, <0.001, =0.009 respectively). There was no difference in the diabetic group (p=0.063). There is not a statistically significant interaction between groups and TG parameters (p=0.317). |
| There was a significant difference in TC values before and after the operation in the groups of participants with no chronic disease and diabetic patients (the unadjusted p values were respectively <0.001, =0.001). There was no difference in the hypertensive group (p=0.193). There is not a statistically significant interaction between groups and TC parameters (p=0.449). |
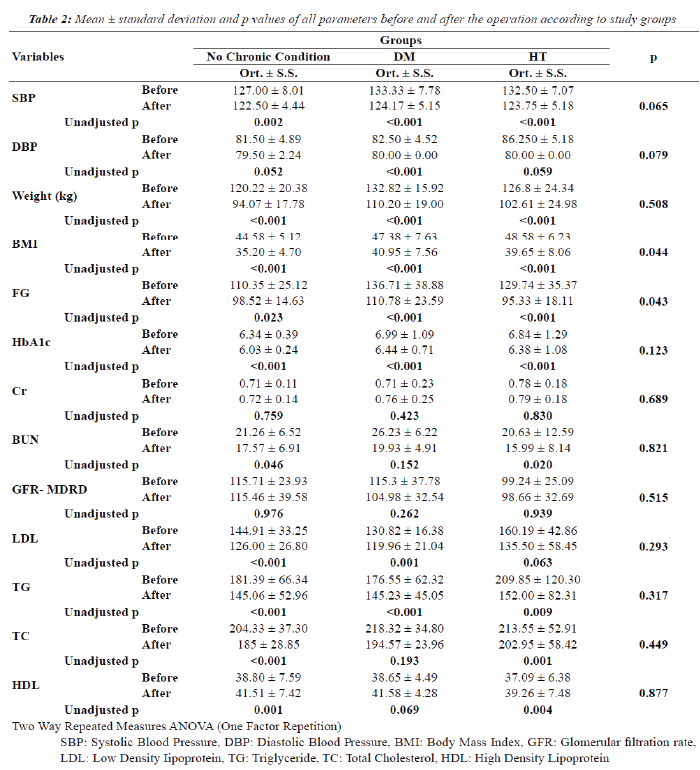
| There was a significant difference in HDL values before and after the operation in the groups of participants with no chronic disease and diabetic patients (the unadjusted p values; =0.001, =0.004, respectively). There was no difference in the hypertensive group (p=0.069). There is not a statistically significant interaction between groups and HDL parameters (p=0.877). (Table 2 presents mean ± standard deviation and p values of all parameters before and after the operation according to study groups). |
| Also, the patients were asked before and after the surgery whether they had physical activity. Whereas 25% of the patients reported that they were doing sports before the surgery, almost all patients mentioned to be doing sports after the surgery, following the advices of physicians. |
 |
Discussion
|
| Obesity and DM2 are two pandemic health problems that are closely related to each other. Changes in life style and medical treatment are main treatment approaches used. However, it is difficult to control the disease in obese DM2 patients. The American Diabetes Association (ADA) and European Association for the Study of Diabetes set out the objectives related to obesity. Yet, hypertension and high LDL values are associated problems in obese patients with DM2 [11,12]. |
| Sleeve gastrectomy is the partial removal of the stomach, particularly the curvature, and is one of the most recommended and increasingly preferred options for the treatment of severe obesity. Sleeve gastrectomy and other bariatric surgery methods contribute to weight loss as well as to recovery in associated health problems such as type 2 DM and HT [13,14]. |
| In our study, the average weight loss was 19.71 kg. Bariatric surgery procedures enable patients to lose weight by restricting the volume taken and causing malabsorption, to achieve a target weight by affecting insulin sensitivity and to maintain the target weight by causing changes in life style [14]. Weight loss is achieved in a couple of months after the surgery and continues for years. The weight loss expected in the first six months after surgery is 4.5-7 kg per months. The rapid weight loss in the first months slows down in subsequent months, and the patient’s weight starts to maintain a steady course. The weight loss may be between 5 and 80% after bariatric surgery procedures [16]. |
| Although it is still unknown how bariatric surgery causes recovery, there are some studies that point to mechanisms such as changes at the level of incretin, ghrelin secretion and increase in GLP 1 secretion [17,18]. |
| Another significant result of our study is the significant decrease in HbA1c values. There was a significant difference in HbA1c value before and after the operation in the group of patients with no chronic disease, group of hypertensive patients and group of diabetic patients (the unadjusted p values were respectively <0.001, <0.001, <0.001). In patients with DM2, medical treatment complemented by surgical treatment causes an improvement in HbA1c level, and this combined treatment helps us to achieve target values in such patients. Surgical procedures are suggested for selected cases in the ADA guidelines [12]. |
| The relationship between hypertension and obesity is well known. Weight loss owing to changes in life style and/or bariatric surgery causes recovery of hypertension associated with obesity and ensures that the recovery is maintained [19]. Particularly recovery of diastolic hypertension may be seen in 70% of hypertensive patients after the obesity surgery. In this study, while there was a significant decrease in SBP values of patients in all groups, there was a significant decrease in DBP values of only obese patients with isolated hypertension [20]. |
| Sleeve gastrectomy leads to positive impacts on DM2 patients in a short period, and regulates glucose homeostasis and increases the levels of GLP-1 and PYY [21]. |
| In this study, we evaluated the change in MRDR and renal functions, considering the values before the surgery and four months after the surgery. There was no significant difference in Cr, BUN and MRDR values before and after the surgery in the group of patients with no chronic disease, group of hypertensive patients and group of diabetics. Obese patients may suffer from hyperfiltration and pathologically high GFR values [22]. While 40% of the participants had hyperfiltration before the obesity surgery, the rate decreased to 25% after the surgery. Although the difference is not statistically significant, we thought that this may be an indicator of recovery of renal functions and this subject should be evaluated in future studies. |
| Dyslipidemia associated with obesity is a well-known cardiovascular risk factor [23]. Research has shown that there is a significant decrease in LDL, triglyceride and total cholesterol values after bariatric surgery, and some patients even give up taking lipid-lowering drugs. Supporting these findings, our study indicated a significant decrease in LDL, TC and TG values and a significant increase in HDL after the operation, which is an important finding with regard to future cardiovascular risks [20,23]. |
| The patients were asked before and after the surgery whether they had physical activity. Whereas 25% of the patients reported that they were doing sports before the surgery, almost all patients mentioned to be doing sports after the surgery, following the advices of physicians. This is a promising finding, indicating an increase in the rate of patients’ adherence to advices on life-style changes. |
| As a result, the benefits of bariatric surgery are manifest in a short period, i.e. four months, in obese patients. The significant recovery in SBP, HbA1c and lipid parameters indicates that this surgery is likely to have additional benefits for selected cases in the future. However, despite the increase in the use of bariatric surgery, change in life style is still the most important treatment for obesity, DM2 and HT. |
|
|
References
- 1. Nocca D, Guillaume F, Noel P, Picot MC, Agarwal R, El Kamel M. Impact of laparoscopic sleeve gastrectomy and laparoscopic gastric bypass on HbA1c blood level and pharmacological treatment of type 2 diabetes mellitus in severe or morbidly obese patients. Results of a multicenter prospective study at 1 year. Obes Surg 2011; 21: 738-743.
-
- 2. Simmons RK, Alberti KG, Gale EA, Colagiuri S, Tuomilehto J, Qiao Q. The metabolic syndrome: useful concept or clinical tool? Report of a WHO Expert Consultation. Diabetologia. 2010; 53: 600-605.
-
- 3. Keskin A, Bilge U. Mental disorders frequency alternative and complementary medicine usage among patients with hypertension and type 2 diabetes mellitus. Niger J Clin Pract 2014; 17: 717-722.
-
- 4. Arcidiacono B, Iiritano S, Nocera A, Possidente K, Nevolo MT, Ventura V. Insulin resistance and cancer risk: an overview of the pathogenetic mechanisms. Exp Diabetes Res 2012; 789174.
-
- 5. Bilge U, Ünalacak M, Ünlüoglu I, Ipek M, Çeler Ö, Akalin A. Relationship between 1,25-dihydroxy Vitamin D levels and homeostatic model assessment insulin resistance values in obese subjects. Niger J ClinPract 2015; 18: 377-380.
-
- 6. Karamanakos SN, Vagenas K, Kalfarentzos F, Alexandrides TK. Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide-YY levels after Rouxen- Y gastric bypass and sleeve gastrectomy: a prospective, double blind study Ann Surg 2008; 247: 401.
-
- 7. Sjöström L, Narbro K, Sjöström CD, Karason K, Larsson B, Wedel H. Swedish Obese Subjects Study. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med 2007 ; 357: 741-752.
-
- 8. A.S. Levey, J.P. Bosch, J.B. Lewis, T. Greene, N. Rogers, D. Roth. A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group Ann Intern Med 1999 ; 130: 461-470.
-
- 9. Obesity, Dyslipidemia, Hyperyension Study Group. Obesity Diagnosis And Treatment Guidelines of the Turkish Society of Endocrinology and Metabolism 2014.
-
- 10. Delanaye P, Radermecker RP, Rorive M, Depas G, KrzesinskiJ M. Indexing glomerular filtration rate for body surface area in obese patients is misleading: concept and example. Nephrol Dial Transplant. 2005; 20: 2024-2028.
-
- 11. Brethauer SA, Aminian A, Romero-Talamás H, Batayyah E, Mackey J, Kennedy L. Can diabetes be surgically cured? Long-term metabolic effects of bariatric surgery in obese patients with type 2 diabetes mellitus. Ann Surg 2013 ; 258: 628-636.
-
- 12. Nathan DM1, Buse JB, Davidson MB, Ferrannini E, Holman RR, Sherwin R, Zinman B. American Diabetes Association; European Association for Study of Diabetes. Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation and adjustment of therapy: a consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care 2009; 32 : 193-203.
-
- 13. Mechanick JI, Youdim A, Jones DB, Garvey WT, Hurley DL, McMahon MM. American Association of Clinical Endocrinologists; Obesity Society ; American Society for Metabolic & Bariatric Surgery. Clinical practice guidelines for the perioperative nuritional, metabolic, and nonsurgical support of the bariatric surgery patient-2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity (Silver Spring) 2013; 21: S1-27.
-
- 14. Gunkova P, Gunka I, Zonca P, Dostalik J, Ihnat P. Laparoscopic sleeve gastrectomy for morbid obesity with natural orifice specimen extraction (NOSE). Bratisl Med J 2015; 116: 422-425.
-
- 15. Lim RB, Blackburn GL, Jones DB. Benchmarking best practices in weight loss surgery. Curr Probl Surg 2010; 47: 79-174.
-
- 16. Nocca D, Guillaume F, Noel P, Picot MC, Agarwal R, El Kamel M. Impact of laparoscopic sleeve gastrectomy and laparoscopic gastric bypass on HbA1c blood level and pharmacological treatment of type 2 diabetes mellitus in severe or morbidly obese patients. Results of a multicenter prospective study at 1 year. Obes Surg 2011; 21: 738-743.
-
- 17. Rubino F. Is type 2 diabetes an operable intestinal disease? A provocative yet reasonable hypothesis. Diabetes Care 2008; 31: S290-296.
-
- 18. Karamanakos SN, Vagenas K, Kalfarentzos F, Alexandrides TK. Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide-YY levels after Rouxen- Y gastric bypass and sleeve gastrectomy: a prospective, double blind study. Ann Surg 2008; 247: 401-407.
-
- 19. Carson JL, Ruddy ME, Duff AE, Holmes NJ, Cody RP, Brolin RE. The effect of gastric bypass surgery on hypertension in morbidly obese patients. Arch Intern Med 1994; 154: 193- 200.
-
- 20. Ikramuddin S, Korner J, Lee WJ, Connett JE, Inabnet WB, Billington CJ. Roux-en-Y gastric bypass vs intensive medical management for the control of type 2 diabetes, hypertension, and hyperlipidemia: the Diabetes Surgery Study randomized clinical trial. JAMA. 2013; 309: 2240-2249.
-
- 21. Peterli R, Wölnerhanssen B, Peters T, Devaux N, Kern B, Christoffel-Courtin C. Improvement in glucose metabolism after bariatric surgery: comparison of laparoscopic Roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy: a prospective randomized - trial. Ann Surg 2009; 250: 234-241.
-
- 22. Chagnac A, Weinstein T, Korzets A, Ramadan E, Hirsch J, Gafter U. Glomerular hemodynamics in severe obesity. Am J Physiol Renal Physiol. 2000; 278: F817-822. 23. Mingrone G, Panunzi S, De Gaetano A, Guidone C, Iaconelli A, Leccesi L. Bariatric surgery versus conventional medical therapy for type 2 diabetes. N Engl J Med 2012 ; 366: 1577-1585.
|

