- Biomedical Research (2010) Volume 21, Issue 3
Current concepts in the treatment of alcoholic liver disease
Ashok V Shinde* and Jayshree V Ganu1Department of Biochemistry, Sinhgad Dental College and Hospital, Pune, Maharashtra 411041
1Department of Biochemistry, Govt. Medical College Miraj, Maharashtra 416410, India
- Corresponding Author:
- Ashok V Shinde
Department of Biochemistry
Sinhgad Dental College and Hospital
Vadgaon Campus, Pune
Maharashtra 411041, India
Accepted date: February 16 2010
Abstract
Alcoholic liver disease (ALD) and its complications are still one of the most frequent causes of death in both developing and developed countries. Abstinence remains the cornerstone of management of all forms of alcoholic liver disease. Treatment modalities for both alcoholic steatohepatitis and alcoholic liver cirrhosis are insufficient. Recent research, which has elucidated the mechanisms of alcohol induced liver injury, offers the prospect of advances in the management of ALD. This review principally focuses on treatment strategies including nutritional support, corticosteroids, anti-inflammatory agents and antioxidant that have been specifically directed at the mechanism involved in the pathogenesis of alcohol related liver injury and considers their current and future role in the management of patients with various stages of ALD. Although these therapies offer a promising response for the future, none have shown consistent benefit. From our study of antioxidant therapy it appears that, antioxidant therapy is more beneficial in alcoholic hepatitis than in alcoholic cirrhosis. Consequently, liver transplantation remains the ultimate option for selected patients alcoholic cirrhosis.
Keywords
Alcoholic steatohepatitis, cirrhosis, corticosteroid, antioxidant, tumor necrosis factor, liver transplantation.
Introduction
Alcohol intake remains the most important cause of cirrhosis in the Western World [1]. The association between alcohol intake and the development of alcoholic liver disease has been well demonstrated [2,3]. Nevertheless, it has been seen that, only a minority of consistent heavy drinkers develop the most advanced form of the disease. It is therefore other factors such as gender [4], genetic background [5], and viral infection play a role in the genesis of ALD. The effects of both the duration and quantity of alcohol consumption on liver disease have also been studied extensively. In this review, we have concentrated on therapies for alcoholic liver disease and attempt to link therapeutic options to recent advances in our understanding of the pathogenesis.
Alcoholic liver Disease
The spectrum of liver damage caused by alcohol is not uniform. Classically, alcoholic liver injury comprises three major forms such as fatty liver, alcoholic hepatitis and alcoholic cirrhosis. Fatty liver is present in over 90% of binge and heavy drinkers. A much smaller percentage of drinkers progress to alcoholic hepatitis, though to be a precursor of cirrhosis. Although alcohol is considered as a direct hepatotoxin, only 10-20% of alcoholics develop alcoholic hepatitis [6].
Abstinence: The Cornerstone of therapy
Cessation of alcohol consumption or a significant reduction in alcohol intake improves histology and or survival of patients with any stage of ALD, [7] therefore; alcohol abstinence is the cornerstone of management for patients with ALD. Treatments that aim to reduce the alcohol intake in alcohol dependent patients include psychological and pharmacological approaches. Psychological treatments such as cognitive behavioral therapy and motivational enhancement therapy have been shown to reduce alcohol intake [8]. As an alternative, some patients may derive benefit from pharmacological therapy. Both acamprosate and naltrexone have been shown to reduce drinking days [9]. Disulfiram, an inhibitor of acetaldehyde dehydrogenase, has been used for many years, although with conflicting results [10].
(A) Therapy for Alcoholism
Acute alcoholic Hepatitis
The clinical syndrome of alcoholic hepatitis includes a wide spectrum of liver damage; from the asymptomatic patient with mild inflammation to the severely ill patient with fever, cholastatis, coagulopathy and leucocytosis [11].
One of the first therapeutic aspects of patient management is to treat alcohol withdrawal with benzodiazepines or related drugs. The administration of fluid, calories, vitamins and minerals is usually required. Overhydration should be avoided, as this can increase ascites, lower the plasma sodium concentration and precipitate gastrointestinal hemorrhage from varices. Vitamin K is usually administered to patients who have a prolonged prothrobmin time. Admission to a critical care unit should be considered for unstable patients. Airway protection should be assured in a patient with encephalopathy [12].
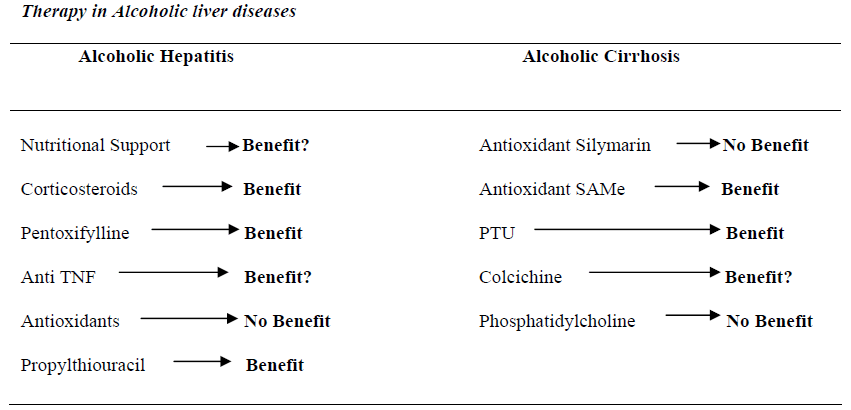
We reviewed the numerous therapies investigated in an attempt to reverse the process of acute alcoholic hepatitis. These include Nutritional support, Corticosteroids, TNF modulation, Propylthiouracil and Antioxidants.
Nutritional Support
The study found that patients who have severe proteincalorie malnutrition had a 6-month mortality rate of 20- 50%, in contrast to mildly malnourished patients in whom the mortality rate was 0%-9% [13,14]. Although individual studies have employed different nutritional formulas and different routes of administration, their chosen endpoints were similar and the results were remarkably consistent. Therefore, contrary to expectations, nutritional supplements produced little or no improvement in the survival rate [15].
Deficiencies of Vitamins and Minerals require replacement. Thiamine 50-100 mg daily may be required with Pyridoxine 100 mg daily. Folic acid is almost needed at 1- 15 mg daily.
Corticosteroids
These agents have well known effects on the immune response, and reduce cytokine production, suppress the formation of aldehyde adducts and inhibit the production of collagen [16].
Corticosteroids have been studied in several randomized double blind trials [17] and have been subject to a number of meta-analyses. Despite this intense interest, neither the source studies nor the meta-analyses have reached a sound conclusion regarding the efficacy of corticosteroids. The most recent study of Mathurin et al reanalyzed the original data (102 patients were treated with placebo and 113 were treated with steroids) [18]. The 28-day survival was higher in the corticosteroid group. This benefit was consistent during the first year of treatment but disappeared at 2 years of follow-up. Despite the apparent benefit of corticosteroids, many clinicians remain skeptical about their use.
Pentoxifylline
Pentoxifylline is a non-selective phosphodiestesase inhibitor that gives a moderate anticytokine effect attributed to a reduced transcription of the gene encodes tumor necrosis factor (TNF) [19]. The drug decreases blood viscosity, red cell and platelet aggregation and improves blood flow. Pentoxifylline is also thought to improve organ microcirculation and tissue oxygenation.
Pentoxifylline has recently been shown to improve short term (4 week) survival in a prospective randomized clinical trial of 96 patients with severe alcoholic hepatitis [20]. Mortality was associated with rising serum TNF–levels, which were reversed using pentoxifylline.
Anti-TNF Therapy
Acute alcoholic hepatitis is a potentially important indication for the use of the direct anti TNF antibody, infliximab. This monoclonal antibody binds to TNF and blocks its biological effects. To date there have been no randomized controlled trials of infliximab, however, two initial reports have demonstrated an improvement in biochemistry and satisfactory profile when used alone [21] or in combination with steroids [22]. Although early pilot studies have suggested that infliximab could be administered safely to patients with severe alcoholic hepatitis, the only randomized controlled study to date has demonstrated a higher probability of death at 2 months in those patients randomized to steroids and infliximab. In addition, there were significantly more severe infections in the infliximab- steroid group without any benefit in liver function [23]. The routine use of these therapies cannot be recommended at present, and their use should be restricted to clinical trials.
(B) Therapies for Acute Alcoholic Hepatitis and /or Alcoholic Cirrhosis
Although the high mortality of severe acute alcoholic hepatitis, coupled with the young age of many patients makes an important area for therapeutic trials, in clinical practice, most patients with ALD have advanced fibrosis or cirrhosis. The most important therapy is to achieve and maintain abstinence from alcohol [24].
Unfortunately, no adjunctive pharmacotherapies have been shown to improve survival, although some have shown promising results. As a result, the management of patients with advanced ALD, is currently directed primarily at the prevention and treatment of complications of portal hypertension, liver failure, & hepatocellular carcinoma & deciding if and when to consider patients for orthotopic liver transplantation.
Pharmacological Therapy
Antioxidants
Studies published in abstract form have failed to show that different kinds of antioxidants confer any benefit in the treatment of alcoholic hepatitis [25,26]
Turning to the use of antioxidants in the setting of cirrhosis, there have been several trials using silymarin (milk thistle) as an antioxidant. Two main trials have evaluated using silymarin, which has potent antioxidant properties in vitro and in vivo [27]. The first trial in 170 patients with cirrhosis reported a beneficial effect on survival [28]. In contrast, a later large study of 200 patients showed no benefits [29]. S-adenosyl Methionine (SAMe) which acts as both an antioxidant by replenishing GSH and a methyl donor has also been evaluated in alcoholic cirrhosis. Mato & Colleagues reported a significant beneficial effect of SAMe treatment [30]. Our study of antioxidant supplementation in ALD patients has demonstrated that, it may have more protective role in alcoholic hepatitis than in alcoholic cirrhosis [31,32]. Further trials with this agent are awaited with interest.
Propylthiouracil (PTU)
The putative mechanism of propylthiouracil to produce a benefit in alcoholics is by reducing hepatic oxygen consumption by hepatocytes. An initiation by Hallal et al found no benefit in alcoholic hepatitis [33]. Some year later December 3, 1987 Orrego et al observed that, administration of propylthiouracil reduced mortality due to alcoholic liver damage [34]. This work was done at Addiction Research Foundation Clinical Institute Toronto, Ont, Canada. For this reason and lack of any confirmatory studies, PTU has not been adopted as a treatment for alcoholic liver cirrhosis. By reviewing the literature, we found many controversial results regarding the efficacy of propylthiouracil in treating the alcoholic patients. Therefore, presently it cannot be recommended for routine use.
Colchicine
Colchicine is an anti-inflammatory and antifibrotic drug. It is of no benefit in alcoholic hepatitis, but long-term treatment of alcoholic cirrhotic patients may improve the survival rate [35]. However, a recent meta-analysis study (1138 patients) demonstrated no significant effects of colchicines on the mortality and other outcomes [36].
Phosphatidylcholine
Phosphatidylcholine has been shown to prevent alcoholic fibrosis in animals by decreasing the activation of stellate cells and stimulating collegenase activity. It can also decrease the activities of Cytochrome P4502E1 and modulate TNF-alpha, so it is beneficial for the treatment of alcoholic liver injury [37]. However a randomized, double blind, clinical trial involving 789 patients showed no effect on the progression of liver fibrosis [38].
Liver transplantation
In 1988, Starzlet et al reported a series of patients with alcoholic liver disease who underwent liver transplantation and who achieved reasonable survival. Since then, alcoholic liver disease has become the first or second most common cause of liver transplantation in the USA and Europe. Alcoholic relapse shows many problems, which frustrate both the pretransplant selection and clinical management of patients after transplant. Between 20 and 50 % of patients who receive a liver transplant acknowledge some alcohol use in the first 5 years after liver transplantation, whereas 10-15 % will resume heavy drinking [39].
Conclusions
The management of patients with ALD is challenging and rewarding. At its care are strategies aimed at achieving and maintaining abstinence, which requires close collaboration between physicians, psychiatrists and psychologists. The high mortality of severe alcoholic hepatitis highlights the need for better therapy and our increased understanding of the precise mechanism of ethanol- induced liver injury, has at last recently been translated into the development of several promising therapeutic modalities. In contrast, little progress has, as yet, been made towards the development of specific pharmacotherapy for advanced fibrosis and cirrhosis. Management of these patients is, therefore, restricted to detecting and treating the usual complications of advanced liver disease and liver transplantation when indicated. Transplantation improves survival in well-selected patients. Relapse to heavy drinking is uncommon and as yet, has not been shown to adversely affect outcome. Our study of antioxidant supplementation demonstrates the beneficial effects of exogenous antioxidants in the prognosis of ALD patients. It will definitely help the clinicians in the better management of alcoholic patients, if antioxidant supplementation is given along with the abstinence.
Acknowledgment
The encouragement and cooperation of Professor Dr Vikas Vartak (Principal) Sinhgad Dental College & Hospital Pune, Maharashtra, is very much appreciated.
References
- Grant BF and Harford TC. Epidemiology of alcoholic liver disease. Semin Liver Dis 1988; 8: 12-25.
- Lelbach WK.Cirrhosis in alcoholics and its relation to the volume of alcohol abuse. Ann. NY. Acad. Sci 1975; 252: 85-105.
- Becker U, Deis A, Sorensen TI, et al. Prediction of risk of liver disease by alcohol intake, sex and age: a perspective population study. Hepatology 1996; 23: 1025- 1029.
- Tuys A. Pequignot G.Great risk of ascitic cirrhosis in females in relation to alcohol consumption. Int J Epidem 1984; 13: 53-57.
- Grove J, Daly AK, Bassendine MF. Association of tumor necrosis factor polymorphism with susceptibility to alcoholic steatohepatitis. Hepatology 1997; 26: 143- 146.
- Anthony S Fauci, Dennis L Kasper, Dan L Longo, et al.eds.Harrison’s Principles of Internal Medicine. 17th ed, McGrawhill 2008:pp 1969-1971.
- Moyer A, Finney JW, Swearinger CE, Vergun P. Brief interventations for alcohol problems: a Meta analytic review of controlled investigations in treatment Seeking populations. Addiction 2002; 97: 279- 292.
- Herbert Tilg & Christopher P Dey. Management strategies in alcoholic liver disease. Nature Clinical Practice Gastroentero and Hepatology 2007; 4: 24-34.
- Stephen F. The management of alcoholic liver disease. Journal of Hepatology 2003; 38:: 1-10.
- Fuller RK, Branchey L, Derman RM, et al. Disulfiram treatment of alcoholism. A Veterans Administration cooperative study. JAMA1986; 19; 256 (11): 1449-1455.
- Arthur J, McCullough and JF Barry O’Connor. Alcoholic liver damage: proposed recommendations for the American college of Gastroenterology. American Journal of Gastroenterology 1998; (93), 11: 2022-2036.
- Tome S, Lucey MR. Review article: Current Management of alcoholic liver disease. Aliment Pharmacolo Ther 2004; 19: 707-714.
- Mihas AA, Heuman D. Alcoholic hepatitis. Updated April 2004. Accessed on Emedicine May 2004.
- Mendelhall CL, Tosch T, RE Weesner, et al. VA cooperative study on alcoholic hepatitis: Prognostic Significance of Protein-Calorie malnutrition. Am. J Clinc Nutri 1986; 43: 213-218.
- Rakel: Conn’s. Current Therapy 2004, 56th edition. Elsevier P. 515-516.
- Elenkov IJ. Modulatory effects of glucocorticoids & catecholamines on human interleukin-12 and interleukin- 10 production. Proc Assoc Am Phycians 1996; 108: 337-381.
- Carithers RL, Diehl AM. Methyl prednisolone therapy in patients with severe alcoholic hepatitis. Ann. Intern Med 1989; 110: 685-690.
- Matherium P, Mendenhall CL, Carithers RL. Corticosteroids improve short term survival in patients with severe alcoholic hepatitis. J Hepatol 2002; 36:480-487.
- Strieter RM, Remick DG, Ward PA, et al. Cellular and molecular regulation of tumor necrosis factor-alpha production by pentoxifylline. Biochem. Biophys Res Commun 1988; 155: 1230-1236.
- Akriviadis E, Botla R, Briggs W, Han S, Raynold T, Shakil O. Pentoxifylline improves Short-term survival in severe alcoholic hepatitis: a double blind, Placebo controlled trial. Gastroenterology 2000; 119:1638-48.
- Jalan R, Williams R, Kaser A, Davies N, Alisa A. Clinical and cytokine response to anti TNF antibody therapy in severe alcoholic hepatitis Hepatology 2001; 34: 441-443.
- Spahr L, Frossard J, Goostra E, et al. Combination of steroids with infliximab or placebo in severe alcoholic hepatitis: a randomized. controlled pilot study. J. Hepatology 2002; 37: 448-455.
- Akerman, P Cote, S Q Yang, C Mc Clain. Antibodies to tumor necrosis factor-alpha inhibit liver regeneration after partial hepatectomy. Ann. J Physiol 1992; 263: 579-585.
- Powell WJ. And Klatskin G. Duration of survival in patients with Laennec’s Cirrhosis Am J Med 1968; 44: 406-420.
- Stewart S, Prince M, Hudson M, et al. A trial of antioxidant therapy alone or with corticosteroids in acute alcoholic hepatitis J Hepatol 2002; 36: 16-18
- Mezey E, Potter J.A. Randomized placebo controlled trial of Vit E in alcoholic hepatitis. Hepatology 2003; 38: 264-266.
- Masini A. Iron induced oxidant stress leads to irreversible mitochondrial dysfunctions. The effect of Slilybin. J. Bioenergy Biomember 2000; 32: 175-182.
- Ferenci P, Dragosics B, Dittirich H. Randomized controlled trial of Silymarin treatment in patients with cirrhosis of liver.J. Hepatol 1989; 9: 105-113.
- Pares A, Planas R, Torres M, et al. Effects of silymarin in alcoholic patients with cirrhosis of liver : results of a controlled, double blind, randomized & multicenter trial. J hepatol 1998 ; 28 : 615-21.
- Mato JM, Camara J, Fernandez De Paz J, et al. Sadenosylmethionine in alcoholic liver cirrhosis.J Hepatol 1999; 30: 1081-1089.
- Shinde AV, Ganu JV, Surwanshi MK, et al. Oxidative stress and role of antioxidant
- Supplementation in alcoholic hepatitis.Med .J. D.Y.P.U 2009; (2): 35-40.
- Shinde A,.Ganu JV. Role of antioxidant supplementation in alcoholic cirrhosis induced oxidative stress. JARBS 2009; 1 (2): 46-51.
- Halle P, Pare P, Kaptein E, et al. Double blind controlled trial of propylthiouracil in patients with severe alcoholic hepatitis. Gastroenterology 1982; 82: 925- 931.
- Orrego H, Blake JE, Blendis LM et al. Long-term treatment of alcoholic liver disease with propylthiouracil. N Eng J Med 1987 (23), 317:1421-1427.
- Kershenobich D, Vargas F, Gent M, et al. Colchicine in the treatment of cirrhosis of the liver. N Eng J Med 1988; 318: 1709-1713.
- Morgan TR, Weiss DG, Nemchausky B Colchicine treatment of alcoholic cirrhosis. Gastroenterology 2005; 128: 882-890.
- Cao Q, Mak KM, Liber CS. Phosphatidylcholine decreases acetaldehyde induced TNF-alpha generation in Kupffer cells of ethanol fed rats. Biochem Biophy Res Commun 2002; 229:459-464.
- Liber CS, Wriss DG. Phosphatidylcholine in alcoholic liver disease. Alcoholism: Clinc Exp Res 2003; 27: 1765-1772.
- Pageaux GP, Micheil, V Coste et al. Alcoholic cirrhosis is a good indication for liver transplantation, even for cases of recidivism. Gut 1999; 45: 421-426.