- Biomedical Research (2015) Volume 26, Issue 2
Clinical outcomes of pelvic fractures in Uzbekistan.
Akbar B Tilyakov#,1, Tae-Woo Kim#,2, Suman K. Shrestha#,2,Ji-Hyo Hwang2, Saliyjan Z Bekchanov1,Erkin Y Valiev1, Kyeong-Dok Kang2, Supriya Jagga2, Do-Young Kim2*,Sang-Soo Lee2*1Republican Research Centre of Emergency Medicine of Republic of Uzbekistan Institution, Farhad Street, 2, Chilanzar Region, Tashkent, Uzbekistan
2Institute for Skeletal Aging & Orthopedic Surgery, Hallym University-College of Medicine, Chuncheon, 200704, Korea
- *Corresponding Authors:
- S.S. Lee
Institute for Skeletal Aging & Orthopedic Surgery
Hallym University-Chuncheon Sacred Heart Hospital
153 Gyodong, Chuncheon, Gangwon-do 200-704
South Korea - D.Y. Kim
Institute for Skeletal Aging & Orthopedic Surgery
Hallym University-Chuncheon Sacred Heart Hospital
153 Gyodong, Chuncheon, Gangwon-do 200-704
South Korea
Accepted: December 30 2014
Abstract
Pelvic bone fractures are very complex and offer challenging situations to orthopedic surgeons. The ideal treatment method for pelvic fractures remains a matter of debate till date. The objective of the present study is to introduce the treatment modalities and clinical outcomes of pelvic fractures at our center in Uzbekistan. For study, 285 patients admitted from February, 2010 to January, 2014 with pelvic injury at the head center of the Republican Research Center of Emergency Medicine of Uzbekistan were enrolled. The age of the patients ranged from 25 years to 55 years. Clinical outcomes were analyzed in 182 patients who were operated and had followed up for at least 6 months. Study population was divided into three groups according to the morphology of fracture and stability of the pelvic ring. Out of 285 patients, surgical treatments were performed in 205 (71.9%) cases. Unstable pelvic fractures were 80 (28.1%). Among the surgically managed patients, transosseous osteosynthesis by external fixator was in 103 (50.2%) cases, osteosynthesis by internal fixation was in 42 (20.5%) cases, and combined osteosynthesis was in 60 (29.3%) cases. Polytraumatized patients were 202 (70.9%). Overall mortality observed was 26 (9.1%). Clinical outcomes were excellent in 114 of the cases (62.4%) and good in 48 (26.4%). Using external fixator, surgical treatment of pelvic fracture showed satisfactory clinical outcome in Uzbekistan region. However, more combination of external fixator and internal fixation was necessary in unstable pelvic fracture compared with stable or partially stable pelvic fracture.
Keywords
Pelvis, Fracture, Treatment, External fixator.
Introduction
The acute management of a patient with pelvic fracture and unrelenting hemorrhage present a complex challenge to the orthopedic surgeons [1]. Fractures of the pelvis ring are reported to represent 4% to 8% of all fractures encountered [2,3]. These trauma are commonly associated with multiple injuries and a high mortality rate [2,4,5]. There are an increased number of incidences of pelvic ring fractures over the last decade because of rising number of high-speed accidents and trauma [3,4]. One of the main injuries at high-energy trauma is pelvic fracture which accounts for about 10% to 40% of the cases [5-8]. Mortality rate of pelvic fractures in association with multiple injuries ranges from 30% to 58% [3,8]. Pelvic fractures represent the third most common cause of death in trauma [4,6]. Delayed recognition and inappropriate management of the trauma patient with pelvic injury can lead to a poor and fatal outcome [4]. Multiple trauma associated with pelvic injury is also the leading causes of death and disability in Uzbekistan.
Fundamental objective of the emergency management of pelvic ring injury is control of hemorrhage, restoration of hemodynamic, and prompt evaluation and treatment of associated injuries. Clinical process of achieving these goals has evolved significantly. However, regardless of the consensus that displaced pelvic ring injuries are the most serious orthopedic injury requiring prompt surgical stabilization, controversy still exists regarding the recommended treatment and outcome [3,9,10]. More growing interests have been observed recently in the use of external fixation, as it involves minimally invasive, relatively easy and quick procedure to achieve pelvic stability promoting the fracture healing as well as to decrease the amount of hemorrhage and soft tissue injury [2,11]. This combined effect may decrease the mortality associated with major unstable pelvic fractures as well as decrease the incidence of associated complications, such as respiratory, renal, failure and disseminated intravascular coagulopathy.
Various methods of stabilization of unstable pelvic ring injuries have been described [1,7,12]. Many studies introduced the methods of external fixation for pelvic ring stabilization [7,12,13], which is also one of the methods of fixation of these fractures in Republican Research Center of Emergency Medicine, Uzbekistan. This research institution is the head center for the emergency medical service structure of Uzbekistan. It provides qualified multidisciplinary specialists services to the patients, intensive care and is equipped with high quality diagnostic tools such as computed tomography. One of the essential parts of the evaluation of any significant pelvic injury, including the posterior pelvic ring structure, which is usually poorly seen on standard radiographs, is the computed tomography [14].
However, it is not always available at the district level of trauma service in Uzbekistan. Hence, the patients with the unstable pelvic fracture are referred to the head center for the better evaluation and management of these patients from its regional branches. Therefore, the objective of our study is to introduce the clinical outcomes and the trend of surgical treatment methods of pelvic fractures in National Emergency Referral Center in Uzbekistan during February 2010-January 2014.
Materials and Methods
Study design and Population
This study is designed as a retrospective study, using reviews of medical records of patients admitted during February 2010 to January 2014 at Republican Research Centre of Emergency Medicine of Republic of Uzbekistan. Identification of the patients and their data’s were obtained from the hospital records section after approval from the Institutional Review Board (IRB). Total of 285 patients with pelvic ring fracture who were treated in this institution from February 2010 to January 2014 were enrolled in this study. The study population included 207 (72.6%) male patients and 78 (27.4%) females, with male to female ratio of 2.6:1. The age ranged from 25 to 55 years. Isolated acetabular fractures, pathological fractures and cases with uncontrolled extra pelvic bleeding were excluded. Clinical outcomes were analyzed in 182 patients who were followed up for at least 6 months.
Perioperative Management
Treatments of pelvic injuries are one of the parts of the management of the polytraumatized patients [11,15]. A great attention has been paid to the diagnosis and management of associated life-threatening injuries, as the majority of patients have been received with different levels of shock [16]. In the emergency department these patients were evaluated and managed according to the standard Advanced Trauma Life Support (ATLS) guidelines [16]. A patient with hemorrhagic shock was considered with systolic blood pressure less than 90mmHg after receiving two liters intravenous crystalloid [3]. Anti-shock procedure has been carried out for the hemodynamically unstable patients immediately [17,15]. Further assessment of patients included focused abdominal sonography, multispiral computer tomography (MSCT) of the chest, abdomen and pelvis, plain radiograph of the skull, throracolumbar spine were performed following the primary survey and resuscitation [14].
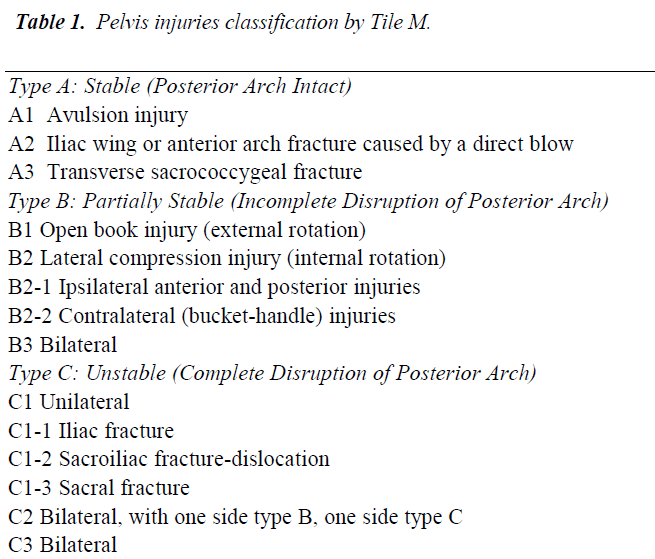
All pelvic fractures were classified by experienced orthopedic surgeons and have been divided into three types A, B and C by the Tile classification adopted by the OTA [18] (Table 1) and were enrolled in Group I, Group II and Group III, respectively (Table 2). Patients with the minimal displacements, without damage in continuity of posterior arch of the pelvic ring without anatomic-functional disorders were managed by traditional conventional ways. External fixator with the use of our backbone apparatus were applied in pelvic injuries of type B1, type B2 fractures and in type C1.1 fractures when there is a partial congruence of the sacroiliac joint. Stabilization with external fixator in combination with open reduction and internal fixation were performed in the patients with severe rotational and vertically-unstable injuries.
Clinical and Radiological Assessment
Hospital charts of the patients with pre- and postoperative anteroposterior, as well as special inlet and outlet views of pelvis radiographs and computed tomography (CT) scans were reviewed. To evaluate postoperative stability of pelvic rim, interrelations in symphysis pubis and sacroiliac joint as well as maximal residual displacement [15] was assessed by radiographs and CT scans. Clinical outcomes were evaluated by assessing Majeed score including pain, standing position, sitting position, work efficiency and sexual activity. A score greater than 85 is considered as excellent, between 70 and 85 good, between 55 and 69 satisfactory and less than 55 as poor [19]. Demographic details, mechanism and stability of fracture, surgical treatment, associated injuries, hemodynamic status of the patient on arrival, resuscitation and transfusion requirements, mode of treatment and length of hospital stay and mortality were also evaluated.
Results
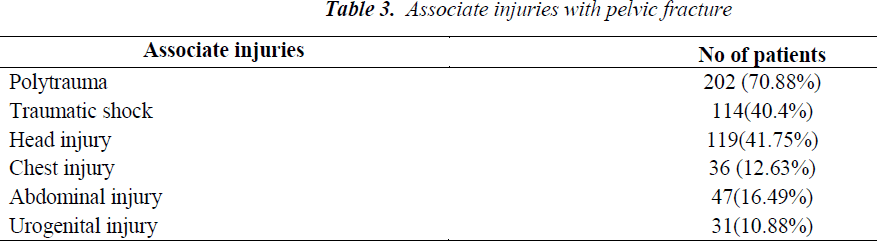
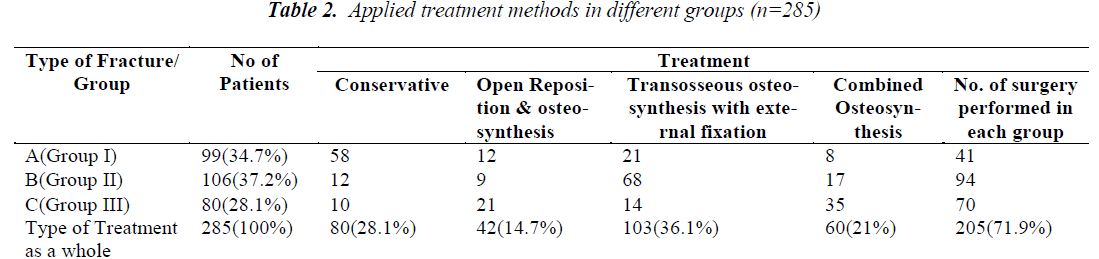
1. Data collected after treatment of 285 patients with different types of pelvis injuries was evaluated. Among 285 patients, 99 patients (34.7%) had type A injury, 106 pa tients (37.2 %) were in type B and 80 patients (28.1%) were in type C (Table 2). 202 patients (70.9%) had polytrauma injuries while 114 patients (40.4%) had traumatic shock of different levels of severity (Table 3). 205 patients (71.93%) among 285 of this study were managed by operative interventions.
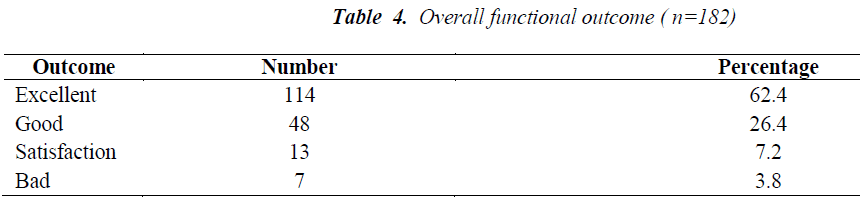
2. All the operated patients had undergone surgery in early post-traumatic period within 10 days. In all cases the stability of pelvic ring has been achieved and it has been proved by radiological finding of normal interrelations in symphysis pubis and in sacroiliac joint as well as maximal residual displacement [15]. Among 205 patients who had undergone surgical treatment, 182 (88.8%) were available for the follow up evaluation in the period from 6 months to 3 years. Amid surgically treated 182 cases, clinical outcomes were excellent in 114 (62.6%) cases, good in 48(26.4%), satisfactory in 13(7.2%) and poor in 7(3.8%) (Table 4).
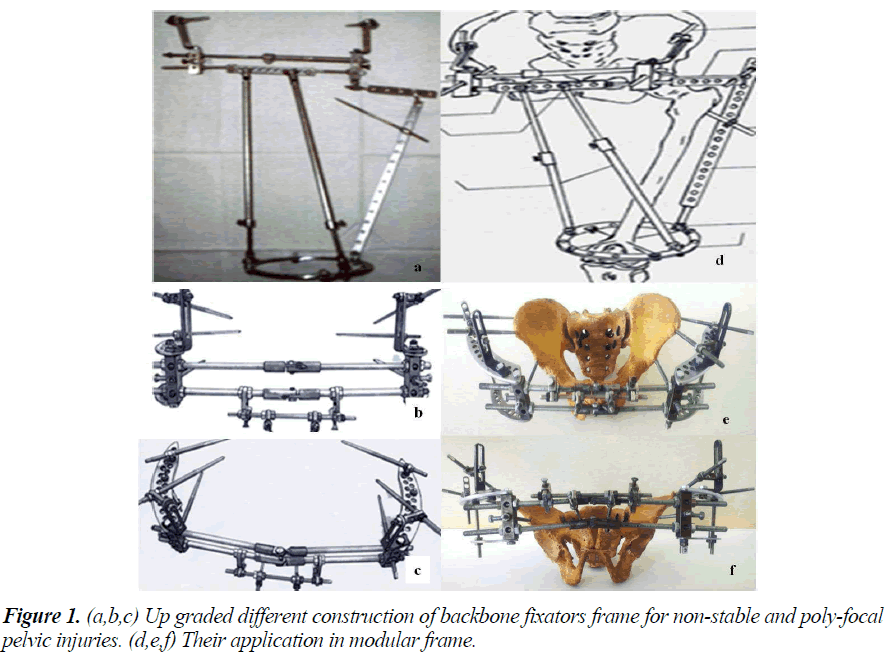
3. Amongst surgicaly treated 205 patients, 103 patients (50.4%) had undergone closed reduction and stabilization by external fixator. 68 patients (72.3%) out of group II (type B) were managed with this technique (Table 2). In this treatment group, the patients were ambulated on an average after 10 to12 days. The external fixator was removed in 56+5 days in type B and 74+4 days in type C fractures. Also, 42 patients (20.5%) and 60 patients (29.3%) had undergone osteosynthesis by internal fixation and combined osteosynthesis, respectively. All the apparatus of external fixation were worked-out in the Republican Research Centre of Emergency Medicine (Fig. 1).
4. In three cases (2.9%) among 103 patients treated with external fixator, there was development of deep inflammation around the pins site, where as 15 patients (14.6%) cases had superficial pin tract infection.
5. The average amount of blood transfused was 2L of packed red blood cell (range, 0.8L to 4.8L) and most of the transfusion were done on the first day of admission of these patients. 114 patients (40.4%) of our study population had hypovolemic shock associated with thoracic, abdominal and other organs injuries. Blood transfusions were required in 73 patients (25.6 %); 26 patients (24.5%) in group II and 47 patients (58.2%) in Group III.
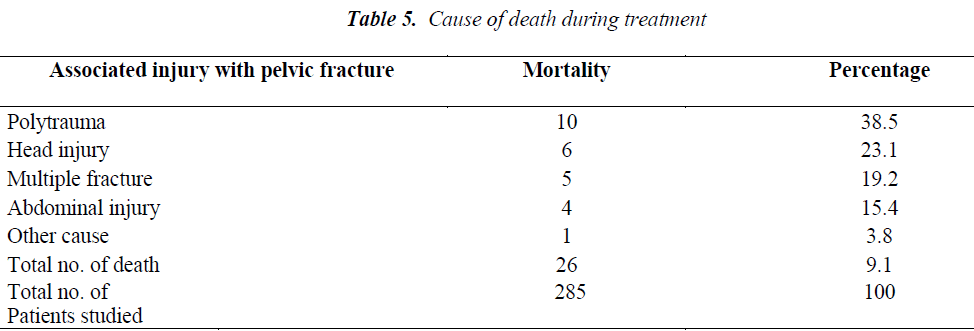
6. The mortality rate in current study was found as 9.1 % (26 patients), of which 19 patients were male and 7 of them were female. 13 patients died within 1 to 3 days of arrival, 7 patients within 4 to 10 days and 6 patients after 10 days of their arrival in the hospital. Mortality of pelvic fracture associated with the multiple injuries is shown in the Table 5.
7. Patients surgically treated have returned to their work without further significant disability and complication in an average of 8 weeks in group I, 12 to 16 weeks in group II and in group III in 30 to 32 weeks.
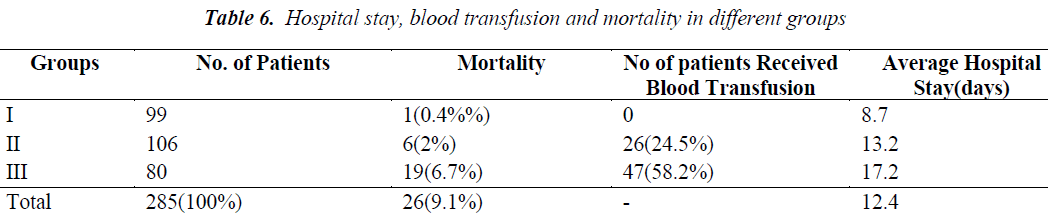
8. The average hospital stay of the patients in our study was found about 8.7 days in group I, 13.2 days in group II and 17.2 days in group III (Table 6).
Discussion
Trauma and its associated injuries are the leading causes of death and disability in Uzbekistan region. National emergency developmental model of Republic of Uzbekistan is supported by its Ministry of Health. There have been significant achievements in the field of public health care of Uzbekistan, and advancement in emergency medicine service is regarded as one of it. The emergency medical service structure of Uzbekistan consists of the head center in Tashkent at the Republican Research Center of Emergency Medicine, which is the trauma center of level I. Under its umbrella, there are 13 regional branches – trauma center of level II. And 175 sub-branches - emergency medical units – trauma center of level III at the periphery. These peripheral units coordinate and work closely with the head center, where they refer the most critical and complicated cases. This helps to improve the survival rates of patients with severe pelvic fracture by timely recognizing and referring the cases to the higher centers. It also helps to collect and analyze clinical and epidemiologic data and thereby provides a statistical base to support clinical audit and ultimately improves the development of trauma services in Uzbekistan. Injury surrounding the pelvic ring is one among them.
Pelvic fractures result from the high energy trauma and are usually associated with multiple injuries, surgical treatment of which is technically demanding and challenging [2,3,10]. The ideal treatment for unstable pelvic fractures remains a matter of debate [9,20,21]. Unstable pelvic fracture and hemodynamic instability require an urgent stabilization of the pelvis as a fundamental part of the resuscitation. In this study, these situations were mostly managed by urgent stabilization with external fixator (Fig. 2). Herein out of 285 patients, we have reported the outcome of 182 patients that were managed surgically with the follow up of 6 months to 3 years. Majority of the patients in our study were treated with minimally invasive application of external fixator, 103 patients (50.2%), or combination of external fixation and internal fixation, 60 patients (29.3%). This study has shown an overall promising result of different methods of treatment modalities, with the excellent clinical result in 114 (62.6%) cases, good in 48 (26.4%) cases, satisfactory in 13 (7.2%) cases and bad in 7 (3.8%) cases. Similar to our results, study conducted by Takashi Suzuki et al. [22] for 57 pelvic fractures has also shown their finding with excellent result in 50.8% cases, good in 22.8% cases, satisfactory in 15.7 % cases and poor in 10.5% cases, with similar modality of treatment.
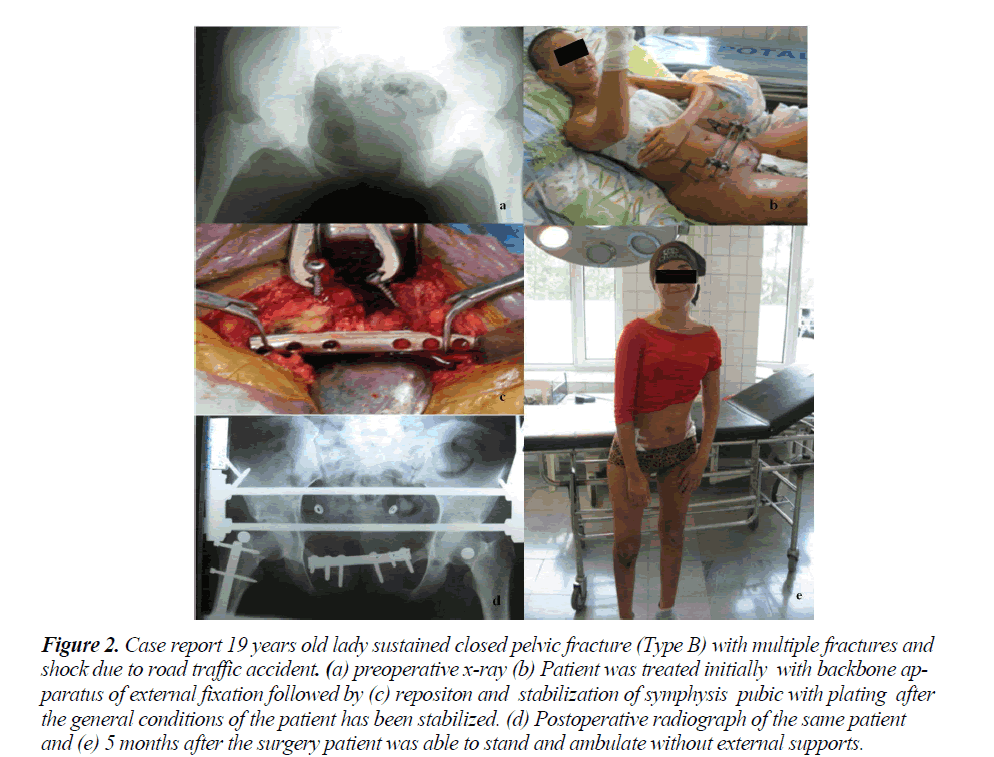
Figure 2: Case report 19 years old lady sustained closed pelvic fracture (Type B) with multiple fractures and shock due to road traffic accident. (a) preoperative x-ray (b) Patient was treated initially with backbone apparatus of external fixation followed by (c) repositon and stabilization of symphysis pubic with plating after the general conditions of the patient has been stabilized. (d) Postoperative radiograph of the same patient and (e) 5 months after the surgery patient was able to stand and ambulate without external supports.
Although there has been significant achievement in declining the mortality rate following pelvic fracture however, still 10% of these patients died despite of these achievements [23]. In our study, we have found that the mortality rate was 9.1% (26 patients). Early mortality in relation to pelvic fracture was due to uncontrolled hemorrhage and associated injuries; whereas late mortality was related with the sepsis. It has been shown that a high correlation exists between the mortality rate and initial hemodynamic status of the patients. The mean blood transfusion requirement is around 5 to 8 units in the pelvic fractures [23]. In our study, the average amount of blood transfused was 2L of packed red blood cell. The period of hospital stay in our study relied on the morphology of the fracture, mechanism of injury, severity of the trauma and the associated injury. The overall average hospital stay was about 12.4 days. There were observed superficial pin tract infections in 15 patients (14.6%), in external fixator group, which were managed with conservative treatment. Whereas in 3 cases, there were development of deep inflammation around the pins site which was treated by early removal of the fixator and course of antibiotic therapy. Pin site infection related with the external fixation in the treatment of pelvic fracture has been reported to about 2 to 40% with mean of 18% [11]. Nevertheless, none of the cases developed osteomyelitis. Similar result with us has also been reported in a study by Scagleone et al. [2]. Pin site infection was observed to depend on patient’s constitutional appearance, duration of application of the fixator and patients’ compliance with taking care of the pins sites.
In our study, we have observed that external fixation using backbone apparatus had major role during surgical treatment of pelvic bone fracture in Uzbekistan. This method of fixation of the pelvic fracture is technically easy for application in urgent situations and seems to be a promising method. However, more combination of external fixation and internal fixation was necessary in unstable pelvic fracture (groupIII) compared with stable (groupI) or partially stable (groupII) pelvic fracture.
There are some limitations in the current study which can be summarized as follows: The value of this study may be limited by its retrospective design, lack of a control group and long term outcome. The interpretation of treatment outcome of this injured patient population may be biased by neurological and other concomitant injuries.
Conclusion
Using external fixator, surgical treatment of pelvis fracture showed satisfactory clinical outcome in Uzbekistan region. However, more combination of external fixator and internal fixation was necessary in unstable pelvic fracture compared with stable or partially stable pelvic fracture.
Acknowledgements
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (NRF- 2014R1A1A4A03009388) and by Hallym University Research Fund.
Compliance with ethical requirements
This retrospective study was carried out following the acquisition of institutional ethical approval.
References
- Tosounidis TI, Giannoudis PV. Pelvic fractures presenting with haemodynamic instability: treatment options and outcomes. The surgeon : journal of the Royal Colleges of Surgeons of Edinburgh and Ireland. 2013;11(6): 344-351.
- Scaglione M, Parchi P, Digrandi G, Latessa M, Guido G. External fixation in pelvic fractures. Musculoskele- tal surgery. 2010; 94 (2): 63-70.
- Ertel W, Keel M, Eid K, Platz A, Trentz O. Control of severe hemorrhage using C-clamp and pelvic packing in multiply injured patients with pelvic ring disruption. Journal of orthopaedic trauma. 2001; 15(7): 468-474.
- Katsoulis E, Giannoudis PV. Impact of timing of pelvic fixation on functional outcome. Injury. 2006; 37 (12): 1133-1142.
- Hasankhani EG, Omidi-Kashani F. Treatment outcomes of open pelvic fractures associated with extensive perineal injuries. Clinics in orthopedic surgery. 2013; 5(4): 263-268.
- Giannoudis PV, Grotz MR, Tzioupis C, Dinopoulos H, Wells GE, Bouamra O, et al. Prevalence of pelvic fractures, associated injuries, and mortality: the United Kingdom perspective. The Journal of trauma. 2007; 63(4): 875-883.
- Slater SJ, Barron DA. Pelvic fractures-A guide to classification and management. European journal of radiology. 2010; 74(1): 16-23.
- Pizanis A, Pohlemann T, Burkhardt M, Aghayev E, Holstein JH. Emergency stabilization of the pelvic ring: Clinical comparison between three different techniques. Injury. 2013; 44(12): 1760-1764.
- Sathy AK, Starr AJ, Smith WR, Elliott A, Agudelo J, Reinert CM, et al. The effect of pelvic fracture on mortality after trauma: an analysis of 63,000 trauma patients. The Journal of bone and joint surgery American volume. 2009; 91(12): 2803-2810.
- Abrassart S, Stern R, Peter R. Unstable pelvic ring injury with hemodynamic instability: what seems the best procedure choice and sequence in the initial management? Orthopaedics & traumatology, surgery & research : OTSR. 2013; 99(2): 175-182.
- Mason WT, Khan SN, James CL, Chesser TJ, Ward AJ. Complications of temporary and definitive external fixation of pelvic ring injuries. Injury. 2005; 36(5): 599-604.
- Trokhova VG. Transosseous osteosynthesis in the treatment of traumatic pelvic ring disruptions. Orthopedics. 1994; 17(12): 1125-1128.
- Keshishyan RA, Rozinov VM, Malakhov OA, Kuznetsov LE, Strunin EG, Chogovadze GA, et al. Pelvic polyfractures in children. Radiographic diagnosis and treatment. Clinical orthopaedics and related research. 1995; 320: 28-33.
- Gill K, Bucholz RW. The role of computerized tomographic scanning in the evaluation of major pelvic fractures. The Journal of bone and joint surgery American volume. 1984;66(1): 34-39.
- Mardanpour K, Rahbar M. The outcome of surgically treated traumatic unstable pelvic fractures by open reduction and internal fixation. Journal of injury & violence research. 2013; 5(2): 77-83.
- Kortbeek JB, Al Turki SA, Ali J, Antoine JA, Bouillon B, Brasel K, et al. Advanced trauma life support, 8th edition, the evidence for change. The Journal of trauma. 2008;64(6): 1638-1650.
- Asadollahi S, de Steiger R, Gruen R, Richardson M. Management guideline in haemodynamically unstable patients with pelvic fractures: Outcomes and challenges. Emergency medicine Australasia: EMA. 2010; 22(6): 556-564.
- Tile M. Pelvic ring fractures: should they be fixed? The Journal of bone and joint surgery British volume. 1988; 70(1): 1-12.
- Majeed SA. Grading the outcome of pelvic fractures.The Journal of bone and joint surgery British volume. 1989; 71(2): 304-306.
- Schweitzer D, Zylberberg A, Cordova M, Gonzalez J. Closed reduction and iliosacral percutaneous fixation of unstable pelvic ring fractures. Injury. 2008; 39(8): 869-874.
- Noordeen MH, Taylor BA, Briggs TW, Lavy CB. Pin placement in pelvic external fixation. Injury. 1993; 24(9): 581-584.
- Suzuki T, Shindo M, Soma K, Minehara H, Nakamura K, Uchino M, et al. Long-term functional outcome after unstable pelvic ring fracture. The Journal of trauma. 2007; 63(4): 884-888.
- Dyer GS, Vrahas MS. Review of the pathophysiology and acute management of haemorrhage in pelvic fracture. Injury. 2006;37(7): 602-613.