Research Article - Biomedical Research (2017) Volume 28, Issue 18
Clinical effect of two-ports thoracoscopic pulmonary lobectomy and systemic lymphadenectomy for bronchogenic carcinoma
Shimeng Wang1, Lin Li1, Qi Liu2 and Guo-Dong Gao3*
1Department of Thoracic Surgery, Heze Municipal Hospital, Shandong Province, PR China
2Qingdao City Center Medical Group, Customer Service Center, PR China
3Jining No.1 People’s Hospital, Shandong Province, PR China
Accepted on August 28, 2017
Abstract
Objective: To investigate clinical effect of two-ports thoracoscopic pulmonary lobectomy and systemic lymphadenectomy in curing bronchogenic carcinoma well.
Background: Single-port and multiple-ports thoracoscopic surgery treating lung cancer were reported more. Each of them has their own advantages and disadvantages, and now two-ports thoracoscopic surgery treating lung cancer is more widely used.
Methods: A quantity of 124 patients with bronchogenic carcinoma involved in our hospital from August 2014 to June 2016 were randomly divided into two groups, two-ports VATS group and thoracotomy group (respectively 62 cases) on the basis of the method of random number table. The operative time, blood loss in operation, thoracic drainage, postoperative hospital stay and intraoperative lymph nodes dissection and operation complications were contrasted between both of two-ports VATS group and thoracotomy group.
Results: The operation time of two-ports VATS group was significantly higher than that of thoracotomy group (P<0.05). The intraoperative blood loss, thoracic drainage and hospital stay of two-ports VATS group were distinctly lower than those of thoracotomy group<0.05). There was no obvious difference in the number of intraoperative lymphadenectomy between the two groups (P>0.05). The complication rate of two-ports VATS group was significantly lower than that of thoracotomy group (P<0.05).
Conclusion: Two-ports thoracoscopic pulmonary lobectomy and systemic lymphadenectomy are a secure and effective method for the treatment of lung cancer. It is worthy of popularization and application.
Keywords
Two-ports Video-assisted thoracoscopic surgery (VATS), Thoracoscopic pulmonary lobectomy, Systemic lymphadenectomy, Bronchogenic carcinoma, Lung cancer
Introduction
Bronchogenic carcinoma is a common clinical disease, which is also called for lung cancer, and is often occurring on the elderly patients. Cough, chest pain, and fever are its main clinical symptoms, which is a serious threat to patient’s life. Surgical treatment is the preferred treatment for lung cancer and commonly used surgery is pulmonary lobectomy and systemic lymph node dissection [1]. But thoracic surgery is companied with severe trauma, more bleeding and serious postoperative pain. In recent years, there has been a Video- Assisted Thoracoscopic Surgery (VATS) as the representative of the minimally invasive thoracic surgery [2,3]. It is to remove tumor itself and its transfer site, keeping functional lung tissue, to the most extent. At present, three-ports thoracoscopic surgery is more commonly used, which is used to be a gold standard test for curing lung cancer. However, the number of incision and surgical trauma is still large, likely to cause back muscle bleeding. Although some people have used a single-port VATS for lung cancer at abroad, and achieved good results, it is advantageous of a small trauma, less bleeding, and rapid recovery after surgery [4]. But this method is required for surgeons to be with the relatively high operative technique, and it is easy to ignore the dissection of hidden parts of lymph nodes, easily leading to postoperative recurrence of lung cancer. At home and abroad, reports on the single-port thoracoscopic treatment of lung cancer are relatively small, and its clinical treatment is not accurate.
Combined with the advantages and disadvantages of three-ports and single-port thoracoscopic surgery, two-ports thoracoscopic surgery, not only surgical trauma, intraoperative bleeding control, cleaning lymph nodes thoroughly, but also in the ease of operative technique, has unparalleled advantages compared with three-ports and single-port thoracoscopic surgery. At present, the clinical application of two-ports thoracoscopic surgery is more extensive. This study has selected lung cancer patients in our hospital from August 2014 to June 2016.A total of 124 cases were carried out, respectively by thoracotomy and two-ports thoracoscopic surgery, pulmonary lobectomy and systemic lymph nodes cleaning, to explore its clinical efficacy and complications after surgery.
Materials and Methods
Patient selection
A quantity of 124 patients with bronchogenic carcinoma involved in our hospital, from August 2014 to June 2016, were randomly and averagely divided into two groups, two-ports VATS group and thoracotomy group (respectively 62 cases) on the basis of random number table.
Inclusive criteria: (1) All patients are in accordance with the diagnostic criteria for lung cancer in “The common malignancy diagnosis and treatment norms”; (2) All have signed out informed consent and approved by the Medical Ethics Committee; (3) Selected patients are probably diagnosed by chest CT, bronchoscopic biopsy and aspiration biopsy; (4) The surgical method is pulmonary lobe dissection and systemic lymphadenectomy; (5) There is also no far metastasis.
Exclusive criteria: (1) Patients who are complicated with cardiovascular and cerebrovascular diseases and respiratory system infection; (2) Patients with ediastinal and pleural thickening, involving the surrounding blood vessels, tissues and organs; (3) Patients who cannot cooperate with us; (4) Patients who once underwent lung surgery and chemotherapy; (5) Patients who were treated with immunosuppressive agents and hormones; (6) Patients with severe liver and kidney thrombosis diabetes or coagulopathy; (7) Patients who were not able to accept follow-up after surgery . Two group patients were carried out surgery by the same surgeon.
Surgical methods
Two-ports thoracoscopic surgery group: patients were implemented of intravenous anesthesia and tracheal intubation. Using two-ports thoracoscopic lobe dissection and systemic lymphadenectomy surgery, the patients were to keep the lateral position, put pillow under shoulder, put soft pad under waist, increase the intercostal space. In the middle of the axillary line 7 to 8 ribs, 1 cm incision is ready for the observation port. The thoracoscopy was put into it to check the tumor location, size and whether has happened far transfer. After determining the location, 4~5 cm outside the tumor or chest, skin incision was regarded as based operative port. The length of the incision is longer, easy to operate and remove the lobes. In the scapular 1.5 cm, operative incision was ready for a secondary operative port, into which was implanted the scatheless oval clamp and separation clamp, without stretching the ribs, respectively. Fully separate from lung lobes, free lesions of the lung lobe, deal leaf lobes with the electrocautery method, and remove the lobes. Cut the medial diaphragm of superior vena cava, separate the lymph nodes and lift it. Coagulate the lymph nodes in basal part of small blood vessels and lymphatic vessels, and wholly resect lymph nodes together with the surrounding adipose tissue. After cleaning the lymph nodes, repeatedly rinse the thoracic cavity with saline, until no fresh blood spilled. Then, close the chest and suture incision.
Thoracotomy group: According to the lesion location, choose the 5th or 6th intercostal space into the chest. Carry out a 20 cm posterolateral incision, retain the front saw muscle, and broke the 6th rib. Distractor was used to support the ribs in order to implement pulmonary lobectomy and systemic lymphadenectomy. The routine method is to remove the lobes and clean the lymph nodes. Then, rinse the thoracic cavity with saline.
Observed indicators
The operative time, blood loss in operation, thoracic drainage, hospital stay, intraoperative lymphadenectomy and operation complications were compared between both of thoracoscopic group and thoracotomy group.
Statistical analysis
SPSS17.0 was used for statistical analysis. The data of operation time, intraoperative blood loss, thoracic drainage, postoperative hospitalization time and lymph node dissection were measured by mean ± SD. Two independent samples t-test was applied for comparing between two groups. The complications of count data, expressed as a percentage, used the chi-square test on group’s comparison. P<0.05 is suggesting the disparity was statistically distinct existed.
Results
There were no significant difference in the age, sex, type, tumors size, tumors position and tumors staging of all lung cancer patients in both two-ports thoracoscopic surgery group and thoracotomy group (P>0.05), as Table 1.
| Index | Two-ports VATS group (n=62) | Thoracotomy group (n=62) | P |
|---|---|---|---|
| Age (y) | 54.3 ± 12.1 | 53.8 ± 10.4 | 0.785 |
| Male | 43 (69.4) | 39 (62.9) | 0.448 |
| Squamous cell carcinoma | 53 (85.5) | 48 (77.4) | 0.248 |
| Tumor size (cm) | 2.2 ± 1.3 | 2.5 ± 1.2 | 0.236 |
| Tumor location* | |||
| LUL | 12 (19.4) | 13 (21.0) | 0.886 |
| LLL | 16 (25.8) | 15 (24.2) | |
| RUL | 11 (17.7) | 14 (22.6) | |
| RML | 14 (22.6) | 10 (16.1) | |
| RLL | 9 (14.5) | 10 (16.1) | |
| TNM stage | |||
| I | 34 (54.8) | 32 (51.6) | 0.927 |
| II | 21 (33.9) | 22 (35.5) | |
| III | 7 (11.3) | 8 (12.9) | |
| *LUL: Left Upper Lobe; LLL: Left Lower Lobe; RUL: Right Upper Lobe; RML: Right Middle Lobe; RLL: Right Lower Lobe. | |||
Table 1. Clinical data features of all the patients involved (Mean ± SD).
Two-ports thoracoscopic surgery group: The operation time was 146.5 ± 38.2 min, the intraoperative blood loss was 210.1 ± 56.4 ml, the thoracic drainage was 827.6 ± 103.9 ml, the hospital stay was 10.3 ± 2.4 d and the quantity of dissecting lymph nodes was 14.6 ± 5.2.
Thoracotomy group: The operation time was 121.4 ± 35.3 min, the blood loss was 387.8 ± 67.2 ml, the thoracic drainage was 1310.7 ± 234.1 ml, the hospital stay was 16.5 ± 4.2 d and the quantity of dissecting lymph nodes was 15.7 ± 2.9. (P<0.05).
The operation time of two-ports thoracoscopic surgery group was obviously higher than that of the thoracotomy surgery group (P<0.05). But about the intraoperative blood loss, thoracic drainage and hospital stay, the two-ports thoracoscopic surgery group was distinctly lower than those of the thoracotomy group (P<0.05).
There was no obviously disparity in the number of intraoperative lymph node dissection between both of two groups (P>0.05), as the Table 2.
| Cases | Operation time (min) | Intraoperative blood loss (ml) | Thoracic drainage (ml) | Hospital stay (d) | The number of cleaning lymph nodes (n) | |
|---|---|---|---|---|---|---|
| Two-ports VATS group | 62 | 146.5 ± 38.2 | 210.1 ± 56.4 | 827.6 ± 103.9 | 10.3 ± 2.4 | 14.6 ± 5.2 |
| Thoracotomy group | 62 | 121.4 ± 35.3 | 387.8 ± 67.2 | 1310.7 ± 234.1 | 16.5 ± 4.2 | 15.7 ± 2.9 |
| P | 0.048 | 0.013 | 0.006 | 0.015 | 0.178 |
Table 2. Operation index of patients with two-ports VATS group and thoracotomy group (Mean ± SD).
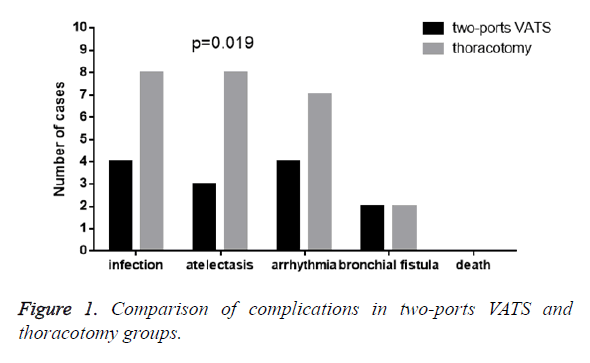
Two-ports thoracoscopic surgery group was discovered 13 patients with complications, with the 21% incidence rate. Of them, it included 4 cases with infection, 3 cases with atelectasis, 4 cases with arrhythmia, 2 cases with bronchial fistula, and no deaths. Thoracotomy group was founded out 25 cases with complications, the 40% incidence rate. Of them, there are 8 cases with infection, 8 cases with atelectasis, 7 cases with arrhythmia, in 2 cases with bronchial fistula, and no deaths. On the incident rate of complication, two-ports thoracoscopic surgery group was distinctly lower than that in thoracotomy group (P<0.05), shown as Figure 1.
Discussion
Lung cancer, known as bronchial lung cancer, is a commonly primary malignant tumor. According to statistics, nearly 18% of cancer patients throughout the world are bronchogenic carcinoma patients [1]. However, the cause of bronchogenic carcinoma has not been widely recognized by the medical profession and some studies have a voice that its occurrence is closely related to long-term much smoking. Clinical manifestations of lung cancer are more complex, for example, the pathological type of the tumor, the occurrence of parts, metastasis, and whether the complications will have a certain impact on patient’s symptoms and signs. Therapies mainly include chemotherapy, radiotherapy and surgical treatment [5,6]. Preoperative chemotherapy effective rate is approximately 60% to 70%, resection rate 56% to 90%, complete resection rate 46% to 76%, almost 10% completely pathological remission, the average 3 y survival rate of complete resection 40%. The role of some new chemotherapeutic agents in preoperative treatment is currently being studied. Preoperative radiotherapy alone is currently considered as little effect and the effect of postoperative radiotherapy is currently considered: (1) All randomized trials have shown that bronchogenic carcinoma patients on stage I and II have implemented, after complete resection, postoperative radiotherapy not to prolong survival period. So it is no necessity to do postoperative routine radiotherapy; (2) For N2 stage lung cancer patients, postoperative radiotherapy can reduce local recurrence, but it failed to extend the survival period [7,8]; (3) Currently, postoperative radiotherapy is mainly used for surgical residue, postoperative pathological examination for mediastinal lymph nodes metastasis and some prospective clinical trials.
Owing to an amazing morbidity and mortality of lung cancer, therefore, in order to improve clinical effects of curing bronchogenic carcinoma, it is the key to early diagnose and to timely and effective treat. The correct preoperative stage, strict control of lung cancer surgery indications, standardized lung cancer radical surgery is a key guarantee of improving the surgical effect of bronchogenic carcinoma. Surgical treatment is the first choice and the main curing method of bronchogenic carcinoma, methods and treatment purposes of that include the following three points: (1) Resection surgery, is to throughout clean the primary carcinoma lesions and metastatic lymph nodes, in order to achieve the purpose of cure; (2) Reducing tumor surgery, is to resect the vast majority of the tumor, to create favourable conditions for other treatment; (3) Alleviating symptoms surgery, that is, to engaged in surgery on refractory pleural cavity and pericardial effusion to slow the development of its symptoms. The common method is pulmonary lobectomy and systemic lymph node dissection. Traditional thoracic surgery is leading to large trauma, necessary to cut off the patients more chest wall muscles, while surgery also need to open the chest to pull the ribs, making patients prolong postoperative recovery time, companied with more complications. With rapidly developing progress of new thoracoscopic technology, in 2015 National Comprehensive Cancer Network (NCCN) published lung cancer clinical guidelines, which already has regarded thoracoscopic pulmonary lobectomy and systemic lymphadenectomy as one of the guiding surgery treating early lung carcinoma [9]. This established the status of thoracoscopic surgery (VATS) in curing bronchogenic carcinoma. VATS is a minimally invasive treatment technique that eliminates the need for greater incision, avoids major trauma to the patients, reduces intraoperative blood loss, alleviates postoperative pain and inflammatory response, lightens lung injury, and allows patients to recover as soon as possible [10]. The thoracoscopic surgery has a good clinical effect, with the short treatment time, less bleeding, faster postoperative recover, the significant effect, worthy of clinical promotion.
In different medical centers, operative technique of thoracoscopic pulmonary lobectomy is definitely distinct. Currently, at home and abroad, the most commonly used method in medical institutions is three-ports method, consist of a cavity port, a main operation port and a deputy operation port. But the three-ports thoracoscopy technique is existed as the following defects: (1) If the patient’s chest is small and then, when the device into the small activity space, short route will result in more difficult operation; (2) After operation, nerve and muscle next to axillary line incision will be susceptible to damage. Patients will be poor tolerance, even a small number of whom is happening mild movement disorders, sensory abnormalities and other adverse reactions; (3) Back muscles are rich blood supplied, with more levels, which are inclined to bleeding and difficult to prevent bleeding. At abroad, there were some experts who have used single-port VATS for curing bronchogenic carcinoma, which has made good effects [4]. Migliore reported in single-port VATS technology for the first time, in 2003, but it was only used for the diagnosis and treatment of relatively simple pleural related diseases, such as pleural, malignant nodules, pleural effusions and empyema [11]. In 2011, Spanish Gonzalez, for the first time, applied a single-hole VATS for pulmonary lobectomy [12]. There are also some researches on hospitals in our country to carry out a single hole thoracoscopic treatment of lung cancer. In 2015 China, Wang et al. contrasted single-port with traditional multiple-ports thoracoscopic lobectomy and systemic lymph node dissection. The results showed that single-port thoracoscopic surgery processed a lot of advantages, such as, short operation time, less bleeding, placement of drainage tube for a short time, less postoperative thoracic drainage, postoperative recovery and others. Compared with multiple-ports VATS operation, the single-port thoracoscopic surgery can effectively reduce the damage to chest wall, to the maximum extent. But due to the single-port thoracoscopic pulmonary lobectomy saved the other two deputies operation ports; all operations are limited to a port. The surgeon is demanded to high operative technique, difficult to operate. The hole diameter is smaller, it will be inclined to result in equipment Inter-cross, narrow field of view and other issues.
Compared with single-port and multiple-port thoracoscopic technique, two-ports thoracoscopic pulmonary lobectomy and systemic lymph nodes dissection has the following advantages: (1) The surgery cleaning lymph node is not affected by the adjoin location of lymph nodes with blood vessels, and the indications are more widely; (2) Because the relationship between lymph nodes and blood vessels is relatively close, two-ports thoracoscopic surgery can separate them under direct vision, with high safety; (3) The procedure can achieve the effect of traditional thoracotomy treatment. In this study, the number of lymph nodes dissection between two groups patients is no distinct statistics disparity (P>0.05), which indicates that thoracoscopic pulmonary lobectomy combined with systemic lymphadenectomy can completely clean the lymph nodes and achieve the effect of systemic cleaning; (4) The approach can result in tiny damage and small incision. It cuts off muscle less, does not destroy the integrity of the chest wall, does not affect the ribs, operate meticulously, reduces the amount of intraoperative blood loss, and less affects respiratory muscle function; (5) Two-ports thoracoscopic surgery can fully clean mediastinal lymph nodes metastasis, effectively control the patient’s residual cancer cells, and reduce tumor growth and recurrence rate, which is conducive to patients postoperative rehabilitation. In this study, the operation time of the two-ports thoracoscopic surgery group was distinguishly higher than that of another group. The blood loss in operation, thoracic drainage and hospital stay were distinctly lower than that of another group (P<0.05). It has suggested two-ports thoracoscopic lobectomy and systemic lymph nodes dissection is supporting the above analysis, which has a certain advantage, worthy of clinical application. The study also has found out that the occurrence of infection, atelectasis, bronchial fistula, arrhythmia, death and other complications on patients who underwent two-ports thoracoscopic surgery were significantly lower than the incidence of patients from thoracotomy group, indicating that clinical effect of patients who undergoing two-ports thoracoscopic pulmonary lobec dissection and systemic lymph nodes dissection surgery is superior to traditional thoracotomy. The thoracoscopic magnification imaging system and precision endoscopic surgical instruments is to expand the surgical field of vision, to reduce the body damage on normal tissues and organs, while it thoroughly cleans lymph nodes and prevents tumor recurrence, protecting lung function. However, due to two-ports thoracoscopic pulmonary lobectomy only keeping one main operation port, almost 1-3cm large, all operations have gotten to be carried on by this operation port. Therefore, intraoperative operation is required to be careful to avoid the equipment interference, causing damage to the organizations. Although the treatment of lung cancer has made an important progress, still the treatment effect is not satisfying. Most of reports have indicated that the average 5 y survival rate is still around 35%. It is estimated that almost 20% to 40% of lung carcinoma patients will appear to be brain metastases. The mainly treating methods are glucocorticoids, radiotherapy and surgery, and radiology surgery (radiotherapy) is also more and more used for curing brain metastases of those. Its local effect is similar to surgical resection, so it cannot temporarily replace of the whole brain irradiation, currently used for less than 3cm metastases treatment. For the treatment of multiple brain metastases, we generally apply the whole brain irradiation or three-dimensional radiotherapy supplemented with whole brain irradiation. Kotlvarov summed up 852 surgical failure model cases of lung cancer, distant metastasis accounted for 55.2%, local recurrence accounted for 33.8%, both distant metastasis and local recurrence accounted for 11%. Therefore, to reduce local recurrence and distant metastasis is urgently need to solve the problem in a lung cancer surgery as soon as possible.
Conclusion
Two-ports thoracoscopic pulmonary lobe dissection and systemic lymphadenectomy, for the treatment of lung cancer, has significant clinical efficacy, high safety, lymph nodes cleaning thoroughly, the small trauma for patients. Also, it can reduce postoperative pain, alleviate recurrence, and lighten the incidence of complications, worthy of clinical application.
References
- Baltayiannis N, Chandrinos M, Anagnostopoulos D, Zarogoulidis P, Tsakiridis K, Mpakas A, Machairiotis N, Katsikogiannis N, Kougioumtzi I, Courcoutsakis N, Zarogoulidis K. Lung cancer surgery: an up to date. J Thorac Dis 2013; 5: 425-439.
- Inada K, Shirakusa T, Yoshinaga Y. The role of video-assisted thoracic surgery for the treatment of lung cancer: lung lobectomy by thoracoscopy versus the standard thoracotomy approach. Int Surg 2000; 85: 6-12.
- Vaporciyan AA. 50th anniversary landmark commentary on mountain CF. Assessment of the role of surgery for control of lung cancer. Ann Thorac Surg 1977; 24: 365-373.
- Hou YB, Wang GX, Tan S. 146 cases experience report of lobectomy with single utility port complete video-assisted thoracoscopic surgery on lung cancer. J Clin Med Literature 2016.
- Tanimoto M, Kiura K, Fujiwara Y. Method for determining a lung cancer treatment and method for determining the effectiveness of an agent for treatment of lung cancer. United States Patent Application 20090263838, 2009.
- Alasti H, Cho YB, Vandermeer AD. A novel four-dimensional radiotherapy method for lung cancer: Imaging, treatment planning and delivery. Phys Med Biol 2006; 51: 3251-3267.
- Elias AD, Kumar P, Skarin AT. Radiotherapy versus chemotherapy plus radiotherapy in surgically treated IIIA N2 non-small-cell lung cancer. Clin Lung Cancer 2002; 4: 95-103.
- Le PC, Dunant A, Faivre-Finn C. Postoperative radiotherapy for pathologic N2 non-small-cell lung cancer treated with adjuvant chemotherapy: Need for randomized evidence. J Clin Oncol 2015; 33: 2930-2931.
- Wood DE. National Comprehensive Cancer Network (NCCN) Clinical Practice Guidelines for Lung Cancer Screening. Thorac Surg Clin 2015; 25: 185.
- Meng QS, Tang DF, Chang-Sheng LI. Effect of video-assisted thoracoscopic surgery on lung cancer. J Chin Pract Diagnosis Ther 2014.
- Migliore M. Efficacy and safety of single-trocar technique for minimally invasive surgery of the chest in the treatment of noncomplex pleural disease. J Thorac Cardiovas Surg 2003; 126: 1618-1623.
- Gonzalez D, Garcia J, Fieira E. Video-assisted thoracoscopic lobectomy in the treatment of intralobar pulmonary sequestration. Interact Cardiovasc Thorac Surg 2011; 12: 77-79.