- Biomedical Research (2012) Volume 23, Issue 3
Bifurcation Of brachial artery at it?s commencement-A case report
Shewale SN, Sukre SB, Diwan CVDepartment of Anatomy, Government Medical College, Aurangabad, Maharashtra, India
Accepted date: September 03 2011
Abstract
Normally brachial artery divides into it’s terminal branches namely radial and ulnar arteries at the neck of the radius in the cubital fossa. In the present study ,a case of termination of brachial artery at it’s commencement below the lower border of teres major is being reported. Both the terminal branches, ulnar and radial had superficial course along the medial aspect of biceps brachii. In cubital fossa, biceps tendon was flanked by ulnar and radial arteries on medial and lateral sides respectively. In the forearm, radial artery had more superficial course than ulnar artery. The study is done on the termination of the brachial artery and reported.
Keywords
Brachial artery, radial artery, ulnar artery, bifurcation, trifurcation, variation.
Introduction
Brachial artery is the main artery of the arm. It is the direct continuation of axillary artery at the lower border of teres major muscle and.ends about a centimeter distal to elbow joint (at the level of neck of the radius) by dividing into radial and ulnar arteries [1].Text books of anatomy make a reference to ‘vas aberrans’ in the main brachio antebrachial pattern [2]. Treves and Rogers[3] 1947, Williams et al [1] that these connect the brachial or axillary artery with one or the other artery of forearm usually joining the radial. Treves and Rogers [3] called superficial brachial artery, a common anomaly as a vas aberrans. High origin of radial and ulnar artery forms the highest percentage of variations of brachial artery. Karlsson and Niechajev [4] and Compta [5] found that high origin of radial artery is the commonest vascular pattern variation of the upper extremity.
Material and Methods
Out of 30 human upper limbs dissected by 1st year M.B.B.S. students in department of anatomy of Government Medical College, Aurangabad, only one left upper limb of a male cadaver showed variation in termination of brachial artery.
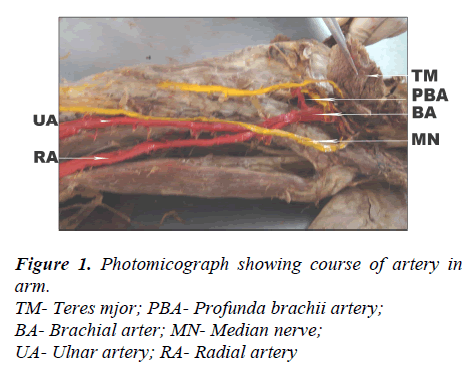
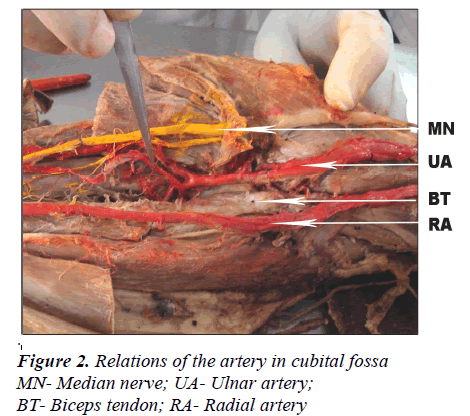
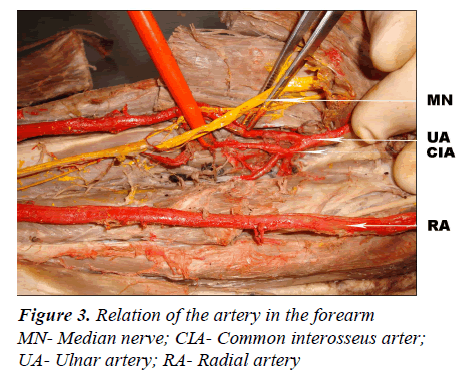
Observation [Figures 1,2 and 3]
In left upper limb of a male cadaver, bifurcation of brachial artery into radial and ulnar arteries at the lower border of teres major was found. Both the arteries had superficial course in the arm along the medial aspect of biceps brachii and radial artery crossed biceps tendon superficially while passing through cubital fossa.
1) Course of ulnar artery
-In the middle of the arm, ulnar artery was crossed by median nerve from lateral to medial side. In the lower part of the arm, it was accompanied by median nerve on its medial side .
-It entered into the cubital fossa deep to the deep head of pronator teres.
-In forearm, it passed between superficial and deep group of flexor muscles with accompanying ulnar nerve on its medial side, and in upper part it gave common interosseus artery, which again divided into anterior and posterior interosseus arteries.
-It finally entered the hand by passing superficial to the flexor retinaculum lateral to pisiform bone and continued in palm as superficial palmar branch.
2) Course of radial artery
-In the middle of the arm, radial artery was crossed by median nerve from lateral to medial side. It entered into the cubital fossa by crossing the tendon of biceps brachii superficially and lateral to it’s tendon.
-In the forearm, it had more superficial course accompanied by tendon of flexor carpi radialis on its medial side and tendon of brachioradialis on its lateral side in distal part.
It finally entered into the palm and continued as deep palmar arch.
In cubital fossa, biceps tendon was flanked by ulnar and radial arteries on medial and lateral sides respectively.
3) Course of profunda brachii artery
The profunda brachii artery arose from the 3rd part of axillary artery. It passed in the posterior compartment of the arm with the radial nerve supplying adjacent muscles.
Embryogenesis
The axis artery of upper limb-bud is derived from the lateral branch of seventh intersegmental artery( subclavian). Proximal part of main trunk forms an axillary continuing as brachial artery and its distal part persists as the anterior interosseus artery.
The radial and ulnar arteries are last arteries to appear in the forearm; at first, the radial artery arises more proximally than the ulnar artery from the main trunk and crosses in front of the median nerve. Later, the radial artery establishes a new connection with the main trunk at or near the level of origin of the ulnar artery. The upper portion of its original stem usually disappears to a large extent. Thus radial and ulnar arteries arise at same level. In this case, the proximal origin of radial artery fails to disappear, and the radial artery does not establish new connection with main trunk near the origin of ulnar artery. Thus the radial artery originates at a higher level and main artery of the limb continues as ulnar artery.
Discussion
In present study, the brachial artery bifurcated into its terminal branches at the lower border of teres major and both the arteries had superficial course in the arm. The laterally placed artery was named as radial artery and medially placed as ulnar artery. In the lower part, the ulnar artery had similar course to that of the brachial artery i.e. it runs along the medial side of the arm on the coracobrachialis and then brachialis muscle. It gave the superior and inferior ulnar collateral arteries as given by brachial artery normally.
Due to this bifurcation the profunda brachii artery which is the first branch given by brachial artery in the arm is given by third part of axillary artery. The origin of profunda brachii artery is quite variable. Charles et al [6] classified the origin of profunda brachii artery into seven types. It is a type IV in which it is a branch of 3rd part of axillary artery in 8.7% cases and 16 % by Anson [7].
According to Adachi [8] this superficial brachial artery is called so because it runs superficial to median nerve whereas usually the brachial artery runs deep to the median nerve.
Keen [9] subdivides superficial brachial artery into 3 types
a) Superficial brachial artery which continue in cubital fossa and bifurcate as usual into radial and ulnar arteries (3.6%).
b) Superficial brachial artery continues as radial artery and known as ‘high origin of radial artery’ (5.9%).
Rosse and Rosse [10] stated that in approximately 30% of individuals there are two brachial arteries in an arm. The two arteries usually unite in cubital fossa and again divide into ulnar, radial arteries. If they don’t unite, the identity of the vessels is determined by their relation to the median nerve and their fate in the forearm.The normal artery, representing the axial artery of the limb, takes the usual course of the normal brachial artery and is crossed superficially by the median nerve. The anomalous artery is more superficial position and named as superficial brachial, ulnar or radial depending on branching pattern.
In present study, both the arteries were crossed by the median nerve superficially from lateral to medial side. So the term superficial brachial artery couldnot be used for any artery.
Earlier investigators have also studied the termination pattern of brachial artery [1,2,11,1,12,13]. Huber [2] in 1930 found additional accessory branches of brachial arteries. He observed trifurcation of brachial artery in to ulnar, radial, common interosseus artery or median arteries. However, Patnaik et al 11] reported trifurcation of brachial artery into ulnar, radial and radial recurrent arteries in right superior extremity of 50 yr old male cadaver.
Bilodi [14].has found that brachial artery trifurcated into ulnar, radial, common interosseus arteries at the neck of radius in the left upper limb. In right upper limb, brachial artery had terminated into ulnar and radial arteries whereas common interosseus artery was given off from radial artery and not from ulnar artery.
High division of brachial artery is the most common variation of brachial artery. Karlsson and Niechajev [4] mentioned that high origin of radial artery is commonest vascular pattern variation in upper extremity observed in 10% patients by angiographic studies. Similar results were reported in 14.27% by Patnaik et al [15], 15% by Anson [7] and 3% by Miller[16].
Mc Cormak et al [17] calling high origin of ulnar artery as superficial ulnar artery found in 2.26% cases and was also observed by Adachi [8] in 1928, 7%,by Muller [18], in 2% and by Quains [19] in 1.7%.
Vare and Bansal [20] reported a case with high division of brachial artery- the superficial is the brachial artey and deep continuing in forearm as interosseus complex.
William et al [1] have mentioned that brachial artery may bifurcate proximally and reunite to form a single trunk. It trifurcates proximally into ulnar, radial, common interosseus arteries. Sometimes slender vasa aberrantia connect the brachial artery to the axillary artery or to one of the forearm arteries usually the radial.
Clinical application
1) This variation may cause difficulties while measuring the blood pressure.
2) Diagnostically it may disturb the evaluation of angiographic images.
3) Interventionally accidental puncture of superficially placed arteries may occur while attempting the venepuncture.
4) It is prone for damage during orthopedic and plastic surgeries.
When aberrant arteries are present it may be mistaken for a vein or in case of injury may cause severe bleeding..
Conclusion
Anomalies in origin and course of principal arteries have practical importance for orthopedicians, radiologists and vascular surgeons.
References
- Williams PL, Bannister LH, Berry M.N, Collins P, Dyson M, Dussek JE, Ferguson MWJ. Gray’s Anatomy. Cardiovascular system 38th Edn. Churchill Livingstone, New York, 1995 , pp1538-1540
- Huber GC. Piersol’s human anatomy in the vascular system 9th Edn. Vol. 1 J.B. Lippincott Co. Philadelphia, 1930 pp 767-791
- Treves, Rogers. Surgical applied anatomy In. the upper extremity. 11th Edn. Cassell and Co.Ltd. London, 1947, pp 247
- Karleson S, Niechajev A. arterial anatomy of the upper extremity. Acta Radiological Diagnosis 1982; 23 (7): 115-121
- Compta XG. Origin of radial artery from the axillary artery and associated hand vascular anomalies. Journal of Hand Surgey 16 A 1991; 16A: 293-296
- Charles C.M. et al. the origin of the deep brachial artery in American white and American negro males. Anatomical Records 1931; 50: 299-302.
- Anson B.J Morris human anatomy in the cardiovascular system- arteries and veins. Thomas M, Edr. Mc Graw Hill Book, New York 1966, pp 708-724
- Adachi B. Das Arterian system des japaner, Kyoto Name of the Journal?1928; 1: 205-210
- Keen JA. A study of arterial variations in the limbs with special reference to symmetry of vascular pattern. American Journal of Anatomy 1961; 108: 245-61
- Rosse Cornelius R, osse Penelope Gaddum, Hollinsheads textbook of anatomy. The free upper limb: arm, forearm and hand. 5th Edn. Lippincott-Raven publishers. Philadelphia, New York,1997, pp 255-258
- Patnaik VVG.,Kalse G, Sigla RK. Trifurcation of Brachial artery – a case report . Journal of the Anatomical Society of India 2001; 50 (2), 163-165
- Romans G.J. Cunningham’s Textbook of anatomy In . The blood vascular system. Arteries of the upper limb 10th Edn Walls E. W. Edr. Oxford university Press, New York 1964; pp 885-893.
- Massie G Surgical Anatomy In. The Upper limb 4th Edn. J& A. Churchill Ltd. London, 1944 , pp 136-139
- Bilodi AK, Sanikop MB. Variation in termination of brachial artery – A case report. Kathmandu Univ Med J 2004; 2 (1): 49-51.
- Patnaik VVG, Kalsey G, Singla RK. Branching pattern of brachial artery – a morphological Study. Journal of the Anatomical Society of India 2002; 51(2): 176-186.
- Miller RA. Observations upon the arrangement of axillary artery and brachial plexus. American Journal of Anatomy 1939; 64: 143-163
- Mc Cormack LJ, Cauldwell EW, Anson BJ. Brachial and antebrachial arterial pattern. Surgery Gynaecology Obstetrics 1953; 96: 43-54.
- Muller. Die Aron- Arlerian des Menschen. Anat.Hefte 22. 1903; 22: 379.
- Quains. The Anatomy of arteries of human body. Taylor and Walton. London, 1844
- Vare AM, Bansal PC. A case of anomalous brachial artery and other associate vascular anomalies in a single upper limb. Journal of Anatomical society of India 1969; 18 (2). 50-53