Research Article - Biomedical Research (2017) Volume 28, Issue 19
Analysis of the accuracy of low-strain air-barium imaging for the early diagnosis of gastric cardia carcinoma
Ji-Chao Pang1#, Yan-Ning Fu1#, Hong-Ying Fang2, Qian Xiang3, Ping-Huai Wang1 and Yu-Zhi Sun1*
1Department of Radiology, Chinese PLA General Hospital, Beijing, PR China
2Department of Radiology, Peking Union Medical College Hospital, Beijing, PR China
3Department of Radiology, Chengdu Aerospace Hospital, Chengdu, Sichuan, PR China
#These authors contributed equally to this paper
Accepted date: September 27, 2017
Abstract
Objective: To analyze the accuracy of low-strain air-barium imaging for the early diagnosis of gastric cardia carcinoma.
Methods: Thirty-seven patients with early gastric cardia carcinoma, as confirmed by gastrointestinal color Doppler ultrasound, low-strain air-barium imaging, gastroscopy, and pathological examination in our hospital from February 2016 to August 2017, were included in this study. The diagnostic accordance and adverse reaction rates of gastrointestinal color Doppler ultrasound were investigated on the basis of pathological results as standard. The imaging characteristics of early gastric cardia carcinoma were examined through low-strain air-barium imaging.
Results: The diagnostic accordance rates of gastrointestinal color Doppler ultrasound and low-strain air-barium imaging were 67.57% and 91.89%, respectively, and their difference was significant (P<0.01). Gastroscopy revealed the following: 21 cases of protrusion type, 11 cases of ulcer type, and 5 cases of flat type. Color Doppler ultrasound showed the following: 16 cases of protrusion type, 6 cases of ulcer type, and 3 cases of flat type. Low-strain air-barium imaging displayed the following: 21 cases of protrusion type, 10 cases of ulcer type, and 3 cases of flat type.
Conclusion: Low-strain air-barium imaging is a noninvasive, simple, and economical technique to examine gastric tissues directly. It yields a high diagnostic rate for early gastric cardia carcinoma and causes minimal adverse reactions. Hence, it is suitable for clinical applications.
Keywords
Low-strain air-barium imaging, Early gastric cardia carcinoma, Diagnosis
Introduction
Gastric cardia carcinoma is a common malignant tumor with a high incidence rate, especially in young patients, but the prognosis of gastric cardia carcinoma in early stages is good [1]. As such, early detection and treatment are necessary. However, the diagnosis of gastric cardia carcinoma is often incorrect or delayed. Although the accuracy of gastroscopy and pathological examination is high, examination procedures are painful, and the acceptance rate of patients is low [2,3]. In contrast to these procedures, low-strain air-barium imaging and gastrointestinal color Doppler ultrasound are noninvasive, painless, and easily accepted by patients [4]. In this study, 37 patients with early gastric cardia carcinoma, as confirmed by gastrointestinal color Doppler ultrasound, low-strain air-barium imaging, and gastroscopy, in our hospital from February 2016 to August 2017 were included and their medical records were analyzed to investigate the diagnostic accordance rate and imaging features of low-strain air-barium imaging.
Materials and Methods
General data and inclusion and exclusion criteria
The following patients were included: patients admitted to our hospital from February 2016 to August 2017; patients with early gastric cardia carcinoma confirmed by gastrointestinal color Doppler ultrasound and low-strain air-barium imaging; patients whose diagnosis was verified by gastroscopy; patients with poor treatment compliance; patients with primary organ failure; patients with abnormal cardiac function; and patients with informed consent.
The following patients were excluded: patients with incomplete clinical data and those who refused to cooperate with the treatment. Thirty-seven patients aged 32-69 years with an average age of 46.3 ± 2.8 years were included in this study. Of these patients, 23 were males and 14 were females. Symptoms included 18 cases of epigastric discomfort and satiety, 13 cases of dysphagia, and 6 cases of epigastric pain. Gastroscopy revealed the following: 21 cases of protrusion type, 11 cases of ulcer type, and 5 cases of flat type.
Examination method
Gastrointestinal color Doppler ultrasound: The patients were instructed to fast for over 12 h. Before the examination was performed, 500 mL of developing agent was mixed with glucose injection, shaken, and orally administered to the patients. The patients were then examined through color Doppler ultrasound (Zibo Chenlan Medical Equipment Sales Company Limited).
Low-strain air-barium imaging: On day 2, the patients fasted for 6 h and intramuscularly received 10 mg of anisodamine before they were examined. After 10 min, 3 mg of aerogenic powder mixed with 10 mL of warm water was orally administered. A digital gastrointestinal machine was manufactured by SIEMENS. After thoracic and abdominal fluoroscopy was completed, the patients at a standing position were orally administered with 100 mL of barium sulfate, and esophageal and cardiac openings were observed. The patients were rotated counterclockwise at a uniform velocity on the examination couch for three revolutions to coat barium evenly on the gastric wall, and the optimum position for observation was obtained. For the second time, the patients were rotated, and multi-axis observation was performed. The patients were allowed to bend down, and the cardia was examined in detail.
Statistical methods
Data were analyzed with SPSS 17.0, expressed as mean ± standard deviation (͞x ± s), and compared by performing a ttest. Frequencies were shown as percentage and analyzed through χ2 test. P>0.05 and P<0.05 indicated non-significant and significant differences, respectively.
Results
Diagnostic accuracy rate of the two examination methods
The diagnostic accuracy rates of gastrointestinal color Doppler ultrasound and low-strain air-barium imaging were 67.57% and 91.89%, respectively, and these values significantly differed (P<0.01; Table 1).
| Group | n | Accuracy | Delayed diagnosis | Misdiagnosis | Diagnostic accuracy rate (%) |
|---|---|---|---|---|---|
| Gastrointestinal color Doppler ultrasound |
37 | 25 (67.57) | 7 (18.92) | 5 (13.51) | 67.57 |
| Low-strain air-barium imaging | 37 | 34 (91.89) | 2 (5.41) | 1 (2.70) | 91.89 |
| χ2 | 6.7729 | ||||
| P | 0.0093 |
Table 1: Diagnostic accuracy rates of gastrointestinal color Doppler ultrasound and low-strain air-barium imaging (n, (%)).
Comparison of diagnostic type between the examination methods
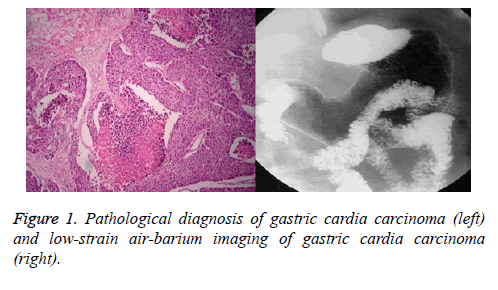
Gastroscopy revealed the following: 21 cases of protrusion type, 11 cases of ulcer type, and 5 cases of flat type. Gastrointestinal color Doppler displayed the following: 16 cases of protrusion type, 6 cases of ulcer type, and 3 cases of flat type. Low-strain air-barium imaging showed the following: 21 cases of protrusion type, 10 cases of ulcer type, and 3 cases of flat type. No significant differences were found between the two groups (P>0.05; Table 2 and Figure 1).
| Group | n | Protrusion-type | Ulcer-type | Flat-type | Delayed diagnosis, misdiagnosis |
|---|---|---|---|---|---|
| Gastrointestinal color Doppler ultrasound | 37 | 16 (43.24) | 6 (16.22) | 3 (13.51) | 12 (32.43) |
| Low-strain air-barium imaging | 37 | 21 (56.76) | 10 (27.02) | 3 (8.11) | 3 (8.11) |
Table 2: Comparison of the diagnostic types of gastrointestinal color Doppler ultrasound and low-strain air-barium imaging (n, (%)).
Discussion
Gastric cardia carcinoma is a common digestive malignant tumor with a high incidence rate accounting for approximately 5%. Poor diet and stress associated with modern life contribute to the yearly increase in the incidence of gastric cardia carcinoma among individuals, especially in the young population. The anatomic position of the cardia is unique, that is, it is the esophageal opening leading to the stomach, and its squamous epithelium possesses a distinct boundary with the gastric columnar epithelium [5]. An irregular cardia gland appearing tubular or branched measures 0.5-4 cm from the annular zone, and its width is approximately 2 cm. Over the past 30 years, the total incidence of gastric carcinoma has been decreasing, whereas the incidence of gastric cardia carcinoma has been increasing [6]. Obstruction in the gastric cardia does not easily occur because of its anatomical features, which differ from those of esophageal carcinoma. The small volume of cardiac carcinoma in its early stages does not readily cause obstruction, and its characteristic symptoms are absent. Difficulty in swallowing possibly induces the progression of carcinoma. The symptoms of gastric cardia carcinoma include mild abdominal discomfort, abdominal distention, indigestion, and dysphagia, but these symptoms are nonspecific and consequently do not alert patients [7]. Patients seek medical help if dysphagia becomes aggravated. Another initial symptom of cardia carcinoma is upper gastrointestinal bleeding, such as hematemesis or asphalt. Patients with severe conditions may collapse, experience shock, or suffer from serious anemia. Gastric cardia carcinoma is also easily misdiagnosed as peptic ulcer bleeding because of the absence of choking symptoms. The pancreas and other retroperitoneal tissues of patients with advanced disease are affected, and persistent dull pain is experienced in the upper abdomen and the lower back. No positive signs are detected in patients with early cardiac carcinoma [8]. Anemia, hypoproteinemia, emaciation, dehydration, or low-protein edema are also observed in patients with middle and advanced stages. If abdominal mass, hepatomegaly, ascites, pelvic mass. Although it is a malignant tumor, the prognosis of early cardiac cancer is better. Therefore, this disease must be detected and treated in early stages.
Cardiac topographic anatomy is complex. The mucosal arrangement of this area is basically irregular, and many benign or physiological variations are observed [9]. It is located below the costal arch, and no peristalsis occurs. Consequently, misdiagnosis or delayed diagnosis is often encountered in clinical examinations. Although the accuracy rates of gastroscopy and pathological examination are higher, pain during examination is greater and the rate of acceptance is lower. Low-strain air-barium imaging and gastrointestinal color Doppler ultrasound examinations are noninvasive and painless and are therefore easily accepted by patients. However, images produced by gastrointestinal color Doppler ultrasound are characterized by some limitations, which result in difficulty in diagnosis [10]. The rates of misdiagnosis and delayed diagnosis are higher. X-ray manifestations of early cardia carcinoma are as follows [11]: polyploid-like filling defect; mild leaflet without pedicle; disrupted peripheral mucosa; small barium spots on the polyp surface; cardia stenosis; stiffness; poor expansibility; barium shunt; uneven, interrupted, and distorted peripheral mucosa; a niche with irregular edges and uneven density; flattened cardiac mucosal folds; irregular and amorphous barium staining area; and thickened gastric cardia wall of more than 2 cm. This study demonstrated that the accuracy rates of gastrointestinal color Doppler ultrasound and low-strain air-barium imaging examination were 67.57% and 91.89%, respectively, and these values significantly differed (P<0.01). Pathological examination and gastroscopy revealed the following: 21 cases of protrusion type, 11 cases of ulcer type, and 5 cases of flat type. Gastrointestinal color Doppler ultrasound displayed the following results: 16 cases of protrusion type, 6 cases of ulcer type, and 3 cases of flat type. Low-strain air-barium imaging showed the following: 21 cases of protrusion type, 10 cases of ulcer type, and 3 cases of flat type.
Conclusion
Low-strain air-barium imaging is a non-invasive, simple, economical, and direct examination technique with a high diagnostic rate for the early diagnosis of gastric cardia carcinoma. Its induced adverse reactions are less than those of other methods. Thus, this technique is suitable for clinical applications. However, our study is limited by various factors. Only the patients in our hospital in this region were included. In the future, research scope and samples should be expanded to confirm the value of low-strain air-barium examination in the early diagnosis of cardiac carcinoma.
References
- Colak MC, Colak C, Erdil N, Sandal S. Potential risk factors for early large pleural effusion after coronary artery bypass grafting surgery. Biomed Res-India 2017; 28: 625-629.
- Trawicki MC, Volz LM. Epidural for high-dose radiation brachytherapy in a noncompliant, super-obese patient with severe pulmonary hypertension. Saudi J Anaesth 2017; 11: 343-345.
- Chen J, Du F, Hu B, Chi C, Chu H, Jiang L, Li P, Gong Z5. Severe Cardiotoxicity in a Patient with Colorectal Cancer Treated with Bevacizumab. Anticancer Res 2017; 37: 4557-4561.
- Colak MC, Colak C, Erdil N, Sandal S. Potential risk factors for early large pleural effusion after coronary artery bypass grafting surgery. Biomed Res-India 2017; 28: 625-629.
- Xing J, Lu J. Effects of mTOR on Neurological Deficits after Transient Global Ischemia. Transl Neurosci 2017; 8: 21-26.
- Zhang L, Yang Y, Zhang J, Zhou X, Dong H, Zhou Y. Barium sulfate aspiration: Severe chemical pneumonia induced by a massive reflux of contrast medium during small bowel barium enema. Forensic Sci Int 2015; 253: 16-19.
- Rule R, Baschar H, Cordiviola C, Prozzi G, Farina OH. Pharmacokinetics and Tissue Penetration of Ceftazidime Administered During Hysterectomy and Oophorectomy in Canine Females. Lat Am J Pharm 2014; 33: 1579-1582.
- Hirano Y, Hattori M, Yagi D, Maeda K, Douden K, Hashizume Y. Laparoscopic surgery for the ascending colon cancer associated with malrotation of the midgut. Indian J Surg 2013; 75: 71-73.
- Jiang XW, Ge CX, Ge SF, Li WL. Potential Bisphenol AF-Irinotecan Interaction during the Treatment of Renal Cell Carcinoma. Lat Am J Pharm 2016; 35: 2036-2040.
- Boiron M, Benchellal Z, Alison D, Huten N. Impaired air-liquid settling during swallowing in gastroesophageal reflux disease. A digital videofluoroscopic study. Dis Esophagus 2009; 22: 68-73.
- Kurkcu R. The comparison of body composition bioelectrical impedance analysis method of primary school students who do and don’t do exercise. Biomed Res-India 2017; 28: 1107-1109.