Research Paper - Otolaryngology Online Journal (2016) Volume 6, Issue 3
A Risk Factor for Stroke from the ENT Clinic: Plaque or Cardiogenic Embolism?
Koichi Tsunoda1*, Kenji Ito2, Sotaro Sekimoto2, Atsunobu Tsunoda2 and Tatuya Yamasoba3
1Department of Artificial Organs and Otolaryngology, National Hospital Organization Tokyo Medical Center, Tokyo, Japan
2Department of Otolaryngology Head and Neck Surgery, Tokyo Medical and Dental University, Tokyo, Japan
3Department of Otolaryngology Head and Neck Surgery, Tokyo University, Tokyo, Japan
- *Corresponding Author:
- Koichi Tsunoda
Department of Artificial Organs and Otolaryngology, National Hospital Organization Tokyo Medical Center, 2-5-1 Higashigaoka, Meguro-ku, Tokyo, 152-8902, Japan
Tel: 81-3-3411-0111
Fax: 81-3-3411-0185
E-mail: tsunodakoichi@kankakuki.go.jp
Received date: June 08, 2016; Accepted date: June 13, 2016; Published date: June 17, 2016
Abstract
Objective: We previously suggested that aberrations of the carotid arteries, which may occur when the neck is bent forward, should be considered as new risk factors for ischemic stroke. We analyzed the results of carotid artery ultrasound examination in previous case and control groups, focusing in particular on the atherosclerotic risk factor in stroke, to determine the significance of arterial aberration and its relation to ischemic stroke. Data Sources and Review Methods: We analyzed the original data from our previous 235 casecontrol study patients among those who underwent complete routine cervical ultrasound and had all cholesterol data available. Results: Although plaque was present in the CCA in about one-half of the control group, none had experienced a stroke. At the same time, two-thirds of the case (stroke) patients had plaque in the CCA. This indicates that plaque tends to be a risk for stroke, although the difference between the two groups was not statistically significant. Conclusion: The results of the present analysis indicate that: 1) the degree of atherosclerosis was the same in both the case and control groups, because there were no statistically significant differences between them in cholesterol values; 2) the only difference between the two groups was the aberration of the carotid artery; and 3) aberration of the carotid artery tends to be a risk factor for stroke. The mechanism of cerebral infarction is speculated to be artery-to-artery embolism from the carotid plaque. The aberration of the carotid artery occurs, which triggered by plaque reaching the cerebellum.
Keywords
Head and neck, Carotid artery, Aberration, embolism, plaque
Introduction
Carotid abnormalities (CAs) are found in more than half of patients with cardiovascular or cerebral ischemic symptoms who undergo ultrasound examination. Atherosclerosis, hypertension, and aging may all play an important role in the development of CAs, although aging appears more important than atherosclerosis [1]. On the other hand, one study suggested that CAs are not important stroke risk factors [2]. Previous studies mainly focused on the cervical common carotid artery (CCA) and the sections of the external and internal carotid arteries around the CCA bifurcation.
However, aberration of the internal carotid artery (ICA) sometimes occurs inside the mouth in elderly patients with bent posture [3], which is difficult to diagnose in ultrasound examination. Patients with asymptomatic carotid artery stenosis who have a 60% or greater reduction in arterial diameter and whose general health makes them good candidates for elective surgery will have a lower 5-year risk of ipsilateral stroke if carotid endarterectomy performed with less than 3% preoperative morbidity and mortality is added to aggressive management of modifiable risk factors [4]. However, even when magnetic resonance angiography (MRA) is performed within 2 months after actual aberration occurs it is difficult to detect such aberrations because ultrasound or MRA studies are performed in the supine rather than seated position [5].
We previously suggested that aberrations of the carotid arteries in the head (ICA) [6] and neck (common carotid artery, CCA) [7], which may occur when the neck is bent forward, should be considered as new risk factors for ischemic stroke. In addition, a casecontrol study suggested that aberrant (Ab)-ICA and Ab-CCA were risk factors for stroke and that bent (head-down) posture was a risk factor for the development of aberrant arteries [8].
Although patients with lacunar infarction were excluded from the case group in our previous study, we wanted to determine the actual cause of stroke. Why were the aberrations related to ischemic stroke? Were they due to plaque or cardiogenic embolism? We therefore decided to analyze the results of carotid artery ultrasound examination in the same case and control groups, focusing in particular on the atherosclerotic risk factor in stroke, to determine the significance of arterial aberration and its relation to ischemic stroke.
Methods
We analyzed the original data from our previous case-control study [8] using the chi-squared test and paired t-test. This case-control study was performed at the National Hospital Organization Tokyo Medical Center after the Ethics Committee of each had approved the study protocol. We compared the presence or absence of Ab-ICA or Ab-CCA and of plaque in the cervical carotid artery between 72 stroke patients and 163 individuals in the control group. The total cholesterol, triglyceride, low-density lipoprotein cholesterol, and high-density lipoprotein cholesterol levels were also compared between the two groups. The previous study specifically examined the relationships among bent posture, height loss, aberration of the carotid arteries, and ischemic stroke risk in a case-control manner. Both case and control patients with established risk factors for stroke, such as a history of atrial fibrillation, arrhythmia, heart valve disease, diabetes, blood clotting abnormalities (hematocrit >55%, platelet count >500,000/μl), and who were receiving anticoagulant therapy were excluded from the study [7]. Furthermore, among the 235 patients, only 24 underwent complete routine cervical ultrasound and had all cholesterol data available. As a result, the current analysis involved only a subset of 9 in the control group (without ischemic stroke) and 15 stroke patients in the case group.
Results
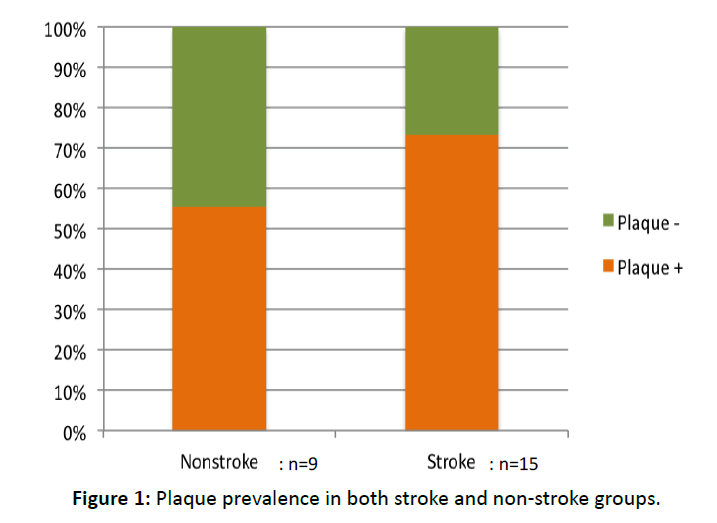
The characteristics of the case and control groups are shown in (Table 1). There were no arterial aberrations in the control group. On the other hand, all ischemic stroke patients were found to have Ab- ICA or Ab-CCA. Cervical ultrasound examination of the carotid artery detected plaque in 5 of 9 in the control group and in 11 of 15 in the case group. As shown in (Figure 1), plaque prevalence was higher in the stroke group than in the control group, although the difference did not reach statistical significance (odds ratio=0.45; 95% CI=0.06–3.1; Fisher’s P-value=0.32; Table 2).
| Stroke | ICA/CCA Aberration | Plaque | TC mg/dl | TG mg/dl | LDL mg/dl | HDL mg/dl | ||
|---|---|---|---|---|---|---|---|---|
| Non-stroke controls | 1 | ? | ? | ? | 248 | 254 | 143 | 54 |
| 2 | ? | ? | ? | 254 | 231 | 154 | 54 | |
| 3 | ? | ? | ? | 225 | 129 | 136 | 63 | |
| 4 | ? | ? | ? | 173 | 99 | 85 | 68 | |
| 5 | ? | ? | + | 255 | 79 | 169 | 70 | |
| 6 | ? | ? | + | 213 | 156 | 100 | 82 | |
| 7 | ? | ? | + | 217 | 75 | 121 | 81 | |
| 8 | ? | ? | + | 208 | 153 | 120 | 57 | |
| 9 | ? | ? | + | 238 | 120 | 155 | 59 | |
| Ischemic stroke cases | 1 | + | + | ? | 216 | 134 | 123 | 66 |
| 2 | + | + | ? | 196 | 98 | 131 | 45 | |
| 3 | + | + | ? | 238 | 79 | 162 | 60 | |
| 4 | + | + | ? | 244 | 136 | 133 | 65 | |
| 5 | + | + | + | 262 | 516 | 105 | 53 | |
| 6 | + | + | + | 257 | 102 | 189 | 47 | |
| 7 | + | + | + | 244 | 113 | 180 | 41 | |
| 8 | + | + | + | 177 | 115 | 72 | 82 | |
| 9 | + | + | + | 249 | 174 | 159 | 55 | |
| 10 | + | + | + | 224 | 307 | 81 | 81 | |
| 11 | + | + | + | 186 | 124 | 117 | 44 | |
| 12 | + | + | + | 205 | 215 | 116 | 46 | |
| 13 | + | + | + | 127 | 107 | 75 | 36 | |
| 14 | + | + | + | 218 | 111 | 151 | 44 | |
| 15 | + | + | + | 258 | 225 | 169 | 44 |
Table 1: Stroke occurrence, arterial aberration, plaque presence, and cholesterol values in the two groups in the current subset analysis.
| Stroke (N=15) | Non-stroke (N=9) | Odds ratio (95%CI) | P value | |
|---|---|---|---|---|
| Plaque | 11 (73.3%) | 5 (55.6%) | 0.4545 (0.07-3.07) | 0.32 |
| ICA/CCA abberration | 15 (100%) | 0 | INF | 7.6E-7 |
Table 2: Stroke patients and non-stroke controls with and without plaque and arterial aberration.
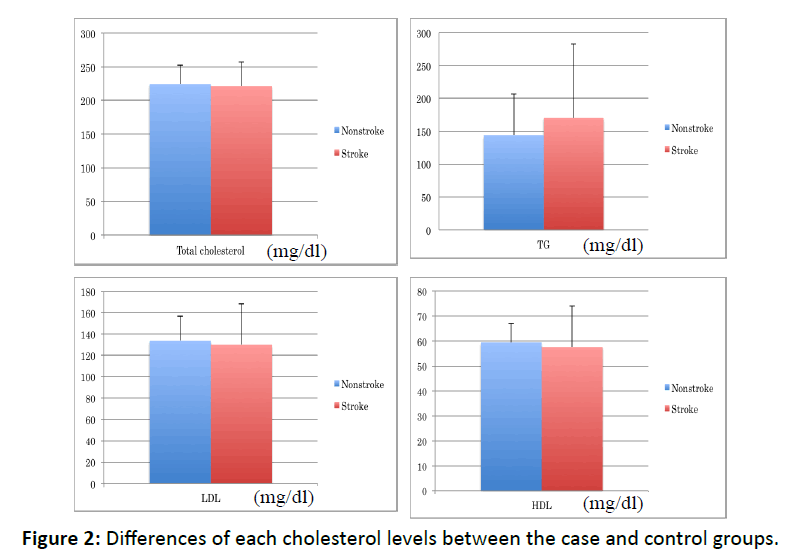
(Figure 2) shows the differences between total cholesterol, triglyceride, low-density lipoprotein cholesterol, and high-density lipoprotein cholesterol levels between the case and control groups. The t-test results indicated no significant differences in cholesterol ratios between the two groups.
Discussion
Based on previous results, we estimated that the risk of ischemic stroke was 90.2% based on carotid artery aberration and 91.4% when all risk factors (aberration of the carotid artery, height loss, bent posture) were analyzed. Aberration of carotid arteries caused by cervical bent posture was found to predict ischemic stroke risk in the previous casecontrol study [8]. The purpose of that study was to evaluate the accuracy of aberration of the carotid artery as an ischemic stroke risk factor, and therefore patients with established risk factors for stroke were excluded. Thus the subset of patients analyzed in this study was much smaller.
Although plaque was present in the CCA in about one-half of the control group, none had experienced a stroke. At the same time, two-thirds of the case (stroke) patients had plaque in the CCA. This indicates that plaque tends to be a risk for stroke, although the difference between the two groups was not statistically significant.
We previously treated patients in whom plaque caused ischemic stroke when their carotid artery became bent. Those patients reported an unusual strange sensation (USS) when the aberration occurred. The USS around the pharynx results from a separation of the pharyngeal wall, which contains the mucosa, submucosa, and superior pharyngeal constrictor muscle, due to Ab-ICA. When that separation occurs, patients feel a USS in the throat. The experience in treating those patients suggested that the occurrence of the separation indicates an increased risk of stroke in the near future and that an ischemic embolism could be triggered [5].
Conclusion
The results of the present analysis indicate that: 1) the degree of atherosclerosis was the same in both the case and control groups, because there were no statistically significant differences between them in cholesterol values; 2) the only difference between the two groups was the aberration of the carotid artery; and 3) aberration of the carotid artery tends to be a risk factor for stroke. The mechanism of cerebral infarction is speculated to be artery-toartery embolism from the carotid plaque. In other words, plaque in the carotid arteries causes an ischemic stroke when aberration of the carotid artery occurs, triggered by plaque reaching the cerebellum.
Acknowledgments
This research was supported by a Grant-in-Aid for Clinical Research from the National Hospital Organization, Japan.
References
- Del Corso L, Moruzzo D, Conte B, Agelli M, Romanelli AM, et al. (1998) Tortuosity, kinking, and coiling of the carotid artery: expression of atherosclerosis or aging? Angiology49: 361-371.
- Togay-I?ikay C, Kim J, Betterman K, Andrews C, Meads D, et al. (2005) Carotid artery tortuosity, kinking, coiling: stroke risk factor, marker, or curiosity? ActaNeurolBelg105: 68-72.
- Tsunoda K, Takanosawa M, Matsuda K (1997) Aberrant internal carotid artery in the mouth.Lancet350:340.
- (1995) Executive Committee for the Asymptomatic Carotid Atherosclerosis Study. Endarterectomyfor asymptomatic carotid artery stenosis. JAMA 273: 1421-1428.
- Suto Y, Tsunoda K, Chong T, Morita Y, Nakamura Y, et al. (2011) Common but critical sensation in older adults. J Am GeriatrSoc59: 1963-1964.
- Tsunoda K, Sakai Y, Kikkawa YS, Aikawa J, Murakami R (2003) Bent (head-down) posture and aberrant internal carotid artery in the mouth. A new risk factor for stroke? Ann Intern Med 139:W-56.
- Tsunoda K, Bitou S, Shinogami M (2005) Bent (head-down) posture and aberrant common carotid arteries ofthe neck: Another new risk factor for stroke? Laryngoscope115:2074-2075.
- Tsunoda K (2011) for the Research Group on the Relationship of Bent Posture and Stroke, National Hospital Organization. Height loss caused by bent posture: A risk factor for stroke from the ENT clinic—is it time to reconsider the physical examination?ActaOtolaryngol131: 1079-1085.