Research Article - Biomedical Research (2016) Volume 27, Issue 4
A case of osteomalacia initially followed as restless leg syndrome for 6 months
Ceyhun Varım1*, Bilgehan Atılgan Acar2, Turkan Atılgan Acar2 and Neslihan Aybala Alagoz21Department of Internal Medicine, Sakarya University Training and Research Hospital, Sakarya, Turkey
2Department of Neurology, Sakarya University Training and Research Hospital, Sakarya, Turkey
Received date: April 19, 2016; Accepted date: May 25, 2016; Published date: May 29, 2016
Abstract
Osteomalacia is a bone disease, characterized by the inability of newly formed bone matrix to undergo mineralization. The most common symptoms are generalized bone pain and widespread body pain, while some patients are asymptomatic. Restless leg syndrome (RLS) is a sensory-motor neurological disease. The main symptoms are abnormal sensations in the legs and dysesthesia. Symptoms worsen at night and affect sleep quality. We present a case of a woman with a progressive hip and feet pain. Many biochemical, clinical, and radiological tests were performed for diagnosis. All were found to be normal. The patient was diagnosed as having RLS. 0.25 mg pramipexole was given for treatment. Patient symptoms patient escalated over six months. The patient was reassessed after six months. Vitamin D levels had not been previously examined. We found low vitamin D and calcium levels, as well as pseudofractures in radiography. The diagnosis was changed to osteomalacia. Vitamin D and calcium treatment were started. Symptoms began to regress from the first week of treatment.
Keywords
Osteomalacia, Vitamin D deficiency, Restless leg syndrome.
Introduction
Osteomalacia is a bone disease characterized by the inability of newly formed bone matrix to undergo mineralization, as well as low bone density. Hence, the ratio of mineralized bone to matrix is reduced and the amount of non-calcified matrix is increased [1]. Osteomalacia divided into four types: osteomalacia with vitamin D deficiency; osteomalacia with hypophosphatemia; osteomalacia with changed metabolism of vitamin D; and osteomalacia with normal calcium and phosphorus metabolism [2]. Osteomalacia with vitamin D deficiency is the most common type worldwide. Osteomalacia prevalence is about 42/100,000 people.
Vitamin D is required for bone formation and absorption of calcium and phosphorus minerals. It is synthesized in the skin and in the body from its predecessors. There are two basic vitamin D predecessor sources, vegetable and animal. Vitamin D2 is known as ergocalciferol and its origin is vegetable food. Vitamin D3 is known as cholecalciferol and its origin is animal food and sunlight. Vitamin D facilitates the absorption of calcium and phosphorus from the gut and stimulates phosphorus reabsorption from the kidneys. Also, vitamin D controls calcium and phosphorus homeostasis in bodily fluids and tissue with calcitonin and parathormone [3].
Restless leg syndrome (RLS) is a sensory-motor neurological disease. The typical clinical features of RLS include an irresistible urge to move the legs that prevent falling asleep, accompanied by dysesthesia and motor restlessness. Symptoms may be unilateral at the onset of disease but over time begins to affect both lower extremities together. Symptoms with a circadian property are characteristic of RLS [4].
Osteomalacia with vitamin D deficiency is usually asymptomatic. The main clinical features are widespread pain that affects hip, vertebrae, ribs and the lower extremities [5]. Other symptoms include bone tenderness, proximal muscle weakness, and loss of muscle tissue [5-7]. Fractures and pseudofractures may occur with little or no trauma, typically involving the ribs, vertebrae, and long bones [6]
We describe the case of a woman with a progressive hip and feet pain. The patient was diagnosed with RLS but the symptoms of the patient increased over a six-month period. The diagnosis was changed as osteomalacia. Vitamin D and calcium treatment were started. The patient's symptoms began to regress from the first week.
Case
A 29-year-old Caucasian female patient presented to the orthopedic clinic with symptoms of pain both two hips and feet which had been present for about six months. Right hip pain was more than the left. The pain was aggravated by activity and was independent from sleeping. The patient's blood count (CBC), erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) levels were measured. These examinations were normal. A right sacroiliac magnetic resonance imaging (MRI) was performed and was normal. The patient was undiagnosed by orthopedic clinic. Then patient was presented to the neurology clinic. Electromyography (EMG) was performed by the neurologist and was normal. Restless legs syndrome was diagnosed. 0.25 mg pramipexole was given for treatment.
The patient’s pain was not reduced and also difficulty in moving was started. Because of these symptoms, the patient was presented to our clinic. A detailed anamnesis was taken from the patient. She was a secretary and preferred a conservative or ‘closed’ clothing style. There was no history of chronic diseases such as diabetes mellitus, hypertension, trauma, chronic diarrhea, malabsorption, lactose intolerance, drinking, smoking and history of surgery. Her family history was out of chronic diseases. She was married and had one son at five years old. Her menstrual periods are normal. She lived in Sakarya, which is a city in the eastern Marmara region of Turkey. The annual sunshine duration of Sakarya is 2190 hours/year, well below the average for Turkey (2623 hours/ years). On the physical examination, she was afebrile, and vital signs were stable. The patient's muscles and joints were examined. Redness, pain, swelling, and heat rise were not detected at the joints, but pain and sensitivity was found in the proximal muscles and BMI was measured at 32.3 kg/m2. Neurological examination was performed by a neurologist. The neurologic examination was unremarkable Examination of the lower extremities revealed deformity without any motor deficit. There was no evidence of central and peripheral findings giving lateralization and localization. The questions for the diagnosis of RLS were posed to the patient. Her answers were not compatible with RLS.
Biochemical examinations were made after the anamnesis and physical examination. ESR, CRP, CBC, Thyroid Function Test (TFT), vitamin B12, ferritin, liver and kidney function tests were normal. There was no increase in inflammatory markers such as ESR, CRP, or Brucella agglutination, and Gruber Widal tests were negative. Calcium [8.2 mg/dl (8.6-10 mg/dl)], phosphorus [2.4 mg/dl (2.5-4.5 mg/dl)] and 25- hydroxycholecalciferol levels were reduced [8.6 ng/dl (25 ng/dl and higher)]; ALP [127 U/L (35-105 U/L)] and parathormone levels were elevated [80.9 pg/ml (10-72 pg/ml)].
Osteoporosis and osteomalacia were considered after anamnesis and biochemical examinations. Dual-energy x-ray absorptiometry (Dexa) was performed for diagnosis of osteoporosis and pelvic radiography were performed for diagnosis of osteomalacia.
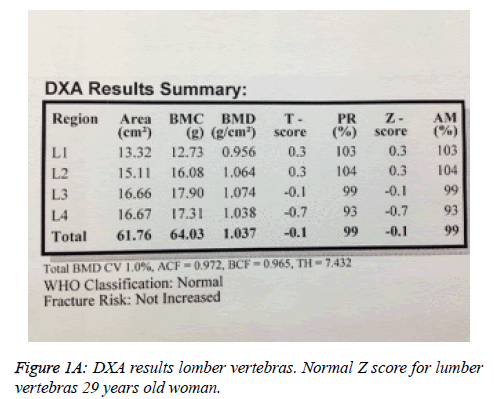
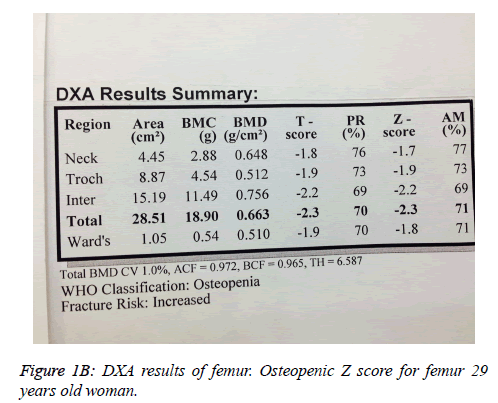
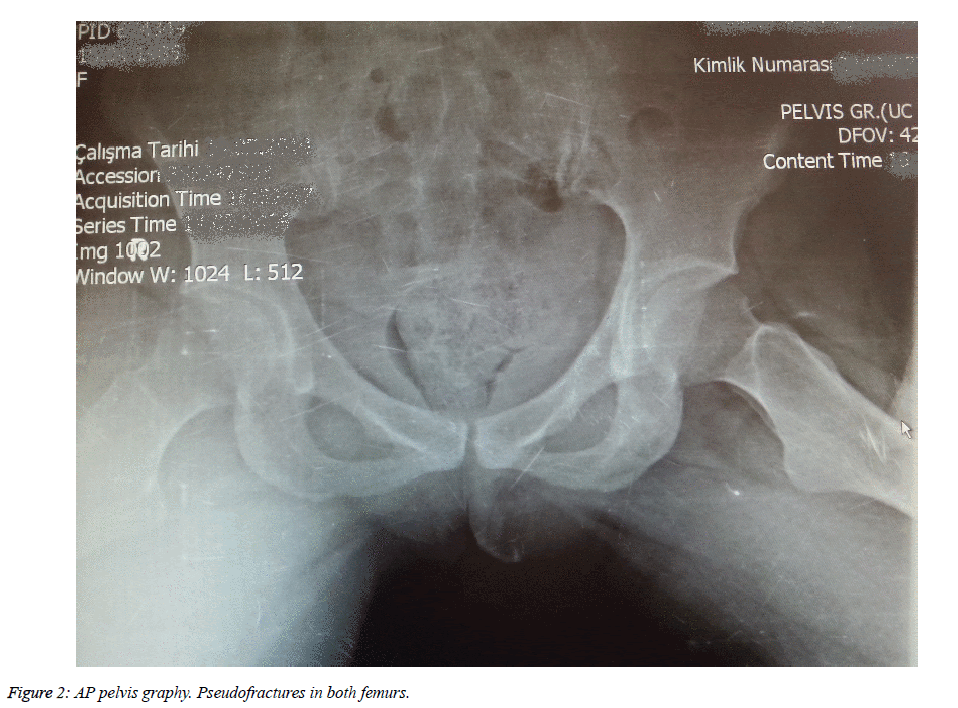
L1-L4 T and Z scores were -0.1, while hip T and Z scores were -2.3 for bone mineral density (Figures 1A and 1B). There were pseudofractures known as Milkman Fractures in both femurs in the anteroposterior pelvic radiography (Figure 2).
These findings were consistent with osteomalacia with vitamin D deficiency. 50,000 IU/week of oral cholecalciferol was started and pramipexole treatment was stopped. Treatment was changed to 1500-2000 IU/day maintenance treatment after eight weeks. Oral calcium supplements (500 mg/day ionized calcium) were started for hypocalcemia. The patient's symptoms began to movement from the first week. First, pain in the hip and feet reduced within a few days. Then, movement was improved. Her vitamin D levels increased to 68.4 ng/dl, while calcium levels increased to 9.8 mg/dl. Dual energy X-Ray absorptiometer (DXA) was planned for the first year of treatment. RLS was thought to be an incorrect diagnosis after treatment with oral cholecalciferol.
Discussion
The most important source of vitamin D is the skin, which is generated when sunlight strikes the skin itself. Living and working areas, as well as religious beliefs, directly affect the relationship with sunlight. The amount of daily solar light begins to decrease. Muslim women prefer closed clothing style. This leads not being able to benefit from sunlight. 23% of the world population is Muslim and half of these are women. Approximately 800000 Muslim women are at risk. Haq et al. reported vitamin D deficiency about 80% in the women in United Arab Emirates, Saudi Arabia, and other Middle Eastern countries [8]. 90% of the world population lives in the Northern Hemisphere. Almost five billion people are not able to fully benefit from sunlight. Industrialization is increasing rapidly around the world. This also leads to more people working indoors. Because of these reasons, osteomalacia with vitamin D deficiency is the most common type in the all around the world.
In the literature, most cases of vitamin D deficiency are induced osteomalacia in the Northern Hemisphere [9-11]. Our patient is a Muslim from Turkey. This is consistent with the literature.
Osteomalacia is seen under age of 50 years. Secondary osteoporosis (SO) is defined as low bone mass due to drug use or disease. It is usually seen under the age of 50 [12]. Secondary osteoporosis should be considered in the differential diagnosis of osteomalacia. Diseases causing SO may be excluded with a good medical history. Definite diagnosis of osteomalacia is confirmed by bone biopsy [13]. Bone mineral density (BMD) is not used in the diagnosis of osteomalacia and differential diagnosis of osteoporosis. A dual energy X-Ray absorptiometer measurements can be used to see the condition of the bones. BMD may be normal or slightly reduced in patients with osteomalacia, but measurement is recommended before starting treatment.
Osteomalacia has no specific symptoms. The main clinical features are widespread pain that affects hip, vertebrae, ribs and the lower extremities [5]. The pain is characterized as dull and aching and is aggravated by activity and general weight bearing. Fractures and pseudofractures may occur with little or no trauma, typically involving the ribs, vertebrae, and long bones [9]. The muscle weakness is characteristically proximal and may be associated with muscle wasting, hypotonia, and discomfort with movement [6].
Vitamin D, ALP, and PTH levels tend to have increased, while calcium and phosphorus levels tend to have decreased in these patients. Diagnosis is usually based on patient symptoms and these laboratory parameters.
Our patient was presented with proximal pain, the pseudofractures were found in the radiography and laboratory parameters were consistent with osteomalacia. L1-L4 T and Z scores were -0.1, while hip T and Z scores were -2.3 for bone mineral density (Figures 1A and 1B). These findings were consistent with the literature.
Restless legs syndrome (RLS), also called Willis-Ekbom disease, is a disease characterized by need or urge to move the legs, usually accompanied by discomfort or annoyance. Symptoms are worse or exclusively present at rest or inactivity, sitting, or lying down. Symptoms are totally or partially relieved with movement. Perceived symptoms during rest and inactivity worsen or occur exclusively at night. The above symptoms are not better explained by other diseases or conditions [14]. These are diagnostic criteria of RLS. Patients must present with all criteria for diagnosis. Diagnosis is based on reported or observed symptoms in the patients. There is no radiologic, biochemical, or laboratory tests for diagnosis [14].
An extensive medical history was not taken from the patient. The doctor did not ask questions concerning RLS, and the methods of diagnosis and the diagnosis itself were incorrect. Our patient had no RLS symptoms. CRP, ESR, and CBC levels were found to be in the normal range. EMG and MRI were carried out. EMG is not typically used in the diagnosis of RLS. Pramipexole is the first line treatment of RLS, and low doses of dopaminergic agents are also used. Our patient used pramipexole, but the diagnosis was incorrect. There was no regression in symptoms with medical treatment. For these reasons, we did not suspect RLS in our patient and carefully reviewed the diagnosis. She had a history of inadequate sunlight exposure. We measured vitamin D levels and found them to be low. Other laboratory tests and radiological examinations were consistent with osteomalacia.
Conclusion
Osteomalacia is a common disease in muslim countries and should not be neglected, especially in female patients who get less contact with sunlight. Detailed anamnesis must be taken from all patients. Examinations for osteomalacia are indicated in patients presenting with symptoms such as difficulty in walking or muscle and joint pain.
References
- The Society of Endocrinology and Metabolism of Turkey. Diagnosis and treatment of metabolic bone diseases. SEMT 2014.
- Fabbriciani G, Pirro M, Leli C, Cecchetti A, Callarelli L, Rinonapoli G, Scarponi AM, Mannarino E. Diffuse muscoskeletal pain and proximal myopathy: do not forget hypovitaminosis D. J ClinRheumatol 2010; 16: 34-37.
- Thacher TD, Clarke BL. Vitamin D insufficiency. Mayo ClinProc 2011; 86: 50-60.
- Benbir D, Kaynak H. Restless Legs Syndrome and Periodic Limb Movement in sleep Disorders. Turkish Journal of Neurology 2014; 10: 117-123.
- Bhan A, Rao AD, Rao DS. Osteomalacia as a result of vitamin D deficiency. Endocrinol Metab Clin North Am 2010; 39: 321-331.
- Lips P, van Schoor NM, Bravenboer N. Vitamin D-related disorders. In: Rosen CJ, Compston JE, Lian JB (Eds) Primer on the metabolic bone diseases and disorders of mineral metabolism. (7thedn) American Society for Bone and Mineral Research, Washington, USA.
- Gifre L, Peris P, Monegal A, Martinez de Osaba MJ, Alvarez L, Guañabens N. Osteomalacia revisited : a report on 28 cases. ClinRheumatol 2011; 30: 639-645.
- Haq A, Svobodová J, Imran S, Stanford C, Razzaque MS. Vitamin D deficiency: A single centre analysis of patients from 136 countries. J Steroid BiochemMolBiol 2016.
- Mac-Way F, Azzouz L, Noel C, Lafage-Proust MH. Osteomalacia induced by vitamin D deficiency in hemodialysis patients: the crucial role of vitamin D correction. Journal of bone and mineral metabolism 2014; 32: 215-219.
- Oh RC, Johnson JD. Chest pain and costochondritis associated with vitamin d deficiency: a report of two cases. Case Rep Med 2012; 2012: 375730.
- Kim SY, Rhee SY, Moon SY, Chon S, Jeong IK, Oh S, Kim JW. A case of osteomalacia caused by severe vitamin D deficiency. Journal of Korean Endocrine Society 2007; 22: 55-61.
- Painter SE, Kleerekoper M, Camacho PM. Secondary osteoporosis: a review of the recent evidence. EndocrPract 2006; 12: 436-445.
- Peach H, Compston JE, Vedi S, Horton LW. Value of plasma calcium, phosphate, and alkaline phosphatase measurements in the diagnosis of histological osteomalacia. J ClinPathol 1982; 35: 625-630.
- http://irlssg.org/diagnostic-criteria/