- Biomedical Research (2016) Volume 27, Issue 2
A case of orthodontic treatment with an atypical pain disorder.
| Masato Kaku1*, Shunichi Kojima1, Hiromi Sumi1, Hanaka Shikata1, Shotoku Kojima1, Taeko Yamamoto1, Tahsin Raquib Abonti1, Yuka Yashima1, Toshitsugu Kawata2 and Kotaro Tanimoto1 1Department of Orthodontics, Applied Life Sciences, Hiroshima University Institute of Biomedical & Health Sciences, 1-2-3 Kasumi, Minami-ku, Hiroshima 734-8553, Japan 2Department of Orthodontics, Kanagawa Dental University 82 Ineoka-cho, Yokosuka-city Kanagawa 238-8580, Japan |
| Corresponding Author: Masato Kaku, Department of Orthodontics, Hiroshima University, Japan. |
| Accepted: January 28, 2016 |
Abstract
This report shows an orthodontic treatment case with a pain disorder. The patient complained of impaired molar masticatory function after a first orthodontic treatment. The lower midline was shifted to the right direction caused by initial occlusal contact at second molars. She had also severe upper molar spontaneous pain, although there was no organic disease at this area. During second orthodontic treatment, the pain increased gradually. She was diagnosed as a Pain disorder (PD) and Tricyclic antidepressants (TCAs) was administered at the pain clinic. Two month after medicinal treatment, the patient stated that the pain had completely disappeared. Also a good occlusion was achieved by the second orthodontic treatment after 1 year. She did not have a pain without any medication and occlusion continued to be stable during these 5 years. Because an atypical odontalgia increases these days, orthodontists should have the knowledge of this disease and appropriate coping to a patient is necessary. There are a few patients with dental pain without any identifiable dental etiology. Such patients are classified under the category of atypical odontalgia. Because an atypical odontalgia such as somatoform pain disorder increases these days, orthodontists should have the knowledge of this disease and appropriate coping to a patient is necessary. This case report suggests that it is possible that PD can be caused by improper orthodontic treatment and dentists should care much about atypical odntalgia such as somatoform pain disorder.
Keywords |
||||||||
| Pain disorder, Non-odontogenic toothache, Tricyclic antidepressant. | ||||||||
Introduction |
||||||||
| Toothache is a general complaint for patients who come to a dental clinic. In most cases, these odontogenic pains are managed well by dental treatments. However, dentists often come upon a patient who has chronic pain in the tooth, head and neck region. It is important that non-odontogenic toothache may not be of dental origin, although, sometimes it is difficult to identify. It is reported that non-odontogenic toothache have some warning symptoms as follow: | ||||||||
| 1. Spontaneous multiple toothaches. | ||||||||
| 2. Inadequate local dental cause for the pain. | ||||||||
| 3. Stimulating, burning, non-pulsatile toothaches. | ||||||||
| 4. Constant, unremitting, non-variable toothaches. | ||||||||
| 5. Persistent, recurrent toothaches. | ||||||||
| 6. Local anesthetic blocking of the offending tooth does not eliminate the pain. | ||||||||
| 7. Failure of the toothache to respond to reasonable dental therapy [1]. | ||||||||
| Thus, dentists should have knowledge of non-odontogenic toothache and they need careful diagnosis before undertaking any treatment [2]. Pain disorder (PD) is one of possible cause of non-odontogenic toothaches which is listed under somatoform pain disorders in the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR) [3]. It is considered that PD is caused by a dysfunction of the serotoninergic and noradrenergic systems, and it is generally accepted that Tricyclic antidepressants (TCAs) is effective in a somatoform pain disorder [4]. If the toothache cannot be explained by dental origin and it matches the criteria of PD, it can be diagnosed as PD. Although an atypical odontalgia increases these days, they are less familiar to orthodontists. So, it is useful to publicizean orthodontic case with PD. In this case report, the orthodontic patient had chronic pain which was diagnosed as PD in the upper molar sections. We demonstrated that the stable occlusion was reconstructed by the orthodontic treatment, and chronic pain associated with PD was relieved by TCA administration. | ||||||||
Diagnosis and Etiology |
||||||||
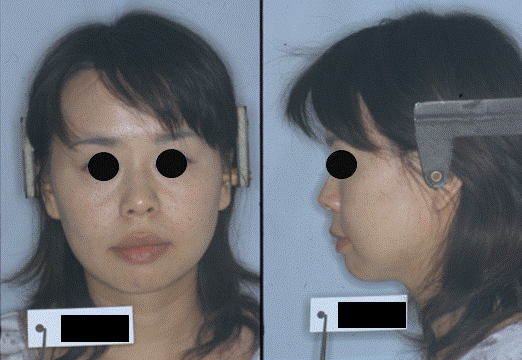
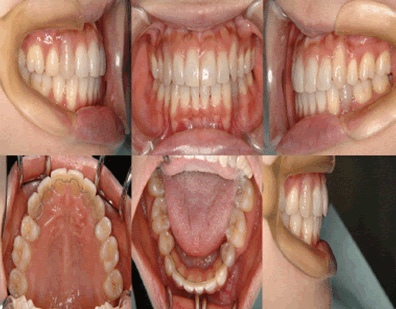
| The patient, a female aged 33 years and 6 month, had previously received an orthodontic treatment by other orthodontist with all first premolars extraction. However, she complained of impaired molar masticatory function and suffered toothache in upper molars from half way of the first orthodontic treatment. The pre-treatment facial photographs showed a straight profile (Figure 1). The intraoral photographs and dental casts revealed a 2.0 mm over jet and a 2.0 mm over bite. | ||||||||
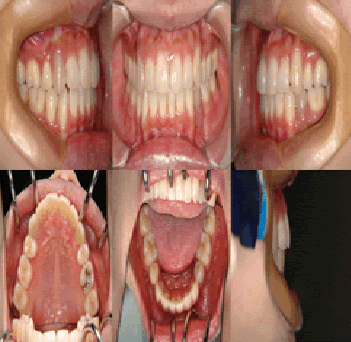
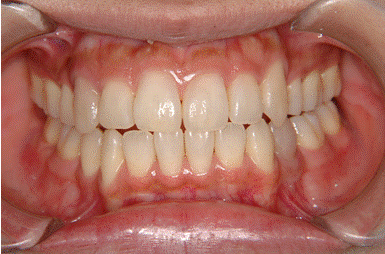
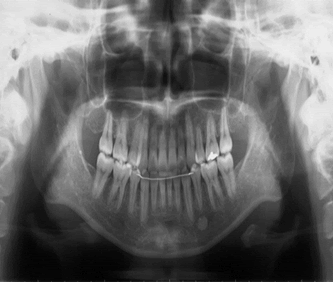
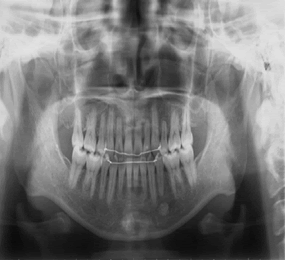
| The both right and left molar relationship was class I, and the teeth were well aligned in either arch. But the lower midline was shifted to the right direction by 2 mm in centric occlusion caused by initial occlusal contact at second molars (Figure 2), although the midline coincided in centric relation (Figure 3). A panoramic radiograph showed no abnormal observation (Figure 4). As shown in the cephalometric measurements, a skeletal Class 1 relationship (ANB angle, 4.2°) with short face type (FMA, 26.3°) was evident. Based on this information, the patient was diagnosed to have a mandibular deviation to the right side with initial occlusal contact at second molars. | ||||||||
Treatment |
||||||||
Objective |
||||||||
| Our treatment goals consisted of improving masticatory function as well as pain relief in molars. The treatment objectives included correcting the dental midline discrepancy. | ||||||||
Alternative treatment |
||||||||
| Both right and left upper second molars showed buccal crown inclination (Figure 5A). So, it was supposed that initial occlusal contact at second molars is caused by incorrect upper second molar inclination. The treatment objectives essentially consisted of control of the second molar inclination. The treatment plan was as follows. | ||||||||
| 1. Lingual crown inclination of upper second molar by lingual arch. | ||||||||
| 2. Alignment of both the upper and lower arch by multibracket system. | ||||||||
| The progress of chronic pain at upper premolars was observed carefully during orthodontic treatment. | ||||||||
Progress |
||||||||
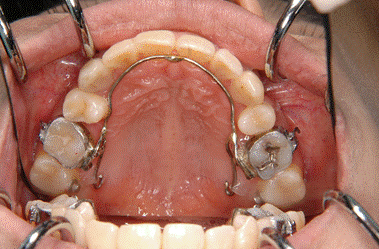
| The lingual arch was placed on the upper first molars. The lingual button was set on the second molars and we moved the second molars lingually by elastic chain (Figure 6). | ||||||||
| 0.018-inch standard edgewise brackets were also bonded on the upper and lower teeth. After two months, the upper second molar inclination was corrected (Figure 5B). However, the pain on the upper molars increased gradually. The patient wished to undergo pulpectomy but we rejected. Therefore, we refereed to a pain clinic and she was diagnosed as a PD and TCAs (imipramine hydrochloride, 10 mg × 2/day) was administered. One month later, the dose of TCAs was increased to 10 mg × 3/day. Two month after medicinal treatment, the patient stated that the pain had completely disappeared. Adverse side effects such as dry mouth and tremor did not occur. Then, the dose was decreased to daily dose of 10 mg until 1 year. | ||||||||
Results |
||||||||
| After 1 year from the beginning of the orthodontic treatment, a good intercuspal relation was achieved and the upper and lower midlines coincided (Figure 7). The patient expressed satisfaction with the occlusion. The post-treatment panoramic radiograph showed that the all of the roots were parallel, but root resorption of upper incisors was observed (Figure 8). After removal of edgewise brackets, lingual bonded retainers were set on both the upper and lower arches between the premolars. The position of the teeth continued to be stable 5 years from the beginning of the retention. The amount of medicine was decreased gradually and completely stopped after 1 year. She did not have a pain without any medication during these 5 years. | ||||||||
Discussion |
||||||||
| While it is not rare to see cases of non-odontogenic pain in a dental clinic, it is difficult for dentists to trace the cause. For such patients, it is possible to diagnose as a PD which is a common disorder with a prevalence of over 40% of patients with non-odontogenic pain [5]. PD with non-odontogenic pain may sometimes occur by specific precipitating oral events such as an improper tooth treatment [6]. In the present case, the patient suffered toothache in upper molars from the beginning of the second orthodontic treatment. At first, we could not diagnose that her molar pain was caused by PD. So, we tried to reduce the Centric relation-Centric occlusion (CR-CO) discrepancy by re-treatment of upper molar inclination. Thereafter, difficulty in mastication disappeared gradually. But the pain in the upper molar section remained in spite of no evidence of an abnormal observation. We refereed to a pain clinic and she was diagnosed as a PD. PD is regarded to occur by a dysfunction of the serotoninergic and noradrenergic systems. So, TCA administration is effective for pain relief [4]. For this patient, imipramine hydrochloride (10 mg × 2/day) was administered at the beginning, but the effect was not observed. Then, the dose was gradually increased to 10 mg × 3/day, because it was suggested that a high dose should be used if the pain does not respond to lower doses [7-10]. As a result, the pain disappeared completely after two months. However, the pain in PD can recur frequently after it disappeared [10]. So, low dose of medication (10 mg/day) was administered for 1 year and periodic checkups were carried out. | ||||||||
| In the present case, adverse side effects such as dry mouth and tremor did not occur. For this reason, the dosage of this patient was lower than that for major depression, which is consistent with previous studies that the management of chronic pain requires lower dosage of TCA than for major depression [11-15]. Orthodontic treatment can contribute to oral health and a more pleasing appearance. However, orthodontists must understand that they may sometimes create a malocclusion accidentally which may be possible to occur extra stress on the chewing muscles that can lead to headaches, TMJ syndrome and neck, shoulder and back pain. Although the association between unsuitable orthodontic treatment and outbreak of PD in this case is not clear, orthodontists should know about this disease and have to treat such patients by keeping in contact with psychiatrists. | ||||||||
Conclusion |
||||||||
| TCA administration is effective for a PD patient. Orthodontists should have the knowledge of this disease and appropriate managing to a patient is necessary. | ||||||||
Figures at a glance |
||||||||
|
||||||||
|
||||||||
References |
||||||||
|