Research Article - Journal of Physical Therapy and Sports Medicine (2018) Volume 2, Issue 2
The Long-Term Effect of a Health and Fitness Testing Program for College Freshman: Does Knowledge Empower Change?
You-jou Hung*, Austin Felts, Ashlie Francis and Kaitlyn Kupper
Department of Physical Therapy, Angelo State University, San Angelo, Texas, United States
- *Corresponding Author:
- You-jou Hung
Department of Physical Therapy, Angelo State University, San Angelo Texas
E-mail: you-jou.hung@angelo.edu
Accepted on December 15, 2018
Citation: Hung Y, Felts A, Francis A, Kupper K. The Long-Term Effect of a Health and Fitness Testing Program for College Freshman: Does Knowledge Empower Change? J Phys Ther Sports Med 2018;2(2):46-52.
Abstract
Introduction: Obesity has been consistently linked to conditions such as cardiovascular disease, stroke, type II diabetes, hypertension, cancer, and orthopaedic pathologies such as arthritis. Several studies have examined the effectiveness of health education on the wellbeing of college freshmen with mixed results. The purpose of the study was to examine the long-term effects of an 8-week interactive laboratory-based health and fitness program on vital signs, body composition, anthropometric measurements, and muscle strength/endurance for college freshmen.
Design: This was a between-groups (experimental group vs. control group) study with repeated measures.
Methods: Forty-seven freshmen (17-20 years old) were recruited to participate in the study. The participant’s body mass index (BMI), waist/hip ratio, body fat percentage, heart rate, respiratory rate, blood pressure, grip strength, and muscle endurance (with push-up and curl-up tests) were first assessed at the baseline level. Twenty-three freshmen participated in the 8-week program (experimental group) while the other 24 students did not participate in any health/fitness program (control group) during their freshman year. Twenty-five participants returned to complete the followup testing a year after the baseline testing.
Results: At the baseline testing, the experimental group exhibited a significantly larger respiration rate (p=.001) and push-ups (p=.002) but smaller diastolic blood pressure (p=031) compared to the control group. However, BMI, waist/hip ratio, and body fat percentage were similar between the 2 groups. At the follow-up testing, the experimental group had significantly increased BMI (p=.012), waist/hip ratio (p=004), and body fat percentage (p=049) compared to the baseline testing. Also, at the follow-up testing, the control group had significantly increased heart rate (p=027) and grip strength (p=045) compared to the baseline testing. Between-group follow-up testing revealed the experimental group had a significantly larger waist/hip ratio (p=.012) but a smaller respiratory rate (p=.034) compared to the control group.
Discussion: Freshmen who participated in the 8-week testing-based health program did not enhance their vital signs, body composition, anthropometric measurements, and muscle strength/endurance more than the control group at the one-year follow-up testing. This study suggests that having hands on testing experience and the knowledge of their test results did not provide enough motivation for the subjects to enhance their health markers, or the enhancement due to taking the course did not retain one-year after the intervention.
Keywords
Freshman; Health; Cardiopulmonary; Anthropometric
Introduction
“The freshman fifteen” is an ominous phrase used in American culture to describe the weight gain that seems to commonly occur during an individual’s first year of college. This change in body weight has historically been attributed to a young person’s premiere attempt at truly independent decision-making given that many college students are no longer supervised by parents/guardians. First time college students can be exposed to the temptations of fast food, poor sleep habits, and reduced physical activity, among a myriad of other potential factors. The phenomena of the “freshman fifteen” has been investigated multiple times in recent decades, and though fifteen pounds may prove to be somewhat of an exaggeration, many studies do seem to support the notion that significant weight and fitness changes frequently occur during this debut year of college life and that the early college years may be a critical time period for weight gain [1]. In a study of 186 first-year college students in the western United States, 23% of the participants gained ≥ 5% of their initial body weight, which, on average, was 9.92 lbs [2]. Another meta-analysis of thirty-two separate studies encompassing 5,549 first-year university students concluded that 60.9% of the students in the study experienced some sort of weight gain with an average gain of 7.5 lbs [3]. Further stratification through BMI analysis of 15,686 participants across twenty-two different countries revealed that 22% of university students were considered overweight or obese [4].
Community health initiative, Healthy Campus 2020, aims to increase the prevalence of health and fitness awareness within college students by 10% in the coming years [5]. Formal education opportunities must be provided within the university setting in order to achieve these goals. However, few studies have been conducted thus far for the purpose of examining and reporting the health behaviours of this highly impressionable student population in response to given health information. A four-week weight control program for female freshman did not prove to hold preventative value [6], while a six-week distance learning attempt did affect weight control efforts by its participants [7]. Shorter programs like these indicated limited influence and were unable to examine the long-term results in the targeted population. A semester long study conducted by Melnyk et al. was able to find significantly increased physical activity levels in its subjects along with a decrease in reports of anxiety and depression in a percentage of participants [8]. Another long-term program (two-year lecture course) resulted in significant weight control, though was unable to indicate whether physical activity level had a part in these results [9]. Based on the current literature, it is unclear how long a health and fitness program should be in order to achieve the maximal benefit yet require the least amount of time.
In order to effectively limit some of the most common modifiable risk factors, such as poor nutrition and sedentary lifestyle, the benefits of a health and fitness program must be retained beyond the time in which it was initially presented. This would enable students to apply the concepts to their daily life in order to make lasting changes. A study comprised of a semester-long program found that students are able to verbalize understanding of metabolism and physiology concepts that had been presented one year prior to the completion of the study [10]. These same students also gained less weight than an age-matched population who did not take part in the study [10]. However, this study was limited by retaining data on females alone while anthropometric measurements taken were confined to body weight and BMI. The majority of implemented freshman health and fitness programs that have been studied thus far maintain a heavy focus on the topics of weight management and dietary adjustments with little emphasis on musculoskeletal performance, body composition, and vital signs [6,11]. To our knowledge, no study had examined the long-term effects of a relatively short program (8-week) on fitness markers including body composition, muscular strength and endurance, vital signs, and several other anthropometric measures.
The goal of the present study is to investigate the long-term effect of a unique health/fitness program with a laboratory-focused educational experience. In addition to providing students proper knowledge on matters such as nutrition and exercise, students who enrolled in the course were taught how to implement some testing protocols and were given the opportunity to practice on their classmates. This intervention gave students the opportunity to learn how to implement and interpret measurements of health/fitness markers, created opportunity for students to educate others interested in avoiding the “freshman fifteen”, and gave students further understanding of health on a personal level. Obtaining their personal data following the initial collection period, the students who took the course were also given the chance to compare their current fitness status to normative data. This was intended to help the students create their own measurable goals for their future health and promote a long-lasting effect from taking the educational course. As mentioned earlier, little effect was found after a 4-week program and some effects were found after a 6-week program. In order to achieve a more comprehensive results without overbearing freshman’s academic course work, an 8-week course was implemented for the study. The hypothesis for this research study was that students who participated in the short 8-week laboratory-focused course were more likely to maintain or enhance their body composition and fitness status one year following the completion of their program than the cohort of students who did not participate in the program.
Materials and Methods
Subjects
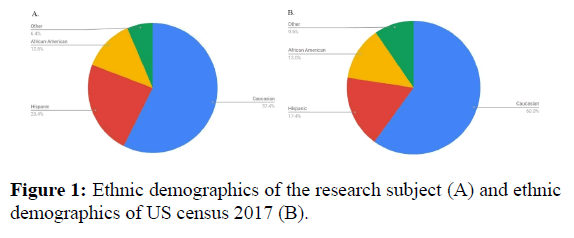
Forty-seven individuals (17-20 years old; 22 males and 25 females) were recruited from Angelo State University (ASU) to participate in the study using non-probability sampling techniques. Subjects were included if they identified as college freshmen currently enrolled at ASU and if they were cleared as safe to participate in physical activity by the Physical Activity Readiness Questionnaire (PAR-Q and YOU). All subjects were required to sign a consent form approved by the Angelo State University Institutional Review Board prior to participation in the study. The experimental group consisted of 23 individuals who voluntarily enrolled in the health and fitness program titled “Avoid the Freshman 15: The Keys to Staying Healthy in College” during the fall of 2016. Twenty-four freshmen who did not participate in the health and fitness program were recruited as the control group. Among the subjects, 57.4% of them identified “Caucasian” as their ethnicity (11 control, 16 experimental), 23.4% “Hispanic” (6 control, 5 experimental), 12.8% “African-American” (6 control, 0 experimental), and 6.4% “other” (1 control, 2 experimental) (Figure 1). When compared to ethnic demographics gathered by the United States census at the time of this study, the research sample was representative of the national population (Figure 1) [12,13].
The control group was not given any formal fitness education during their freshman year of college while the experimental group completed an 8-week freshman educational course. At the one-year follow-up data collection, each individual who initially agreed to return for the second session of fitness testing was contacted through emails, text messages, and phone calls. At least three attempts to contact each participant was made by the researchers. As the results, 25 individuals returned for the follow-up testing, including 15 participants from the control group and 10 participants from the experimental group.
Measures
Participant data was taken at baseline and at one-year follow-up sessions. The same equipment was utilized for all data collection to maximize consistency. A bioelectrical impedance analysis (BIA) machine, BIA 450 (Biodynamics Corp.; Shoreline, WA), was used to measure body fat percentage. The BIA machine involves a low-level electrical signal passing through the body from electrodes (4 electrodes) placed on the participant’s extremities. The electrical signal encounters various resistance at various tissues. Algorithms set in place use this impedance information along with input data including gender, age, height, and weight to calculate body fat percentage and other measures such as total body water and fat-free body mass [14-16].
A DETECTO physician scale (DETECTO; Webb City, MO) was used to measure participant’s height and weight. A Jamar hydraulic hand dynamometer (Jamar; Bolingbrook, Illinois) was used to obtain grip strength measurements. Concurrent validity for this model is found to be acceptable with a correlation coefficient of r ≥ 0.9994 [17]. The CARESCAPE V100 automatic blood pressure monitor w/ Critikon blood pressure cuff was utilized to obtain vitals. This device yields strong reliability and an ICC of 0.987 [18]. Other standard equipment such as tape measures (used for circumference measurements), masking tape, and a metronome app (for the purpose of standardizing sit ups) were also utilized to collect data.
The Physical Activity Readiness Questionnaire (PAR-Q and YOU) form was chosen to screen participants for physical capability to participate in the experiment. This is a questionnaire designed for people aged 15 to 69 in order to give participants and researchers guidance as to whether that individual should seek a doctor’s advisory before increasing his or her physical activity levels. If the subjects answer “yes” to any of the 7 questions in the questionnaire, they were required to be cleared by their doctor before participation.
Procedure
The intervention was an elective freshman only course titled “Avoid the Freshman 15: The Keys to Staying Healthy in College”. It was taught by a professor of the Physical Therapy Department. The instructor has a doctoral degree in Integrative Physiology and has been teaching in the same field for 9 years. Topics such as nutrients, the basics of a healthy diet, weight control, anthropometric measurements and body composition, cardiopulmonary fitness, muscular strength and endurance testing, flexibility, and resistance training were addressed during the course. In addition to the traditional lecture format, students also learned the normal value and the techniques of implementing those health/fitness tests used in the current research. Students had hands on experience of implementing those tests on their classmates in the course. The learning objectives for the course addressed current guidelines for a healthy diet, understanding health and fitness marker testing and interpreting its results, and learning how to design and follow an exercise program to increase cardiopulmonary fitness and muscular strength and endurance. The class was an 8-week course with two 50-minute meetings per week.
The following information for each participant was gathered or measured by the investigators at baseline and one-year follow up testing: height (in), weight (lbs), BMI, body fat percentage (%), heart rate (bpm), blood pressure (mmHg), respiration rate (breaths/min), waist circumference (cm), hip circumference (cm), waist/hip ratio, grip strength (lbs), push-up (successful repetitions), and sit-up (successful repetitions). Grip strength was taken as the strongest grip of three trials with the dominant arm. Waist measurements were taken at the level of the iliac crest and hip measurements were taken around the greatest circumference of the buttocks. For body fat percentage testing, participants were instructed to lay supine on a plinth and remove all metal jewellery. Sites of electrode placement were cleaned with an alcohol swab prior to attachment. Four surface electrodes were placed on the right side of the body: dorsal surface of the wrist between radial and ulnar styloid processes, dorsal surface of the hand at the space between second and third metacarpophalangeal joints, anterior surface of the ankle between medial and lateral malleoli, and anterior surface of the foot at the space between first and second metatarsophalangeal joints. From the seated position, vital signs were measured by the CARESCAPE V100 automatic blood pressure monitor.
Investigators monitored for proper technique and tracked number of push-ups and curl-ups successfully completed according to American College of Sports Medicine standards. For push-ups, the participants were instructed to place a towel on the floor under their chins. They had to lower their bodies until their chins were in contact with the towel before pushing their bodies back up to be counted as a successful push-up. The test was stopped when the subject strained forcibly or could not maintain proper technique for 2 repetitions in a row. For sit-ups, two tape lines were placed 12 cm apart in parallel. Participants were instructed to lay supine with their knee bent, touch the top tape line with their fingers, and to perform a crunch until their fingers touched the lower tape line. A metronome app was set to 40 bpm, and participants were asked to up on one beat and then go down on the next beat (20 curl-ups per minute). The test was stopped when the participant reached 75 curl-ups (maximal number for the test) or when the cadence is broken.
Data Analysis
The IBM SPSS version 21 was used for all statistical analysis. A repeated measure ANOVA was used to compare the data between the baseline and follow-up testing for the control group and the experimental group. One-way ANOVA was used to compare the data between the control group and experimental group for the baseline and one-year follow-up testing.
Results
The following parameters were measured and included in our data analysis: BMI, waist/hip ratio (WHR), body fat percentage (BF%), heart rate (HR), respiration rate (RR), systolic blood pressure (BPS), diastolic blood pressure (BPD), grip strength, push-ups endurance, and curl-up endurance. The same data was collected at the baseline testing for the experimental and control groups and at the one-year follow-up testing for the experimental and control groups.
For the baseline testing, the control group had a higher RR (F=12.19, p=.001), a higher number of push-ups completed (F=10.54, p=.002), and a lower BPD (F=4.987, p=.031) than the experimental group. The rest of the data was similar between the two groups (Table 1). For the experimental group, follow-up data had increased BMI (F=9.799, p=.012), WHR (F=14.57, p=.004), and BF% (F=5.176, p=.049) compared to baseline data. All other variables were similar between baseline and follow-up testing (Table 2). For the control group, follow-up data had increase in HR (F=6.091, p=.027) and grip strength (F=4.844, p=.045) compared to baseline data. All other variables were similar between baseline and follow-up testing (Table 3). For the one-year follow-up testing, WHR was higher in the experimental group than in the control group (F=7.416, p=.012). However, the RR was higher in the control group than in the experimental group (F=5.075, p=.034). All other variables were similar between the 2 groups (Table 4).
| C1 Mean | E1 Mean | C1 STD | E1 STD | F | p | |
|---|---|---|---|---|---|---|
| BMI | 24.06 | 26.55 | 3.88 | 8.51 | 1.681 | 0.201 |
| WHR | 0.8938 | 0.8535 | 0.3419 | 0.0987 | 3.557 | 0.66 |
| BF% | 21.60 | 21.91 | 8.41 | 8.22 | 0.016 | 0.899 |
| HR | 82.08 | 80.30 | 15.27 | 9.972 | 0.2350 | 0.631 |
| RR * | 16.04 | 13.13 | 2.866 | 2.849 | 12.19 | 0.001 |
| BPS | 119.67 | 125.43 | 9.277 | 13.32 | 2.989 | 0.091 |
| BPD * | 67.29 | 73.00 | 8.121 | 9.381 | 4.987 | 0.031 |
| Grip Strength | 96.25 | 93.13 | 22.85 | 33.40 | 0.138 | 0.712 |
| Push-Ups * | 32.38 | 20.65 | 12.88 | 10.65 | 10.54 | 0.002 |
| Sit-Ups | 46.13 | 45.19 | 19.72 | 20.98 | 0.023 | 0.879 |
Table 1: Comparison between the control (C1) and experimental (E1) groups at the baseline level (*p<.05). BMI: body mass index HR: heart rate, WHR: waist/hip ratio RR: respiration rate, BF%: body fat percentage BPS: systolic blood pressure, HR: heart rate BPD: diastolic blood pressure.
| E1 Mean | E2 Mean | E1 STD | E2 STD | F | p | |
|---|---|---|---|---|---|---|
| BMI* | 23.78 | 26.22 | 5.107 | 6.098 | 9.799 | 0.012 |
| WHR* | 0.8242 | 0.9176 | 0.0843 | 0.0256 | 14.57 | 0.004 |
| BF%* | 18.43 | 22.47 | 5.233 | 5.826 | 5.176 | 0.049 |
| HR | 77.90 | 88.30 | 8.913 | 13.79 | 3.057 | 0.114 |
| RR | 13.80 | 13.70 | 2.781 | 3.498 | 0.011 | 0.918 |
| BPS | 122.9 | 127.6 | 14.23 | 11.82 | 20.93 | 0.182 |
| BPD | 71.3 | 71.2 | 11.13 | 9.762 | 0.002 | 0.965 |
| Grip Strength | 99.67 | 96.44 | 28.26 | 26.60 | 1.116 | 0.322 |
| Push-Ups | 24.22 | 26.89 | 10.17 | 19.37 | 0.113 | 0.745 |
| Sit-Ups | 49.00 | 36.11 | 22.90 | 26.27 | 0.957 | 0.357 |
Table 2: Comparison between the baseline (E1) and follow-up (E2) results of the experimental group (* p < .05). BMI: body mass index, HR: heart rate , WHR: waist/hip ratio RR: respiration rate, BF%: body fat percentage, BPS: systolic blood pressure, HR: heart rate, BPD: diastolic blood pressure.
| C1 Mean | C2 Mean | C1 STD | C2 STD | F | p | |
|---|---|---|---|---|---|---|
| BMI | 24.30 | 27.31 | 4.392 | 10.05 | 2.048 | 0.174 |
| WHR | 0.8979 | 0.8867 | 0.3545 | 0.0294 | 1.222 | 0.288 |
| BF | 18.76 | 18.74 | 9.27 | 10.35 | 0.002 | 0.964 |
| HR* | 78.20 | 85.07 | 12.09 | 10.20 | 6.091 | 0.027 |
| RR | 15.60 | 17.00 | 2.849 | 3.645 | 2.292 | 0.152 |
| BPS | 122.8 | 123.3 | 8.986 | 8.639 | 0.028 | 0.869 |
| BPD | 68.67 | 68.33 | 9.363 | 8.112 | 0.022 | 0.883 |
| Grip Strength* | 104.7 | 112.5 | 18.24 | 26.03 | 4.844 | 0.045 |
| Push-Ups | 37.40 | 36.73 | 13.15 | 9.787 | 0.142 | 0.712 |
| Sit-Ups | 46.71 | 41.14 | 21.09 | 25.38 | 2.310 | 0.153 |
Table 3: Comparison between the baseline (C1) and follow-up (C2) results of the control group (* p < .05). BMI: body mass index, HR: heart rate, WHR: waist/hip ratio, RR: respiration rate, BF%: body fat percentage, BPS: systolic blood pressure, HR: heart rate, BPD: diastolic blood pressure.
| C2 Mean | E2 Mean | C2 STD | E2 STD | F | p | |
|---|---|---|---|---|---|---|
| BMI | 27.31 | 26.22 | 10.05 | 6.098 | 0.093 | 0.763 |
| WHR* | 0.8864 | 0.9176 | 0.295 | 0.0256 | 7.416 | 0.012 |
| BF | 21.17 | 22.47 | 14.15 | 5.83 | 0.072 | 0.791 |
| HR | 85.07 | 88.30 | 10.20 | 13.80 | 0.455 | 0.507 |
| RR* | 17.0 | 13.7 | 3.64 | 3.50 | 5.075 | 0.034 |
| BPS | 123.27 | 127.6 | 8.64 | 11.82 | 1.125 | 0.300 |
| BPD | 68.33 | 71.20 | 8.11 | 9.76 | 0.637 | 0.433 |
| Grip Strength | 112.5 | 94.8 | 26.03 | 25.61 | 2.799 | 0.108 |
| Push-Ups | 36.7 | 25.7 | 9.79 | 18.65 | 3.757 | 0.065 |
| Sit-Ups | 41.1 | 36.6 | 25.38 | 24.82 | 0.190 | 0.667 |
Table 4: Comparison between the control (C2) and experimental (E2) groups at the follow-up level (* p < .05). BMI: body mass index, HR: heart rate, WHR: waist/hip ratio, RR: respiration rate, BF%: body fat percentage, BPS: systolic blood pressure, HR: heart rate, BPD: diastolic blood pressure.
Discussion
There were no consistent differences between the control and experimental groups in body composition, cardiorespiratory, and muscular strength and endurance categories at baseline testing. Although the diastolic blood pressure values were higher in the experimental group than in the control group, both groups fell within the normal diastolic blood pressure guidelines (<80 mmHg for adults) [19]. The respiration rate found in the control group was statistically higher than the experimental group. Again, their mean remained within the normal range of 12-20 breaths per minute [20]. Subjects in the control group performed more push-ups than the subjects in the experimental group, indicating subjects in the control group had a superior local muscle endurance over their arms and chests. However, both groups of subjects reached the fair or good classifications for push-ups, and the other 2 strength/ endurance markers (grip strength and curl-up) were similar between the 2 groups [19]. Not having the 2 groups being drastically different at baseline testing could assist in examining and interpreting the effects of the 8-week course.
At one-year follow-up, cardiorespiratory health and muscular strength/endurance markers remained similar to baseline data for the experimental group. However, rejecting our hypothesis, subjects in the experimental group had significant increases in BMI, waist/hip ratio, and body fat percentage. Subjects’ BMI values increased from within the “normal” classification to the “overweight” classification [19]. Waist/hip ratio has been found to be a more significant predictor of cardiovascular disease than BMI [22]. For waist/hip ratio, it moved from moderate to high health risk factors for females and remained in low health risk factors for males [19]. The increase in body fat percentage stayed within normal healthy values for both men and women [19]. All three-body composition and anthropometric measurements had a similar response (worsened in this case), which is consistent with another report [21]. Results of the present study indicates that either those freshmen did not benefit from taking the 8-week educational course, or the course did not have the one-year long-term effect.
At one-year follow-up, cardiorespiratory health, body composition, and muscular endurance markers remained similar to baseline data for the control group. However, this group had significant increases in resting heart rate and grip strength. Although higher resting heart rates can be indicative of several contributors including decreased cardiovascular fitness, increased stress, hormone imbalance, cardiac arrhythmias, or recent activity [23], these values remained within the normal range [20]. It is unclear what caused the increment in grip strength, which remains within the “above average” classification for both males and females [19]. It is interesting to note that subjects in the control group also increased their BMI over the year and changed from “normal” to “overweight” classification. However, this statistic analysis is not significant due to outliers indicated by an increased standard deviation.
At one-year follow-up, only waist/hip ratio and respiratory rate were different between the 2 groups. Waist/hip ratio was significantly higher in the experimental group while respiratory rate was significantly higher in the control group. However, both groups were in the same classification indicating high health risk factors for females and low risk factors for males. The respiratory rates remained within the normal range in both groups despite their difference in statistical analyses.
Limitations of the Study
The small sample size is a limitation of the project, especially for the one-year follow-up phase of the study. Future researchers should consider the use of a tool to measure the subjects’ motivation level toward participating such as a Readiness to Change Questionnaire (RCQ). The model used in the RCQ lays out the stages necessary when attempting to make a lasting lifestyle change [24]. This could help explaining why the educational intervention used in this study did not facilitate long-term changes in all subjects. The result of the present study should serve as the preliminary result for a larger scale multi-center study. In addition, it would be beneficial to examine those health markers right after the 8-week intervention and/or a few months later to examine its short-term effect.
Conclusion
The goal of study was to examine the long-term effects of an 8- week interactive laboratory-based health and fitness program on vital signs, body composition, anthropometric measurements, and muscle strength/endurance for college freshmen. After a year, freshmen who participated in the 8- week testing-based program did not enhance their vital signs, body composition, anthropometric measurements, and muscle strength/endurance more than the control group. This study suggests that having hands on testing experience and the knowledge of their test results did not provide enough motivation for the subject to enhance their health markers, or the enhancement due to taking the course did not persist one year after the intervention. Further investigation is needed to examine if a testing-based program is better than a traditional lecture-based program, and if a course with a longer duration can produce a better outcome for freshmen.
Clinical Implication
In addition to practicing in a clinic, some physical therapists work at a school setting, run health awareness/promotion programs, and/or giving back to the community by sharing their knowledge in health and fitness. It is important to know that participating in a health and fitness course can have multiple benefits for college freshmen, including improving the retention rate [8]. The ideal education model has not yet been developed for managing the “freshman fifteen”. However, physical therapists should continue to explore the field of health promotion and injury prevention as we further establish our role as movement specialists.
Conflict of interest
The authors declare that there is no conflict of interests regarding the publication of this article
References
- Anderson DA, Shapiro JR, Lundgren JD. The freshman year of college as a critical period for weight gain: An initial evaluation. Eating Behaviors. 2003;4(4):363-367. doi:10.1016/s1471-0153(03)00030-8.
- Wengreen HJ, Moncur C. Change in diet, physical activity, and body weight among young-adults during the transition from high school to college. Nutrition Journal. https://nutritionj.biomedcentral.com/articles/10.1186/1475-2891-8-32. Published July 22, 2009.
- Vadeboncoeur C, Townsend N, Foster C. A meta-analysis of weight gain in first year university students: is freshman 15 a myth? BMC Obesity. 2015;2(1). doi:10.1186/s40608-015-0051-7.
- Peltzer K, Pengpid S, Samuels T, et al. Prevalence of overweight/obesity and its associated factors among university students from 22 countries. International Journal of Environmental Research and Public Health. 2014;11(7):7425-7441. doi:10.3390/ijerph110707425.
- McGinnis JM. A healthy campus- forecasting from the 1990 health objectives for the nation. Journal of American College Health. 1987;35(4):158-170. doi:10.1080/07448481.1987.9938983.
- Middleton KR, Perri MG. A randomized trial investigating the effect of a brief lifestyle intervention on freshman-year weight gain. Journal of American College Health. 2014;62(2):101-109. doi:10.1080/07448481.2013.849259.
- Gow RW, Trace SE, Mazzeo SE. Preventing weight gain in first year college students: An online intervention to prevent the “freshman fifteen.” Eating Behaviors. 2010;11(1):33-39. doi:10.1016/j.eatbeh.2009.08.005.
- Melnyk B, Kelly S, Jacobson D, Acroleo K, Shaibi G. Improving physical activity, mental health outcomes, and academic retention in college students with freshman 5 to thrive: COPE/Healthy Lifestyles. Journal of the American Association of Nurse Practitioners. 2014; 26:314-322
- Hivert M-F, Langlois M-F, Bérard P, Cuerrier J-P, Carpentier AC. Prevention of weight gain in young adults through a seminar-based intervention program. International Journal of Obesity. 2007;31(8)1262-1269. doi:10.1038/sj.ijo.0803572.
- Matvienko O, Lewis DS, Schafter E. A college nutrition science course as an intervention to prevent weight gain in female college freshman. Journal of Nutrition Education. 2001;33(2):95-101. doi:10.1016/s1499-4046(06)60172-3.
- Ha E-J, Caine-Bish N. Effect of nutrition intervention using a general nutrition course for promoting fruit and vegetable consumption among college students. Journal of Nutrition Education and Behavior. 2009;41(2):103-109. doi:10.1016/j.jneb.2008.07.001.
- US Census Bureau. Census.gov. Census.gov. https://www.census.gov/. Accessed April 30, 2018.
- Countrymeters.info. United Status of American (USA) Population. Countrymeters. http://countrymeters.info/en/United_States_of_American_(USA). Accessed April 30, 2018.
- Tanita. How BIA Works. https://www.tanita.com/en/howbiaworks/. Accessed April 30, 2018.
- Buchholz AC, Bartok C, Schoeller DA. "The validity of bioelectrical impedance models in clinical populations". Nutr Clin Pract. 2004.19 (5): 433–46. doi:10.1177/0115426504019005433
- Dehghan M, Merchant AT. "Is bioelectrical impedance accurate for use in large epidemiological studies?". Nutr J. 2008 7: 26. doi:10.1186/1475-2891-7-26
- Mathiowetz, Virgil. “Comparison of Rolyan and Jamar Dynamometers for measuring grip strength”. Occupational Therapy International. 2004. 9(3); 201-209. onlinelibrary.wiley.com/doi/pdf/10.1002/oti.165.
- Climie RE, Schultz MG, Nikolic SB, Ahuja KD, Fell JW, Sharman JE. Validity and reliability of central blood pressure estimated by upper arm oscillometric cuff pressure. American Journal of Hypertension. 2012 Apr; 25(4):414-20. Doi:10.1038/ajh.2011.238.
- Swain DP, Brawner CA. ACSM's Resource Manual for Guidelines for Exercise Testing and Prescription. Wolters Kluwer Health/Lippincott Williams and Wilkins; 2014.
- O'Sullivan SB, Schmitz TJ, Fulk GD. Physical Rehabilitation. Philadelphia: FA Davis; 2014.
- Mills TC, Gallagher D, Wang J, Heshka S. International journal of body composition research. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3183503/. Published 2007.
- Czernichow S, Kengne A, Stamatakis E, Hamer M, Batty G. Body mass index, waist circumference and waist-hip ratio: which is the better discriminator of cardiovascular disease mortality risk? Evidence from an individual-participant meta-analysis of 82 864 participants from nine cohort studies. Obesity Reviews.. September 2011;12(9):680-687. Accessed May 2, 2018.
- Purwanto B, Wigati K, Elyana Asnar S. Age and resting heart rate are discriminators to predict endurance without physical test. Folia Medica Indonesiana. 2014;50(2):110-113. Accessed May 1, 2018.
- Readiness to change questionnaire: User’s manual (revised version). NDARC- National Drug and Alcohol Research Centre. https://ndarc.med.unsw.edu.au/resource/readiness-change-questionnaire-users-manual-revised-version. Accessed May 1, 2018.