Case Report - Otolaryngology Online Journal (2016) Volume 6, Issue 3
Secondary Laryngeal Carcinoma: Case Report
- *Corresponding Author:
- Selma Hodzic-Redzic
Department of Otorhinolaryngology, Head and Neck Surgery, University Hospital Centre Zagreb, Croatia, Mali
E-mail: sellhodzic@gmail.com
Received date: April 06, 2016; Accepted date: May 18, 2016; Published date: May 25, 2016
Abstract
Background: Laryngeal metastases are rare and uncommon. Secondary involvement of the larynx with nearby tumors is often, but involvement with distant metastases is very rare. Renal cell carcinoma (RCC) has a very high metastatic potential, however, larynx is rarely involved. Case report: In this text a case of a 63-year-old is described who had laryngeal growth several years after nephrectomy due to renal carcinoma. The laryngeal biopsy was done several times until the final diagnosis was made, thanks to immunohistochemistry. Conclusion: Renal cell carcinoma can cause metastases which may occur years after the primary disease. Metastases to larynx are very rare, however they can appear, therefore they have to be included in our differential diagnosis of laryngeal, and especially secondary laryngeal cancer.
Keywords
Laryngeal metastases; Renal cell carcinoma; Immunohistochemistry
Introduction
Laryngeal metastases are rare and uncommon, and they can represent a challenge during the diagnostic process. They can be the first and sometimes the only presentation of primary disease. Secondary involvement of the larynx with nearby tumors is often, but involvement with distant metastases is rare and not considered sufficiently. Namely, distant metastases represent only 1 % of all laryngeal tumors [1].
Renal metastases to head and neck region are also very uncommon, although due to its properties the renal cell carcinoma has a very high metastatic potential. Most common metastases from the renal cell carcinoma are to lungs, bones, liver, lymph nodes and brain [2]. Head and neck metastases from renal cell carcinoma represent only 8% to 15% of the overall head and neck metastases [3].
Nose, tongue, thyroid gland and parotid glands are included in the reported cases [4]. Renal metastases to the larynx are very rare and described in a very few cases [5,6].
Case presentation
The 63-year-old male patient was referred to our Department in order to obtain the second opinion.
He was complaining of hoarseness for the last three years and denied any other symptoms.
A laryngomicroscopy and biopsy of suspicious lesion on the left ventricular fold were performed at the other Department. Pathohistological diagnosis referred to polyp. Multi-slice computerized tomography (MSCT) imaging of the neck was also performed, which showed calcified lesion of the left and front half of the right lamina of the thyroid cartilage in size of 42 × 19 × 42 mm which was imbued with punctiform calcified parts. A radiological diagnosis referred to chondrosarcoma. Due to this result another biopsy was done through the neck two weeks later. Pathohistological diagnosis showed a carcinoma of myoepithelial differentiation, clear cell variant. Due to these differences in PH diagnosis, the patient was referred to our Department.
From history: due to renal cancer the patient had his left kidney operated before seven years, clear cell variant, pT1b. Moreover, he had his appendix and hydrocele operated, and he had a septoplasty. During the examination the left ventricular fold and left piriform sinus were found protruding. During the examination of neck, there were no enlarged lymph nodes.
Blood tests were done for the most often tumor markers; AFP, CEA, CA 19-9, PSA, NSE, CYFRA 21-1. They were negative.
In radiological features, neck ultrasound revealed a mass on the left laryngeal side, size 3.9 × 2.5 × 3.6 cm with a good internal vascularisation. There were a few small reactive lymph nodes, one without hilum on the right, lower third of the neck in a size of 1.5 × 0.6 × 0.5 cm.
Plain computed tomography of thorax, abdomen and pelvis, and biphasic postcontrasted computer tomography of proximal abdomen and pelvis showed a condition after left nephrectomy and adrenalectomy, without signs of recidivate. On the right suprarenal gland there was a good vascularized mass in a size of 4.3 × 3.1 cm of inhomogeneous structure. In the level of aortal bifurcation, there was an enlarged lymph node in size of 2.8 × 1.8 cm with the same morphology and postcontrast imbibition as the tumor process of the right suprarenal gland. In conclusion: there was a primary tumor on the right suprarenal gland or there was the metastasis of primary renal disease on the right suprarenal gland and retroperitoneal lymph nodes.
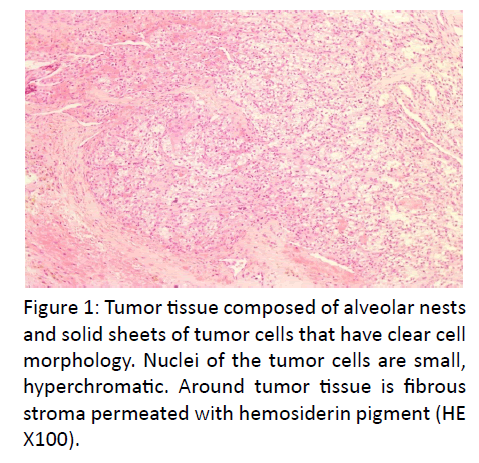
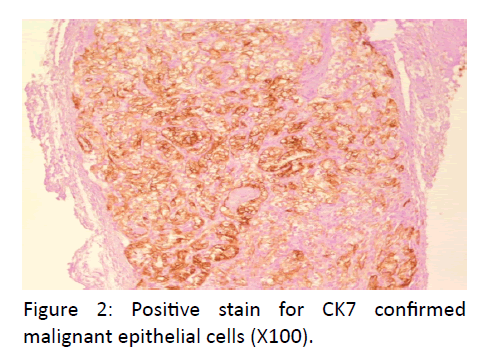
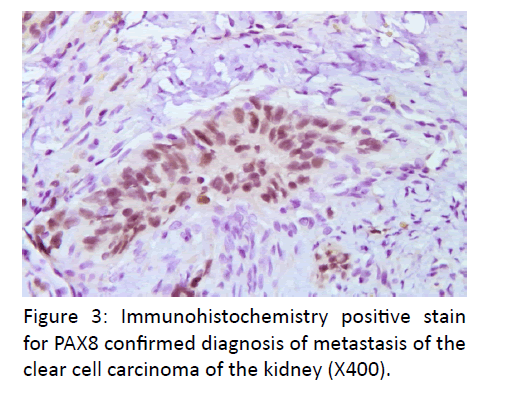
In pathologic features, the laryngomicroscopy and excisional biopsy of the left ventricular fold were performed. The excised specimen consisted of seven irregular parts of tissue measuring 0.3- 0.7 cm. The microscopic examination revealed alveolar formations and atypical, partly polymorph epithelial cells, with a light colored cytoplasm. Immunohistochemically, tissue was positive to CK AE1/AE3, PAX8 and vimentin (Figures 1-3). A revision of paraffin cubes, received from the first institution, was also done. In the second cube two parts of tissue were found which were imbued with alveolar formations, atypical partly polymorph epithelial cells with light colored cytoplasm and small nuclei. Immunohistochemical examination revealed that tissue was diffusely positive to CK, CK19, vimentin, partly positive to S-100 and negative to CD34, calponin, CK20, CD56, SMA, TTF-1, thyroglobulin and p63. Additional immunohistochemical analysis showed a positive tissue to CK7 and PAX 8 and focally positive cells in renal cell carcinoma and CD10.
Tissue was negative on parathormon, PSA, synaptophysin and CK5/6. The tumor also infiltrated the cartilage. It can be concluded that the metastasis of clear cell renal cell carcinoma is present.
Discussion
The renal cell carcinoma comprises 85% of all renal tumors. Among histological types of renal carcinoma such as chromophilic, chromophobe, oncocytic and collecting duct carcinoma, the most frequent is clear cell cancer with prevalence of 80% of all renal patients (6).
It is not easy to diagnose the renal cell carcinoma and it requires very good immunohistochemical techniques.
The renal cell carcinoma has a high potential to metastasize to lungs, bones, liver, lymph nodes, pancreas, adrenal glands, pleura, brain and skin [7]. Metastases to head and neck are very rare; however the most frequent site is the thyroid gland [8].
Laryngeal sites are also very rare; a few cases have been reported. Ferlito et al., reported only seven cases of secondary laryngeal cancers at the Department of Otolaryngology of Padua (Italy) University during 21 years, i.e. from 1966 to 1986. A review of the world literature showed only 113 previously reported cases. The most common metastases resulted from cutaneous melanoma, followed by adenocarcinoma [1].
According to Nicolais et al., only 143 cases of secondary laryngeal tumors were reported in literature at that time. The most common were metastases from cutaneous melanoma and renal cancer, whereas only sporadic cases stemming from lung and colon adenocarcinoma were documented. The authors reported one case of lung carcinoma metastasizing to larynx and two cases of adenocarcinoma metastasizing to larynx [9].
Dee et al., reported a case which represented the only case ever described in literature at that time., They presented isolated supraglottic laryngeal renal cell carcinoma metastases which occurred 7 years after radical nephrectomy had been done [5].
Rufye et al., reported two cases of head and neck metastases following nephrectomy due to renal cancer, i.e. metastases to larynx and to thyroid gland [2].
Due to its lymphatic and vascular circulation, the larynx is a terminally located organ [10], rarely affected by metastases. Supraglottic and subglottic regions are the most common sites for laryngeal metastases, due to theirs rich lymphatic and vascular supply. Our patient had a supraglottic location of tumor.
Signs and symptoms of laryngeal involvement are as usual as with the primary disease. They depend on site and size of the lesion. Our patient had a very clear laryngeal symptom: hoarseness.
Patients with metastatic involvement of the larynx usually have a poor prognosis, as involvement of the larynx might be a sign of outspread disease [10] and it is very unusual to find the laryngeal involvement as a result of metastatic disease alone. More often another metastasis can be found along the laryngeal metastasis [5].
Our patient had an invasion of contralateral suprarenal gland and two suspicious lymph nodes, one on the aortal bifurcation and another one on the lower third of the neck.
Although at the moment of getting diagnose metastases were not confirmed they probably represent metastatic disease.
References
- Ferlito A, Caruso G, Recher G (1998) Secondary laryngeal tumors. Report of seven cases with review of the literature.ArchOtolaryngol Head Neck Surg 114:635-639.
- Demir L, Erten C, Somali I, CanA, Dirican A, et al. (2012) Metastases of renal cell carcinoma to the larynx and thyroid: Two case reports on metastasis developing years after nephrectomy. Can UrolAssoc J 6: E209-E212.
- Pritchyk KM, Schiff BA, Newkirk KA, Krowiak E, Deeb ZE (2002) Metastatic renal cell carcinoma to the head and neck. Laryngoscope 112:1598-602.
- Torres-Carranza E, Garcia-Perla A, Infante-Cossio P, Belmonte-Caro R, Loizaga-IriondoJM, et al. (2006) Airway obstruction due to metastatic renal cell carcinoma to the tongue.Oral Surg Oral Med Oral Pathol Oral RadiolEndod.101:e76-e78.
- Dee SL, Eshghi M and Otto CS (2000) Laryngeal Metastasis 7 Years After Radical Nephrectomy. Archives of Pathology & Laboratory Medicine124: 1833-1834.
- Suh JH, Oak T, Ro JY (2009) Clinicopathologic features of renal cell carcinoma in young adults: a comparison study with renal cell carcinoma in older patients. Int J ClinExpPathol2:489-493.
- deKernion JB, Ramming KP, Smith RB (1978) The natural history of metastatic renal cell carcinoma: a computer analysis. J Urol120: 148-152.
- Willis RA (1931) Metastatic tumors in the thyroid gland. Am J Pathol7: 187-208.
- Nicolai P, Puxeddu R, Cappiello J, Peretti G, Battocchio S, et al. (1996) Metastatic neoplasms to the larynx: report of three cases. Laryngoscope 106:851-855.
- Quinn FB, McCabe BF (1957) Laryngeal metastases from malignant tumors in distant organs. Ann OtolRhinolLaryngol66: 139-143.