Review Article - Journal of Invasive and Non-Invasive Cardiology (2018) Volume 1, Issue 3
IVC filter retrieval
- *Corresponding Author:
- M Jyotsna
Professor, Department of Cardiology, Nizam?s Institute Of Medical Sciences (NIMS), Punjagutta, Hyderabad?TS INDIA
E-mail: mail2jyotsna@rediffmail.com
Accepted date: October 31, 2018
Citation: Jyotsna M, Lalita N. IVC filter r etrieval. J Invasive Noninvasive Cardiol. 2018;1(3):12-19.
Abstract
In this review article the major indications of Inferior Vena Caval (IVC) filter implantation and need for their retrievals are discussed. In addition to the routine methods of retrieval, the advanced methods are also described. Complications, precautions and various treatment strategies have been addressed. As this is an evolving field new advancements are expected in future.
Keywords
IVC filters, Retrieval, Pulmonary thromboembolism, Complications.
Introduction
Inferior Venal Caval (IVC) filters are of proven value for prevention of Pulmonary Thromboembolism (PTE) in subset of patients with Deep Vein Thrombosis (DVT). After an initial protection period of PTE is over and there is resolution of DVT, the IVC filters need to be removed [1]. In literature the reported retrieval rates are as low as 8.5% [2]. The development of dedicated service lines for patients with these devices has positively impacted retrieval rates. Minocha et al. study reporting an increase in retrieval rates from 29% to 60% after the establishment of a dedicated IVC filter service [3].
Indications for IVF filter implantation
Over the past 20 years there is a definite increase in the usage of IVC filters. Now it is used more frequently in DVT (prophylactic indication) than Pulmonary Thromboembolism (PTE) [4,5].
• Contraindication to anticoagulant-only therapy.
• Documented failure of anticoagulant therapy (Recurrent thromboembolic disease despite anticoagulation therapy).
• Concurrent administration of fibrinolytic therapy.
• Pregnancy labor and delivery.
• Severe trauma to the head or spinal cord.
• Thrombolysis of acute ilio-caval venous thrombosis.
• Massive pulmonary embolism–if associated with instability then filter implantation showed decrease incidence of further PTE and mortality [6]. When combined thrombolysis and within 2 days of acute DVT, implantation of filter in this fragile period is shown to be a better choice by Choi et al. [7].
• Severe trauma to or multiple fractures of the long bones.
• Major pelvic or acetabular fractures iliofemoral venous injury. Rosenthal et al. recommended bed side implantation IVC filters under ultrasound guidance in severe trauma patients for prevention of embolization even in the early stages [8].
• Prolonged immobilization with multiple injuries.
• Prophylaxis in the setting of specific surgical procedures, such as malignancy resection, facial injury repair, or gastric bypass.
• Acute withdrawal of oral anticoagulants before general surgery.
• Period of transition to oral anticoagulants due to heparin-induced thrombocytopenia.
• Pulmonary embolus in the setting of diminished cardiopulmonary reserve.
• Young patients at short-term high risk for pulmonary embolus.
• Free-floating vascular thrombus on venography.
• Chronic thromboembolic disease (undergoing pulmonary embolectomy).
• Thromboembolic disease with limited cardiopulmonary reserve (corpulmonale).
• Filter complications-insertion site thrombosis.
Types of filters
a. Permanent filters: In this article we are concentrating on retrieving of filters, so not much discussed about these filters. If any filter related complications occurs in these filter, then surgical removal is the choice of removal.
b. Temporary filters: To overcome the disadvantages of permanent filters, temporary filters were introduced. These filters have an access outside as they remain attached to a wire or catheter. They can usually be left for a week. As infection, thrombosis and migration rate are high, filters are difficult to manage and do not serve the intented purpose properly, these filters are not in use now.
c. Retrieval filters: These filters can be retrieved once the need of filter coverage is over. There is changing trends in implantation and retrievals of filters over two decades. In the past five years the retrieval rates were increased from 12.0% to 17.7%. Implantations and retrievals have been done with equal frequency by both the cardiologists and radiologists (13.0%-13.8%) [9].
Why should IVC filters be removed?
IVC retrieval helps to reduce the risk associated with having a permanent IVC filter (a foreign body within the human body). The following complications can be ameliorated by retrieval of the IVC filter.
a. Occlusion of the filter due to thrombus is the most frequent complication of the filters. Incidence varies from 6% to 30% [10]. The filter related thrombosis was more with first generation filters (especially permanent filters) [11]. The thrombosis was significantly decreased with the subsequently second generation filters OPTEASE and GUNTHER TULIP (temporary filters) [12].
b. IVC filters left in-situ for a long time have been found to develop device-related complications such as fracture, device migration, organ penetration and IVC perforation. IVC perforation is suspected when the filter components extend 3 mm beyond the IVC wall on CT scan [13].
c. We had a case of retrieval filter implantation for massive PTE with DVT on oral anticoagulation. After two months, patient was admitted with acute abdominal pain and fall of hemoglobin. CT abdomen showed large hematoma in the wall of the large bowel along with peri-filter IVC hematoma. After stabilization surgical removal of the filter was done. Similar case of duodenal involvement was reported [14].
d. Post thrombotic syndrome.
e. Patients with the anti-phospholipid syndrome-Usually permanent filters are used and patient requires lifelong anticoagulation in this group. But Baig et al. demonstrated that the safety of retrieval of IVC filters with continuation of anticoagulation [15].
When to remove the IVC filters?
a. Normally IVC filter to be removed as soon as the underlying indication for filter deployment was over, preferably within 30 days [16].
b. For the patients who cannot take anticoagulation temporarily, like immediate postoperative period, the implanted IVC filter should be removed once patient becomes eligible to take anticoagulation.
c. When IVC filter implantation was done for prophylactic reasons like immobilization, then filter to be once patient is ambulated.
d. Special attention should be paid to prophylactic filters placed in trauma patients, a situation in which the filter can typically be removed within a relatively short time interval as patients begin to ambulate or are transitioned to anticoagulation [17].
In earlier studies it was thought that prolonged dwell time after IVC filter implantation is predictor for failure of retrieval. Eventually with the development of different filter specific retrieval devices, even in the longer dwell time cases, filters could be are successfully revived [18-21]. In general, patients of retrieval IVC filters should be followed regularly and all attempts should be made to remove the filter once the crisis period of implanted is tide over [22]. An Informatics approach to facilitate tracking the patient has been proposed by Juluru K [23].
Conditions where advanced retrival techniques are required
a. Embedded hook
b. Severe tilt
c. Filter strut penetration into the caval wall
d. Prolonged dwelling time
e. Advanced age
f. Filter head position
g. Filter design
Methods of IVC filter removal- percutaneous
Route of removal
Conical shape filters like GUNTHER TULIP (WILLIAM COOK EUROPE APS) are to be removed from internal jugular approach only. Polyhedron designed filters like OPTEASE to be removed from the femoral route. Helical designed filters like Crux can be removed in both routes. Usually internal jugular approach is preferred over femoral approach for implantation of IVC filters as filter tilt and filter tip abutment is better, but Choi disproved that. In addition they showed that the femoral route takes less fluoscopic time [24].
Simple retrieval-routine technique
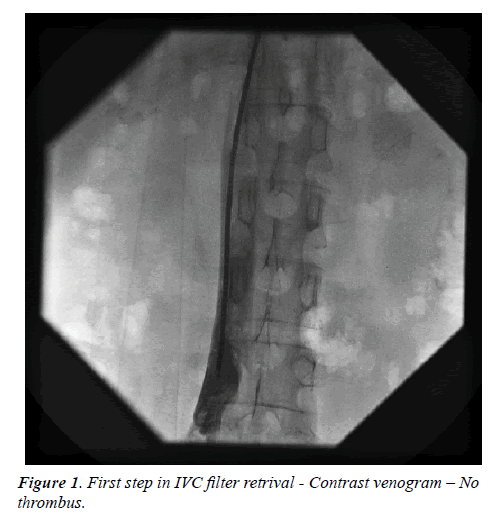
It is always advisable to have a contrast venogram to rule out the presence of thrombus in addition to previous noninvasive tests to see for IVC or filter thrombus (Figure 1). We can use usual snares or separate retrieval kits provided by the companies to remove the filters.
The essential steps in removal are:
i. Hold the hook with snare. Usually the filter collapses if dwell time is shorter. If not sheath manipulations are required for the retrieval.
ii. A sheath to facilitate coaxial collapse of the filter and disengagement from the caval wall. Pushing the sheath over the filter with simultaneous pull on the filter to be done.
iii. Once the filter partially enters into the sheath care to be taken not to release the pull on the snare. A constant pulling force on the filter is required till the whole of collapsed filter enters into the sheath.
Complex retrieval-modification in the retrieval procedure
A complex retrieval was defined as one requiring more than standard sheath and snare technique [25].
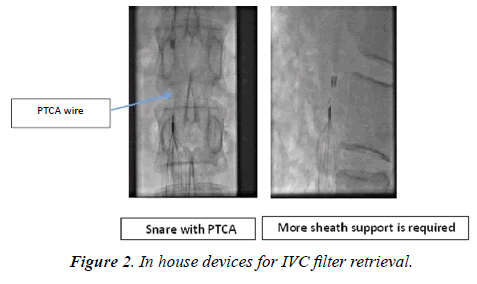
i. Loop or sling technique: Snares can be used to hold the filter hook and retrieve the filter. To hold the filter hook instead of snare, we can use the peripheral 0.35 inches wire (called as Stiff Wire-Displacement Technique) or even coronary wire also can be used. (Figure 2). In the case coronary wire loop more sheath push on the filter is required to separate the filter from the IVC wall. Pull on the hook of the filter by coronary wire may not generate sufficient force for IVC collapse, on other hand may distort or break the wire [26].
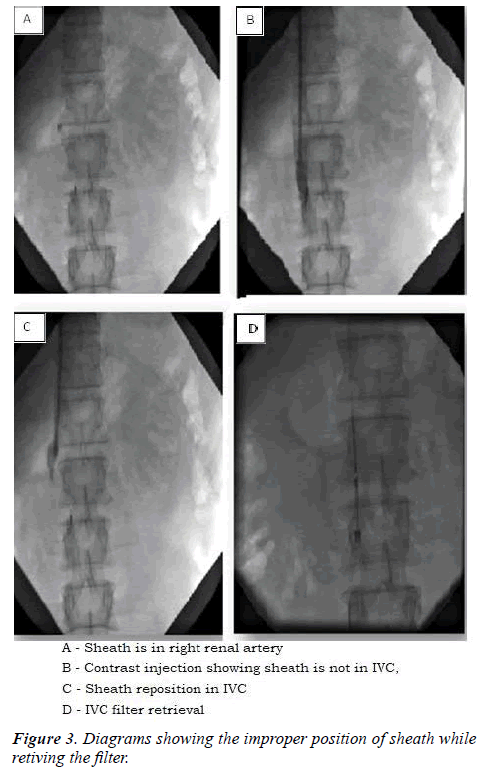
Attention: If your catheter looks as if it is in IVC, but snare dose not reach the filter tip means catheter is a branch than in proper IVC lumen. Then check with contrast in separate views and reposition the sheath (Figure 3).
ii. Balloon displacement: With snare to hold the hook, a peripheral balloon is passed between the filter and IVC wall to dislodge the filter.
iii. Dissection technique (Endomyocardial/Endobronchial forceps dissection techniques): These instruments are used to hold the hook.
iv. Hangman technique: This is a modified loop snare technique. In this a 5-F reverse curve catheter (ex: SOS Omni Catheter from AngioDynamics) and Glidewire (like Terumo wire from Radifocus are used to create a wire loop between the filter neck and IVC wall (hence the name “Hangman”), as opposed to between the filter legs. This method is more suitable when there is severe tilt or embedded hook [27].
v. Telescoping sheaths to increase longitudinal rigidity and prevent buckling as the sheath is passed over the filter.
vi. Realignment Technique: Shaped guide catheter to engage tilted hook.
vii. Dual-Access Technique: The stiff wire was inserted through the femoral or jugular approach between the filter apex and the IVC wall, and snared from the alternate approach. Wire traction is simultaneously applied in caudal and cephalic directions.
A cautionary note: The through-and-through wire should be protected by long covering sheaths or catheters to prevent entry or pelvic vein lacerations during this maneuver (i.e., ‘‘cheese-slicing’’). This approach can release the filter apex from the IVC wall. The snare inserted through the direction of retrieval, is used to remove the repositioned filter.
viii. Sandwich Technique (Parallel Wire and Dual-Sheath Technique): The recalcitrant filter is freed or untilted between the two sheaths as sandwich. In this technique, the guide wires are passed through a guiding catheter along either side of the filter nose. These wires are snared and exteriorized through the opposing sheaths. The catheter and sheath are contact into the snug against the filter, and then the upward or downward force is applied into the filter. Single wire is used for this technique but we recommend the use of parallel wires for the better encapsulate of filter. The parallel wire technique also minimizes the filter disassembly during traction. The retrieval sheath is used to remove the disengaged filter. A variation of this technique was described by Owens et al [27].
ix. Robotic assisted IVC filter retrieval: In this, a 90 cm 9F robotic sheath is advanced into the IVC with the Magellan Robotic System. The CloverSnare® 4-Loop Vascular Retriever (Cook Medical) is to be advanced through the robotic sheath to capture the hook and retrieve the filter [4]. The system’s sterability and flexibility allow for greater control in narrow vessel lumens and complex situations.
x. Excimer Laser Assisted IVC Filter Retrieval: The excimer laser is used to separate the filter from IVC wall.
Causes of failure of routine method for retrieval
The reasons and some of the suggested modifications for the routine IVC filter retrival failure are:
i. Filter tilt: curved inner catheters/sheaths like Flexor sheath with Ansel 2 modification can be used to direct the catheter tip towards the hook [1].
ii. Encasement of the filter hook in the IVC wall by a fibrin cap: above mentioned advanced retival techniques may be useful.
iii. Incorporation of filter elements into the caval wall: Hangmen technique or robotic assited or excimer laser assisted methods may be helpful.
iv. Significant extra-caval perforation of filter elements: Surgical removal is better
v. Filter fracture: Try to remove percutaneously, if failed the removal by surgical route.
vi. Significant filter thrombus: not to plan the removal at that time, better to treat the thrombus first.
vii. Caval occlusion: Is controversial where to remove or leave the filter.
Recent study done by Kleedehn et al. showed that the filter hook orientation did not correlate with retrieval complexity. Filter insertion vein did not correlate with filter tilt. Filter tilt and hook apposition to the caval wall at the time of retrieval correlated with retrieval procedure complexity [25]. Further with COLLECT AND DENALI filters, the tilt rate is further low [28]. According to Gotra et al and Geisbüsch, the shorter dwell time, lower mean tilt, caudal migration and less caval wall penetration are positive predictors of successful IVC filter retrieval [29,30].
Surgical approach
Open surgical approach requires laparotomy and venal reconstruction.
Complications
Even though IVC filter retrieval can be performed as a day care procedure safely, some complications may occur with this procedure [31]. The complication rate varies depending on the type of retrieval and varies from 0.4% in routine to 5.3% with advanced technique [18].
i. IVC dissection
ii. IVC intussusception
iii. IVC thrombus/stenosis
iv. Filter fracture with embedded strut
v. IVC injury with haemorrhage [32]. If haemorrhage occurs then prolonged balloon tamponade may prevent urgent surgery. But the chances of thrombosis and stenosis are there if prolonged balloon inflation is done, so it is advisable to follow these patients subsequently [33].
vi. Vascular injury from complicated venous access
vii. Other complications related to a filter changing position after the original placement
Controversies in retrieval
As a rule all filters to be removed once the indication is lost, but controversy is when there is chronic total occlusion of IVC filters. Acute IVC occlusion is usually symptomatic and required treatment with thrombolysis, but chronic occlusions are not [34].
Imaging modalities
1. Pre-retrieval CT: CT scan as a routine procedure is not required for retrieval. But CT abdomen is useful when dwell time of filter is >180 days or plain X-ray abdomen shows severe tilting or gross displacement or patient has suspicion of bleed due to filter penetration [35].
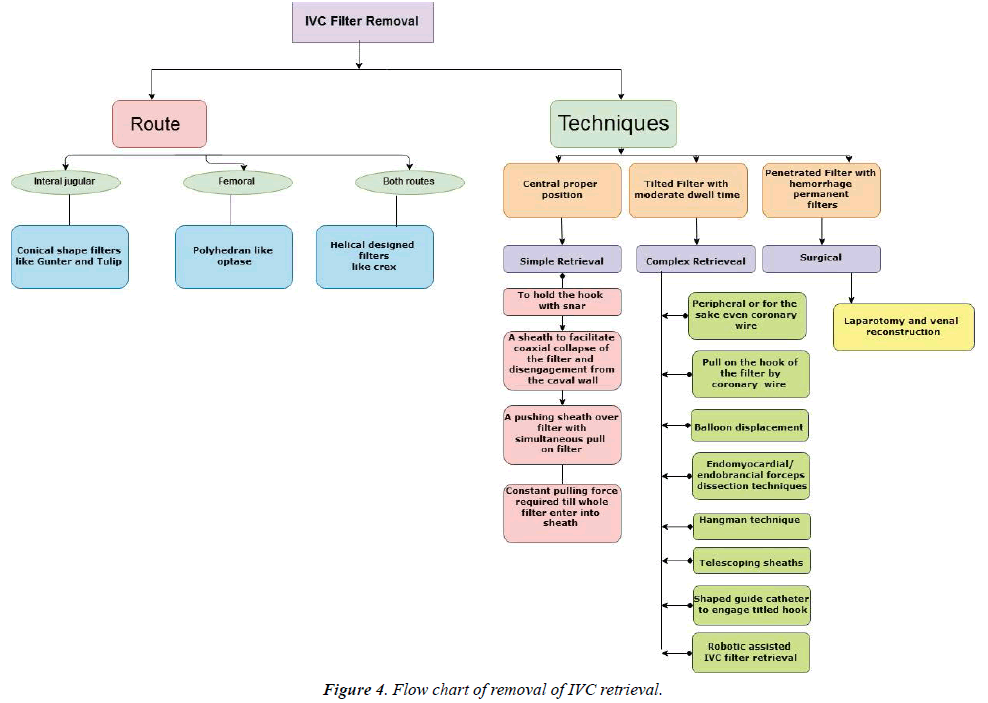
The figure given below to show the flowchart of IVC filter retrieval (Figure 4).
2. Intavascular Ultrasound (IVUS): IVUS, a specialized ultrasound technique has a major role in IVC imaging especially during endovascular procedures. It detects intraluminal thrombus, degree of stenosis and extrinsic structures of vein and it also detects even fibrous bands, webs or trabeculations in recanalized veins which are not well visualized [36].
3. Magnetic Resonance Venography (MRV): MRV is a diagnostic technique which is used to detect IVC thrombus and also post therapy follow up imaging. Contrast and non-contrast are the types of MRV, detect the lumen size of vein, overall extent of thrombus, anatomical and pathological variants. The advantages are high accuracy central veins imaging without operator dependence and lack of radiation (non-contrast) [37].
Studies
For IVC filter implantation even though multiple studies are there, the two important studies are PREPIC 1 and 2. The results of PREPIC 1 and PREPIC 2 do not provide justification for routine placement of IVC FILTER in patients with PTE [38-40].
There are few studies on IVC retrieval:
i. Excimer laser assisted IVC filter retrieval study by Robert Lewandowski is recuiting the cases. Although the technical failures are rare, these are due to excessive endo-luminal scarring at the point of IVC filter implantation. Advanced removal techniques are often employed in difficult cases. The excimer laser sheath has been successfully used at North-western for patients who had failed all other retrieval techniques [41].
ii. Failed retrieval of Inferior Vena Cava (IVC) Filters: Long-Term Outcomes–by Lyon et al. Multiinstitutional registry results showed retrieval of the Celect filter was performed safely as long as 466 days after implantation. Out 95 implantation patients filter retrieval was attempted in 58 patients successfully retrieved in 56 filters (96.6%). Unsuccessful retrieval attempts were attributed to filter tilt or excessive tissue growth with the hook embedded in the endothelium in one [42].
iii. Study of IVC filter retrieval with the Günther Tulip Vena Cava Filter: Smouse et al. filter retrieval was attempted in 275 patients and successful in 248 (90.2%). The mean filter indwell time was 58.9 days of implanted 554 patients. Study demonstrated reliable retrieval rates at 12 weeks, with successful retrievals up to 17 months after implantation [43].
iv. Prospective, multi-center, Single-arm study to assess the safety of retrieval of the recovery G2 Filter (EVEREST): 100 Patients were enrolled consecutively between December 2005 and July 2006. Retrieval was attempted in 61 patients. Fifty-eight of the 61 filters (95%) were successfully retrieved. Retrieval of the recovery G2 filter was safe and successful in most patients. Caudal migration was observed as an unexpected phenomenon. [44]
v. Retrieval rates in the United States: In this study by Ahmed et al. [45] showed that the filter placement volume declining from 61,889 in 2012 to 38,095 in 2016. Filter retrievals however, increased from 4,327 in 2012 to 8,405 in 2016. The net filter retrieval rate per annual filters placed increased from 6.9% in 2012 to 22.1% in 2016, yielding an average filter retrieval rate and compound annual growth rate of 11.6% and 18.1%, respectively.
vi. Analysis of the final DENALI trial data: Stavropoulos et al. in this study showed that in 200 patients Denali IVC filter was implanted and filter placement was technically successful in 199 patients (99.5%). Filters were clinically successful in 190 patients (95%). The rate of PE was 3%. Filter retrieval was attempted 125 times in 124 patients and was technically successful in 121 patients (97.6%) [46].
vii. The RETRIEVE trial by Smouse et al.: A total of 125 patients was implanted with the Crux filter between June 2010 and June 2011 for follow-up 180 days after filter placement and 30 days after filter retrieval. The clinical success rate was 96.0% (120 of 125), device retrieval was successful for 98.1% of patients (53 of 54) and attempted at a mean of 84.6 days after implantation [47].
viii. RexMedical: Option* Vena Cava Filter IDE Study by Johnson, Matthew et al. Placement and retrieval of the Option IVC filter were performed safely and with high rates of clinical success [48].
Conclusion
We have to plan to retrieve all the implanted IVC filterse with a few exceptions as soon the indication of implantation is over. If filter dwell time is less, it is easy to retrieve by conventional simple methods though we may require advanced techniques in few situations. Advanced techniques are associated with more complication rate hence we have to weigh risk vs benefit of retrieval in that particular patient and then to do the appropriate percutaneous or surgical procedure. As this is an evolving field there is scope for development of safer devices and techniques in future.
Acknowledgement
1. Miss. G. Indrani , Phd Student, Dept. of Cardiology, Nizam’s Institute Of Medical Sciences (NIMS) for Art Work
2. Dr. Achukatla Kumar, Research co-ordinator, Dept. Of Cardiology, Nizam’s Institute Of Medical Sciences (NIMS) for Art Work
References
- Laws JL, BS, Lewandowski RJ, et al. Retrieval of Inferior Vena Cava Filters: Technical Considerations. Semin Intervent Radiol. 2016;33(2):144–8.
- Sarosiek S, Crowther M, Sloan JM, et al. Indications, complications, and management of inferior vena cava filters: the experience in 952 patients at an academic hospital with a level I trauma center. JAMA Intern Med. 2013;173(7):513–7.
- Minocha J, Idakoji I, Riaz A, et al. Improving inferior vena cava filter retrieval rates: impact of a dedicated inferior vena cava filter clinic. J VascInterv Radiol. 2010;21(12):1847–51.
- Owji S, Lu T. Robotic-assisted inferior vena cava filter retrieval. Methodist Debakey Cardiovasc J. 2017;13(1):34–6.
- Moynihan GV, Koelzow H. Review article: Do inferior vena cava filters prevent pulmonary embolism in critically ill trauma patients and does the benefit outweigh the risk of insertion? A narrative review article. Emerg Med Australas. 2018.
- Stein PD, Matta F, Lawrence FR, et al. Inferior Vena Cava Filters in Patients with Recurrent Pulmonary Embolism. Am J Med. 2018.
- Stein PD, Dalen. Optimal Therapy for Unstable Pulmonary Embolism. Am J Med. 2018.
- Rosenthal D, Wellons ED, Levitt AB, et al. Role of prophylactic temporary inferior vena cava filters placed at the ICU bedside under intravascular ultrasound guidance in patients with multiple trauma. J Vasc Surg. 2004;40:958-64.
- Morris E, Duszak R Jr, Sista AK, et al. National Trends in Inferior Vena Cava Filter Placement and Retrieval Procedures in the Medicare Population Over Two Decades. J Am Coll Radiol. 2018;15(8):1080-6.
- Imberti D, Ageno W, Carpenedo M, et al. Retrievable vena cava filters: a review. Curr Opin Hematol. 2006;13:351–6.
- Simon M, Athanasoulis CA, Kim D, et al. Simon nitinol inferior vena cava filter: initial clinical experience. Work in progress. Radiology. 1989;172:99-103.
- Asch MR. Initial experience in humans with a new retrievable inferior vena cava filter. Radiology. 2002;225:835–44.
- Imberti D, Ageno W, Dentali F, et al. Retrievable vena cava filters: a clinical review. J Thromb Thrombolysis. 2012.
- Lee JS, Hwang JK, Park SC, et al. Surgical removal of an inferior vena cava filter with duodenal penetration. Interact Cardiovasc Thorac Surg. 2018.
- Baig S, Bert J, Gertner E, et al. Safety of retrievable inferior vena cava filters in patients with the antiphospholipid syndrome. Eur J Rheumatol. 2018;5(2):100-3.
- Rogers FB. Venous thromboembolism in trauma patients: a review. Surgery. 2001;130(1):1–12.
- Sarosiek S, Crowther M, Sloan JM, et al. Indications, complications, and management of inferior vena cava filters: the experience in 952 patients at an academic hospital with a level I trauma center. JAMA Intern Med. 2013;173:513-7.
- Al-Hakim R, Kee ST. Inferior vena cava filter retrieval: effectiveness and complications of routine and advanced techniques. J Vasc Interv Radiol. 2014;256:933–9.
- Desai KR, Lewandowski RJ, Salem R, et al. Retrieval of inferior vena cava filters with prolonged dwell time: a single-center experience in 648 retrieval procedures. JAMA Intern Med. 2015;175(9):1572–4.
- Kidane B, Madani AM, Vogt K, et al. The use of prophylactic inferior vena cava filters in trauma patients: a systematic review. Injury. 2012;43:542-7.
- Rajasekhar A, Lottenberg R, Lottenberg L, et al. Pulmonary embolism prophylaxis with inferior vena cava filters in trauma patients: a systematic review using the meta-analysis of observational studies in epidemiology (MOOSE) guidelines. J Thromb Thrombolysis. 2011;32:40-6.
- Holly BP, Funaki B, Lessne ML, et al. Inferior Vena Cava Filters: Why, Who, and for How Long? Clin Chest Med. 2018;39(3):645-50.
- Juluru K, Elnajjar P. An Informatics Approach to Facilitate Clinical Management of Patients With Retrievable Inferior Vena Cava Filters. AJR Am J Roentgenol. 2018;211(3):178-84.
- Choi SJ, Lee SY, Ryeom HK, et al. Femoral versus jugular access for Denali Vena Cava Filter placement: Analysis of fluoroscopic time, filter tilt and retrieval outcomes. Clin Imaging. 2018;52:337-42.
- Kleedehn M, Moore K, Longo K, et al. An analysis of factors associated with increased fluoroscopy time or the need for complex techniques at IVC filter retrieval. Eur Radiol. 2018:P5766-7.
- Al-Hakim R, Kee S, Olinger K, et al. Inferior vena cava filter retrieval: effectiveness and complications of routine and advanced techniques. J Vasc Interv Radiol. 2014;25:933-9.
- Al-Hakim R, McWilliams J, Derry W, et al. The Hangman technique: a modified loop snare technique for the retrieval of inferior vena cava filters with embedded hook. J Vasc Interv Radiol. 2014.
- Bae JH, Lee SY. Filter tilting and retrievability of the Celect and Denali inferior vena cava filters using propensity score-matching analysis. Eur J Radiol Open. 2018;5:153-8
- Gotra A, Doucet C, Delli Fraine P, et al. Predicting inferior vena cava (IVC) filter retrievability using positional parameters: A comparative study of various filter types. Diagn Interv Imaging. 2018;99(10):615-24
- Geisbüsch P, Benenati JF, Peña CS, et al. Retrievable inferior vena cava filters: factors that affect retrieval success. Cardiovasc Intervent Radiol. 2012;35(5):1059–65.
- Ayad MT, Gillespie DL. Long-term complications of inferior vena cava filters. J Vasc Surg Venous Lymphat Disord. 2018.
- Thuong G, Van Ha. Complications of Inferior Vena Caval Filters. EurRadiol. 2018.
- Lee JT, Goh GS, Joseph T, et al. Prolonged balloon tamponade in the initial management of inferior vena cava injury following complicated filter retrieval, without the need for surgery. J Med Imaging Radiat Oncol. 2018.
- Clements W. Inferior Vena Cava Filters in the Asymptomatic Chronically Occluded Cava: To Remove or Not Remove? Cardiovasc Intervent Radiol. 2018.
- Dinglasan L, Oh J, Schmitt J, et al. Complicated inferior vena cava filter retrievals: associated factors identified at preretrieval CT. Radiology. 2012;266:347-54.
- Neglén P, Berry M A, Raju S, et al. Endovascular surgery in the treatment of chronic primary and post-thrombotic iliac vein obstruction. Eur J Vasc Endovasc Surg. 2000;20(6):560–71.
- Zoretic JA, Collins JD. Considerations for Imaging the Inferior Vena Cava (IVC) with/without IVC Filters. Semin Intervent Radiol. 2016;33(2):109–21.
- Rajasekar A. Inferior vena cava filters: current best practices. J Thromb Thrombolysis. 2015;39:315–27.
- PREPIC Study Group. Eight-year follow-up of patients with permanent vena cava filters in the prevention of pulmonary embolism: the PREPIC (Prevention du Risqued’ Embolie Pulmonaire par Interruption Cave) randomized study. Circulation. 2005;112(3):416–22.
- Mismetti P, Ennezat PV, Quere I, et al. Prevention of pulmonary embolism recurrences by retrievable vena cava filter: results of the randomized multicenter trial PREPIC 2. International Society of Thrombosis and Hemostasis Annual Meeting, 2013:11(2).
- Northwestern University. Excimer Laser Assisted IVC Filter Retrieval. ClinicalTrials.gov. 2018.
- Lyon SM, Riojas GE. Short- and Long-term Retrievability of the Celect Vena Cava Filter: Results from a Multiinstitutional Registry. J Vasc Interv Radiol. 2009;20:1441–8.
- Smouse HB. Long-term Retrieval Success Rate Profile for the Gu¨ nther Tulip Vena Cava Filter. J Vasc Interv Radiol. 2009;20:871–7.
- Bzzinkert CA, Drooz AT. Technical success and safety of retrieval of the G2 filter in a prospective, multicenter study. J Vasc Interv Radiol. 2009;20(11):1449-53.
- Osman Ahmed. Rising Retrieval Rates of Inferior Vena Cava Filters in the United States: Insights From the 2012 to 2016 Summary Medicare Claims Data. Journal of the American College of Radiology. 2018.
- Stavropoulos SW, Chen JX. Analysis of the Final denali Trial Data: A Prospective, Multicenter Study of the Denali Inferior Vena Cava Filter. J Vasc Interv Radiol. 2016;27:1531–8.
- Smouse HB, Mendes R. The RETRIEVE Trial: Safety and Effectiveness of the Retrievable Crux Vena Cava Filter. J Vasc Interv Radiol. 2013;24:609–21.
- Johnson, Matthew S. The Safety and Effectiveness of the Retrievable Option Inferior Vena Cava Filter: A United States Prospective Multicenter Clinical Study. J Vasc Intervent Radiol. 2010;21( 8):1173 –84.