Research Article - Allied Journal of Medical Research (2020) Volume 4, Issue 2
Impact of the covid-19 pandemic on health care workersâ?? mental health: A cross-sectional study.
Ahmed Aoun1,2*, Yassmeen Abdel Rahman2,3, Nawras Maher Mostafa2,4, Islam Kassem2,5, Mai Badrah6, Shady Ahmed Moussa2,7
1Department of Pediatric Medicine, Cairo University, Cairo, Egypt
2Primary Health Care Corporation (PHCC), Qatar
3Department of Family Medicine, MOPH, Egypt
4Restorative and Endodontics in private sector, Iraq
5Department of Maxillofacial Surgeon, Alexandria University Hospital, Alexandria, Egypt
6Department of Internal Medicine, Alexandria University, Alexandria, Egypt
7Department of Pediatric Dentistry and Dental Public Health, Zagazig University, Zagazig, Egypt
- Corresponding Author:
- Ahmed Aoun
Department of Pediatric Medicine
Cairo University
Cairo, Egypt
E-mail: ahmadaon@hotmail.com
Accepted date: October 01, 2020
Citation: Aoun A, Rahman YA, Mostafa NM, Kassem I, Badrah M, et al. Impact of the covid-19 pandemic on health care workers? mental health: A cross-sectional study. Allied J Med Res 2020;4(1):57-62.
Abstract
The background: Since the onset of the current outbreak of COVID-19 infection among humans in Wuhan (China) and it’s spreading around the globe causing heavy impacts on global and mental health. Healthcare workers (HCW) and professionals now work in stressful environments both physically and mentally. Hence, addressing the mental health wellbeing of medical workers is important for better prevention and control of the pandemic.
Aim: To assess the magnitude of mental health problems namely anxiety and depression among HCW during COVID-19 pandemic in the Middle East region mainly and different countries around the globe.
Design: An online survey was designed to screen for anxiety using the “GAD-7 score” while depression was screened for using the “PHQ-2 score” among HCW involved in the care of suspected or confirmed COVID-19 cases.
Results: Analysis of participants' responses showed that 23.6% of the study sample have a moderate- to-severe grade of anxiety (n=368) while 27.4% show depression (n=426). A comparison of anxiety and depression scores among the participants shows a significant difference in GAD-7 (p=0.001) and PHQ-2 (p<0.001) scores based on their job. GAD-7 scores were higher among nurses in comparison to physicians (p=0.002). Dentists have higher PHQ-2 scores as compared to physicians (p=0.015), nurses (p<0.001) and other non-medical HCW (p<0.001) while physicians have higher PHQ-2 scores in comparison to nurses (p=0.05) and other HCW (p<0.001). We also found that moderate to severe anxiety is affected by age (p=0.024) and sex (p=0.001) being higher at females at a younger age. Being a nurse (p<0.001 ) practicing in a region outside the Middle East (p=0.001) was also associated with having moderate to severe anxiety. As for depression, it is affected by age (p<0.001) and sex (p=0.023). Being a young female is associated with having depression. Depression is also related to the job (p=0.011) and the region of residence (p=0.001) being higher in the Middle East region. HCW who spend their leisure time studying or involved in research have a higher prevalence of depression compared to those involved in other activities (p=0.005). About 71% of participants who have depression and/or moderate to severe anxiety (n=369) agree or strongly agree that those changes they experience are related to the COVID-19 pandemic.
Conclusion: COVID-19 pandemic affects the mental well-being of HCW in the Middle East region at almost a comparable extent to other HCW all over the globe. Age, sex, job, and activities at leisure time largely affect the mental well-being of HCW.
Keywords
Mental health, Healthcare workers, COVID-19, Anxiety, Depression, Middle East.
Introduction
Since the first case of novel coronavirus disease 2019 was diagnosed in December 2019, it has swept across the world and on January 30, 2020, WHO (World Health Organization) announced the occurrence of the novel coronavirus and declared a PHEIC (Public Health Emergency of International Concern). On February 11, 2020, novel coronavirus was officially named by WHO as Coronavirus Disease 2019; COVID-19. The pandemic not only brought the high mortality rate from the viral infection but also psychological unrest and mental catastrophe to the whole world. With the rapid progression of the pandemic, the disease was first reported in the Middle East region on the 29th of January 2020 in the United Arab Emirates and spread quickly to reach 8,56,650 cases in the region according to the latest WHO statement [1-3].
The COVID-19 pandemic carried a lot of uncertainty about its clinical presentation, epidemiological features, fast transmission pattern, the seriousness of public health impact, novelty, scale, implication on international public health, and underprepared health facilities to address it. All of this can have an impact on the incidence of psychological problems such as fear and anxiety among all people ranging from healthy to at-risk individuals to care-workers. A sense of fear and anxiety could arise among healthcare workers (HCW) working in hospitals, inpatient and outpatient care, large tertiary care centres, community-based hospitals, primary care settings, and all isolation units. The HCW who are exposed and in direct contact with the confirmed and suspected coronavirus cases are vulnerable to both high-risk infection and mental health problems [4,5].
As pandemic progresses, healthcare services demand increases sharply. Furthermore, many countries face inadequacy of manpower as well as resources to cope with it. Thus, HCW had to face this increased workload with the fear of being infected. Reports about mental health derangement in HCW started to raise reporting fear, emotional disturbance and sleep disorders, depressive symptoms, and anxiety. Moreover, there were not adequate services to provide counselling and psychiatric screening services for anxiety, depression, and suicidality for physicians who have been dealing with infected persons. It is also meaningful to postulate that many HCW develop PTSD, depression, anxiety, and burnout after the cessation of the pandemic. Along with the physicians, the frontline HCW (paramedics, ambulance personnel, and other healthcare workers) developing mental disorders such as depression, anxiety, and PTSD were reported. Also, the pandemic has critical reflections on dental practitioners who are in a state of anxiety and fear while working in their respective fields. Currently, many of them have either modified their services according to recommended guidelines to emergency treatment only or even suspended their work for an uncertain period [6-10].
Some experts highlighted the growing need to explore such problems and collect high-quality data on the mental health effects of the COVID-19 pandemic across the whole population and vulnerable groups. Moreover, addressing how mental health consequences for vulnerable groups can be mitigated under pandemic conditions, and the impact of repeated media consumption and health messaging around COVID-19. They also recommended discovering, evaluating, and refining interventions to address the psychological, and social aspects of the pandemic [11].
From its part, the World Health Organization declared that managing HCW mental health and psychosocial wellbeing during this time is as important as managing their physical health to face the COVID-19 pandemic. In order to have a competent and efficient healthcare system during the COVID-19 pandemic, the need to evaluate HCW mental well-being and exploring the reasons standing beyond their concerns and fears became of utmost importance [12].
Materials and Methods
An online self-reported cross-sectional survey was designed to screen for anxiety and depression among HCW working in facilities dealing with suspected or confirmed COVID-19 cases using GAD-7 and PHQ-2 questionnaires, respectively. The data of participants who agreed to enroll was kept anonymous and confidential. The survey was divided into 4 sections: (1) General idea and consent to participate, (2) Demographic data, (3) Mental health assessment, (4) Subjective opinion of participants about the relation of their mental health changes to the COVID-19 pandemic on a 5-point Likert scale. Mental health assessment was done using the GAD-7 questionnaire, anxiety was considered according to the scores obtained. Scores of 5-9, 10-14, and 15-21 were interpreted as mild, moderate, and severe levels of anxiety respectively. To assess for depression, the PHQ-2 questionnaire was used. A score of 3 points or more on the PHQ-2 questionnaire is suggestive of depression. The survey was made available online in the period between 15th March and 1st May 2020. The survey was approved by the ethics committee in Zagazig University, Egypt [13].
Statistical Analysis
We aimed for a target sample size of at least 1535 participants to ensure a confidence level of 95% and margin of error within ± 2.5% of the surveyed values. The sample size was calculated using an online sample size calculator. We collected 1594 responses to the survey including duplicate responses (n=22), and those who refused to enroll (n=15). We ended up with 1557 of valid responses. Validated data was tabulated, entered, and analysed using SPSS (version 22). Kruskal Wallis test was used for the analysis of non-parametric quantitative data and the pairwise Mann-Whitney test was used for Post-hoc analysis. A p-value ≤ 0.05 was considered to be statistically significant. Chi-square χ2 test was used to test the impact of different variables on the prevalence of anxiety and depression among the responses obtained. Multivariate logistic regression analysis was used to test the impact of different variables on the prevalence of anxiety and depression among the study group. The association between risk factors and outcomes are presented as odds ratio (OR) and 95% confidence interval (CI) after controlling for other variables like age, sex, job and region where participants work [14,15].
Results
Demographic characteristics
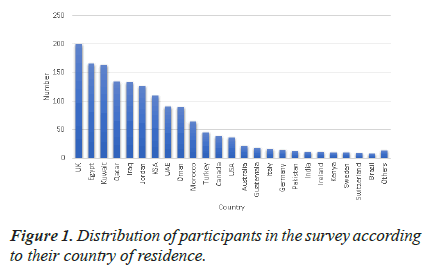
A total number of 1557 HCW, working in facilities dealing with suspected or confirmed COVID-19 patients, responded to the survey in various countries. 1125 of participants work in the Middle East (represented by Egypt, Kuwait, Qatar, Iraq, Jordan, KSA, UAE, Oman, Morocco, and Turkey) while 432 work in countries outside the Middle East region (represented by UK, USA, Canada, Australia, Italy, Germany, India, Pakistan, and others) as shown in Figure 1.
The participants vary regarding their age groups, sex, jobs, and the region where they reside and practice. Participants belong to different age groups with about 72% as males and 28% as females. More than two-thirds of participants are HCW who live in the Middle East region (n=1125). The demographic, personal, and workplace characteristics of participants are summarized in Table 1. Activities done during leisure time could be related to the mental well-being of everyone including HCW. A section in the survey was included to explore the commonest activity done during the spare time of HCW. More than half of the study samples prefer to spend their time at home with their families and friends. Some prefer reading, TV watching, or get involved in other activities.
| Characteristic | Region | Total No. (%)c |
|
|---|---|---|---|
| Countries in the Middle East No. (%)a |
Countries outside the Middle East No. (%)b |
||
| Participants | 1125 (100) | 432 (100) | 1557 (100) |
| Age groups (year) | |||
| Below 25 | 19 (1.7) | 0 (0) | 19 (1.2) |
| 25-34 | 276 (24.5) | 64 (14.8) | 340 (21.8) |
| 35-44 | 485 (43.1) | 232 (53.7) | 717 (46.1) |
| 45-54 | 255 (22.7) | 72 (16.7) | 327 (21) |
| 55 and above | 90 (8) | 64 (14.8) | 154 (9.9) |
| Sex | |||
| Men | 810 (72) | 312 (72.2) | 1122 (72.1) |
| Women | 315 (28) | 120 (27.8) | 435 (27.9) |
| Job | |||
| Dentist | 453 (40.3) | 317 (73) | 770 (49.5) |
| Physician | 437 (38.9) | 94 (21.7) | 531(34) |
| Nurse | 122 (10.9) | 10 (2.3) | 132 (8.5) |
| Pharmacist | 56 (5) | 11 (2.5) | 67 (4.3) |
| Administrative job | 55 (4.9) | 2 (0.5) | 57 (3.7) |
| Preferred activities during leisure time | |||
| Family and friends | 598 (53.2) | 244 (56.5) | 842 (54.1) |
| Reading | 218 (19.3) | 58 (13.4) | 276 (17.7) |
| TV watching and social media | 196 (17.4) | 56 (13) | 252 (16.1) |
| Study/research | 92 (8.2) | 24 (5.6) | 116 (7.5) |
| Sports activity | 21 (1.9) | 50 (11.6) | 71 (4.6) |
Note: aPercentage calculated relative to the number of participants from the ME.
bPercentage calculated relative to the number of participants out of the ME.
cPercentage calculated relative to the total number of participants.
Table 1: Demographic and workplace characteristics of HCW participating in the survey.
Mental health screening and severity of measurements
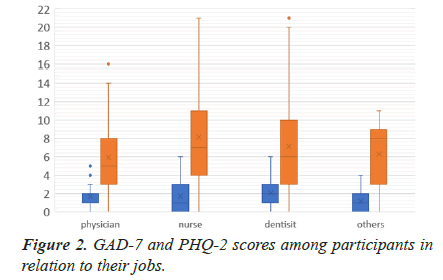
Screening for HCW mental health was focused on screening for anxiety and depression. Analysis of participants' responses to the GAD-7 section of the questionnaire revealed that 23.6% of the study sample have a moderate-to-severe grade of anxiety (n=368). This prevalence rises to around 60% if the mild grade of anxiety is included (n=949). Screening for depression was done using the PHQ-2 tool showing that 27.4% of the sample size are likely to have depression (n=426). A comparison of anxiety and depression scores among the participants shows a significant difference in GAD-7 (p=0.001) and PHQ-2 (p<0.001) scores based on their job. Post-hoc analysis showed higher GAD-7 scores among nurses in comparison to physicians (p=0.002). Dentists showed higher PHQ-2 scores compared to physicians (p=0.015), nurses (p<0.001) and other non-medical HCW (p<0.001) while physicians have higher PHQ-2 scores in comparison to nurses (p=0.05) and other HCW (p<0.001) as shown in Figure 2.
Mental health screening and related variables
Using the chi-square χ2 test to analyse the relationship between moderate to severe anxiety and other variables, we found that moderate to severe anxiety is affected by age (p=0.024) and sex (p=0.001) being higher at females at a younger age. Being a nurse (p<0.001) practicing in a region outside the Middle East (p=0.001) was also associated with having moderate to severe anxiety. We also found that it is related to leisure time activities (p=0.023) being higher in those spending their time watching TV, following social media, or those who were used to practice sports. As for depression, it is affected by age (p<0.001) and sex (p=0.023). being a young female is associated with having depression. Depression is also related to the job (p=0.011), and the region of residence (p=0.001) being higher in the Middle East region. HCW who spend their leisure time studying or involved in research have a higher prevalence of depression compared to other activities (p=0.005) as shown in Table 2.
| Variable | Participants | Anxietya | Depression | ||
|---|---|---|---|---|---|
| N | %b | p | % b | p | |
| Total | 1557 | 23.6 | 0.024 | 27.4 | <0.001 |
| Age group (year) | |||||
| Below 25 | 19 | 47.4 | 47.4 | ||
| 25-34 | 340 | 27.9 | 30.3 | ||
| 35-44 | 717 | 22.3 | 28.2 | ||
| 45-54 | 327 | 22.0 | 29.1 | ||
| 55 and above | 154 | 20.8 | 11.0 | ||
| Sex | |||||
| Men | 1122 | 21.4 | 0.001 | 25.8 | 0.023 |
| Women | 435 | 29.4 | 31.5 | ||
| Job | |||||
| Dentist | 770 | 26.9 | < 0.001 | 30.3 | 0.011 |
| Physician | 531 | 17.7 | 24.3 | ||
| Nurse | 132 | 38.6 | 30.3 | ||
| Pharmacist | 67 | 23.9 | 25.4 | ||
| Administrative job | 57 | 0 | 12.3 | ||
| Preferred activities during leisure time | |||||
| Family and friends | 598 | 22.7 | 0.023 | 29.5 | 0.005 |
| Reading | 218 | 23.9 | 21.0 | ||
| TV watching and social media | 196 | 26.2 | 23.4 | ||
| Study/research | 92 | 16.4 | 37.1 | ||
| Sports activity | 21 | 36.6 | 25.4 | ||
| Region | |||||
| Middle East | 1125 | 21.3 | 0.001 | 29.8 | 0.001 |
| Other countries | 432 | 29.6 | 21.1 | ||
Note: aModerate to severe
bPercentage calculated relative to the total number of participants in each category
Table 2: Prevalence of depression and moderate to severe anxiety among the study group and related factors.
Risk factors of anxiety and depression
Multivariate logistic regression analysis was used to analyse risk factors associated with anxiety and depression after control for other confounders. We found that working as nurse (OR 3.65; 95% CI 1.89-7.1; p<0.001) or dentist (OR 1.95; 95% CI 1.1-3.46; p=0.022) outside the Middle East region (OR 1.51; 95% CI 1.15-1.99; p=0.003) is associated with moderate to severe anxiety. Meanwhile we found that depression was associated with working as a physician (OR 1.7; 95% CI 1.03-2.82; p=0.04), nurse (OR 2.07; 95% CI 1.12-3.83; p=0.021) or dentist (OR 2.32; 95% CI 1.41-3.81; p=0.001) working in the Middle East region (OR 1.78; 95% CI 1.34-2.37; p<0.001).
Subjective opinions about mental health status in relation to COVID-19 pandemic
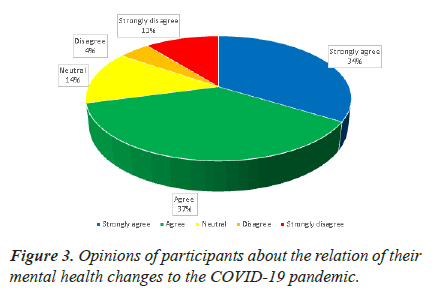
In the survey, a section was included to assess participants’ opinions about the relationship between their mental health status and its relation to the COVID-19 pandemic. Out of 521 responses that showed features suggestive of anxiety and/or depression, about 71% (n=369) agree or strongly agree that those changes they experience are related to the COVID-19 pandemic as shown in Figure 3.
Discussion
During the COVID-19 pandemic, a lot of stressors arise among all people like concerns about disease outcome, effective treatment, and available vaccination. Moreover, the implementation of unfamiliar public health measures that compromise personal freedoms, growing financial losses, and conflicting messages from authorities are among the major stressors that undoubtedly contribute to widespread emotional distress and increased risk for psychiatric illness associated with COVID-19. Besides the above-mentioned reasons, other reasons specific for HCW do exist. Among those reasons are the frequent exposure and risk of infection, fear of contagion and spreading the virus to families or friends, the novel nature of the disease, shortages of protective equipment for HCW, fatigue, extended workloads, separation from families, and others [16-18].
In our survey, we demonstrated the impact of such stressors on HCW mental wellbeing. The prevalence of moderate to severe anxiety among HCW involved was 23.6% (n=368). The prevalence of anxiety among the study group rises up to 60% (n=949) if the mild grade of anxiety is included. The prevalence of depression shows comparable results of 27.4% among the study sample (n=426). This goes with what Pappa found in their systematic review of 13 studies, that pooled prevalence of Anxiety was 23.2% and depression rate of 22.8% [19]. Also, in Canada, a survey about the psychosocial effects of Severe Acute Respiratory Syndrome on hospital staff, 29% of the respondents scored above the threshold point on the 12-item General Health Questionnaire, indicating probable emotional distress. This illustrates the need for timely mental health care for HCW during the COVID-19 outbreak [19,20].
As for associated factors to mental health outcomes, we found that depression and moderate-to-severe anxiety are affected by age, sex, and job being higher in females at a younger age who work as nurses. This goes with what Lai found in their study where they reported that females working as nurses reported more severe degrees of all measurements of mental health symptoms than other health care workers [21]. Our findings also go with what Pappa found in their systematic review revealing that there are gender and occupational differences with female HCW and nurses exhibiting higher rates of affective symptoms compared to male and other medical staff respectively [19].
As for preferred activities during leisure time, we found that moderate to severe anxiety is higher in those spending their time watching TV or following social media while depression outcome was higher in HCW who spend their leisure time studying or doing extra work compared to other activities. It seems contradictory for us that HCW who prefer to spend their leisure time practicing sport showed a higher prevalence of moderate-to-severe anxiety. However, this could be related to the unusual implementation of public health measures that include restricting group activities and even total lockdown in some countries. This may prevent them from practicing sport, hence increasing their stress.
The prevalence of depression and moderate-to-severe anxiety among the study group working in the Middle East region is almost comparable to those working in other regions despite the relatively lower prevalence of COVID-19 cases in relation to other regions e.g. Europe and the USA at time of the study; March and April. We found that more prevalence of depression and less prevalence of moderate to severe anxiety among the study group who work in the Middle East region. This could be explained by the past and ongoing experience of HCW in the Middle East region with the related Coronavirus (MERS-CoV), which is actually endemic in some countries, and its fatal outcomes as demonstrated in recent research. Furthermore, some countries in the region may have a lower capacity of healthcare systems with limited resources and a lack of timely logistics. Also, the lack of public awareness about measures of safety and protection, and other social factors could be the reason why we got such responses in the Middle East region.
We can find that the results from all the available research so far on this topic and the data from our study that it is clear that the HCW in the COVID-19 pandemic are under enormous physical and mental stress. As per WHO recommendations, managing HCW mental health and psychosocial well-being is as important as managing their physical health and safety [12]. In China, Yong Liu reported that psychotherapists have been invited to join medical teams to evaluate and deal with potential stress and depression for the safety of the HCW [22]. Other reports from China showed that building organized psychological intervention plans targeting HCW were developed. Those plans involved building online courses to guide medical staff to deal with common psychological problems; a psychological assistance hotline, and psychological interventions, which provided various group activities to release stress [22-26].
Therefore, we recommend to look further and analyse the fears and needs of HCW to alleviate their stresses. Moreover, Psychiatrists should be involved and closely work and monitor the mental wellbeing of frontline HCW. Furthermore, designated “wellness champions” can provide a point of contact for staff concerns, raising their awareness about the stressors and risks facing them in their fight against COVID-19 pandemic, advocate for their welfare and distribute messages of support and gratitude. We urge healthcare officials and healthcare policy-makers to take what is mentioned in this work and others into consideration during strategic planning and policy-making. Last but not the least, when the crisis is over, adequate time is to be made to reflect on and learn from those stressful situations.
Conclusion
As we demonstrated in our study, the mental wellbeing of HCW is affected due to the current COVID-19 pandemic in different countries around the world in general, and also in the Middle East region. We think that part of the successful and sustainable measures to contain this global pandemic is to take care of the mental and physical wellbeing of frontline HCW particularly those at risk e.g. young age, females, and nurses as demonstrated before. This should be taken into consideration during healthcare planning to tackle the pandemic in the Middle East region.
References
- Chunfeng X. A novel approach of consultation on 2019 novel coronavirus (COVID-19)-Related psychological and mental problems: structured letter therapy. Psychiatry Investig. 2020;17:175-76.
- WHO. Novel Coronavirus(2019-nCoV) Situation Report-9. 2020.
- WHO. Coronavirus disease (COVID-19) Situation Report-151.2020.
- Mak IWC, Chu CM, Pan PC, et al. Long-term psychiatric morbidities among SARS survivors. Gen Hosp Psychiatry. 2009;31:318–26.
- Rana W, Mukhtar S, Mukhtar S. Mental health of medical workers in Pakistan during the pandemic COVID-19 outbreak. 2020;51:102080.
- Kar S K, Yasir-Arafat SM, Kabir R, et al. Coping with Mental Health Challenges During COVID-19. Coronavirus Disease 2019 (COVID-19). 2020;199-213.
- WHO. Regional Office for Europe. Mental health and COVID-19. 2020.
- Li W, Yang Y, Zi-Han L, et al. Progression of mental health services during the COVID-19 outbreak in China. Int J Biol Sci. 2020;16:1732-38.
- Ahmed MA, Jouhar R, Ahmed N, et al. Fear and Practice Modifications among Dentists to Combat Novel Coronavirus Disease (COVID-19) Outbreak. Int J Environ Res. 2020;17:2821.
- Moussa S, Mostafa N, Arafa A, et al. The Novel Coronavirus (2019-nCoV) Outbreak as a New Challenge in the Dental Field. J Dent Oral DisordTher. 2020;8:6.
- Holmes E A, O'Connor RC, Perry VH, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020;7:547-60.
- WHO. Mental health and psychosocial considerations during the COVID-19 outbreak. 2020.
- Spitzer RL, Kroenke K, Williams JBW, et al. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166:1092-97.
- Whooley M A, Avins A L, Miranda J, et al. Case-finding instruments for depression. Two questions are as good as many. J Gen Intern Med. 1997;12:439-45.
- Select Statistical Services. Population Proportion – Sample Size. 2020..
- Pfefferbaum B, North C S. Mental Health and the Covid-19 Pandemic. NEJM. 2020.10.1056.
- kumar R, Philip R. COVID-19 and mental health: A review of the existing literature. Asian J Psychiatr. 2020;52:102066.
- Yu-Tao X, Yang Y, Li W, et al. Timely mental health care for the 2019 novel coronavirus outbreak is urgently needed. Lancet Psychiatry. 2020;7:228-29.
- Pappa S, Ntella V, Giannakas T, et al. Prevalence of depression, anxiety, and insomnia among healthcare workers during the COVID-19 pandemic: A systematic review and meta-analysis. Brain Behav Immun. 2020;5:26.
- Chung JPY, Wai-Song Y. Staff mental health self-assessment during the COVID-19 outbreak. East Asi Arch Psy. 2020;30:34.
- Lai J, Simeng M, Ying W, et al. Factors Associated With Mental Health Outcomes Among Health Care Workers Exposed to Coronavirus Disease. JAMA Netw Open. 2019;3:203976.
- WHO. Coronavirus disease (COVID-2019) situation reports. World Helath Organization. 2020.
- Temsah MH, Al-Sohime F, Alamro N, et al. The psychological impact of COVID-19 pandemic on health care workers in a MERS-CoV endemic country. J Infect Public Health. 2020;13:877-882.
- Liu Y, Li J, Feng Y. Critical care response to a hospital outbreak of the 2019-nCoV infection in Shenzhen, China. Crit Care. 2020;24:56.
- Chen Q, Liang M, Li Y, et al. Mental health care for medical staff in China during the COVID-19 outbreak. Lancet Psychiatry. 2020;7:15-16.
- Kang L, Li Y, Shaohua H, et al. The Mental Health of Medical Workers in Wuhan, China Dealing With the 2019 Novel Coronavirus. Lancet Psychiatry. 2020;7:14.