Research Article - Otolaryngology Online Journal (2017) Volume 7, Issue 4
A Study on Deep Neck Space Infections
Nirmal Kumar J, Sankaranaarayanan G* and Greeshma
Department of ENT, Upgraded Institute of Otorhinolaryngology, Madras Medical College and Rajiv Gandhi Government General Hospital, Chennai, Tamilnadu, India
- Corresponding Author:
- Sankaranarayanan G
Department of ENT
Upgraded Institute of Otorhino Laryngology
Madras Medical College and Rajiv Gandhi Government General Hospital
Chennai, Tamilnadu, India
Tel: 09444468277
E-mail: sankar.ent@gmail.com
Received Date: October 23, 2017; Accepted Date: November 01, 2017; Published Date: November 07, 2017
Abstract
Aim: To do a cross-sectional analysis of cases of neck space infections as to the symptomatology, causes, investigations, complications and treatment so that our understanding on this improves thereby improving our treatment outcome.
Materials and Methods: A review of 17 treated cases of Deep Neck Space Infection (DNSI) in our department from September 2015 to September 2016 was carried out. A standard proforma was used for data collection and the following variables were recorded including age and gender, symptoms, etiology, co-morbidities (diabetes, HIV), site of infection, bacteriology, growth culture and antibiotic sensitivity, surgical intervention and duration of treatment.
Results: The most common source for Deep Neck Space infection is dental in origin. The most common symptoms were neck swelling and pain, followed by odynophagia. Submandibular space and parapharyngeal space involvement were more common in odontogenic DNSI. Bacteriology reveals Klebsiella species as the most common organism. Mean duration of hospital stay was 14 days with minimum of 8 days and maximum of 33 days.
Conclusions: DNSI is a potentially life threatening condition. The deep location and complexity of this region makes the diagnosis and treatment of these infections challenging. Its presentation maybe masked and bacterial cultures may not be conclusive but it still needs early diagnosis and prompt management whether conservative or surgical. The gold standard imaging modality for the diagnosis of DNSI is computed Tomography. With the advent of better radiological imaging modalities and better effectiveness of antibiotics, we are now able to treat these infections successfully and reduce the rate of complications.
Keywords
Deep neck space infections, Submandibular, Parapharyngeal space, Neck abscess
Introduction
Fascia is dense connective tissue and neck is draped with layers of fascia with potential spaces between them referred as neck spaces. Deep Neck Space Infections (DNSI) implies infection in the potential spaces either with abscess formation or with cellulites. In the past the incidence of DNSI were more common, the advent of broad spectrum antibiotics has significantly brought down the incidence of these infections [1]. Antibiotics usage at adequate strength and duration has brought a significant decrease in the occurrence and progression of the disease. These infections are severe and inadequate treatment may lead to progression and can be associated with high morbidity and mortality.
The primary sources of DNSI are the dentition and tonsils, other sources may be from salivary glands, malignancies and foreign bodies. Commonly DNSI follows infections like dental caries, tonsillitis, and trauma to head and neck or in intravenous drug abusers. Odontogenic infection is one of the most common causes especially in developing countries [2]. Before the antibiotic era, tonsil and peritonsillar region were the source of infection in almost 70% cases [3] of DNSI, but now dental origin is considered the most common cause [4]. The odontogenic infections like periapical lesions with pulp necrosis and bacterial invasion into periapical tissues and periodontal lesions associated with periodontal pockets cause DNSI.
As to bacteriology of DNSI the common organisms implicated are Streptococci, Staphylococcus aureus, Peptostreptococcus species and anaerobes [5,6]. Mostly they are polymicrobial. Clinical manifestations depend upon the spaces involved and include fever, pain, fatigue, swelling, malaise, odynophagia, dysphagia, dyspnea, otalgia, trismus [7].
In immunocompromised patients with diabetes mellitus, patients on steroid therapy, chemotherapy or those with HIV infection [8] the course of the disease may be more rapidly progressive with sometimes a fatal outcome. DNSI even with extensive and adequate antibiotic therapy still remains serious and can cause significant morbidity, 10-20% of cases go for life threatening complications [9,10].
Dreaded complication includes Descending necrotizing mediastinitis resulting from retropharyngeal extension of infection into the posterior mediastinum. Septic shock is associated with 40-50% mortality rate [11,12]. cardiac tamponade resulting from Pleural and pericardial effusion may also be seen. Suppurative thrombophlebitis of internal jugular vein associated with pulmonary embolism, thrombosis of cavernous sinus and erosion of carotid artery have been also been reported [13].
Prompt surgical drainage of the abscess followed by antibiotics is the main line of treatment. In cases of cellulitis non-surgical management with appropriate antibiotics is given [14]. Surgical treatment of odontogenic infections with the aim of removing the source is important [15]. Cure without any complications should be our aim and entails early diagnosis and appropriate aggressive treatment.
Materials and Methods
17 treated cases of DNSI in ENT Department of Rajiv Gandhi Government General Hospital and Madras Medical College, Chennai from September 2015-September 2016 was analysed for this study. We collected details including age/sex, habits like alcohol and smoking, presence of other co morbid or predisposing diseases and clinical presentation. We did culture and sensitivity and other routine lab examination. We analysed the possible etiology, effective treatment methods, presence of complications and duration of hospital stay.
For establishing which of the neck spaces were involved the following were taken into account a) Clinical findings, b) Radiological evidences from CT and c) surgical treatment. All deep neck space infection patients treated as in patients were included. Infections related to tumours were excluded. We didn’t include those who had incomplete data. A total of 17 cases of DNSI with above criteria qualified for the studies.
Results
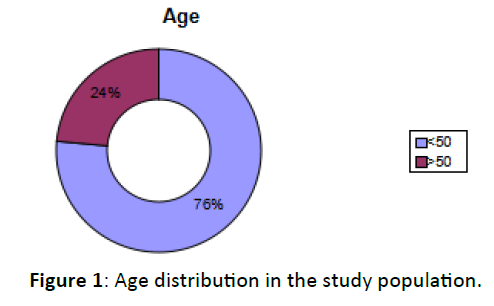
There were 17 patients in our study, 12 of which were males and 5 females; with a minimum age of 25 years and a maximum of 65 years. The mean age of our patients was 42.8 years. Seven patients (41%) had diabetes either known previously or newly diagnosed at the time of admission. One patient was diagnosed to be HIV positive (5%). One patient was a known case of rheumatic heart disease on anticoagulants. One patient was earlier treated by radiotherapy for carcinoma tongue (5%). 9 male patients were smokers (Figure 1).
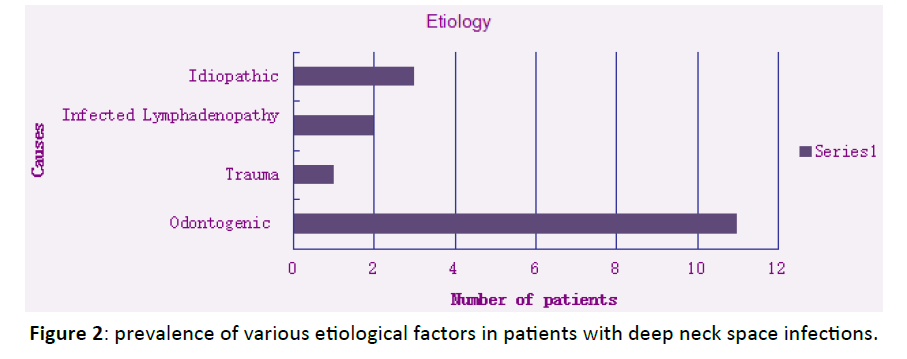
The most common cause of DNSI in our series was of dental infections in origin. 11 patients (64.7%) had dental infections, 1 patient (5.8%) had trauma as the etiological factor, 1 patient (5.8%) had infected lymphadenopathy and in 4 patients (23.5%) exact causes were unknown (Figure 2).
Most patients presented with swelling in the neck and pain (88%). Two patients with buccal space infection presented with cheek swelling. 14 patients (82.3%) had odynophagia. 8 patients (47%) had preceding history of dental pain. 3 other patients with odontogenic cause had no dental pain. 2 patients (11.7%) had airway compromise.
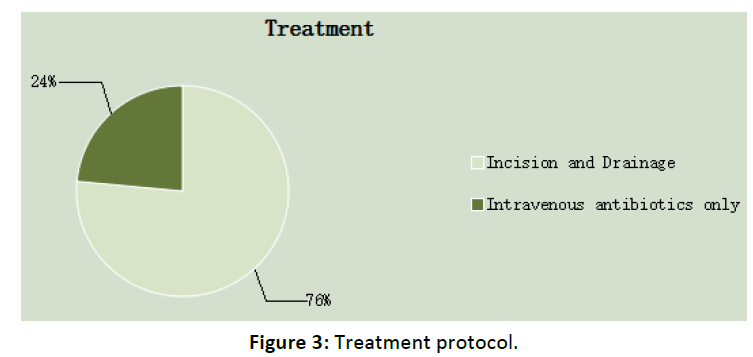
In our series, 11 patients (64.7%) had submandibular space involvement. 2 patients had buccal space involvement. In 3 patients extension to masseteric space was present. In 2 cases parapharyngeal extension was noted on imaging. In 3 patients parotid space involvement was present. 13 patients were treated with surgical intervention in the form of incision and drainage. 4 patients were managed conservatively with intravenous antibiotics only (Figure 3).
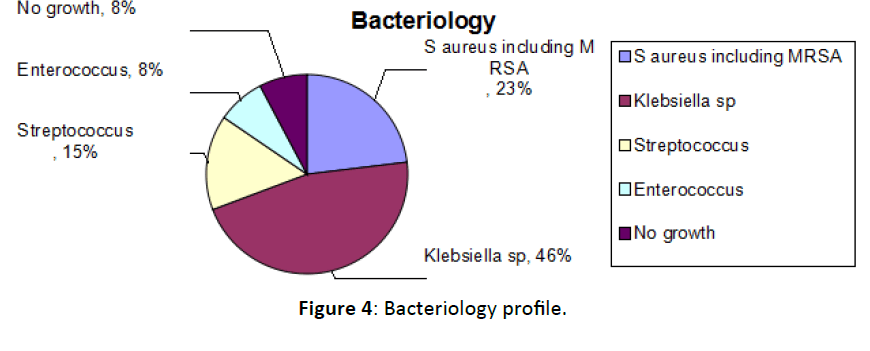
The pus was sent for culture and sensitivity. Cultures revealed Klebsiella species (pneumoniae and oxytoca) in 6 patients (46.1%), Staphylococcus aureus including one case methicillin resistant variety in 3 cases (23%), Streptococcus species in 2 patients (15.3%), Enterococcus in 1 patient (7.6%). In one patient bacterial cultures did not reveal any growth (Figure 4).
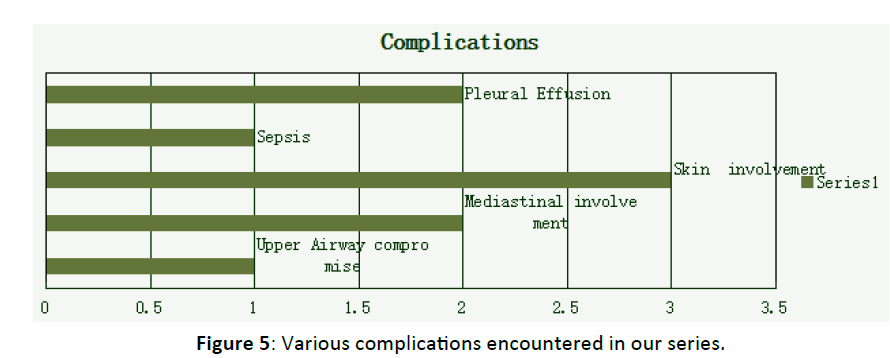
In our series four patients went in for complications, 2 patients developed Mediastinitis. These 2 patients also developed a pleural effusion that necessitated intercostal drainage tube insertion. 1 patient went in for severe respiratory distress warranting a tracheostomy. 3 patients had skin involvement. One patient went into sepsis. The cause of death was due to septic shock. The origin of infection was unknown. The patient was not a diabetic or immunisely compromised. For our series the mortality rate is 5.8% (n=1) (Figure 5).
Discussion
Review of literature shows many similarities and few differences as to results of our study compared with other similar studies. The mean age that was affected most by infection in our series was 42.8 years and is similar to other studies where the mean age varied from 36 to 57 years [4,16]. In our series we had 12 male patients and 5 female patients concurring with the fact that the disease was twice more common in males as many authors have reported [17,18].
In personal history elicited Smoking, tobacco chewing and alcohol consumption were the most commonly associated habits that was brought out. Diabetes was the most commonly found systemic disease in our study (41%) compared to other studies in literature which has reported a 16-20% of incidence [18]. Associated hypertension should be given importance for this factor may indicate heart or lung disease and may be a determining factor as to outcome. HIV has been found in 1% of cases in the literature [4], compared to incidence of 1 patient in our study.
The various clinical presentations in our study were swelling of the neck, fever, malaise, trismus, odynophagia, poor general health condition and these may or may not be associated with a primary condition. This is similar to that found in other similar studies [19]. Poorer prognosis was noted in the presence of toxemia, tachycardia, respiratory failure and signs of tissue necrosis. The primary source for DNSI varies from sites from head and neck like teeth, salivary glands, lymphoid tissue and tonsil. Odontogenic infections were the most common cause in our series 65%, followed by the disease in oropharynx compared with other studies which report dental infections 31-80% and tonsillar origin in 1.5-3.4% [20,21]. Tonsillar infection is more common in children [22,23]. Other causes in our study were trauma to upper jaw in one case, suppurative lymphadenopathy in 2 cases and idiopathic in the rest. Diabetes was a coexisting disease in many cases.
Tung et al. [6] and Gerd [24] have reported in their study on DNSI that the most common site of infection was the parapharyngeal space and was seen in 71 (38.4%) and 138 (59%) cases respectively. In our patients submandibular space involvement was the most common and was seen in 11, parapharyngeal space involvement was demonstrated in 2 patients. Parhiscar et al.4 and Staflors et al. [25] in their study concurred with Tung et al. study reporting that parapharyngeal space involvement was more common but in a report by Meher et al. [26] submandibular space was the most common site encountered which was similar to our report.
Jurgen et al. [24] reported Streptococci, S aureus and Anaerobes as the most common organisms. Bakir et al. [9] showed that 20 (58.8%) of culture positive patients had polymicrobila growth and the most common organisms were Peptostreptococcus (21.3%), S epidermidis (19.7%). However in our study there were 12 patients with positive cultures, Klebsiella species in 6 patients (46%) followed by Staphylococcus in 2 patients (15.3%), Streptococcus in 2 patients (15.3%) and MRSA in 1 patient (7.6%) and Enterococcus in 1 patient (7.6%). The use of antibiotics before taking sample for culture may be the reason for negative culture in other cases.
Since the 1970s the CT scan evidently has improved the diagnosis of DNSI. Contrast CT is still the appropriate imaging to be done since it helps in correct diagnosis indicating the extent of disease, differentiating cellulitis from abscess [25] and helps evaluate any complication. CT scan also helps to decide whether surgical intervention is indicated [27]. Patients with radiological evidence of cellulites responded well to medical treatment, whereas those with abscess have greater complications and usually require surgical management who otherwise may go for complications due to aggressive nature of this condition. Ultrasonogram of neck should be done and helps in early detection of abscess fromation [27]. In our study CT scan was done in 13 patients (76.4%) and ultrasonogram in 4 patients (23.5%).
Surgical drainage of the purulent abscess via an external approach [2,28] is the management accepted and practiced universally. In contrast to this, Mayor et al. recommended broad spectrum intravenous antibiotics along with high doses of corticosteroids. Bakir et al. [9] in their study on 173 cases of DNSI showed that 78 patients (40.5%) were treated successfully with only intravenous antibiotics and the remaining 95 patients (59.5%) were treated surgically. The various studies concur that patients with cellulitis or minimal abscess intravenous antibiotics alone is sufficient. CT Evidence of abscess requires open surgical drainage. In our study surgical intervention was carried out in 13 patients (76.4%) of DNSI, rest of the 4 patients were treated conservatively with intravenous antibiotics [29].
Airway management gains importance when patients present with trismus or signs of upper airway obstruction particularly in Ludwig’s angina, in which there is edema of the floor of the oral cavity. Airway compromise is usually due to laryngeal edema and pushing of the tongue upwards and backwards. Parhiscar et al. [4] in his study of 210 patients with neck abscesses reported a need for tracheostomy in 44% of cases. In our study tracheostomy was done in 1 patient (5.8%). We agree that adequate management of airway with intubation or tracheostomy wherever necessary is a priority in the initial approach to DNSI [30,31]. When there is acute respiratory difficulty attempting intubation can sometimes worsen an already damaged airway and in such case Tracheostomy should be done.
Our complication rate was 23.5%. Neck space infections may rapidly progress to necrotising fascitis, descending mediastinitis, and septic shock in few cases. In such cases the mortality rate is 40- 50%. Mortality rate in our series was 5.8%. 1 patient died due to infection followed by septic shock.
Conclusion
Deep Neck Space Infections are still a challenging disease for clinicians and should be treated aggressively and promptly. The current study enabled us to conclude that:
• Smoking and alcohol consumption were the most common social habits –steps like counselling and medications to help stop them should be initiated.
• Old age, diabetes and immunocompromised status associated withDNSI may lead to complications and hence should be evaluated at the earliest and given aggressive treatment.
• The submandibular and peritonsillar space involvement were more common.
• Klebsiella species, Staphylococcus aureus and Streptococci are the main microorganisms involved in this condition.
• CT is the investigation of choice for diagnosis of DNSI.
• All patients should be started with intravenous antibiotic therapy preferably culture directed.
• DNSI associated with septic shock and mediastinitis have high morbidity and mortality rates and needs prompt and appropriate intervention.
Early suspicion, prompt diagnosis and aggressive treatment are essential.
References
- Wang LF, Kuo WR, Tsai SM, Huang KJ (2003) Characterizations of life threatening deep cervical space infections: A review of one hundred ninety six cases. American J Otolaryngol 24: 111-117.
- Wong TY (1999) A nationwide survey of deaths from oral and maxillofacial infections: The Taiwanese experience. J Oral Maxillofac Surg 57: 1297-1299.
- Weed H, Forest L (1998) Deep neck infection. J Otolaryngol Head Neck Surg 3: 2515-2524.
- Parhiscar A, Harel G (2001) Deep neck abscess: A retrospective review of 210 cases. Ann Otol Rhinol Laryngol 110: 1051-1054.
- Ungkanont K, Yellon RF, Weissman JL, Casselbrant ML, Gonzalez VH, et al. (1995) Head and neck space infections in infant and children. Otolaryngol Head Neck Surg 112: 375-382.
- Huang TT, Liu TC, Chen PR, Tseng FY, Yeh TH, et al. (2004) Deep neck infection: Analysis of 185 cases. J Otolaryngol Head Neck Surg 26: 854-860.
- Hasegawa J, Hidaka H, Tateda M (2011) An analysis of clinical risk factors of deep neck infection. Auris Nasus Larynx 38: 101-107.
- Vieira F, Allen SM, Stocks RSM, Thompson JW (2008) Deep neck infections. Otolaryngol Clin N Am 12: 459-483.
- Bakir S, Tanriverdi MH, Gun R (2012) Deep neck space infections: A retrospective review of 173 cases. American J Otolaryngol 33: 56-63.
- Boscolo RP, Stellin M, Muzzi E (2012) Deep neck space infections: A study of 365 cases highlighting recommendations for management and treatment. Eur Arch Otorhinolaryngol 269: 1241-1249.
- Chen MK, Wen YS, Chang CC, Huang MT, Hsiao HC (1998) Predisposing factors of life-threatening deep neck infection: Logistic regression analysis of 214 cases. J Otolaryngol 27: 141-144.
- Chen MK, Wen YS, Chang CC, Lee HS, Huang MT, et al. (2000) Deep neck infections in diabetic patients. Am J Otolaryngol 21: 169-173.
- Blomquist Ik, Bayer AS (1988) Life-threatening deep fascial space infections of the head and neck. Infect Dis Clin North Am 2: 237-264.
- Mayor GP, Millán JMS, Martínez VA (2001) Is conservative treatment of deep neck space infections appropriate? Head And Neck 23: 126-133.
- Morton H, Richard G (2002) Oral and Maxillofacial Infections. In: Topacian RG, Goldberg MH, Hupp JR, editor. New York, St. Louis WB Saunders, United States pp: 158-186.
- Bahu SJ, Shibuya TY, Meleca RJ, Mathog RH, Yoo GH, et al. (2001) Craniocervical necrotizing fasciitis: An 11-year experience. Otolaryngol Head Neck Surg 125: 245-252.
- Sakaguchi M, Sato S, Ishiyama T, Katsuno S, Taguchi K (1997) Characterization and management of deep neck infections. Int J Oral Max Surg 26: 131-134.
- Sethi DS, Stanley RE (1994) Deep neck abscesses--changing trends. J Laryngol Otol 108: 138-143.
- Levitt GW (1971) The surgical treatment of deep neck infections. Laryngoscope 81: 403-411.
- Estrera AS, Landay MJ, Grisham JM, Sinn DP, Platt MR (1983) Descending necrotizing mediastinitis. Surg Gynecol Obstet 157: 545-552.
- Furst IM, Ersil P, Caminiti M (2001) A rare complication of tooth abscess-ludwigs angina and mediastinitis. J Can Dent Assoc 67: 324-327.
- Choi SS, Vezina LG, Grundfast KM (1997) Relative incidence and alternative approaches for surgical drainage of different types of deep neck abscesses in children. Arch Otolaryngol Head Neck Surg 123: 1271-1275.
- Cmejrek RC, Coticchia JM, Arnold JE (2002) Presentation, diagnosis, and management of deep-neck abscesses in infants. Arch Otolaryngol Head Neck Surg 128: 1361-1364.
- Ridder GJ, Technau-Ihling K, Sander A, Boedeker CC (2005) Spectrum and management of deep neck space infections: an 8-year experience of 234 cases. Otolaryngol Head Neck Surg 133: 709-714.
- Stalfors J, Adielsson A, Ebenfelt A, Nethander G, Westin T (2004) Deep neck space infections remain a surgical challenge. A study of 72 patients. Acta Oto?Laryngologica 124: 1191-1196.
- Meher R, Jain A, Sabharwal A, Gupta B, Singh I (2005) Deep neck abscess: A prospective study of 54 cases. J Laryngol and Otology 119: 299-302.
- Smith II JL, Hsu JM, Chang J (2006) Predicting deep neck space abscess using computed tomography. Am J Otolaryngol 27: 244-247.
- Bottin R, Marioni G, Rinaldi R, Boninsegna M, Salvadori L, et al. (2003) Deep neck infection: A present day complication. A retrospective review of 83 cases. Eur Arch Otorhinolaryngol 260: 576-579.
- Eftekharian A, Roozbahany NA, Vaezeafshar R, Narimani N (2009) Deep neck infections: A retrospective review of 112 cases. Eur Arch Otorhinolaryngol 266: 273-277.
- Heindel DJ (1987) Deep neck abscesses in adults: management of a difficult airway. Anesth Analg 66: 774-776.
- Shockley WW (1999) Ludwig Angina: A review of current airway management. Arch Otolaryngol Head Neck Surg 125: 600.