Research Article - Journal of Clinical Pathology and Laboratory Medicine (2017) Journal of Clinical Pathology and Laboratory Medicine (Special Issue 2-2017)
Biochemical evaluation of creatinine and urea in patients with renal failure undergoing hemodialysis.
- *Corresponding Author:
- Nisha Rajendran
Vivek Institute of Laboratory Medicine, Chennai, India
Tel: 9159122733
E-mail: vivekinstitute2011@gmail.com
Accepted date: July 14, 2017
Citation: Nisha R, Srinivasa Kannan SR, Thanga Mariappan K, et al. Biochemical evaluation of creatinine and urea in patients with renal failure undergoing hemodialysis. J Clin Path Lab Med. 2017;1(2):1-5.
Abstract
Renal failure is one among the slowly progressive diseases of kidney function characterized generally by low glomerular filtration (GRF). The replacement therapy of renal failure by hemodialysis involves the removal of excessive toxic fluids and toxic metabolic end products from the body. In this background, the present attempt was focused to evaluate and correlate the value of various biochemical markers in blood serum from the pre and post dialysis renal failure patients. Among many biochemical parameters in blood, serum creatinine and urea are emerging as a source of more sensitive markers for the detection of the renal failure. Thus, the analytical part of this study included the samples from 50 patients with renal failure before and after hemodialysis for the prevalence of creatinine and urea level. A colorimetrical method using fully automated analyser (Cobas C311) for the analysis of creatinine and urea concentrations in human serum was adopted. The mean values of these two components in post dialysis group were lower when compared to the pre dialysis group, and the concentration of urea was found to be lower than that of creatinine. The incidence of serum creatinine and serum urea was significantly high before hemodialysis and reduced significantly after hemodialysis. The study revealed a significant statistical relationship between the availability of creatinine and urea in blood serum of the pre and post dialysis samples from renal failure patients.
Keywords
Renal failure, Hemodialysis, Blood serum, Creatinine and urea profiles.
Introduction
Diseases of the kidneys are amongst the most important causes of death and disability in many countries throughout the world [1,2]. Renal failure is a systemic disease and usually turns into a route cause for several kidney and urinary tract diseases. Renal failure induces a slow and progressive decline of kidney function enhanced by various factors including infections, auto immune diseases, diabetes and other endocrine disorders, cancer, and toxic chemicals [3]. It is usually a result of complications arising from other serious medical conditions. Unlike acute renal failure, which happens quickly and suddenly, chronic renal failure occurs gradually - over a period of weeks, months, or years - as the kidneys slowly stop working, leading to an end-stage renal disease (ESRD) [4,5]. High blood pressure is one of the leading causes of kidney failure. It may also damage the blood vessels in the kidney affecting the secretion of waste products. Waste may secrete extra cellular fluids and further raise the blood pressure eventually leading to ESRD [6]. Anemia parallels the degree of renal impairment and it is a most important cause is the failure of renal erythropoietin secretion.
Hemodialysis is one of the renal replacement therapy [7]. The technique plays a vital role in the process for the extracorporeal removal of waste products such as creatinine, urea and free water from the blood, when the kidneys are impaired. The principle behind hemodialysis is the diffusion of solutes through a semi permeable membrane. Hemodialysis is usually performed with uremic patients for two to three times a week and the required times for dialysis vary from two to four hours [8]. The difference in the time of dialysis depends on various factors, including kidney function, amount of waste in body, level of salts and body weight. Dialysis improves many symptoms of kidney failure, but some problems including hypertension, anemia and itch often require additional drug treatments as well [9].
The progression of kidney damage is marked by the rise in two important chemical substances in the blood - creatinine and urea whose evaluation in serum helps to assess Glomerular Filtration Rate (GFR) followed by renal function. However, neither creatinine nor urea is directly toxic and they are only a measure of kidney function [10]. Creatinine is produced from muscles and is excreted through the kidneys along with other waste products. Creatinine concentration in serum is maintained by the balance between its generation and excretion by the kidneys. It has been estimated that 2% of the body’s creatine is converted into creatinine every day, resulting in the daily generation of creatinine at a fairly constant rate (male: 20 to 25 mg/kg/day; female 15 to 20 mg/kg/day) [11]. Males have higher serum creatinine levels than females because males have greater muscle mass. The quantity of creatinine in serum depends on their generation, glomerular filtration and tubular secretion of serum creatinine. Calculations based on serum creatinine and the age groups of the patient are used to estimate more precisely the degree of kidney function [12,13]. These calculated values are called the estimated glomerular filtration rate or eGFR. Sometimes a 24 hour urine collection and blood test together are used to measure the efficiency of kidney’s removal (or clearance) of creatinine from the body. These results are known as creatinine clearance [14]. Other factors affecting creatinine concentrations include age, sex, ethnicity, body habits and diet. However, neither creatinine nor urea are directly toxic and are just substances used to measure kidney function [15]. Urea is an organic compound and plays a vital role in the metabolism of nitrogen-containing compounds. It is a waste product from dietary protein and is also filtered into urine by the kidneys [16,17]. Urea nitrogen is a normal waste nitrogen product found in blood that comes from the breakdown of protein from foods. Healthy kidneys remove urea nitrogen from blood, but the level of urea in blood rises with kidney failure occurs [4]. An attempt has been made to evaluate the increase of creatinine and urea in patient’s serum of various age groups with renal failure during pre and post hemodialysis.
Materials and Methods
Patients and samples collection
Random samples from patients with renal failure were collected from Dr. Jayasekaran Center for Kidney Diseases, Nagercoil, Tamilnadu during December 2016 and January 2017. The analytical study enrolled 50 patients with signs and symptoms of renal failure as identified by expert nephrologists and epidemiologists who critically reviewed and confirmed the persistence of kidney injury in all patients, using a standardized process. Among them, the percentage of males and females were 70% and 30% were their age ranging between 20 and 80 years. The study was commenced after receiving the approval of Institutional Review Board against submission of an individual written consent letter from all patients. The blood samples (5 ml) were collected from these patients before and after hemodialysis and was then centrifuged individually at 3000 rpm for 10 minutes to separate serum and stored at -20°C for biochemical evaluation.
Estimation of serum creatinine
The creatinine levels in the samples were assessed by Jaffe Kinetic assay (22, 2002). Creatinine in the serum sample reacted with picric acid in an alkaline solution (i.e., alkaline picrate) of the reagent and developed an orange colored complex. The quantity of creatinine in the test samples was calculated against the intensity of the color developed during the fixed time. The intensity of the color was measured using a fully automated Cobas C311 analyzer for detection of serum creatinine.
Estimation of serum urea
Urea levels in the samples were hydrolyzed by urease to form ammonium and carbonate [18]. Next, L-glutamate was produced by the reactions between ammonium and 2-oxoglutarate in the presence of glutamate dehydrogenase and the coenzyme NADH. During this reaction, 2 moles of NADH were oxidized to NAD+ for each mole of urea hydrolyzed. The rate of decrease in the NADH concentration was directly proportional to the urea concentration in the serum sample which was photometrically determined using fully automated Cobas C311 analyzer.
Statistical analysis
The results obtained were subjected to statistical analysis to check whether there was any correlation between creatinine and urea level in the samples on pre and post hemodialysis with SPSS version 22.0 statistical software.
Result and Discussion
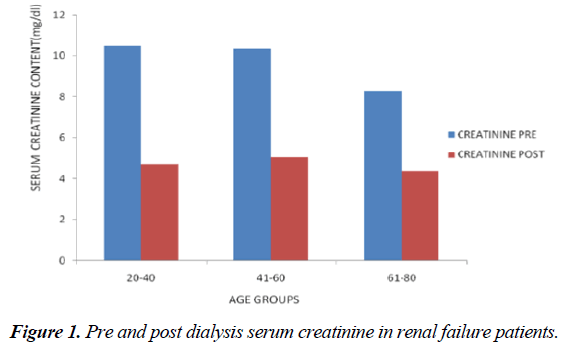
Renal failure is a gradual, progressive and irreversible loss of normal functioning of kidneys. Increased levels of urea and creatinine excretion in blood by impaired kidneys made very complication in patients with renal failure before hemodialysis. A total of 50 patients who were diagnosed in kidney care centre for renal failure based on their clinical history, clinical examinations and renal function tests were randomly evaluated. Bio markers levels of such as serum creatinine and serum urea before and after the hemodialysis session were screened. The details of the patients are cited in Table 1 and creatinine levels in Figure 1.
| Sampling Period | Sex wise | Age Group in Years(%) | |||||
|---|---|---|---|---|---|---|---|
| Total | Distribution(%) | ||||||
| From | To | Number ofCases(n) | Male (n) |
Female (n) |
21-40Years(n) | 41-60Years(n) | 61-80Years(n) |
| 50 | 35 | 15 | 8 | 30 | 12 | ||
| 2016 | 2017 | (100%) | (70%) | (30%) | (16%) | (60%) | (24%) |
Note: n- Number of patients
Table 1: Clinical characteristics of 112 colorectal cancer patients.
The mean SD values of serum creatinine before and after hemodialysis were compared separately in 3 age groups of subjects (21-40 yrs, 41-60 yrs and 61-80 yrs) and are summarized in Table 2. Creatinine is a resultant of muscle metabolism and its elevated level in blood indicates kidney disease. The mean values of serine creatinine level were observed to be less in the age group between 61 and 80 years. A statistically significant difference in the mean values of creatinine was observed in all the three age groups when compared with the reference range. The difference between age groups may be attributed to the fact that smaller body size has lower metabolic demands and shorter individuals require less renal function.
| Serum Creatinine levels (mg/dl) | |||||||
|---|---|---|---|---|---|---|---|
| S.No. | Age Group (Years) | No. of Cases (n) | Pre hemodialysis | Post hemodialysis | |||
| Mean±SD | T-Value | P-value | Mean±SD | T-Test | |||
| 1 | 21-40 | 8 | 10.48 ± 3.06 | 9.681 | 0 | 4.67 ± 1.97 | 6.67 |
| 2 | 41-60 | 30 | 10.35 ± 3.23 | 17.54 | 0 | 5.03 ± 1.76 | 15.61 |
| 3 | 61-80 | 12 | 8.27 ± 2.60 | 10.99 | 0 | 4.36 ± 1.54 | 9.75 |
(Data are presented as Mean ± Standard Deviation; n-Number of subjects; P ≤ 0.05: significant)
Table 2: Incidence of serum creatinine in renal failure patient?s during pre and post hemodialysis.
Serum creatinine level was significantly higher than normal range (up to 1.4 mg/dl) in renal failure patients undergoing dialysis (p<0.005). All selected patients had the mean serum creatinine level as 10.48 ± 3.06 mg/dl in the age between 21 and 40 years, 10.35 ± 3.23 mg/dl in the age group between 41 and 60 years and 8.27 ± 2.60 mg/dl in the age group between 61 and 80 before dialysis. Increasing level of creatinine in serum may cause itching and damage to nerve endings. Hemodialysis portrayed an effective impact on serum creatinine level which reduced to near normal value. Analytical results showed that all hemodialysed patients (50 nos.) had serum creatinine below 5.03 ± 1.76 after dialysis. Paired t-test exhibited a significant to the mean SD values of serum creatinine in all 3 age groups (t-test = 6.67, 15.61 and 9.75 in the age groups of 21 to 40 yrs, 41 to 60 yrs and 61 to 80 yrs respectively) and the p-values were 0.0001 (Table 2). Creatinine clearance is the best method for the examination of kidney functioning. The results of the present study strongly indicate that different factors like age, sex and physical status of person affect serum creatinine level as suggested by Noor ul et al. [5]. The results of this present study were near to the findings of Attika and Lubna [19] in renal failure patients undergoing hemodialysis which enacted positive effect on a significant fall in serum creatinine level. Reduction in the level of creatinine during hemodialysis is also used as a surrogate marker of the inadequacy of dialysis. It was also noted that people between the age group of 41 and 60 years were more prone to kidney failure which might be due to conditions like hypertension, diabetes or some other age related changes.
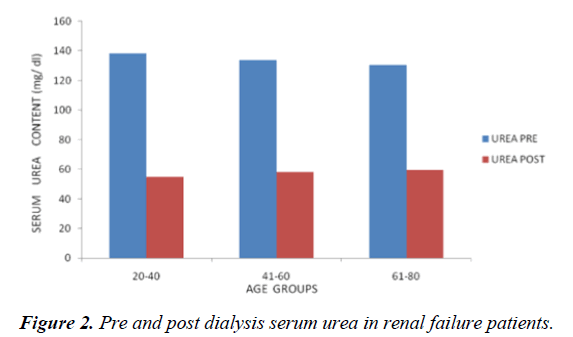
There was significant difference in the levels of serum urea observed before and after hemodialysis with respect to different age groups (Table 3). Generally urea accumulation in blood serum of kidney failure patients arises from the degradation of food and tissues such as muscle. The high level of urea in blood leads the body very sick unless remove it from the blood streams by kidneys [20]. mass differences [21] ( Table 3) represented the increased mean values of serum urea in all 3 age groups before hemodialysis (138.44 ± 49.31 mg/dl in 21 to 40 years; 133.98 ± 36.41 mg/dl in 41 to 60 years; 130.58 ± 23.11mg/dl in 61-80 years) when compared to the mean values of after hemolysis (54.87 ± 28.82 mg/dl in the age between 21 and 40 years; 58.26 ± 19.95 mg/dl in the age between 41 and 60 years; 58.26 ± 19.95 mg/dl in the age between 41 and 60 years (Figure 2).
| Serum Urea levels (mg/dl) | ||||||||
|---|---|---|---|---|---|---|---|---|
| S.No. | Age Group (Years) |
No. of Cases (n) |
Pre hemodialysis | Post hemodialysis | ||||
| Mean ± SD | T value Test |
P value |
Mean ± SD | T-Test | P value |
|||
| 1. | 21-40 | 8 | 138.44 ± 49.31 | 8.42 | 0.000 | 54.87 ± 28.82 | 5.38 | 0.001 |
| 2. | 41-60 | 30 | 133.98 ± 36.41 | 20.15 | 0.000 | 58.26 ± 19.95 | 15.99 | 0.000 |
| 3. | 61-80 | 12 | 130.58 ± 23.11 | 19.57 | 0.000 | 59.66 ± 16.05 | 12.87 | 0.000 |
(Data are presented as Mean± Standard Deviation; n-Number of subjects; P = 0.05: significant)
Table 3: Incidence of serum urea in renal failure patient?s during pre and post hemodialysis.
During hemodialysis, excess urea from the patient’s blood is slightly removed in order to prevent accumulation. The occurrence of balanced amount of consumed proteins is also an important step to avoid excessive production of urea [22]. The hemodialytic process carried out in the studied patients was perceived to be efficient, because significantly reduced levels of creatinine and urea were recorded ensuingly. According to Draczevski and Teixeira [1], the assessed pre- and posthemodialysis urea levels, obtained reflected a significant reduction in serum levels, indicating hemodialysis as an efficient technique. Removal of waste during dialysis also depends upon proper timings of dialysis, patient awareness, and appropriate dialyzer and dietary habits of patients [23]. Urea and creatinine levels are important biomarkers as they play a pivotal role in diagnosis and follow-up of kidney failure. Urea, one of the by-products of protein metabolism, accumulates in the blood of patients with kidney failure and causes uremia [24-26].
Conclusion
A firm relationship was observed between serum creatinine and serum urea levels among renal failure patients presenting information on renal function among varied age groups. Both serum creatinine and serum urea are widely accepted biomarkers to assess the renal functions. Hemodialysis forms an effective process as an efficient and indispensable process for the filtration of undesired metabolites such as creatinine and urea in patients at considerable range thereby increasing their life expectancy. However, today’s health research warrants newer techniques for an early detection and quicker prevention of complications that arise from kidney.
Acknowledgments
The author would like to thank Mrs. Shabeena Merrin, Principal, Ms. G. Pradeepha, Dr. Ranjit Jeyasekaran, Trustees, Dr. Jeyasekharan Medical Trust, Nagercoil, Prof. Dr. C. Ratnam Nadar, Ph.D., Prof. Dr. S. Ramesh, and other technicians of our institution for their help in the manuscript preparation, data collection and sampling.
References
- Draczevski L, Teixeira ML. Avaliaçãodoperfilbioquímico e parâmetroshematológicosempacientessubmetidos à hemodiálise. Rev Saud Pesq. 2011;4:15-22.
- Mascha V, Rashmi K, Priyadarshi SS, et al. Comparing age wise reference intervals for serum creatinine concentration in a “reality check” of the recommended cut-off. Indian J ClinBiochem. 2006;21:90-94.
- Eduardo OC, Kaue A, Idania AA, et al. Influence of hemodialysis on the plasma concentration of adenosine deaminase in patients with chronic kidney disease. J Bras Patol Med Lab. 2015;51:153-157.
- RusulArifAA, Haider S. A study of some biochemical changes in patients with chronic renal failure undergoing hemodialysis. Int J CurrMicrobiol App Sci. 2014;3: 581-586.
- Noor ul A, Raja Tahir M, JavaidAsad M, et al. Evaluatingurea and creatinine levels in chronic renal failure pre and post dialysis: A prospective study. J Cardiovasc Disease. 2014:2:1-5.
- Azra K. Estimation of blood urea (BUN) and serum creatinine level in patients of renal disorder. J FundamAppl Sci. 2014;4:199-202.
- Raghunandan S, Deepak Kumar S, Ram Lakhan M. Effectiveness of Self Instructional Module (SIM) on knowledge regarding home care management among patients with chronic renal failure undergoing haemodialysis at selected hospital of Punjab. IOSR J Nurs Health Sci. 2016;5:20-31.
- Wendy E, Bloembergen DC, Friedrich K, et al. Relationship of dose of hemodialysis and cause-specific mortality. Kidney Int.1996;50:557-565.
- Toma I, Marinho JS, Limeres JJ, et al. Changes in salivary composition in patients with renal failure. Arch Oral Biol. 2008;53: 528–532.
- Renuga DTS, Gunasekaran S, Wesley HJ, et al. Analysis on renal failure patient’s blood samples: Characterization and efficacy study. Indian J Sci Technol. 2009;2:46-50.
- Kunitoshi I, Yoshiharu I, Koshiro F. Risk factors of end-stage renal disease and serum creatinine in a community-based mass screening. Kidney Int. 1997;51:850-854.
- William R, Clark K, Bruce A, et al. Quantification of creatinine kinetic parameters in patients with acute renal failure. Kidney Int. 1998;54:554-560.
- Mohamd SMA, Muna AB, LeelaBabiker M, et al. Hematological changes post- hemo and peritoneal dialysis among renal failure patients in Sudan. Saudi J Kidney Dis Transpl. 2008;19:274-279.
- Yassin MM, Abdel Monem HL, Ahmed JAT, et al. Homocystiene and hematological indices in Hemodialysis Patients. Ibnosina J Med Biomed Sci. 2014;6:173-179.
- Saba ZA, Layla AM, Dhafer SK. Study of some biochemical changes in serum of patients with chronic renal failure. Irq Nat J Chem. 2012;4:270-280.
- Akbar D, Mohammad M, Shadi T, et al. Anemia and thrombocytopenia in acute and chronic renal failure. Int J HematolOncol Stem Cell Res. 2013;7:34-39.
- Ossman DH, Marouf BH, Ameen KH. Effect of extracorporeal unfractionated heparin on hematological and electrolyte markers in hemodialyzed patients. JPPA. 2014;4:431-439.
- Rock RC, Walker WG, Hennings CD. Nitrogen metabolites and renal function. In:Tietz NW, ed. Fundamentals of Clinical Chemistry, 3rd ed. Philadelphia: WB Saunders. 1987;669-704.
- Attika K, Lubna Z. Effect of hemodialysis on mean prothrombin time and activated partial thromboplastin time in patients of end stage renal disease. Journal RMC. 2015;19:247-249.
- Khaled MD, Faiz A, Abdelgader AT, et al. Effect of haemodialysis on some metabolic products of CKD patients in Libya. WJPPS. 2015;4:45-54.
- Felix C, Stefan CV, Dan R,et al. Hemodialysis- induced electrolyte variation ( serum calcium, magnesium, and bicarbonate) and intradialytic heart rhythm disorders. Int J Bioflux Society. 2014;6:11-14
- Gonella GM. Effect of dialysis on certain biochemical parameters in chronic renal failure patients. International Journal of Contemporary Medical Research. 2016;3: 2454-7379.
- Merzah KS, Hasson SF. The biochemical changes in patients with chronic renal failure. : Int J PharmaMed Bio Sci. 2015;4:75-79.
- Entedhar RS, Nawal AM. Biochemical changes in chronic renal failure pre and post hemodilysis.J Environ SciEng Technol. 2016;5:190-195.
- Suresh M, Mallikarjuna RN, Sharan BSM, et al. Hematological changes in chronic renal failure. . IJSRP. 2012;2:2250-3153.
- ShivanandaNayak B. Manipal manual of clinical biochemistry. Jay Pee Brothers’Medical Publishers (p) Ltd, New Delhi. 2002;98-99.